Abstract
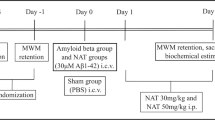
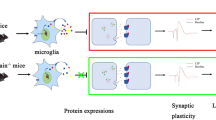
Alzheimer’s disease (AD) is a neurodegenerative disease which is characterized by progressive memory loss, the accumulation of β-amyloid peptide (Aβ) (mainly Aβ1-42), and more recently, by neuroinflammation, which has been highlighted as playing a central role in the development and progress of AD. This study utilized 100-day-old Balb/c mice for the induction of an AD-like dementia model. The animals were administered with Aβ1-42 oligomers (400 pmol/site) or artificial cerebrospinal fluid (ACSF) into the left cerebral ventricle. Twenty-four hours after intracerebroventricular administration, the animals were treated with minocycline (50 mg/kg, via oral gavage) for 17 days. The animals’ locomotion was evaluated using the open-field test. The spatial memory was tested using the Y-maze, and the aversive memory was evaluated using the inhibitory avoidance task. Treatment with minocycline was shown to improve both spatial and aversive memories in mice that were submitted to the dementia model. In addition, minocycline reduced the levels of Aβ and microglial activation in the animals that received the administration of Aβ1-42 oligomers. Moreover, the results suggest that the decrease in microglial activation occurred because of a reduction in the levels of toll-like receptors 2 (TLR2) content, and its adapter protein MyD88, as well as a reduction in the levels of the protein NLRP3, which is indispensable in the assembly of inflammasome. These observations were evaluated via immunohistochemistry and confirmed using the Western blot analysis. Treatment with minocycline had no effect in preventing apoptotic morphologic alterations of the neurons. Thus, the anti-inflammatory effect of minocycline involves TLR2 receptors and NLRP3, besides being beneficial by ameliorating memory impairments.

Graphical Abstract






Similar content being viewed by others
References
Pierce AL, Bullain SS, Kawas CH (2017) Late-Onset Alzheimer Disease. Neurol Clin 35(2):283–293. https://doi.org/10.1016/j.ncl.2017.01.006
Vickers JC, Mitew S, Woodhouse A, Fernandez-Martos CM, Kirkcaldie MT, Canty AJ, McCormack GH, King AE (2016) Defining the earliest pathological changes of Alzheimer’s disease. Curr Alzheimer Res 13(3):281–287
Lambert JC, Ibrahim-Verbaas CA, Harold D, Naj AC, Sims R, Bellenguez C, DeStafano AL, Bis JC et al (2013) Meta-analysis of 74,046 individuals identifies 11 new susceptibility loci for Alzheimer’s disease. Nat Genet 45(12):1452–1458. https://doi.org/10.1038/ng.2802
Heppner FL, Ransohoff RM, Becher B (2015) Immune attack: the role of inflammation in Alzheimer disease. Nat Rev Neurosci 16(6):358–372. https://doi.org/10.1038/nrn3880
Lasagna-Reeves CA, Glabe CG, Kayed R (2011) Amyloid-β annular protofibrils evade fibrillar fate in Alzheimer disease brain. J Biol Chem 286(25):22122–22130. https://doi.org/10.1074/jbc.M111.236257
Borlikova GG, Trejo M, Mably AJ, Mc Donald JM, Sala Frigerio C, Regan CM, Murphy KJ, Masliah E et al (2013) Alzheimer brain-derived amyloid beta-protein impairs synaptic remodeling and memory consolidation. Neurobiol Aging 34(5):1315–1327. https://doi.org/10.1016/j.neurobiolaging.2012.10.028
