Abstract
Background
Case series have reported reversible left ventricular dysfunction, also known as stress cardiomyopathy or Takotsubo cardiomyopathy (TCM), in the setting of acute neurological diseases such as subarachnoid hemorrhage. The relative associations between various neurological diseases and Takotsubo remain incompletely understood.
Methods
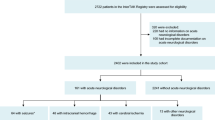
We performed a cross-sectional study of all adults in the National Inpatient Sample, a nationally representative sample of US hospitalizations, from 2006 to 2014. Our exposures of interest were primary diagnoses of acute neurological disease, defined by ICD-9-CM diagnosis codes. Our outcome was a diagnosis of TCM. Binary logistic regression models were used to examine the associations between our pre-specified neurological diagnoses and TCM after adjustment for demographics.
Results
Among acute neurological diagnoses, the strongest associations were seen with subarachnoid hemorrhage (odds ratio [OR] 11.7; 95% confidence interval [CI] 10.2–13.4), status epilepticus (OR 4.9; 95% CI 3.7–6.3), and seizures (OR 1.3; 95% CI 1.1–1.5). In a sensitivity analysis including secondary diagnoses of acute neurological diagnoses, associations were also seen with transient global amnesia (OR 2.3; 95% CI 1.5–3.6), meningoencephalitis (OR 2.1; 95% CI 1.7–2.5), migraine (OR 1.7; 95% CI 1.5–1.8), intracerebral hemorrhage (OR 1.3; 95% CI 1.1–1.5), and ischemic stroke (OR 1.2; 95% CI 1.1–1.3). In addition, female sex was strongly associated with Takotsubo (OR 5.1; 95% CI 4.9–5.4).
Conclusion
TCM appears to be associated with varying degrees with several acute neurological diseases besides subarachnoid hemorrhage.



Similar content being viewed by others
References
Maron BJ, Towbin JA, Thiene G, et al. Contemporary definitions and classification of the cardiomyopathies: an American Heart Association Scientific Statement from the Council on Clinical Cardiology, Heart Failure and Transplantation Committee; Quality of Care and Outcomes Research and Functional Genomics and Translational Biology Interdisciplinary Working Groups; and Council on Epidemiology and Prevention. Circulation. 2006;113:1807–16.
Samuels MA. The brain–heart connection. Circulation. 2007;116:77–84.
Lyon AR, Rees PS, Prasad S, Poole-Wilson PA, Harding SE. Stress (Takotsubo) cardiomyopathy—a novel pathophysiological hypothesis to explain catecholamine-induced acute myocardial stunning. Nat Clin Pract Cardiovasc Med. 2008;5:22–9.
Pelliccia F, Kaski JC, Crea F, Camici PG. Pathophysiology of Takotsubo syndrome. Circulation. 2017;135:2426–41.
Finsterer J, Wahbi K. CNS disease triggering Takotsubo stress cardiomyopathy. Int J Cardiol. 2014;177:322–9.
Santoro F, Carapelle E, Cieza Ortiz SI, et al. Potential links between neurological disease and Tako-Tsubo cardiomyopathy: a literature review. Int J Cardiol. 2013;168:688–91.
Porto I, Della Bona R, Leo A, et al. Stress cardiomyopathy (Tako-Tsubo) triggered by nervous system diseases: a systematic review of the reported cases. Int J Cardiol. 2013;167:2441–8.
Pant S, Deshmukh A, Mehta K, et al. Burden of arrhythmias in patients with Takotsubo cardiomyopathy (apical ballooning syndrome). Int J Cardiol. 2013;170:64–8.
Yaguchi M, Yaguchi H, Takahashi N. A case of asymptomatic Takotsubo cardiomyopathy with intraventricular thrombus associated with epileptic seizure. Brain Nerve. 2011;63:897–900.
Stöllberger C, Huber JO, Enzelsberger B, Finsterer J. Fatal outcome of epileptic seizure-induced Takotsubo syndrome with left ventricular rupture. Eur J Neurol. 2009;16:e116–7.
Bybee KA, Kara T, Prasad A, et al. Systematic review: transient left ventricular apical ballooning: a syndrome that mimics ST-segment elevation myocardial infarction. Ann Intern Med. 2004;141:858–65.
Brinjikji W, El-Sayed AM, Salka S. In-hospital mortality among patients with Takotsubo cardiomyopathy: a study of the National Inpatient Sample 2008 to 2009. Am Heart J. 2012;164:215–21.
Elixhauser A, Steiner C, Harris DR, Coffey RM. Comorbidity measures for use with administrative data. Med Care. 1998;36:8–27.
Austin SR, Wong YN, Uzzo RG, Beck JR, Egleston BL. Why summary comorbidity measures such as the Charlson Comorbidity Index and Elixhauser score work. Med Care. 2015;53:e65–72.
Deshmukh A, Kumar G, Pant S, Rihal C, Murugiah K, Mehta JL. Prevalence of Takotsubo cardiomyopathy in the United States. Am Heart J. 2012;164(66–71):e1.
El-Sayed AM, Brinjikji W, Salka S. Demographic and co-morbid predictors of stress (Takotsubo) cardiomyopathy. Am J Cardiol. 2012;110:1368–72.
Khera R, Light-McGroary K, Zahr F, Horwitz PA, Girotra S. Trends in hospitalization for Takotsubo cardiomyopathy in the United States. Am Heart J. 2016;172:53–63.
Davies KR, Gelb AW, Manninen PH, Boughner DR, Bisnaire D. Cardiac function in aneurysmal subarachnoid haemorrhage: a study of electrocardiographic and echocardiographic abnormalities. Br J Anaesth. 1991;67:58–63.
