Abstract
Pesticide exposure is recognized as a risk factor for Alzheimer’s disease (AD). We investigated early signs of AD-like pathology upon exposure to a pyrethroid pesticide, cypermethrin, reported to impair neurodevelopment. We treated weanling rats with cypermethrin (10 and 25 mg/kg) and detected dose-dependent increase in the key proteins of AD, amyloid beta (Aβ), and phospho-tau, in frontal cortex and hippocampus as early as postnatal day 45. Upregulation of Aβ pathway involved an increase in amyloid precursor protein (APP) and its pro-amyloidogenic processing through beta-secretase (BACE) and gamma-secretase. Tau pathway entailed elevation in tau and glycogen-synthase kinase-3-beta (GSK3β)-dependent, phospho-tau. GSK3β emerged as a molecular link between the two pathways, evident from reduction in phospho-tau as well as BACE upon treating GSK3β inhibitor, lithium chloride. Exploring the mechanism revealed an attenuated heparin-binding epidermal growth factor (HB-EGF) signaling and downstream astrogliosis-mediated neuroinflammation to be responsible for inducing Aβ and phospho-tau. Cypermethrin caused a proximal reduction in HB-EGF, which promoted astrocytic nuclear factor kappa B signaling and astroglial activation close to Aβ and phospho-tau. Glial activation stimulated generation of interleukin-1 (IL-1), which upregulated GSK3β, and APP and tau as well, resulting in co-localization of Aβ and phospho-tau with IL-1 receptor. Intracerebral insertion of exogenous HB-EGF restored its own signaling and suppressed neuroinflammation and thereby Aβ and phospho-tau in cypermethrin-exposed rats, proving a central role of reduced HB-EGF signaling in cypermethrin-mediated neurodegeneration. Furthermore, cypermethrin stimulated cognitive impairments, which could be prevented by exogenous HB-EGF. Our data demonstrate that cypermethrin induces premature upregulation of GSK3β-dependent Aβ and tau pathways, where HB-EGF signaling and neuroinflammation serve as essential regulators.







Similar content being viewed by others
Change history
30 August 2019
The original version of this article unfortunately contained mistakes. The authors noticed that Fig.��1C (cortex), 1D (hippocampus), 4A (cortex), 4B (cortex) and the beta actin Western blot of Supplement 2A in the original article had errors.
References
Maccioni RB, Munoz JP, Barbeito L (2001) The molecular bases of Alzheimer’s disease and other neurodegenerative disorders. Arch Med Res 32:367–381
Parron T, Requena M, Hernandez AF, Alarcon R (2011) Association between environmental exposure to pesticides and neurodegenerative diseases. Toxicol Appl Pharmacol 256:379–385
Ray DE, Fry JR (2006) A reassessment of the neurotoxicity of pyrethroid insecticides. Pharmacol Ther 111:174–193
Gupta A, Agarwal R, Shukla GS (1999) Functional impairment of blood-brain barrier following pesticide exposure during early development in rats. Hum Exp Toxicol 18:174–179
Singh AK, Tiwari MN, Upadhyay G, Patel DK, Singh D, Prakash O et al (2012) Long term exposure to cypermethrin induces nigrostriatal dopaminergic neurodegeneration in adult rats: postnatal exposure enhances the susceptibility during adulthood. Neurobiol Aging 33:404–415
Sery O, Povova J, Misek I, Pesak L, Janout V (2013) Molecular mechanisms of neuropathological changes in Alzheimer’s disease: a review. Folia Neuropathol 51:1–9
Sobow T, Flirski M, Liberski PP (2004) Amyloid-beta and tau proteins as biochemical markers of Alzheimer’s disease. Acta Neurobiol Exp 64:53–70
Fein JA, Sokolow S, Miller CA, Vinters HV, Yang F, Cole GM et al (2008) Co-localization of amyloid beta and tau pathology in Alzheimer’s disease synaptosomes. Am J Pathol 172:1683–1692