Yang T, Li S, Xu H (2017) Large soluble oligomers of amyloid beta-protein from Alzheimer brain are far less neuroactive than the smaller oligomers to which they dissociate. 37 (1):152–163. doi:https://doi.org/10.1523/jneurosci.1698-16.2017
Ferreira ST, Clarke JR, Bomfim TR, De Felice FG (2014) Inflammation, defective insulin signaling, and neuronal dysfunction in Alzheimer’s disease. Alzheimers Dement 10(1, Supplement):S76–S83. https://doi.org/10.1016/j.jalz.2013.12.010
Solfrizzi V, D'Introno A, Colacicco AM, Capurso C, Todarello O, Pellicani V, Capurso SA, Pietrarossa G et al (2006) Circulating biomarkers of cognitive decline and dementia. Clin Chim Acta 364(1–2):91–112. https://doi.org/10.1016/j.cca.2005.06.015
Harries LW, Bradley-Smith RM, Llewellyn DJ, Pilling LC, Fellows A, Henley W, Hernandez D, Guralnik JM et al (2012) Leukocyte CCR2 expression is associated with mini-mental state examination score in older adults. Rejuvenation Res 15(4):395–404. https://doi.org/10.1089/rej.2011.1302
Westin K, Buchhave P, Nielsen H, Minthon L, Janciauskiene S, Hansson O (2012) CCL2 is associated with a faster rate of cognitive decline during early stages of Alzheimer’s disease. PLoS One 7(1):e30525. https://doi.org/10.1371/journal.pone.0030525
Nayak D, Roth TL, McGavern DB (2014) Microglia development and function. Annu Rev Immunol 32:367–402. https://doi.org/10.1146/annurev-immunol-032713-120240
Kigerl KA, de Rivero Vaccari JP, Dietrich WD, Popovich PG, Keane RW (2014) Pattern recognition receptors and central nervous system repair. Exp Neurol 258:5–16. https://doi.org/10.1016/j.expneurol.2014.01.001
Lin W, Ding M, Xue J, Leng W (2013) The role of TLR2/JNK/NF-kappaB pathway in amyloid beta peptide-induced inflammatory response in mouse NG108-15 neural cells. Int Immunopharmacol 17(3):880–884. https://doi.org/10.1016/j.intimp.2013.09.016
Zolezzi JM, Inestrosa NC (2017) Wnt/TLR dialog in neuroinflammation, relevance in Alzheimer’s disease. Front Immunol 8:187. https://doi.org/10.3389/fimmu.2017.00187
Udan ML, Ajit D, Crouse NR, Nichols MR (2008) Toll-like receptors 2 and 4 mediate Abeta(1-42) activation of the innate immune response in a human monocytic cell line. J Neurochem 104(2):524–533. https://doi.org/10.1111/j.1471-4159.2007.05001.x
Liu S, Liu Y, Hao W, Wolf L, Kiliaan AJ, Penke B, Rube CE, Walter J et al (2012) TLR2 is a primary receptor for Alzheimer’s amyloid beta peptide to trigger neuroinflammatory activation. J Immunol 188(3):1098–1107. https://doi.org/10.4049/jimmunol.1101121
Heneka MT, Kummer MP, Stutz A, Delekate A, Schwartz S, Vieira-Saecker A, Griep A, Axt D et al (2013) NLRP3 is activated in Alzheimer’s disease and contributes to pathology in APP/PS1 mice. Nature 493(7434):674–678. https://doi.org/10.1038/nature11729
Parajuli B, Sonobe Y, Horiuchi H, Takeuchi H, Mizuno T, Suzumura A (2013) Oligomeric amyloid beta induces IL-1beta processing via production of ROS: implication in Alzheimer’s disease. Cell Death Dis 4:e975. https://doi.org/10.1038/cddis.2013.503
Heneka MT, Kummer MP, Latz E (2014) Innate immune activation in neurodegenerative disease. Nat Rev Immunol 14(7):463–477. https://doi.org/10.1038/nri3705
Tan MS, Yu JT, Jiang T, Zhu XC, Tan L (2013) The NLRP3 inflammasome in Alzheimer’s disease. Mol Neurobiol 48(3):875–882. https://doi.org/10.1007/s12035-013-8475-x
