Abstract
Purpose
Currently available randomized trial evidence has shown no reductions in type 2 diabetes (T2D) complications important to patients with tight glycemic control. Yet, economic analyses consistently find tight glycemic control to be cost-effective. To understand this apparent paradox, we systematically identified and appraised economic analyses of tight glycemic control for T2D.
Methods
We searched multiple databases from January 2016 to January 2018 for cost-effectiveness or cost-utility analyses of any glucose-lowering treatments for adults with T2D using simulations with long—40 years to lifetime—time horizons. Reviewers selected and appraised each study independently and in duplicate with good reproducibility.
Results
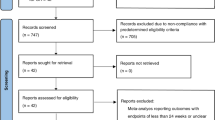
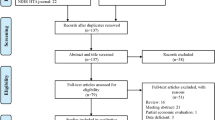
We found 30 analyses, most comparing the glycemic impact of glucose-lowering drugs and applying their impact on HbA1c to model (most commonly IMS CORE or Cardiff T2DM) their impact on the incidence of diabetes-related complication. Models drew from observational evidence of the correlation of HbA1c levels and diabetes-related complication rates; none used estimates of the effect of lowering HbA1c on these outcomes from systematic reviews of randomized trials. Sensitivity analyses, when conducted, demonstrate substantial loss of cost-effectiveness as simulations approach the results seen in these trials.
Conclusions
Reliance on the association between glycemic control and diabetes-related complications evident in observational studies but not apparent in randomized trial bias the estimates of the cost-effectiveness of interventions to improve glycemic control.

Similar content being viewed by others
Availability of data and material
At request.
References
International Diabetes Federation IDF Diabetes Atlas (2017), http://www.diabetesatlas.org
Economic Costs of Diabetes in the U.S. in 2017. Diabetes Care 41(5):917–928 (2018)
S.E. Nissen, K. Wolski, Effect of rosiglitazone on the risk of myocardial infarction and death from cardiovascular causes. N. Engl. J Med. 356(24), 2457–2471 (2007)
T.A. Zelniker, S.D. Wiviott, I. Raz, K. Im, E.L. Goodrich, M.P. Bonaca et al. SGLT2 inhibitors for primary and secondary prevention of cardiovascular and renal outcomes in type 2 diabetes: a systematic review and meta-analysis of cardiovascular outcome trials. Lancet 393(10166), 31–39 (2019)
M.A. Bethel, R.A. Patel, P. Merrill, Y. Lokhnygina, J.B. Buse, R.J. Mentz et al. Cardiovascular outcomes with glucagon-like peptide-1 receptor agonists in patients with type 2 diabetes: a meta-analysis. Lancet Diabetes Endocrinol. 6(2), 105–113 (2018)
A.J. Palmer, P. Clarke, A. Gray, J. Leal, A. Lloyd, D. Grant et al. Computer modeling of diabetes and its complications: a report on the Fifth Mount Hood challenge meeting. Value Health 16(4), 670–685 (2013)
Computer modeling of diabetes and its complications: a report on the Fourth Mount Hood Challenge Meeting. Diabetes Care 30(6):1638–1646 (2007)
D. Moher, A. Liberati, J. Tetzlaff, D.G. Altman, Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. J. Clin. Epidemiol. 62(10), 1006–1012 (2009)
M.F. Drummond, M.J. Sculpher, G.W. Torrance, B.J. O’Brien, G.L. Stoddart. Methods for the Economic Evaluation of Health Care Programme. 3rd edn. (Oxford University Press, Oxford, 2005)
R. Rodriguez-Gutierrez, V.M. Montori, Glycemic control for patients with type 2 diabetes mellitus: our evolving faith in the face of evidence. Circul. Cardiovasc. Qual. Outcomes 9(5), 504–512 (2016)
J.C. Davis, M.C. Robertson, M.C. Ashe, T. Liu-Ambrose, K.M. Khan, C.A. Marra, Does a home-based strength and balance programme in people aged > or =80 years provide the best value for money to prevent falls? A systematic review of economic evaluations of falls prevention interventions. Br. J. Sports Med. 44(2), 80–89 (2010)
C.F. Chiou, J.W. Hay, J.F. Wallace, B.S. Bloom, P.J. Neumann, S.D. Sullivan et al. Development and validation of a grading system for the quality of cost-effectiveness studies. Med. Care 41(1), 32–44 (2003)
J.J. Ofman, S.D. Sullivan, P.J. Neumann, C.F. Chiou, J.M. Henning, S.W. Wade et al. Examining the value and quality of health economic analyses: implications of utilizing the QHES. J. Managed Care Pharm. 9(1), 53–61 (2003)
S.E. Rutstein, J.T. Price, N.E. Rosenberg, S.M. Rennie, A.K. Biddle, W.C. Miller, Hidden costs: the ethics of cost-effectiveness analyses for health interventions in resource-limited settings. Glob Public Health 12(10), 1269–1281 (2017)
I. Dhaliwal, E. Duflo, R. Glennerster, C. Tulloch, Comparative cost-effectiveness analysis to inform policy in developing countries: a general framework with applications for education. In P. Glewwe (ed) Education Policy in Developing Countries, pp 285–341 (University of Chicago Press, 2013) http://hdl.handle.net/1721.1/116111
H.G. Eichler, S.X. Kong, W.C. Gerth, P. Mavros, B. Jonsson, Use of cost-effectiveness analysis in health-care resource allocation decision-making: how are cost-effectiveness thresholds expected to emerge?. Value Health 7(5), 518–528 (2004).