Pozueta J, Lefort R, Shelanski ML (2013) Synaptic changes in Alzheimer’s disease and its models. Neuroscience 251:51–65
Dodart JC, Mathis C, Ungerer A (2000) The beta-amyloid precursor protein and its derivatives: from biology to learning and memory processes. Rev Neurosci 11:75–93
Hardy J, Selkoe DJ (2002) The amyloid hypothesis of Alzheimer’s disease: progress and problems on the road to therapeutics. Science 297:353–356
Pooler AM, Polydoro M, Wegmann S, Nicholls SB, Spires-Jones TL, Hyman BT (2013) Propagation of tau pathology in Alzheimer’s disease: identification of novel therapeutic targets. Alzheimers Res Ther 5:49
Hooper C, Killick R, Lovestone S (2008) The GSK3 hypothesis of Alzheimer’s disease. J Neurochem 104:1433–1439
Su Y, Ryder J, Li B, Wu X, Fox N, Solenberg P et al (2004) Lithium, a common drug for bipolar disorder treatment, regulates amyloid-beta precursor protein processing. Biochemistry 43:6899–6908
Qing H, He G, Ly PT, Fox CJ, Staufenbiel M, Cai F et al (2008) Valproic acid inhibits Abeta production, neuritic plaque formation, and behavioral deficits in Alzheimer’s disease mouse models. J Exp Med 205:2781–2789
Ly PT, Wu Y, Zou H, Wang R, Zhou W, Kinoshita A et al (2013) Inhibition of GSK3beta-mediated BACE1 expression reduces Alzheimer-associated phenotypes. J Clin Invest 123:224–235
Griffin WS, Stanley LC, Ling C, White L, MacLeod V, Perrot LJ et al (1989) Brain interleukin 1 and S-100 immunoreactivity are elevated in Down syndrome and Alzheimer disease. Proc Natl Acad Sci U S A 86:7611–7615
Wang HM, Zhang T, Huang JK, Sun XJ (2013) 3-N-butylphthalide (NBP) attenuates the amyloid-beta-induced inflammatory responses in cultured astrocytes via the nuclear factor-kappaB signaling pathway. Cell Physiol Biochem 32:235–242
Rogers JT, Lahiri DK (2004) Metal and inflammatory targets for Alzheimer’s disease. Curr Drug Targets 5:535–551
Ghosh S, Wu MD, Shaftel SS, Kyrkanides S, LaFerla FM, Olschowka JA et al (2013) Sustained interleukin-1beta overexpression exacerbates tau pathology despite reduced amyloid burden in an Alzheimer’s mouse model. J Neurosci 33:5053–5064
Tiwari MN, Singh AK, Agrawal S, Gupta SP, Jyoti A, Shanker R et al (2012) Cypermethrin alters the expression profile of mRNAs in the adult rat striatum: a putative mechanism of postnatal pre-exposure followed by adulthood re-exposure-enhanced neurodegeneration. Neurotox Res 22:321–334
Maurya SK, Rai A, Rai NK, Deshpande S, Jain R, Mudiam MK et al (2012) Cypermethrin induces astrocyte apoptosis by the disruption of the autocrine/paracrine mode of epidermal growth factor receptor signaling. Toxicol Sci 125:473–487
Opanashuk LA, Mark RJ, Porter J, Damm D, Mattson MP, Seroogy KB (1999) Heparin-binding epidermal growth factor-like growth factor in hippocampus: modulation of expression by seizures and anti-excitotoxic action. J Neurosci 19:133–146
Oyagi A, Moriguchi S, Nitta A, Murata K, Oida Y, Tsuruma K et al (2011) Heparin-binding EGF-like growth factor is required for synaptic plasticity and memory formation. Brain Res 1419:97–104
Oyagi A, Hara H (2012) Essential roles of heparin-binding epidermal growth factor-like growth factor in the brain. CNS Neurosci Ther 18:803–810
Martin R, Cordova C, Nieto ML (2012) Secreted phospholipase A2-IIA-induced a phenotype of activated microglia in BV-2 cells requires epidermal growth factor receptor transactivation and proHB-EGF shedding. J Neuroinflammation 9:154
Schenk GJ, Dijkstra S, van het Hof AJ, van der Pol SM, Drexhage JA, van der Valk P et al (2013) Roles for HB-EGF and CD9 in multiple sclerosis. Glia 61:1890–1905