Daniels MJD, Rivers-Auty J, Schilling T, Spencer NG, Watremez W, Fasolino V, Booth SJ, White CS et al (2016) Fenamate NSAIDs inhibit the NLRP3 inflammasome and protect against Alzheimer’s disease in rodent models. Nat Commun 7:12504. https://doi.org/10.1038/ncomms12504
Song L, Pei L, Yao S, Wu Y, Shang Y (2017) NLRP3 inflammasome in neurological diseases, from functions to therapies. Front Cell Neurosci 11:63. https://doi.org/10.3389/fncel.2017.00063
Chen M, Ona VO, Li M, Ferrante RJ, Fink KB, Zhu S, Bian J, Guo L et al (2000) Minocycline inhibits caspase-1 and caspase-3 expression and delays mortality in a transgenic mouse model of Huntington disease. Nat Med 6(7):797–801. https://doi.org/10.1038/77528
Choi Y, Kim HS, Shin KY, Kim EM, Kim M, Kim HS, Park CH, Jeong YH et al (2007) Minocycline attenuates neuronal cell death and improves cognitive impairment in Alzheimer’s disease models. Neuropsychopharmacology 32(11):2393–2404. https://doi.org/10.1038/sj.npp.1301377
Noble W, Garwood C, Stephenson J, Kinsey AM, Hanger DP, Anderton BH (2009) Minocycline reduces the development of abnormal tau species in models of Alzheimer’s disease. FASEB J 23(3):739–750. https://doi.org/10.1096/fj.08-113795
Parachikova A, Vasilevko V, Cribbs DH, LaFerla FM, Green KN (2010) Reductions in amyloid-beta-derived neuroinflammation, with minocycline, restore cognition but do not significantly affect tau hyperphosphorylation. J Alzheimer’s Dis 21(2):527–542. https://doi.org/10.3233/jad-2010-100204
Resende R, Ferreiro E, Pereira C, Resende de Oliveira C (2008) Neurotoxic effect of oligomeric and fibrillar species of amyloid-beta peptide 1-42: involvement of endoplasmic reticulum calcium release in oligomer-induced cell death. Neuroscience 155(3):725–737. https://doi.org/10.1016/j.neuroscience.2008.06.036
Ruiz-Muñoz AM, Nieto-Escamez FA, Aznar S, Colomina MT, Sanchez-Santed F (2011) Cognitive and histological disturbances after chlorpyrifos exposure and chronic Aβ(1–42) infusions in Wistar rats. NeuroToxicology 32(6):836–844. https://doi.org/10.1016/j.neuro.2011.05.014
Gomes GM, Dalmolin GD, Cordeiro MN, Gomez MV, Ferreira J, Rubin MA (2013) The selective A-type K+ current blocker Tx3-1 isolated from the Phoneutria nigriventer venom enhances memory of naïve and Aβ25-35-treated mice. Toxicon 76:23–27. https://doi.org/10.1016/j.toxicon.2013.08.059
Laursen SE, Belknap JK (1986) Intracerebroventricular injections in mice. Some methodological refinements. J Pharmacol Methods 16(4):355–357
Ferretti MT, Allard S, Partridge V, Ducatenzeiler A, Cuello AC (2012) Minocycline corrects early, pre-plaque neuroinflammation and inhibits BACE-1 in a transgenic model of Alzheimer’s disease-like amyloid pathology. J Neuroinflammation 9:62. https://doi.org/10.1186/1742-2094-9-62
Garwood CJ, Cooper JD, Hanger DP, Noble W (2010) Anti-inflammatory impact of minocycline in a mouse model of tauopathy. Front Psychiatry 1:136. https://doi.org/10.3389/fpsyt.2010.00136
Salehi-Sadaghiani M, Javadi-Paydar M, Gharedaghi MH, Zandieh A, Heydarpour P, Yousefzadeh-Fard Y, Dehpour AR (2012) NMDA receptor involvement in antidepressant-like effect of pioglitazone in the forced swimming test in mice. Psychopharmacology 223(3):345–355. https://doi.org/10.1007/s00213-012-2722-0
Dellu F, Fauchey V, Le Moal M, Simon H (1997) Extension of a new two-trial memory task in the rat: influence of environmental context on recognition processes. Neurobiol Learn Mem 67(2):112–120
