Abstract
Background
Malignant brain edema (MBE) is a life-threatening complication that can occur after mechanical thrombectomy (MT) for acute ischemic stroke. The hypoperfusion intensity ratio (HIR) reflects the tissue-level perfusion status within the ischemic territory. This study investigated the association between HIR and MBE occurrence after MT in patients with anterior circulation large artery occlusion.
Methods
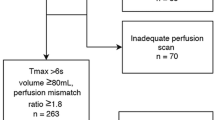
We conducted a retrospective cohort study of patients who received MT at a comprehensive stroke center from February 2020 to June 2022. Using computed tomography perfusion, the HIR was derived from the ratio of tissue volume with a time to maximum (Tmax) > 10 s to that with a Tmax > 6 s. We dichotomized patients based on the occurrence of MBE following MT. The primary outcome, assessed using a multivariable logistic regression model, was the MBE occurrence post MT. The secondary outcome focused on favorable outcomes, defined as achieving a modified Rankin Scale score of 0–2 at 90 days.
Results
Of the 603 included patients, 90 (14.9%) developed MBE after MT. The median HIR exhibited a significantly higher value in the MBE group compared with the non-MBE group (0.5 vs. 0.3; P < 0.001). Multivariable logistic regression analysis indicated that a higher HIR (adjusted odds ratio [aOR] 8.98; 95% confidence interval [CI] 2.85–28.25; P < 0.001), baseline large infarction (Alberta Stroke Program Early Computed Tomography Score < 6; aOR 1.77; 95% CI 1.04–3.01; P = 0.035), internal carotid artery occlusion (aOR 1.80; 95% CI 1.07–3.01; P = 0.028), and unsuccessful recanalization (aOR 8.45; 95% CI 4.75–15.03; P < 0.001) were independently associated with MBE post MT. Among those with successful recanalization, a higher HIR (P = 0.017) and baseline large infarction (P = 0.032) remained as predictors of MBE occurrence. Furthermore, a higher HIR (P = 0.001) and the occurrence of MBE (P < 0.001) both correlated with reduced odds of achieving favorable outcomes.
Conclusions
The presence of a higher HIR on pretreatment perfusion imaging serves as a robust predictor for MBE occurrence after MT, irrespective of successful recanalization.


Similar content being viewed by others
References
Goyal M, Menon BK, van Zwam WH, et al. Endovascular thrombectomy after large-vessel ischaemic stroke: a meta-analysis of individual patient data from five randomised trials. Lancet. 2016;387(10029):1723–31.
Jovin TG, Nogueira RG, Lansberg MG, et al. Thrombectomy for anterior circulation stroke beyond 6 h from time last known well (AURORA): a systematic review and individual patient data meta-analysis. Lancet. 2022;399(10321):249–58.
Huo X, Ma G, Tong X, et al. Trial of endovascular therapy for acute ischemic stroke with large infarct. N Engl J Med. 2023;388(14):1272–83.
Yoshimura S, Sakai N, Yamagami H, et al. Endovascular therapy for acute stroke with a large ischemic region. N Engl J Med. 2022;386(14):1303–13.
Sarraj A, Hassan AE, Abraham MG, et al. Trial of endovascular thrombectomy for large ischemic strokes. N Engl J Med. 2023;388(14):1259–71.
Vahedi K, Hofmeijer J, Juettler E, et al. Early decompressive surgery in malignant infarction of the middle cerebral artery: a pooled analysis of three randomised controlled trials. Lancet Neurol. 2007;6(3):215–22.
Huang X, Chen C, Wang H, Cai Q, Li Z, Xu J, Yuan L, Xu X, Yang Q, Zhou Z, Liu X. The ACORNS grading scale: a novel tool for the prediction of malignant brain edema after endovascular thrombectomy. J Neurointerventional Surg. 2023;15(e2):e190–7.
Guo W, Xu J, Zhao W, et al. A nomogram for predicting malignant cerebral artery infarction in the modern thrombectomy era. Front Neurol. 2022;13:934051.
Bernsen MLE, Kauw F, Martens JM, et al. Malignant infarction after endovascular treatment: Incidence and prediction. Int J Stroke. 2022;17(2):198–206.
Kimberly WT, Dutra BG, Boers AMM, et al. Association of reperfusion with brain edema in patients with acute ischemic stroke: a secondary analysis of the MR CLEAN trial. JAMA Neurol. 2018;75(4):453–61.
Maier IL, Behme D, Schnieder M, et al. Early computed tomography-based scores to predict decompressive hemicraniectomy after endovascular therapy in acute ischemic stroke. PLoS ONE. 2017;12(3):e0173737.
Huang X, Yang Q, Shi X, et al. Predictors of malignant brain edema after mechanical thrombectomy for acute ischemic stroke. J Neurointerv Surg. 2019;11(10):994–8.
Olivot JM, Mlynash M, Inoue M, et al. Hypoperfusion intensity ratio predicts infarct progression and functional outcome in the DEFUSE 2 Cohort. Stroke. 2014;45(4):1018–23.
Guenego A, Fahed R, Albers GW, et al. Hypoperfusion intensity ratio correlates with angiographic collaterals in acute ischaemic stroke with M1 occlusion. Eur J Neurol. 2020;27(5):864–70.
de Havenon A, Mlynash M, Kim-Tenser MA, et al. Results from DEFUSE 3: good collaterals are associated with reduced ischemic core growth but not neurologic outcome. Stroke. 2019;50(3):632–8.
