Abstract
Purpose of Review
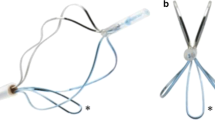
The purpose of the present systematic review is to offer a narrative synthesis of the available literature regarding the role of the temporary implantable nitinol device (TIND) (Medi-Tate®; Medi-Tate Ltd., Or Akiva, Israel) for the treatment of benign prostatic hyperplasia (BPH)-related lower urinary tract symptoms (LUTS), specifically focusing on the follow-up data.
Recent Findings
Current available evidences are limited in this topic. Sample size of patients available for analysis is small. Moreover, the duration of follow-up period is intermediate and longer follow-up is required. At the available 3 years follow-up, the TIND implantation is safe, effective, and well tolerated.
Summary
The extended follow-up of the first and only available cohort of patients who underwent TIND for LUTS related to BPH corroborated previous literature findings. Further studies are required in order to assess the durability of TIND outcomes over a longer follow-up, to better define the indications of this approach, and to demonstrate the advantages of second-generation device over the first.


Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of great importance
Roehrborn CG. Current medical therapies for men with lower urinary tract symptoms and benign prostatic hyperplasia: achievement and limitations. Rev Urol. 2008;10:14–25.
Verhamme KM, Dieleman JP, Bleumink GS, Bosch JL, Stricker BH, Sturkenboom MC. Treatment strategies, patterns of drug use and treatment discontinuation in men with LUTS suggestive of benign prostatic hyperplasia: the Triumph Project. Eur Urol. 2003;44:539–45.
• Dahm P, Brasure M, MacDonald R, et al. Comparative effectiveness of newermedications for lower urinary tract symptoms attributed to benign prostatic hyperplasia: a systematic review and meta-analysis. Eur Urol. 2017;71(4):570–81. A complete resign of the available medical treatment of BPH.
Marszalek M, Ponholzer A, Pusman M, Berger I, Madersbacher S. Transurethral resection of the prostate. Eur Urol Suppl. 2009;8:504–12.
Oelke M, Bachmann A, Descazeaud A, Emberton M, Gravas S, Michel MC, et al. EAU guidelines on the treatment and follow-up of non-neurogenic male lower urinary tract symptoms including benign prostatic obstruction. Eur Urol. 2013;64:118–40.
DE Nunzio C, Lombardo R, Nacchia A, Deroma M, Alkhatatbeh H, Brassetti A, et al. Young academic urologist benign prostatic obstruction nomogram predicts clinical outcome in patients treated with transurethral resection of prostate: an Italian cohort study. Minerva Urol Nefrol. 2017; https://doi.org/10.23736/S0393-2249.17.03008-9.
Geavlete P. Is classical transurethral resection of the prostate, the gold standard endoscopic treatment for benign prostate hyperplasia, in real danger of being replaced? Eur Urol. 2010;58:356–9.
Rieken M, Presicce F, Autorino R, DE Nunzio C. Clinical significance of intravesical prostatic protrusion in the management of benign prostatic enlargement: a systematic review and critical analysis of current evidence. Minerva Urol Nefrol. 2017 Dec;69(6):548–55. https://doi.org/10.23736/S0393-2249.17.02828-4.
Lourenco T, Pickard R, Vale L, Grant A, Fraser C, MacLennan G, et al. Minimally invasive treatments for benign prostatic enlargement: systematic review of randomized controlled trials. BMJ. 2008;337:a1662.
Gravas S, Bachmann A, Reich O, Roehrborn CG, Gilling PJ, De La Rosette J. Critical review of lasers in benign prostatic hyperplasia (BPH). BJU Int. 2011;107:1030–43.
Naspro R, Gomez Sancha F, Manica M, Meneghini A, Ahyai S, Aho T, et al. From “gold standard” resection to reproducible “future standard” endoscopic enucleation of the prostate: what we know about anatomical enucleation. Minerva Urol Nefrol. 2017 Oct;69(5):446–58. https://doi.org/10.23736/S0393-2249.17.02834-X.
Brassetti A, DE Nunzio C, Delongchamps NB, Fiori C, Porpiglia F, Tubaro A. Green light vaporization of the prostate: is it an adult technique? Minerva Urol Nefrol. 2017 Apr;69(2):109–18. https://doi.org/10.23736/S0393-2249.16.02791-0. Epub 2016 Dec 1. Review.
