Abstract
The conventional management strategies of myocardial infarction (MI) are effective to sustain life; however, myocardial regeneration has not been achieved owing to the inherently poor regenerative capacity of the native myocardium. Stem cell-based therapies are promising; however, lineage specificity and undesired differentiation profile are challenging. Herein, we focused on the epicardial fat (EF) as an ideal source for mesenchymal stem cells (MSCs) owing to the proximity and same microvasculature with cardiac muscle. Unfortunately, the epicardial adipose tissue derived stem cells (EATDS) remain understudied regarding their phenotype heterogeneity and cardiac regeneration potential. As EF closely reflects the cardiac pathology during ischemia, the present study aims to determine the EATDS subpopulations under simulated ischemic and reperfused conditions employing single cell RNA sequencing (scRNAseq). EATDS were isolated from three hyperlipidemic Yucatan microswine and were divided into Control, Ischemia (ISC), and Ischemia/reperfusion (ISC/R). The scRNAseq analysis was performed using 10 genomics platform which revealed 18 unique cell clusters suggesting the existence of heterogeneous phenotypes. The upregulated genes were taken into consideration and subsequent functional assessment revealed the cardioprotective phenotypes with diverse mechanisms including epigenetic regulation (Cluster 1), myocardial homeostasis (Cluster 1), cell integrity and cell cycle (Clusters 2 and 3), prevention of fibroblast differentiation (Cluster 4), differentiation to myocardial lineage (Cluster 6), anti-inflammatory responses (Clusters 5, 8, and 11), prevention of ER-stress (Cluster 9), and increasing the energy metabolism (Cluster 10). These unique phenotypes of heterogeneous EATDS population open significant translational opportunities for myocardial regeneration and cardiac management.
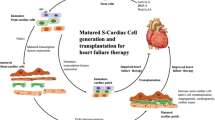
Graphical abstract












Similar content being viewed by others
Data Availability
Data with the raw counts matrices and annotation are available upon request from the authors through proper channels.
Code Availability
NA.
References
Joo, H. J., Kim, J.-H., & Hong, S. J. (2017). Adipose tissue-derived stem cells for myocardial regeneration. Korean Circulation Journal, 47(2), 151–159. https://doi.org/10.4070/kcj.2016.0207.
Thankam, F. G., & Agrawal, D. K. (2020). Infarct zone: A novel platform for exosome trade in cardiac tissue regeneration. Journal of Cardiovascular Translational Research. https://doi.org/10.1007/s12265-019-09952-8.
Lambert, C., Arderiu, G., Bejar, M. T., Crespo, J., Baldellou, M., Juan-Babot, O., & Badimon, L. (2019). Stem cells from human cardiac adipose tissue depots show different gene expression and functional capacities. Stem Cell Research & Therapy, 10(1), 361. https://doi.org/10.1186/s13287-019-1460-1.
Kim, J.-H., Hong, S. J., Park, C.-Y., Park, J. H., Choi, S.-C., Woo, S.-K., … Lim, D.-S. (2016). Intramyocardial adipose-derived stem cell transplantation increases pericardial fat with recovery of myocardial function after acute myocardial infarction. PLoS ONE, 11(6), e0158067. https://doi.org/10.1371/journal.pone.0158067.
Mayfield, A. E., Tilokee, E. L., & Davis, D. R. (2014). Resident cardiac stem cells and their role in stem cell therapies for myocardial repair. Canadian Journal of Cardiology, 30(11), 1288–1298. https://doi.org/10.1016/j.cjca.2014.03.018.
Wu, Y., Zhang, A., Hamilton, D. J., & Deng, T. (2017). Epicardial fat in the maintenance of cardiovascular health. Methodist DeBakey Cardiovascular Journal, 13(1), 20–24. https://doi.org/10.14797/mdcj-13-1-20.
Ege, M. R. (2020). Epicardial adipose tissue: Good or bad for cardiac function? Herz, 45(3), 299–299. https://doi.org/10.1007/s00059-018-4731-1.
Gui, C., Parson, J., & Meyer, G. A. (2021). Harnessing adipose stem cell diversity in regenerative medicine. APL Bioengineering, 5(2), 021501. https://doi.org/10.1063/5.0038101.