Singh A, Yadav S, Srivastava V, Kumar R, Singh D, Sethumadhavan R et al (2013) Imprinting of cerebral and hepatic cytochrome p450s in rat offsprings exposed prenatally to low doses of cypermethrin. Mol Neurobiol 48:128–140
Tanno M, Kuno A, Ishikawa S, Miki T, Kouzu H, Yano T, et al. (2014) Translocation of GSK-3beta, a trigger of permeability transition, is kinase activity-dependent and mediated by interaction with VDAC2. J Biol Chem 289(42):29285–96
Phiel CJ, Wilson CA, Lee VM, Klein PS (2003) GSK-3alpha regulates production of Alzheimer’s disease amyloid-beta peptides. Nature 423:435–439
Schmid AW, Lynch MA, Herron CE (2009) The effects of IL-1 receptor antagonist on beta amyloid mediated depression of LTP in the rat CA1 in vivo. Hippocampus 19:670–676
Sinha RA, Khare P, Rai A, Maurya SK, Pathak A, Mohan V et al (2009) Anti-apoptotic role of omega-3-fatty acids in developing brain: perinatal hypothyroid rat cerebellum as apoptotic model. Int J Dev Neurosci 27:377–383
Rai A, Maurya SK, Khare P, Srivastava A, Bandyopadhyay S (2010) Characterization of developmental neurotoxicity of As, Cd, and Pb mixture: synergistic action of metal mixture in glial and neuronal functions. Toxicol Sci 118:586–601
Engvall E, Perlmann P, Enzyme-linked immunosorbent assay (ELISA) (1971) Quantitative assay of immunoglobulin G. Immunochemistry 8:871–874
Yadav RS, Chandravanshi LP, Shukla RK, Sankhwar ML, Ansari RW, Shukla PK et al (2011) Neuroprotective efficacy of curcumin in arsenic induced cholinergic dysfunctions in rats. Neurotoxicology 32:760–768
Kuperstein I, Broersen K, Benilova I, Rozenski J, Jonckheere W, Debulpaep M et al (2010) Neurotoxicity of Alzheimer’s disease Abeta peptides is induced by small changes in the Abeta42 to Abeta40 ratio. EMBO J 29:3408–3420
Rodriguez JJ, Olabarria M, Chvatal A, Verkhratsky A (2009) Astroglia in dementia and Alzheimer’s disease. Cell Death Differ 16:378–385
Akama KT, Albanese C, Pestell RG, Van Eldik LJ (1998) Amyloid beta-peptide stimulates nitric oxide production in astrocytes through an NFkappaB-dependent mechanism. Proc Natl Acad Sci U S A 95:5795–5800
Yu AC, Lee YL, Eng LF (1991) Inhibition of GFAP synthesis by antisense RNA in astrocytes. J Neurosci Res 30:72–79
Eng LF, Ghirnikar RS, Lee YL (2000) Glial fibrillary acidic protein: GFAP-thirty-one years (1969-2000). Neurochem Res 25:1439–1451
Kamphuis W, Middeldorp J, Kooijman L, Sluijs JA, Kooi EJ, Moeton M et al (2014) Glial fibrillary acidic protein isoform expression in plaque related astrogliosis in Alzheimer’s disease. Neurobiol Aging 35:492–510
Carloni M, Nasuti C, Fedeli D, Montani M, Amici A, Vadhana MS et al (2012) The impact of early life permethrin exposure on development of neurodegeneration in adulthood. Exp Gerontol 47:60–66
Chen NN, Luo DJ, Yao XQ, Yu C, Wang Y, Wang Q et al (2012) Pesticides induce spatial memory deficits with synaptic impairments and an imbalanced tau phosphorylation in rats. J Alzheimer’s Dis 30:585–594
Schraen-Maschke S, Sergeant N, Dhaenens CM, Bombois S, Deramecourt V, Caillet-Boudin ML et al (2008) Tau as a biomarker of neurodegenerative diseases. Biomark Med 2:363–384
Stoothoff WH, Johnson GV (2005) Tau phosphorylation: physiological and pathological consequences. Biochim Biophys Acta 1739:280–297
Avila J, Lucas JJ, Perez M, Hernandez F (2004) Role of tau protein in both physiological and pathological conditions. Physiol Rev 84:361–384
Muyllaert D, Kremer A, Jaworski T, Borghgraef P, Devijver H, Croes S et al (2008) Glycogen synthase kinase-3beta, or a link between amyloid and tau pathology? Genes Brain Behav 7(Suppl 1):57–66