D.T. Jamison, J.G. Breman, A.R. Measham, G. Alleyne, M. Claeson, D.B. Evans, et al. editors. in Priorities in Health. (The International Bank for Reconstruction and Development/The World Bank, Washington (DC), 2006)
I. Williams, S. McIver, D. Moore, S. Bryan, The use of economic evaluations in NHS decision-making: a review and empirical investigation. HealthTechnol Assess 12(7), iii–175 (2008). https://doi.org/10.3310/hta12070
J. Rosenstock, S.E. Kahn, O.E. Johansen, B. Zinman, M.A. Espeland, H.J. Woerle, et al. Effect of linagliptin vs glimepiride on major adverse cardiovascular outcomes in patients with type 2 diabetes: the CAROLINA randomized clinical trial. JAMA 322(12), 1155–1166 (2019). https://doi.org/10.1001/jama.2019.13772
B.M. Scirica, D.L. Bhatt, E. Braunwald, P.G. Steg, J. Davidson, B. Hirshberg et al. Saxagliptin and cardiovascular outcomes in patients with type 2 diabetes mellitus. N. Engl. J. Med. 369(14), 1317–1326 (2013)
J.B. Green, M.A. Bethel, P.W. Armstrong, J.B. Buse, S.S. Engel, J. Garg et al. Effect of sitagliptin on cardiovascular outcomes in type 2 diabetes. N. Engl. J. Med. 373(3), 232–242 (2015)
S.P. Marso, G.H. Daniels, K. Brown-Frandsen, P. Kristensen, J.F. Mann, M.A. Nauck et al. Liraglutide and cardiovascular outcomes in type 2 diabetes. N. Engl. J. Med. 375(4), 311–322 (2016)
B. Zinman, C. Wanner, J.M. Lachin, D. Fitchett, E. Bluhmki, S. Hantel et al. Empagliflozin, cardiovascular outcomes, and mortality in type 2 diabetes. N. Engl. J. Med. 373(22), 2117–2128 (2015)
S.P. Marso, S.C. Bain, A. Consoli, F.G. Eliaschewitz, E. Jodar, L.A. Leiter et al. Semaglutide and cardiovascular outcomes in patients with type 2 diabetes. N. Engl. J. Med. 375(19), 1834–1844 (2016)
Centers for Disease Control and Prevention. National Diabetes Statistics Report, 2020. (Centers for Disease Control and Prevention, U.S. Dept of Health and Human Services, Atlanta, GA, 2020)
R. G. McCoy. et al. Hospital readmissions among commercially insured and medicare advantage beneficiaries with diabetes and the impact of severe hypoglycemic and hyperglycemic events. J. Gen. Intern. Med. 32, 1097–1105 (2017). https://doi.org/10.1007/s11606-017-4095-x
H. Shao, S. Zhai, D. Zou, M.U. Mir, N.K. Zawadzki, Q. Shi et al. Cost-effectiveness analysis of dapagliflozin versus glimepiride as monotherapy in a Chinese population with type 2 diabetes mellitus. Curr. Med. Res. Opin. 33(2), 359–369 (2017)
S. Sabapathy, C. Neslusan, K. Yoong, A. Teschemaker, P. Johansen, M. Willis, Cost-effectiveness of canagliflozin versus sitagliptin when added to metformin and sulfonylurea in type 2 diabetes in Canada. J. Popul. Ther. Clin. Pharmacol. 23(2), e151–e168 (2016)
L.H. Chuang, B.G. Verheggen, M. Charokopou, D. Gibson, S. Grandy, B. Kartman, Cost-effectiveness analysis of exenatide once-weekly versus dulaglutide, liraglutide, and lixisenatide for the treatment of type 2 diabetes mellitus: an analysis from the UK NHS perspective. J. Med. Econ. 19(12), 1127–1134 (2016)
D. Bruhn, A.A. Martin, R. Tavares, B. Hunt, R.F. Pollock, Cost-utility of albiglutide versus insulin lispro, insulin glargine, and sitagliptin for the treatment of type 2 diabetes in the US. J. Med. Econ. 19(7), 672–683 (2016)
C. Tzanetakos, A. Bargiota, G. Kourlaba, G. Gourzoulidis, N. Maniadakis, Cost effectiveness of exenatide once weekly versus insulin glargine and liraglutide for the treatment of type 2 diabetes mellitus in Greece. Clin. Drug. Investig. 38(1), 67–77 (2018)
B. Hunt, N. Kragh, C.C. McConnachie, W.J. Valentine, M.C. Rossi, R. Montagnoli, Long-term cost-effectiveness of two glp-1 receptor agonists for the treatment of type 2 diabetes mellitus in the italian setting: liraglutide versus lixisenatide. Clin. Ther. 39(7), 1347–1359 (2017)