Helo S, Holland B, McVary KT. Convective radiofrequency water vapor thermal therapy with Rezūm system. Curr Urol Rep. 2017 Oct;18(10):78. https://doi.org/10.1007/s11934-017-0728-1.
Gratzke C, Bachmann A, Descazeaud A, Drake MJ, Madersbacher S, Mamoulakis C, et al. EAU guidelines on the assessment of non-neurogenic male lower urinary tract symptoms including benign prostatic obstruction. Eur Urol. 2015;67(6):1099–109.
Perera M, Roberts MJ, Doi SA, Bolton D. Prostatic urethral lift improves urinary symptoms and flow while preserving sexual function for men with benign prostatic hyperplasia: a systematic review and meta-analysis. Eur Urol. 2015;67(4):704–13.
Welliver C, Essa A. Sexual side effects of medical and surgical benign prostatic hyperplasia treatments. Urol Clin N Am. 2016;43:393–404.
Porpiglia F, Fiori C, Bertolo R, Garrou D, Cattaneo G, Amparore D. Temporary implantable nitinol device (TIND): a novel, minimally invasive treatment for relief of lower urinary tract symptoms (LUTS) related to benign prostatic hyperplasia (BPH): feasibility, safety and functional results at 1 year of follow-up. BJU Int. 2015;116(2):278–87. https://doi.org/10.1111/bju.12982.
Grise P, Plante M, Palmer J, Martinez-Sagarra J, Hernandez C, Schettini M, et al. Evaluation of the transurethral ethanol ablation of the prostate (TEAP) for symptomatic benign prostatic hyperplasia (BPH): a European multi-center evaluation. Eur Urol. 2004;46:496–501.
Ahyai SA, Gilling P, Kaplan SA, Kuntz RM, Madersbacher S, Montorsi F, et al. Meta-analysis of functional outcomes and complications following transurethral procedures for lower urinary tract symptoms resulting from benign prostatic enlargement. Eur Urol. 2010 Sep;58(3):384–97. https://doi.org/10.1016/j.eururo.2010.06.005.
• Magistro G, Chapple CR, Elhilali M, Gilling P, McVary KT, Roehrborn CG, et al. Emerging minimally invasive treatment options for male lower urinary tract symptoms. Eur Urol. 2017;72(6):986–97. https://doi.org/10.1016/j.eururo.2017.07.005. A resign of the currently available less invasive treatments for BPH.
Wei JT, Dunn RL, Litwin MS, Sandler HM, Sanda MG. Development and validation of the expanded prostate cancer index composite (EPIC) for comprehensive assessment of health-related quality of life in men with prostate cancer. Urology. 2000;56:899–905.
•• Porpiglia F, Fiori C, Bertolo R, Giordano A, Checcucci E, Garrou D, et al. Three-year follow-up of temporary implantable nitinol device (TIND®) implantation for the treatment of benign prostatic obstruction. BJU Int. 2018; https://doi.org/10.1111/bju.14141. The only available up-to-date study published on TIND with three years of follow-up.
Porpiglia F, Fiori C, Bertolo R, Amparore D. Meditate temporary implantable nitinol device. Curr Bladder Dysfunct Rep. 2017;12:124–8.
Porpiglia F, Fiori C, Amparore D, et al. The new meditate (r) temporary implantable nitinol device (i-TIND) in the treatment of bladder outlet obstruction due to BPH: results of one arm, multi-center prospective, study. J Urol. 2017;197(4, Supplement: S):E512–2. https://doi.org/10.1016/j.juro.2017.02.1224.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Riccardo Bertolo, Cristian Fiori, Daniele Amparore, and Francesco Porpiglia each declare no potential conflicts of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Benign Prostatic Hyperplasia
Rights and permissions
About this article
Cite this article
Bertolo, R., Fiori, C., Amparore, D. et al. Follow-up of Temporary Implantable Nitinol Device (TIND) Implantation for the Treatment of BPH: a Systematic Review. Curr Urol Rep 19, 44 (2018). https://doi.org/10.1007/s11934-018-0793-0
Published:
DOI: https://doi.org/10.1007/s11934-018-0793-0