Hou, W., Duan, L., Huang, C., Li, X., Xu, X., Qin, P., … Jin, W. (2021). Mesenchymal stem cell subpopulations and their heterogeneity of response to inductions revealed by single-cell RNA-seq. bioRxiv, 2021.05.07.443197. https://doi.org/10.1101/2021.05.07.443197.
Thankam, F. G., Ayoub, J. G., Ahmed, M. M. R., Siddique, A., Sanchez, T. C., Peralta, R. A., … Agrawal, D. K. (2020). Association of hypoxia and mitochondrial damage associated molecular patterns in the pathogenesis of vein graft failure: A pilot study. Translational Research. https://doi.org/10.1016/j.trsl.2020.08.010.
Thankam, F. G., Chandra, I. S., Kovilam, A. N., Diaz, C. G., Volberding, B. T., Dilisio, M. F., … Agrawal, D. K. (2018). Amplification of mitochondrial activity in the healing response following rotator cuff tendon injury. Scientific Reports, 8(1), 1–14. https://doi.org/10.1038/s41598-018-35391-7.
Farbehi, N., Patrick, R., Dorison, A., Xaymardan, M., Janbandhu, V., Wystub-Lis, K., … Harvey, R. P. (n.d.). Single-cell expression profiling reveals dynamic flux of cardiac stromal, vascular and immune cells in health and injury. eLife, 8. https://doi.org/10.7554/eLife.43882.
Wolmarans, E., Mellet, J., Durandt, C., Joubert, F., & Pepper, M. S. (2021). Single-cell transcriptome analysis of human adipose-derived stromal cells identifies a contractile cell subpopulation. Stem Cells International, 2021, e5595172. https://doi.org/10.1155/2021/5595172.
Wang, W., Gao, D., & Wang, X. (2018). Can single-cell RNA sequencing crack the mystery of cells? Cell Biology and Toxicology, 34(1), 1–6. https://doi.org/10.1007/s10565-017-9404-y.
Nurzynska, D., Di Meglio, F., Romano, V., Miraglia, R., Sacco, A. M., Latino, F., … Castaldo, C. (2012). Cardiac primitive cells become committed to a cardiac fate in adult human heart with chronic ischemic disease but fail to acquire mature phenotype: Genetic and phenotypic study. Basic Research in Cardiology, 108(1), 320. https://doi.org/10.1007/s00395-012-0320-2.
Urbanek, K., Torella, D., Sheikh, F., De Angelis, A., Nurzynska, D., Silvestri, F., … Anversa, P. (2005). Myocardial regeneration by activation of multipotent cardiac stem cells in ischemic heart failure. Proceedings of the National Academy of Sciences of the United States of America, 102(24), 8692–8697. https://doi.org/10.1073/pnas.0500169102.
Sebastião, M. J., Serra, M., Pereira, R., Palacios, I., Gomes-Alves, P., & Alves, P. M. (2019). Human cardiac progenitor cell activation and regeneration mechanisms: Exploring a novel myocardial ischemia/reperfusion in vitro model. Stem Cell Research & Therapy, 10(1), 77. https://doi.org/10.1186/s13287-019-1174-4.
Docshin, P. M., Karpov, A. A., Eyvazova, Sh. D., Puzanov, M. V., Kostareva, A. A., Galagudza, M. M., & Malashicheva, A. B. (2018). Activation of cardiac stem cells in myocardial infarction. Cell and Tissue Biology, 12(3), 175–182. https://doi.org/10.1134/S1990519X18030045.
Yang, W., Zhang, S., Ou, T., Jiang, H., Jia, D., Qi, Z., … Ge, J. (2020). Interleukin-11 regulates the fate of adipose-derived mesenchymal stem cells via STAT3 signalling pathways. Cell Proliferation, 53(5), e12771. https://doi.org/10.1111/cpr.12771.
Okada, T., & Suzuki, H. (2021). The role of tenascin-C in tissue injury and repair after stroke. Frontiers in Immunology, 11, 3553. https://doi.org/10.3389/fimmu.2020.607587.