Faizy TD, Kabiri R, Christensen S, et al. Perfusion imaging-based tissue-level collaterals predict ischemic lesion net water uptake in patients with acute ischemic stroke and large vessel occlusion. J Cereb Blood Flow Metab. 2021;41(8):2067–75.
Murray NM, Culbertson CJ, Wolman DN, Mlynash M, Lansberg MG. Hypoperfusion intensity ratio predicts malignant edema and functional outcome in large-vessel occlusive stroke with poor revascularization. Neurocrit Care. 2021;35(1):79–86.
Sarraj A, Kleinig TJ, Hassan AE, et al. Association of endovascular thrombectomy vs medical management with functional and safety outcomes in patients treated beyond 24 hours of last known well: The select late study. JAMA Neurol. 2023;80(2):172–82.
von Elm E, Altman DG, Egger M, et al. Strengthening the reporting of observational studies in epidemiology (STROBE) statement: guidelines for reporting observational studies. BMJ. 2007;335(7624):806–8.
von Kummer R, Broderick JP, Campbell BC, et al. The heidelberg bleeding classification: classification of bleeding events after ischemic stroke and reperfusion therapy. Stroke. 2015;46(10):2981–6.
Higashida RT, Furlan AJ, Roberts H, et al. Trial design and reporting standards for intra-arterial cerebral thrombolysis for acute ischemic stroke. Stroke. 2003;34(8):e109–37.
Yang P, Zhang Y, Zhang L, et al. Endovascular thrombectomy with or without intravenous Alteplase in acute stroke. N Engl J Med. 2020;382(21):1981–93.
Wardlaw JM, Sellar R. A simple practical classification of cerebral infarcts on CT and its interobserver reliability. AJNR Am J Neuroradiol. 1994;15(10):1933–9.
Ong CJ, Gluckstein J, Laurido-Soto O, Yan Y, Dhar R, Lee JM. Enhanced detection of Edema in malignant anterior circulation stroke (EDEMA) score: a risk prediction tool. Stroke. 2017;48(7):1969–72.
Investigators RBT, Qiu Z, Li F, et al. Effect of Intravenous Tirofiban vs Placebo before endovascular Thrombectomy on functional outcomes in large vessel occlusion stroke: The RESCUE BT randomized clinical trial. JAMA. 2022;328(6):543–53.
Haggenmüller B, Kreiser K, Sollmann N, Huber M, Vogele D, Schmidt SA, Beer M, Schmitz B, Ozpeynirci Y, Rosskopf J, Kloth C. Pictorial review on imaging findings in cerebral CTP in patients with acute stroke and its mimics: a primer for general radiologists. Diagnostics. 2023;13(3):447.
van Horn N, Broocks G, Kabiri R, Kraemer MC, Christensen S, Mlynash M, Meyer L, Lansberg MG, Albers GW, Sporns P, Guenego A. Cerebral hypoperfusion intensity ratio is linked to progressive early edema formation. J Clin Med. 2022;11(9):2373.
Winkelmeier L, Heit JJ, Adusumilli G, et al. Hypoperfusion intensity ratio is correlated with the risk of parenchymal hematoma after endovascular stroke treatment. Stroke. 2023;54(1):135–43.
Guenego A, Mlynash M, Christensen S, et al. Hypoperfusion ratio predicts infarct growth during transfer for thrombectomy. Ann Neurol. 2018;84(4):616–20.
Faizy TD, Mlynash M, Kabiri R, Christensen S, Kuraitis G, Meyer L, Bechstein M, Van Horn N, Lansberg MG, Albers G, Fiehler J. Favourable arterial, tissue-level and venous collaterals correlate with early neurological improvement after successful thrombectomy treatment of acute ischaemic stroke. J Neurol Neurosurg Psychiatr. 2022;93(7):701–6.
Maslias E, Nannoni S, Bartolini B, et al. Early-versus-Late endovascular stroke treatment: similar frequencies of Nonrevascularization and Postprocedural cerebrovascular complications in a large single-center cohort study. AJNR Am J Neuroradiol. 2023;44(6):687–92.
Albers GW, Marks MP, Kemp S, et al. Thrombectomy for stroke at 6 to 16 hours with selection by perfusion imaging. N Engl J Med. 2018;378(8):708–18.
Author information
Authors and Affiliations
Contributions
Conceptualization: WH; data collection: WC, JL, MW, ZG; data analysis: WC, XW, SY, LY; drafting of the manuscript: WC; study supervision and organization: WH; revising of the manuscript: XW.
Corresponding author
Ethics declarations
Conflicts of interest
There are no conflicts of interest to declare.
Ethical Approval
The local institutional ethics committees (Beijing Chaoyang Hospital and Linyi People’s Hospital) approved the study in accordance with the Declaration of Helsinki.
Informed Consent
The institutional review boards waived the need for informed consent for the retrospective study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is related to the commentary article available at https://doi.org/10.1007/s12028-023-01901-3.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Chen, W., Wang, X., Liu, J. et al. Association Between Hypoperfusion Intensity Ratio and Postthrombectomy Malignant Brain Edema for Acute Ischemic Stroke. Neurocrit Care 40, 196–204 (2024). https://doi.org/10.1007/s12028-023-01900-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-023-01900-4