Roesler R, Walz R, Quevedo J, de-Paris F, Zanata SM, Graner E, Izquierdo I, Martins VR et al (1999) Normal inhibitory avoidance learning and anxiety, but increased locomotor activity in mice devoid of PrP(C). Brain Res Mol Brain Res 71(2):349–353
Lowry OH, Rosebrough NJ, Farr AL, Randall RJ (1951) Protein measurement with the Folin phenol reagent. J Biol Chem 193(1):265–275
Allen Institute. Allen Mouse Brain Atlas (updated 23/04/2016). http://mouse.brain-map.org/static/atlas
Paxinos G, Franklin KBJ (2004) The mouse brain in stereotaxic coordinates. Academic Press, San Diego
Dhull DK, Bhateja D, Dhull RK, Padi SS (2012) Differential role of cyclooxygenase isozymes on neuronal density in hippocampus CA1 region of intracerebroventricular streptozotocin treated rat brain. J Chem Neuroanat 43(1):48–51. https://doi.org/10.1016/j.jchemneu.2011.10.001
Mukumoto N, Nakayama M, Akasaka H, Shimizu Y, Osuga S, Miyawaki D, Yoshida K, Ejima Y et al (2017) Sparing of tissue by using micro-slit-beam radiation therapy reduces neurotoxicity compared with broad-beam radiation therapy. J Radiat Res 58(1):17–23. https://doi.org/10.1093/jrr/rrw065
Tu S, Wong S, Hodges JR, Irish M, Piguet O, Hornberger M (2015) Lost in spatial translation—a novel tool to objectively assess spatial disorientation in Alzheimer’s disease and frontotemporal dementia. Cortex 67:83–94. https://doi.org/10.1016/j.cortex.2015.03.016
Foxe D, Leyton CE, Hodges JR, Burrell JR, Irish M, Piguet O (2016) The neural correlates of auditory and visuospatial span in logopenic progressive aphasia and Alzheimer’s disease. Cortex 83:39–50. https://doi.org/10.1016/j.cortex.2016.07.003
Garcez ML, Mina F, Bellettini-Santos T, Carneiro FG, Luz AP, Schiavo GL, Andrighetti MS, Scheid MG et al (2017) Minocycline reduces inflammatory parameters in the brain structures and serum and reverses memory impairment caused by the administration of amyloid beta (1-42) in mice. Prog Neuro-Psychopharmacol Biol Psychiatry 77:23–31. https://doi.org/10.1016/j.pnpbp.2017.03.010
Bruno MA, Leon WC, Fragoso G, Mushynski WE, Almazan G, Cuello AC (2009) Amyloid beta-induced nerve growth factor dysmetabolism in Alzheimer disease. J Neuropathol Exp Neurol 68(8):857–869. https://doi.org/10.1097/NEN.0b013e3181aed9e6
Biscaro B, Lindvall O, Tesco G, Ekdahl CT, Nitsch RM (2012) Inhibition of microglial activation protects hippocampal neurogenesis and improves cognitive deficits in a transgenic mouse model for Alzheimer’s disease. Neurodegener Dis 9(4):187–198. https://doi.org/10.1159/000330363
Seabrook TJ, Jiang L, Maier M, Lemere CA (2006) Minocycline affects microglia activation, Abeta deposition, and behavior in APP-tg mice. Glia 53(7):776–782. https://doi.org/10.1002/glia.20338
Wang Y, Cella M, Mallinson K, Ulrich JD, Young KL, Robinette ML, Gifillian S, Krishnan GM et al (2015) TREM2 lipid sensing sustains microglia response in an Alzheimer’s disease model. Cell 160(6):1061–1071. https://doi.org/10.1016/j.cell.2015.01.049
Tursi SA, Lee EY (2017) Bacterial amyloid curli acts as a carrier for DNA to elicit an autoimmune response via TLR2 and TLR9. 13(4):e1006315. doi:https://doi.org/10.1371/journal.ppat.1006315