Findley, A. S., Monziani, A., Richards, A. L., Rhodes, K., Ward, M. C., Kalita, C. A., & Luca, F. (2021). Functional dynamic genetic effects on gene regulation are specific to particular cell types and environmental conditions. eLife, 10, e67077. https://doi.org/10.7554/eLife.67077.
Verhelst, J., Hulpiau, P., & Saelens, X. (2013). Mx proteins: Antiviral gatekeepers that restrain the uninvited. Microbiology and Molecular Biology Reviews : MMBR, 77(4), 551–566. https://doi.org/10.1128/MMBR.00024-13.
Kavanagh, K. L., Jörnvall, H., Persson, B., & Oppermann, U. (2008). Medium- and short-chain dehydrogenase/reductase gene and protein families. Cellular and Molecular Life Sciences, 65(24), 3895. https://doi.org/10.1007/s00018-008-8588-y.
Jin, X., Chen, C., Li, D., Su, Q., Hang, Y., Zhang, P., & Hu, W. (2017). PRDX2 in myocyte hypertrophy and survival is mediated by TLR4 in acute infarcted myocardium. Scientific Reports, 7(1), 6970. https://doi.org/10.1038/s41598-017-06718-7.
Han, Y.-H., Jin, M.-H., Jin, Y.-H., Yu, N.-N., Liu, J., Zhang, Y.-Q., … Sun, H.-N. (2020). Deletion of peroxiredoxin II inhibits the growth of mouse primary mesenchymal stem cells through induction of the G0/G1 cell-cycle arrest and activation of AKT/GSK3β/β-catenin signaling. In Vivo, 34(1), 133–141. https://doi.org/10.21873/invivo.11754.
Di Liegro, C. M., Schiera, G., & Di Liegro, I. (2018). H1.0 linker histone as an epigenetic regulator of cell proliferation and differentiation. Genes, 9(6), 310. https://doi.org/10.3390/genes9060310.
Chen, E., Yang, L., Ye, C., Zhang, W., Ran, J., Xue, D., … Hu, Q. (2018). An asymmetric chitosan scaffold for tendon tissue engineering: In vitro and in vivo evaluation with rat tendon stem/progenitor cells. Acta Biomaterialia, 73, 377–387. https://doi.org/10.1016/j.actbio.2018.04.027.
Torres, C. M., Biran, A., Burney, M. J., Patel, H., Henser-Brownhill, T., Cohen, A.-H. S., … Scaffidi, P. (2016). The linker histone H1.0 generates epigenetic and functional intratumor heterogeneity. Science (New York, N.Y.), 353(6307), aaf1644. https://doi.org/10.1126/science.aaf1644.
Yao, J., Guihard, P. J., Blazquez-Medela, A. M., Guo, Y., Liu, T., Boström, K. I., & Yao, Y. (2016). Matrix Gla protein regulates differentiation of endothelial cells derived from mouse embryonic stem cells. Angiogenesis, 19(1), 1–7. https://doi.org/10.1007/s10456-015-9484-3.
Feng, Y., Liao, Y., Huang, W., Lai, X., Luo, J., Du, C., … Zhang, Q. (2018). Mesenchymal stromal cells-derived matrix Gla protein contribute to the alleviation of experimental colitis. Cell Death & Disease, 9(6), 691. https://doi.org/10.1038/s41419-018-0734-3.
Wei, F.-F., Trenson, S., Monney, P., Yang, W.-Y., Pruijm, M., Zhang, Z.-Y., … Staessen, J. A. (2018). Epidemiological and histological findings implicate matrix Gla protein in diastolic left ventricular dysfunction. PLoS ONE, 13(3), e0193967. https://doi.org/10.1371/journal.pone.0193967.
Milliron, H. Y., Weiland, M. J., Kort, E. J., & Jovinge, S. (2019). Isolation of cardiomyocytes undergoing mitosis with complete cytokinesis. Circulation Research, 125(12), 1070–1086. https://doi.org/10.1161/CIRCRESAHA.119.314908.