M. Kvapil, M. Prazny, P. Holik, K. Rychna, B. Hunt, Cost-effectiveness of IDegLira versus insulin intensification regimens for the treatment of adults with type 2 diabetes in the Czech Republic. Diabetes Ther. 8(6), 1331–1347 (2017)
S. Gu, X. Wang, Q. Qiao, W. Gao, J. Wang, H. Dong, Cost-effectiveness of exenatide twice daily vs insulin glargine as add-on therapy to oral antidiabetic agents in patients with type 2 diabetes in China. Diabetes, Obes. Metab. 19(12), 1688–1697 (2017)
M.J. Davies, D. Glah, B. Chubb, G. Konidaris, P. McEwan, Cost effectiveness of IDegLira vs. alternative basal insulin intensification therapies in patients with type 2 diabetes mellitus uncontrolled on basal insulin in a UK setting. PharmacoEconomics. 34(9), 953–966 (2016)
T. Dilla, D. Alexiou, I. Chatzitheofilou, R. Ayyub, J. Lowin, K. Norrbacka, The cost-effectiveness of dulaglutide versus liraglutide for the treatment of type 2 diabetes mellitus in Spain in patients with BMI >/= 30 kg/m(2). J. Med. Econ. 20(5), 443–452 (2017)
H. Kousoulakou, M. Hatzikou, V. Baroutsou, J. Yfantopoulos, Cost effectiveness of vildagliptin versus glimepiride as add-on treatment to metformin for the treatment of diabetes mellitus type 2 patients in Greece. Cost Eff. Resour Alloc. 15, 19 (2017)
U. Permsuwan, K. Thavorn, P. Dilokthornsakul, S. Saokaew, N. Chaiyakunapruk, Cost-effectiveness of insulin detemir versus insulin glargine for Thai type 2 diabetes from a payer’s perspective. J. Med. Econ. 20(9), 991–999 (2017)
B. Hunt, D. Glah, M. van der Vliet, Modeling the long-term cost-effectiveness of ideglira in patients with type 2 diabetes who are failing to meet glycemic targets on basal insulin alone in The Netherlands. Diabetes Ther. 8(4), 753–765 (2017)
X. Zhang, S. Liu, Y. Li, Y. Wang, M. Tian, G. Liu, Long-term effectiveness and cost-effectiveness of metformin combined with liraglutide or exenatide for type 2 diabetes mellitus based on the CORE diabetes model study. PLoS ONE 11(6), e0156393 (2016)
S. Gu, Y. Mu, S. Zhai, Y. Zeng, X. Zhen, H. Dong, Cost-effectiveness of dapagliflozin versus acarbose as a monotherapy in type 2 diabetes in China. PloS ONE 11(11), e0165629 (2016)
J. Gordon, P. McEwan, U. Sabale, B. Kartman, B.H. Wolffenbuttel, The cost-effectiveness of exenatide twice daily (BID) vs insulin lispro three times daily (TID) as add-on therapy to titrated insulin glargine in patients with type 2 diabetes. J. Med. Econ. 19(12), 1167–1174 (2016)
S. Roze, E. Duteil, J. Smith-Palmer, S. de Portu, W. Valentine, B.F. de Brouwer et al. Cost-effectiveness of continuous subcutaneous insulin infusion in people with type 2 diabetes in the Netherlands. J. Med. Econ. 19(8), 742–749 (2016)
B. Hunt, M. Mocarski, W.J. Valentine, J. Langer, Evaluation of the long-term cost-effectiveness of IDegLira versus liraglutide added to basal insulin for patients with type 2 diabetes failing to achieve glycemic control on basal insulin in the USA. J. Med. Econ. 20(7), 663–670 (2017)
B. Hunt, M. Mocarski, W.J. Valentine, J. Langer, IDegLira versus insulin glargine U100: a long-term cost-effectiveness analysis in the US setting. Diabetes Ther. 8(3), 531–544 (2017)
G. Vega-Hernandez, R. Wojcik, M. Schlueter, Cost-effectiveness of liraglutide versus dapagliflozin for the treatment of patients with type 2 diabetes mellitus in the UK. Diabetes Ther. 8(3), 513–530 (2017)
C. Tzanetakos, N. Tentolouris, G. Kourlaba, N. Maniadakis, Cost-effectiveness of dapagliflozin as add-on to metformin for the treatment of type 2 diabetes mellitus in Greece. Clin. Drug Investig. 36(8), 649–659 (2016)