Henry CJ, Huang Y, Wynne A, Hanke M, Himler J, Bailey MT, Sheridan JF, Godbout JP (2008) Minocycline attenuates lipopolysaccharide (LPS)-induced neuroinflammation, sickness behavior, and anhedonia. J Neuroinflammation 5:15–15. https://doi.org/10.1186/1742-2094-5-15
Shahzad K, Bock F, Al-Dabet MM, Gadi I, Nazir S, Wang H, Kohli S, Ranjan S et al (2016) Stabilization of endogenous Nrf2 by minocycline protects against Nlrp3-inflammasome induced diabetic nephropathy. Sci Rep 6:34228. https://doi.org/10.1038/srep34228
Li J, Chen J, Mo H, Chen J, Qian C, Yan F, Gu C, Hu Q et al (2016) Minocycline protects against NLRP3 inflammasome-induced inflammation and P53-associated apoptosis in early brain injury after subarachnoid hemorrhage. Mol Neurobiol 53(4):2668–2678. https://doi.org/10.1007/s12035-015-9318-8
Lu Y, Xiao G, Luo W (2016) Minocycline suppresses NLRP3 inflammasome activation in experimental ischemic stroke. Neuroimmunomodulation 23(4):230–238. https://doi.org/10.1159/000452172
Chen W, Zhao M, Zhao S, Lu Q, Ni L, Zou C, Lu L, Xu X et al (2017) Activation of the TXNIP/NLRP3 inflammasome pathway contributes to inflammation in diabetic retinopathy: a novel inhibitory effect of minocycline. Inflamm Res 66(2):157–166. https://doi.org/10.1007/s00011-016-1002-6
Wu Z, Zou X, Zhu W, Mao Y, Chen L, Zhao F (2016) Minocycline is effective in intracerebral hemorrhage by inhibition of apoptosis and autophagy. J Neurol Sci 371:88–95. https://doi.org/10.1016/j.jns.2016.10.025
Zhu S, Stavrovskaya IG, Drozda M, Kim BY, Ona V, Li M, Sarang S, Liu AS et al (2002) Minocycline inhibits cytochrome c release and delays progression of amyotrophic lateral sclerosis in mice. Nature 417(6884):74–78. https://doi.org/10.1038/417074a
Sancho M, Herrera AE, Gortat A, Carbajo RJ, Pineda-Lucena A, Orzaez M, Perez-Paya E (2011) Minocycline inhibits cell death and decreases mutant Huntingtin aggregation by targeting Apaf-1. Hum Mol Genet 20(18):3545–3553. https://doi.org/10.1093/hmg/ddr271
Haghi-Aminjan H, Asghari MH, Goharbari MH, Abdollahi M (2017) A systematic review on potential mechanisms of minocycline in kidney diseases. Pharmacol Rep 69(4):602–609. https://doi.org/10.1016/j.pharep.2017.02.001
He Y, Zeng MY, Yang D, Motro B, Nunez G (2016) NEK7 is an essential mediator of NLRP3 activation downstream of potassium efflux. Nature 530(7590):354–357. https://doi.org/10.1038/nature16959
Liston A, Masters SL (2017) Homeostasis-altering molecular processes as mechanisms of inflammasome activation. Nat Rev Immunol 17(3):208–214. https://doi.org/10.1038/nri.2016.151
Wang D, Zhang J, Jiang W, Cao Z, Zhao F, Cai T, Aschner M, Luo W (2017) The role of NLRP3-CASP1 in inflammasome-mediated neuroinflammation and autophagy dysfunction in manganese-induced, hippocampal-dependent impairment of learning and memory ability. Autophagy 13:1–14. https://doi.org/10.1080/15548627.2017.1293766
Acknowledgments
This study was supported by UNESC, CAPES, and CNPq (Universal/409859/2016-8- Brazil). JB is a 2 CNPq Research Fellow.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Garcez, M.L., Mina, F., Bellettini-Santos, T. et al. The Involvement of NLRP3 on the Effects of Minocycline in an AD-Like Pathology Induced by β-Amyloid Oligomers Administered to Mice. Mol Neurobiol 56, 2606–2617 (2019). https://doi.org/10.1007/s12035-018-1211-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-018-1211-9