Shoji, M., Ueda, M., Nishioka, M., Minato, H., Seki, M., Harada, K., … Kuzuhara, T. (2019). Jiadifenolide induces the expression of cellular communication network factor (CCN) genes, and CCN2 exhibits neurotrophic activity in neuronal precursor cells derived from human induced pluripotent stem cells. Biochemical and Biophysical Research Communications, 519(2), 309–315. https://doi.org/10.1016/j.bbrc.2019.09.003.
Li, H., Yao, Z., He, W., Gao, H., Bai, Y., Yang, S., … Luo, G. (2016). P311 induces the transdifferentiation of epidermal stem cells to myofibroblast-like cells by stimulating transforming growth factor β1 expression. Stem Cell Research & Therapy, 7, 175. https://doi.org/10.1186/s13287-016-0421-1.
Tan, J., Peng, X., Luo, G., Ma, B., Cao, C., He, W., … Wu, J. (2010). Investigating the role of P311 in the hypertrophic scar. PLoS ONE, 5(4), e9995. https://doi.org/10.1371/journal.pone.0009995.
Plaisance, I., Perruchoud, S., Fernandez-Tenorio, M., Gonzales, C., Ounzain, S., Ruchat, P., … Pedrazzini, T. (2016). Cardiomyocyte lineage specification in adult human cardiac precursor cells via modulation of enhancer-associated long noncoding RNA expression. JACC: Basic to Translational Science, 1(6), 472–493. https://doi.org/10.1016/j.jacbts.2016.06.008.
Wang, Y., Niu, Z., Guo, Y., Wang, L., Lin, F., & Zhang, J. (2017). IL-11 promotes the treatment efficacy of hematopoietic stem cell transplant therapy in aplastic anemia model mice through a NF-κB/microRNA-204/thrombopoietin regulatory axis. Experimental & Molecular Medicine, 49(12), e410–e410. https://doi.org/10.1038/emm.2017.217.
Tsujioka, H., Kunieda, T., Katou, Y., Shirahige, K., Fukazawa, T., & Kubo, T. (2017). interleukin-11 induces and maintains progenitors of different cell lineages during Xenopus tadpole tail regeneration. Nature Communications, 8(1), 495. https://doi.org/10.1038/s41467-017-00594-5.
Obana, M., Maeda, M., Takeda, K., Hayama, A., Mohri, T., Yamashita, T., … Fujio, Y. (2010). Therapeutic activation of signal transducer and activator of transcription 3 by interleukin-11 ameliorates cardiac fibrosis after myocardial infarction. Circulation, 121(5), 684–691. https://doi.org/10.1161/CIRCULATIONAHA.109.893677.
Graustein, A. D., Misch, E. A., Musvosvi, M., Shey, M., Shah, J. A., Seshadri, C., … Hawn, T. R. (2018). Toll-like receptor chaperone HSP90B1 and the immune response to Mycobacteria. PLoS ONE, 13(12), e0208940. https://doi.org/10.1371/journal.pone.0208940.
Ben Mkaddem, S., Pedruzzi, E., Werts, C., Coant, N., Bens, M., Cluzeaud, F., … Vandewalle, A. (2010). Heat shock protein gp96 and NAD(P)H oxidase 4 play key roles in Toll-like receptor 4-activated apoptosis during renal ischemia/reperfusion injury. Cell Death & Differentiation, 17(9), 1474–1485. https://doi.org/10.1038/cdd.2010.26.
Kern, P., Balzer, N. R., Bender, F., Frolov, A., Sowa, J.-P., Bonaguro, L., … Mass, E. (2020). Creld2 function during unfolded protein response is essential for liver metabolism homeostasis. bioRxiv, 2020.01.28.923136. https://doi.org/10.1101/2020.01.28.923136.
Kim, Y., Park, S.-J., Manson, S. R., Molina, C. A. F., Kidd, K., Thiessen-Philbrook, H., … Chen, Y. M. (n.d.). Elevated urinary CRELD2 is associated with endoplasmic reticulum stress–mediated kidney disease. JCI Insight, 2(23), e92896. https://doi.org/10.1172/jci.insight.92896.