Mayer SA, Lin J, Homma S, et al. Myocardial injury and left ventricular performance after subarachnoid hemorrhage. Stroke. 1999;30:780–6.
Parekh N, Venkatesh B, Cross D, et al. Cardiac troponin I predicts myocardial dysfunction in aneurysmal subarachnoid hemorrhage. J Am Coll Cardiol. 2000;36:1328–35.
Banki N, Kopelnik A, Tung P, et al. Prospective analysis of prevalence, distribution, and rate of recovery of left ventricular systolic dysfunction in patients with subarachnoid hemorrhage. J Neurosurg. 2006;105:15–20.
Lee VH, Connolly HM, Fulgham JR, Manno EM, Brown RD, Wijdicks EF. Tako-tsubo cardiomyopathy in aneurysmal subarachnoid hemorrhage: an underappreciated ventricular dysfunction. J Neurosurg. 2006;105:264–70.
Schneider F, Kadel C, Pagitz M, Sen S. Takotsubo cardiomyopathy and elevated troponin levels following cerebral seizure. Int J Cardiol. 2010;145:586–7.
Chin PS, Branch KR, Becker KJ. Postictal neurogenic stunned myocardium. Neurology. 2005;64:1977–8.
Hocker S, Prasad A, Rabinstein AA. Cardiac injury in refractory status epilepticus. Epilepsia. 2013;54:518–22.
Belcour D, Jabot J, Grard B, et al. Prevalence and risk factors of stress cardiomyopathy after convulsive status epilepticus in ICU patients. Crit Care Med. 2015;43:2164–70.
Bobinger T, Köhrmann M, Raaz-Schrauder D, Schwab S, Kallmünzer B. Lost memories can break your heart: a case report of transient global amnesia followed by takotsubo cardiomyopathy. Clin Res Cardiol. 2013;102:693–6.
Quick S, Speiser U, Richter N, et al. Transient global amnesia and broken heart syndrome: two faces of one pathology. Clin Auton Res. 2015;25:189–91.
Pantoni L, Bertini E, Lamassa M, Pracucci G, Inzitari D. Clinical features, risk factors, and prognosis in transient global amnesia: a follow-up study. Eur J Neurol. 2005;12:350–6.
Summers MR, Lennon RJ, Prasad A. Pre-morbid psychiatric and cardiovascular diseases in apical ballooning syndrome (tako-tsubo/stress-induced cardiomyopathy): potential pre-disposing factors? J Am Coll Cardiol. 2010;55:700–1.
Quinette P, Guillery-Girard B, Dayan J, et al. What does transient global amnesia really mean? Review of the literature and thorough study of 142 cases. Brain. 2006;129:1640–58.
Templin C, Ghadri JR, Diekmann J, et al. Clinical features and outcomes of Takotsubo (stress) cardiomyopathy. N Engl J Med. 2015;373:929–38.
Bartsch T, Deuschl G. Transient global amnesia: functional anatomy and clinical implications. Lancet Neurol. 2010;9:205–14.
Wittstein IS, Thiemann DR, Lima JA, et al. Neurohumoral features of myocardial stunning due to sudden emotional stress. N Engl J Med. 2005;352:539–48.
Nasr DM, Tomasini S, Prasad A, Rabinstein AA. Acute brain diseases as triggers for stress cardiomyopathy: clinical characteristics and outcomes. Neurocrit Care. 2017. https://doi.org/10.1007/s12028-017-0412-9.
Jung JM, Kim JG, Kim JB, et al. Takotsubo-like myocardial dysfunction in ischemic stroke: a hospital-based registry and systematic literature review. Stroke. 2016;47:2729–36.
Krause T, Werner K, Fiebach JB, et al. Stroke in right dorsal anterior insular cortex is related to myocardial injury. Ann Neurol. 2017;81:502–11.
Templin C, Napp LC, Ghadri JR. Takotsubo syndrome: underdiagnosed, underestimated, but understood? J Am Coll Cardiol. 2016;67:1937–40.
Madhavan M, Prasad A. Proposed Mayo Clinic criteria for the diagnosis of Tako-Tsubo cardiomyopathy and long-term prognosis. Herz. 2010;35:240–3.
Boland TA, Lee VH, Bleck TP. Stress-induced cardiomyopathy. Crit Care Med. 2015;43:686–93.
Funding
Financial support for this study was provided by Grant K23NS082367 (Dr. Kamel) from the National Institute of Neurological Disorders and Stroke and a grant from the Michael Goldberg Stroke Research Fund (Dr. Kamel).
Author information
Authors and Affiliations
Contributions
NAM conceived and designed the study, interpreted the data, drafted the article and revised it for important intellectual content, and gave final approval of the version to be published. AC acquired, analyzed, and interpreted the data, revised the article for important intellectual content, and gave final approval of the version to be published. OLA acquired the data, revised the article critically for important intellectual content, and gave final approval of the version to be published. MC acquired and analyzed the data, revised the article critically for important intellectual content, and gave final approval of the version to be published. AEM conceived and designed the study, interpreted the data, revised the article for important intellectual content, and gave final approval of the version to be published. SBM conceived and designed the study, interpreted the data, revised the article for important intellectual content, and gave final approval of the version to be published. HK conceived and designed the study, interpreted the data, revised the article for important intellectual content, and gave final approval of the version to be published.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to report.
Rights and permissions
About this article
Cite this article
Morris, N.A., Chatterjee, A., Adejumo, O.L. et al. The Risk of Takotsubo Cardiomyopathy in Acute Neurological Disease. Neurocrit Care 30, 171–176 (2019). https://doi.org/10.1007/s12028-018-0591-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-018-0591-z