Wen Y, Planel E, Herman M, Figueroa HY, Wang L, Liu L et al (2008) Interplay between cyclin-dependent kinase 5 and glycogen synthase kinase 3 beta mediated by neuregulin signaling leads to differential effects on tau phosphorylation and amyloid precursor protein processing. Neuron 28:2624–2632
Takashima A, Murayama M, Murayama O, Kohno T, Honda T, Yasutake K et al (1998) Presenilin 1 associates with glycogen synthase kinase-3beta and its substrate tau. Proc Natl Acad Sci U S A 95:9637–9641
Wang L, Chiang HC, Wu W, Liang B, Xie Z, Yao X et al (2012) Epidermal growth factor receptor is a preferred target for treating amyloid-beta-induced memory loss. Proc Natl Acad Sci U S A 109:16743–16748
Jin K, Mao XO, Del Rio Guerra G, Jin L, Greenberg DA (2005) Heparin-binding epidermal growth factor-like growth factor stimulates cell proliferation in cerebral cortical cultures through phosphatidylinositol 3′-kinase and mitogen-activated protein kinase. J Neurosci Res 81:497–505
Jin K, Mao XO, Sun Y, Xie L, Jin L, Nishi E et al (2002) Heparin-binding epidermal growth factor-like growth factor: hypoxia-inducible expression in vitro and stimulation of neurogenesis in vitro and in vivo. J Neurosci 22:5365–5373
Marikovsky M, Breuing K, Liu PY, Eriksson E, Higashiyama S, Farber P et al (1993) Appearance of heparin-binding EGF-like growth factor in wound fluid as a response to injury. Proc Natl Acad Sci U S A 90:3889–3893
Lee JY, Seo YN, Park HJ, Park YJ, Chung CP (2012) The cell-penetrating peptide domain from human heparin-binding epidermal growth factor-like growth factor (HB-EGF) has anti-inflammatory activity in vitro and in vivo. Biochem Biophys Res Commun 419:597–604
Mehta VB, Besner GE (2003) Inhibition of NF-kappa B activation and its target genes by heparin-binding epidermal growth factor-like growth factor. J Immunol 171:6014–6022
Mehta VB, Besner GE (2005) Heparin-binding epidermal growth factor-like growth factor inhibits cytokine-induced NF-kappa B activation and nitric oxide production via activation of the phosphatidylinositol 3-kinase pathway. J Immunol 175:1911–1918
Maurya SK, Mishra J, Tripathi VK, Sharma R, Siddiqui MH (2014) Cypermethrin induces astrocyte damage: role of aberrant Ca(2+), ROS, JNK, P38, matrix metalloproteinase 2 and migration related reelin protein. Pestic Biochem Physiol 111:51–59
Gonzalez A, Pariente JA, Salido GM (2007) Ethanol stimulates ROS generation by mitochondria through Ca2+ mobilization and increases GFAP content in rat hippocampal astrocytes. Brain Res 1178:28–37
Kleinman MT, Araujo JA, Nel A, Sioutas C, Campbell A, Cong PQ et al (2008) Inhaled ultrafine particulate matter affects CNS inflammatory processes and may act via MAP kinase signaling pathways. Toxicol Lett 178:127–130
Roy Choudhury G, Ryou MG, Poteet E, Wen Y, He R, Sun F et al (2014) Involvement of p38 MAPK in reactive astrogliosis induced by ischemic stroke. Brain Res 1551:45–58
Kitazawa M, Cheng D, Tsukamoto MR, Koike MA, Wes PD, Vasilevko V et al (2011) Blocking IL-1 signaling rescues cognition, attenuates tau pathology, and restores neuronal beta-catenin pathway function in an Alzheimer’s disease model. J Immunol 187:6539–6549
Spires-Jones T, Knafo S (2012) Spines, plasticity, and cognition in Alzheimer’s model mice. Neural Plast 2012:319836
Acknowledgments
Funding from CSIR Network project-INDEPTH and miND are acknowledged. We acknowledge Dr. Debabrata Ghosh, CSIR-IITR, for helping in making Fig. 7; Mr Rajesh Khushwaha for helping in making Figs. 2 and 4; and Dr. Naibedya Chattopadhyay, CSIR-CDRI, for useful suggestions in writing the manuscript.