Lim, K., Lim, K., Price, A., Orr, B., Eberhart, C., & Bar, E. (2014). Inhibition of monocarboxylate transporter-4 depletes stem-like glioblastoma cells and inhibits HIF transcriptional response in a lactate-independent manner. Oncogene, 33(35), 4433–4441. https://doi.org/10.1038/onc.2013.390.
Zhu, Y., Wu, J., & Yuan, S.-Y. (2013). MCT1 and MCT4 expression during myocardial ischemic-reperfusion injury in the isolated rat heart. Cellular Physiology and Biochemistry: International Journal of Experimental Cellular Physiology, Biochemistry, and Pharmacology, 32(3), 663–674. https://doi.org/10.1159/000354470.
Pang, Z., Junkins, R. D., Raudonis, R., MacNeil, A. J., McCormick, C., Cheng, Z., & Lin, T.-J. (2018). Regulator of calcineurin 1 differentially regulates TLR-dependent MyD88 and TRIF signaling pathways. PLoS ONE, 13(5), e0197491. https://doi.org/10.1371/journal.pone.0197491.
Corbalan, J. J., & Kitsis, R. N. (2018). RCAN1–calcineurin axis and the set-point for myocardial damage during ischemia-reperfusion. Circulation Research, 122(6), 796–798. https://doi.org/10.1161/CIRCRESAHA.118.312787.
Sobrado, M., Ramirez, B. G., Neria, F., Lizasoain, I., Arbones, M. L., Minami, T., … Cano, E. (2012). Regulator of calcineurin 1 (Rcan1) has a protective role in brain ischemia/reperfusion injury. Journal of Neuroinflammation, 9(1), 48. https://doi.org/10.1186/1742-2094-9-48.
Hesse, J., Owenier, C., Lautwein, T., Zalfen, R., Weber, J. F., Ding, Z., … Schrader, J. (2021). Single-cell transcriptomics defines heterogeneity of epicardial cells and fibroblasts within the infarcted murine heart. eLife, 10, e65921. https://doi.org/10.7554/eLife.65921.
Cui, Y., Zheng, Y., Liu, X., Yan, L., Fan, X., Yong, J., … Tang, F. (2019). Single-cell transcriptome analysis maps the developmental track of the human heart. Cell Reports, 26(7), 1934-1950.e5. https://doi.org/10.1016/j.celrep.2019.01.079.
Ruiz-Villalba, A., Romero, J. P., Hernández, S. C., Vilas-Zornoza, A., Fortelny, N., Castro-Labrador, L., … Prósper, F. (2020). Single-cell rna sequencing analysis reveals a crucial role for CTHRC1 (collagen triple helix repeat containing 1) cardiac fibroblasts after myocardial infarction. Circulation, 142(19), 1831–1847. https://doi.org/10.1161/CIRCULATIONAHA.119.044557.
Acknowledgements
Authors are grateful to Dr. Hung Long, SC2 Core—Children Hospital Los Angeles, and Dr Anja Bastin and Dr. Elizabeth Collins, 10x genomics, for their technical support in multiple aspects of scRNAseq analysis.
Funding
The research work of FT is supported by the startup funds from WU and DK Agrawal is supported by research grants R01 HL144125 and R01HL147662 from the National Institutes of Health, USA. The content of this original article is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Author information
Authors and Affiliations
Contributions
FT – conceptualization, experiments, data generation and analysis, manuscript preparation, and manuscript edits. DK—conceptualization, data generation and analysis, manuscript preparation, and manuscript edits.
Corresponding author
Ethics declarations
Ethics Approval and Consent to Participate
NA.
Consent for Publication
Both the authors have read the manuscript and agreed to publish in CMLS.
Conflict of Interest
All the authors have read the manuscript and declare no conflict of interest.
Competing Interests
The authors declare no competing financial and/or non-financial interests or other interests that might be perceived to influence the results and/or discussion reported in this paper. No writing assistance was utilized in the production of this manuscript.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Thankam, F.G., Agrawal, D.K. Single Cell Genomics Identifies Unique Cardioprotective Phenotype of Stem Cells derived from Epicardial Adipose Tissue under Ischemia. Stem Cell Rev and Rep 18, 294–335 (2022). https://doi.org/10.1007/s12015-021-10273-0
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12015-021-10273-0