Abstract
Background
Sepsis is the most frequent cause of systemic inflammatory response syndrome (SIRS). Procalcitonin (PCT) and C-reactive protein (CRP) are well-known predictors of sepsis. Serum PCT levels are associated with blood culture positivity in patients with sepsis, but the magnitude of elevation of PCT and CRP levels at the onset of sepsis is unknown in Gram-negative (GN) bacteremia and in Gram-positive (GP) bacteremia.
Aims
To evaluate the PCT and CRP levels in 72 h at the onset of sepsis in GN and GP bacteremia.
Methods
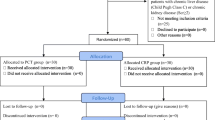
We retrospectively analyzed the data from 648 blood-positive specimens from three integrated teaching hospitals in Xiamen, China. One hundred and forty-seven adult patients with sepsis within 72 h enrolled in the study. Serum PCT and CRP level were assessed according GN or GP bacteremia.
Results
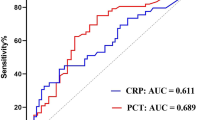
A total of 147 (22.68 %) patients were eligible for inclusion in the study, including 56 GP sepsis and 91 GN sepsis. PCT, but not CRP levels, was significantly higher in patients in the GP group than in the GN group (23.64 vs 6.18 ng/mL, p < 0.001). The area under the receiver-operating characteristic (ROC) curve of PCT was 0.73 (95 % confidence interval 0.65–0.81) and that under the ROC curve of CRP was 0.52 (95 % confidence interval 0.43–0.62). A positive predictive value of 72.5 % and a negative predictive value of 67.9 % were achieved with a PCT cutoff value of 2.1 ng/ml.
Conclusion
Serum PCT levels are higher in GN sepsis than GP sepsis in 72 h. There are not differences in CRP. The separation of PCT and CRP phenomenon is helpful for early diagnosis of GP sepsis.


Similar content being viewed by others
References
Prucha M, Bellingan G, Zazula R (2015) Sepsis biomarkers. Clin Chim Acta 440:97–103
Martin G, Brunkhorst FM, Janes JM et al (2009) The international PROGRESS registry of patients with severe sepsis: drotrecogin alfa (activated) use and patient outcomes. Crit Care 13:R103
Uzzan B, Cohen R, Nicolas P et al (2006) Procalcitonin as a diagnostic test for sepsis in critically ill adults and after surgery or trauma: a systematic review and meta-analysis. Crit Care Med 34:1996–2003
Christ-Crain M, Jaccard-Stolz D, Bingisser R et al (2004) Effect of procalcitonin-guided treatment on antibiotic use and outcome in lower respiratory tract infections: cluster-randomised, single-blinded intervention trial. Lancet 363:600–607
Charles PE, Ladoire S, Aho S et al (2008) Serum procalcitonin elevation in critically ill patients at the onset of bacteremia caused by either Gram negative or Gram positive bacteria. BMC Infect Dis 8:38
Koivula I, Hämäläinen S, Jantunen E et al (2011) Elevated procalcitonin predicts Gram-negative sepsis in haematological patients with febrile neutropenia. Scand J Infect Dis 43:471–478
Ansar W, Ghosh S (2013) C-reactive protein and the biology of disease. Immunol Res 56:131–142
Bouadma L, Luyt CE, Tubach F et al (2010) Use of procalcitonin to reduce patients’ exposure to antibiotics in intensive care units (PRORATA trial): a multicentre randomised controlled trial. Lancet 375:463–474
Jeong S, Park Y, Cho Y et al (2012) Diagnostic utilities of procalcitonin and C-reactive protein for the prediction of bacteremia determined by blood culture. Clin Chim Acta 413:1731–1736
American College of Chest Physicians/Society of Critical Care Medicine Consensus Conference (1992) Definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. Crit Care Med 20:864–874
Phua J, Ngerng WJ, See KC et al (2013) Characteristics and outcomes of culture-negative versus culture-positive severe sepsis. Crit Care 17:R202
Svaldi M, Hirber J, Lanthaler AI et al (2001) Procalcitonin-reduced sensitivity and specificity in heavily leucopenic and immunosuppressed patients. Br J Haematol 115:53–57
Sánchez-Yepes M, Aznar-Oroval E, Lorente-Alegre P et al (2014) Use of procalcitonin and C-reactive protein as infection markers in febrile neutropenic patients undergoing haematopoietic stem cell transplant. Enferm Infect Microbiol Clin 32:418–423
Leli C, Cardaccia A, Ferranti M et al (2014) Procalcitonin better than C-reactive protein, erythrocyte sedimentation rate, and white blood cell count in predicting DNAemia in patients with sepsis. Scand J Infect Dis 46:745–752
Müller B, White JC, Nylén ES, Snider RH et al (2001) Ubiquitous expression of the calcitonin-i gene in multiple tissues in response to sepsis. J Clin Endocrinol Metab 86:396–404
Niederman MS (2008) Biological markers to determine eligibility in trials for community-acquired pneumonia: a focus on procalcitonin. Clin Infect Dis 47(Suppl 3):S127–S132
Dandona P, Nix D, Wilson MF et al (1994) Procalcitonin increase after endotoxin injection in normal subjects. J Clin Endocrinol Metab 79:1605–1608
Tavares E, Minano FJ (2010) Immunoneutralization of the aminoprocalcitonin peptide of procalcitonin protects rats from lethal endotoxaemia: neuroendocrine and systemic studies. Clin Sci 119:519–534
Linscheid P, Seboek D, Nylen ES et al (2003) In vitro and in vivo calcitonin I gene expression in parenchymal cells: a novel product of human adipose tissue. Endocrinology 144:5578–5584
Oberhoffer M, Vogelsang H, Jäger L et al (1999) Katacalcin and calcitonin immunoreactivity in different types of leukocytes indicate intracellular procalcitonin content. J Crit Care 14:29–33
Mikula T, Cianciara J, Wiercinska-Drapalo A (2011) Is there any influence of immune deficit on procalcitonin results? Hum Immunol 72(12):1194–1197
Hangai S, Nannya Y, Kurokawa M (2014) Role of procalcitonin and C-reactive protein for discrimination between tumor fever and infection in patients with hematological diseases. Leuk Lymphoma 56:910–914
Azarpira N, Ramzi M, Aghdaie M et al (2009) Procalcitonin and C-reactive protein serum levels after hematopoietic stem-cell transplant. Exp Clin Transplant 7:115–118
Acknowledgments
We sincerely thank Xiao Mei Liu, Lin Hui Zhan, Jin Chen, MD, Xiao Yan Zhao, Yi Yang, and Hao Xu for their assistance provided during the study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Hui Heng Liu declares that she has no conflict of interest. Min Wei Zhang declares that he has no conflict of interest. Jiu Bing Guo declares that he has no conflict of interest. Juan Li declares that she has no conflict of interest. Lei Su declares that he has no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the Ethical Committee of the Zhongshan Hospital of Xiamen University.
Rights and permissions
About this article
Cite this article
Liu, H.H., Zhang, M.W., Guo, J.B. et al. Procalcitonin and C-reactive protein in early diagnosis of sepsis caused by either Gram-negative or Gram-positive bacteria. Ir J Med Sci 186, 207–212 (2017). https://doi.org/10.1007/s11845-016-1457-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11845-016-1457-z