Conflict of Interest
The authors declare no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Suppl. 1
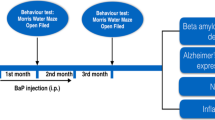
Timeline of treatments. A: To investigate the effect of cypermethrin alone; B: To investigate the role of GSK3β- inhibition (by LiCl) in cypermethrin-treated rats; C: To investigate the effect of exogenous HB-EGF in cypermethrin-treated rats; D: To investigate the effect of IL-1R1-inhibition (by IL-1Ra) in cypermethrin-treated rats. (GIF 30 kb)
High Resolution Image
(TIFF 233 kb)
Suppl. 2
LiCL and IL-1Ra suppress GSK3β and IL-1R1. A. Representative western blot and densitometry of GSK3β normalized with β-actin in cortex (LHS) and hippocampus (RHS) of rats treated with cypermethrin and/or LiCl (V= vehicle treated, VL= LiCl + vehicle treated, Cyp= cypermethrin treated and CypL = LiCl + cypermethrin treated). B. Representative western blot and densitometry of IL-1R1 normalized with β-actin in cortex (LHS) and hippocampus (RHS) of rats treated with cypermethrin and/or IL-1Ra (V= vehicle treated, VRa= IL-1Ra + vehicle treated, cyp= cypermethrin treated and cypRa= IL-1Ra + cypermethrin treated). Data represent means ± SE of five rats. ***P<0.001, **P<0.01 and *P<0.05 compared to vehicle (V) or as indicated. (GIF 23 kb)
High Resolution Image
(TIFF 201 kb)
Suppl. 3
Cypermethrin induces microglial activation in close proximity of Aβ 1-42 and p-tau. A: Representative photomicrograph (40×-magnification) of microglial marker (Iba-1) (green fluorescence), Aβ1-42 (red fluorescence), nucleus (blue fluorescence), and the three merged in the same field in cortex of cypermethrin-treated rats. B. Representative imunohistochemical photomicrograph of microglial marker (CD68) (red fluorescence), p-tau (green fluorescence), nucleus (blue fluorescence), and the three merged in the same field in cortex of cypermethrin-treated rats. The sections are representatives of five different rats. (GIF 63 kb)
High Resolution Image
(TIFF 948 kb)
Suppl. 4
IL-1Ra suppresses Aβ and p-tau. A-B: Representative western blot and densitometry of Aβ1-42 (A) and p-tau (B) normalized with β-actin in cortex (LHS) and hippocampus (RHS) of rats treated with cypermethrinand/or IL-1Ra (V= vehicle treated, VRa= IL-1Ra + vehicle treated, cyp= cypermethrin treated and cypRa= IL-1Ra + cypermethrin treated). Data represent means ± SE of five rats. ***P<0.001, **P<0.01 and *P<0.05 compared to vehicle (V) or as indicated. (GIF 20 kb)
High Resolution Image
(TIFF 178 kb)
Suppl. 5
Cypermethrin induces neuronal localization of IL-1R1 and GSK3β. A-B. Representative photomicrograph (40×-magnification) of IL-1R1 (green fluorescence) (A) and GSK3β (green fluorescence) (B), MAP2 (red fluorescence), nucleus (blue fluorescence), and the three merged in the same field. The sections are representatives of five different rats. (GIF 83 kb)
High Resolution Image
(TIFF 1279 kb)
Rights and permissions
About this article
Cite this article
Maurya, S.K., Mishra, J., Abbas, S. et al. Cypermethrin Stimulates GSK3β-Dependent Aβ and p-tau Proteins and Cognitive Loss in Young Rats: Reduced HB-EGF Signaling and Downstream Neuroinflammation as Critical Regulators. Mol Neurobiol 53, 968–982 (2016). https://doi.org/10.1007/s12035-014-9061-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-014-9061-6