B. Hunt, G. Vega-Hernandez, W.J. Valentine, N. Kragh, Evaluation of the long-term cost-effectiveness of liraglutide vs lixisenatide for treatment of type 2 diabetes mellitus in the UK setting. Diabetes, Obes. Metab. 19(6), 842–849 (2017)
R. Roussel, L. Martinez, T. Vandebrouck, H. Douik, P. Emiel, M. Guery et al. Evaluation of the long-term cost-effectiveness of liraglutide therapy for patients with type 2 diabetes in France. J. Med. Econ. 19(2), 121–134 (2016)
P. Mezquita-Raya, A. Ramirez de Arellano, N. Kragh, G. Vega-Hernandez, J. Pohlmann, W.J. Valentine, et al. Liraglutide versus lixisenatide: long-term cost-effectiveness of GLP-1 receptor agonist therapy for the treatment of type 2 diabetes in Spain. Diabetes Ther. 8(2), 401–415 (2017). https://doi.org/10.1007/s13300-017-0239-6
A. Ericsson, A. Lundqvist, Cost effectiveness of insulin degludec plus liraglutide (IDegLira) in a fixed combination for uncontrolled type 2 diabetes mellitus in Sweden. Appl. Health Econ. Health Policy 15(2), 237–248 (2017)
U. Permsuwan, N. Chaiyakunapruk, P. Dilokthornsakul, K. Thavorn, S. Saokaew, Long-term cost-effectiveness of insulin glargine versus neutral protamine hagedorn insulin for type 2 diabetes in Thailand. Appl. Health Econ. Health Policy 14(3), 281–292 (2016)
J. Sánchez-Covisa, J. Franch, D. Mauricio, N. López-Martínez, L.-H. Chuang, M. Capel, Análisis de coste-efectividad de saxagliptina como tratamiento triple oral (con metformina y una sulfonilurea) en el manejo de la diabetes tipo 2 en España. PharmacoEconomics 13(1), 25–35 (2015)
J. Gordon, P. McEwan, M. Hurst, J. Puelles, The cost-effectiveness of alogliptin versus sulfonylurea as add-on therapy to metformin in patients with uncontrolled type 2 diabetes mellitus. Diabetes Ther. 7(4), 825–845 (2016)
S. Gu, Y. Zeng, D. Yu, X. Hu, H. Dong, Cost-effectiveness of saxagliptin versus acarbose as second-line therapy in type 2 diabetes in China. PLoS ONE 11(11), e0167190 (2016)
U. Permsuwan, P. Dilokthornsakul, S. Saokaew, K. Thavorn, N. Chaiyakunapruk, Cost-effectiveness of dipeptidyl peptidase-4 inhibitor monotherapy in elderly type 2 diabetes patients in Thailand. Clin. Econ. Outcomes Res. 8, 521–529 (2016)
Yahoo. Currency Converter Yahoo Finance Web Site (2018), https://finance.yahoo.com/currency-converter/-
Author information
Authors and Affiliations
Contributions
F.J.B.: conceptualization, methodology, formal analysis, investigation, data curation, writing—original draft, visualization. F.J.K.T.: formal analysis, investigation, data curation. O.J.P.: formal analysis, visualization, writing—review and editing. J.A.Z-H.: formal analysis, data curation, visualization. L.J.P.: software, resources. N.D.S.: methodology, validation, writing—review and editing, visualization. G.G.: methodology, validation, writing—review and editing, visualization. R.R-G.: conceptualization, methodology, validation, visualization, writing—review and editing, supervision, project administration. V.M.M.: conceptualization, methodology, validation, visualization, writing—review and editing, supervision, project administration.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Barrera, F.J., Toloza, F.J., Ponce, O.J. et al. The validity of cost-effectiveness analyses of tight glycemic control. A systematic survey of economic evaluations of pharmacological interventions in patients with type 2 diabetes. Endocrine 71, 47–58 (2021). https://doi.org/10.1007/s12020-020-02489-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-020-02489-w