Abstract
Objectives
Although follow-up surveillance after resection for lung cancer is commonly performed in clinical practice, there is no standard follow-up program. We attempted to establish follow-up examination schedules that we considered would be acceptable to the majority of doctors, and would like to propose them as standard postoperative follow-up pathways.
Methods
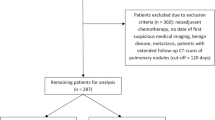
We carried out a retrospective analysis of patients’ data and reviewed the time of detection of recurrence and the site of recurrence after resection. Published papers were also reviewed. The postoperative follow-up pathways were established based on these data.
Proposed follow-up pathway
The follow-up period was set at as 5 years after resection, and physical examinations, chest radiography, chest CT and blood examination are recommended. Two follow-up pathways were proposed taking the risk of recurrence into consideration: the Risk of recurrence-based pathway and the Comprehensive pathway. In the Risk of recurrence-based pathway, the follow-up examination schedule is modified according to the risk of recurrence. In the Comprehensive pathway, a single universal examination schedule is recommended for all patients. The choice between these two pathways is left to the discretion of the attending doctor.
Conclusions
We proposed two follow-up pathways, based on retrospective analysis of patients’ data and a review of published papers, which we considered would be acceptable to the majority of doctors and would be suited to the current medical environment in Japan. A prospective study to evaluate the efficacy of the follow-up pathways is ongoing.

Similar content being viewed by others
References
Egermann U, Jaeggi K, Habicht JM, Perruchoud AP, Dalquen P, Soler M. Regular follow-up after curative resection of nonsmall cell lung cancer: a real benefit for patients? Eur Respir J. 2002;19:464–8.
Virgo KS, Naunheim KS, McKirgan LW, Kissling ME, Lin JC, Johnson FE. Cost of patient follow-up after potentially curative lung cancer treatment. J Thorac Cardiovasc Surg. 1996;112:356–63.
Walsh GL, O’Connor M, Willis KM, Milas M, Wong RS, Nesbitt JC, et al. Is follow-up of lung cancer patients after resection medically indicated and cost-effective? Ann Thorac Surg. 1995;60:1563–70 (discussion 1570–1562).
Younes RN, Gross JL, Deheinzelin D. Follow-up in lung cancer: how often and for what purpose? Chest. 1999;115:1494–9.
Chiu CH, Chern MS, Wu MH, Hsu WH, Wu YC, Huang MH, et al. Usefulness of low-dose spiral CT of the chest in regular follow-up of postoperative non-small cell lung cancer patients: preliminary report. J Thorac Cardiovasc Surg. 2003;125:1300–5.
Westeel V, Choma D, Clement F, Woronoff-Lemsi MC, Pugin JF, Dubiez A, et al. Relevance of an intensive postoperative follow-up after surgery for non-small cell lung cancer. Ann Thorac Surg. 2000;70:1185–90.
Watanabe T, Itabashi M, Shimada Y, Tanaka S, Ito Y, Ajioka Y, et al. Japanese Society for Cancer of the Colon and Rectum (JSCCR) guidelines 2010 for the treatment of colorectal cancer. Int J Clin Oncol. 2012;17:1–29.
Pretreatment evaluation of non-small-cell lung cancer. The American Thoracic Society and The European Respiratory Society. Am J Respir Crit Care Med. 1997;156:320–32.
Pfister DG, Johnson DH, Azzoli CG, Sause W, Smith TJ, Baker S Jr, et al. American Society of Clinical Oncology treatment of unresectable non-small-cell lung cancer guideline: update 2003. J Clin Oncol. 2004;22:330–53.
Felip E, Stahel RA, Pavlidis N. ESMO Minimum Clinical Recommendations for diagnosis, treatment and follow-up of non-small-cell lung cancer (NSCLC). Ann Oncol. 2005;16(Suppl 1):i28–9.
Rubins J, Unger M, Colice GL. Follow-up and surveillance of the lung cancer patient following curative intent therapy: ACCP evidence-based clinical practice guideline (2nd edition). Chest. 2007;132:355S–67S.
Follow-up of non-small lung cancer. American College of Radiology appropriateness criteria, 2005 2007; http://www.acr.org.
Sawada S, Suehisa H, Yamashita M, Nakata M, Okumura N, Okabe K, et al. Current status of postoperative follow-up for lung cancer in Japan: questionnaire survey by the Setouchi Lung Cancer Study Group-A0901. Gen Thorac Cardiovasc Surg. 2012;60:104–11.
Okada M, Nishio W, Sakamoto T, Harada H, Uchino K, Tsubota N. Long-term survival and prognostic factors of five-year survivors with complete resection of non-small cell lung carcinoma. J Thorac Cardiovasc Surg. 2003;126:558–62.
Martini N, Rusch VW, Bains, Kris MG, Downey RJ, Flehinger BJ, et al. Factors influencing ten-year survival in resected stages I to IIIa non-small cell lung cancer. J Thorac Cardiovasc Surg. 1999;117:32–6 (discussion 37–38).
Nakao M, Yoshida J, Goto K, Ishii G, Kawase A, Aokage K, et al. Long-term outcomes of 50 cases of limited-resection trial for pulmonary ground-glass opacity nodules. J Thorac Oncol. 2012;7(1563–1566):15. doi:10.1097/JTO.1560b1013e3182641b3182645c.
Altorki N, Kent M, Pasmantier M. Detection of early-stage lung cancer: computed tomographic scan or chest radiograph? J Thorac Cardiovasc Surg. 2001;121:1053–7.
Lee JI, Lee YJ, Park KY, Park CH, Jeon YB, Choi CH, et al. Fate of newly detected lesions during postoperative surveillance for non-small cell lung cancer. Ann Thorac Surg. 2013;95:1867–71.
Diederich S, Semik M, Lentschig MG, Winter F, Scheld HH, Roos N, et al. Helical CT of pulmonary nodules in patients with extrathoracic malignancy: CT-surgical correlation. AJR Am J Roentgenol. 1999;172:353–60.
Okada M, Nishio W, Sakamoto T, Uchino K, Yuki T, Nakagawa A, et al. Prognostic significance of perioperative serum carcinoembryonic antigen in non-small cell lung cancer: analysis of 1,000 consecutive resections for clinical stage I disease. Ann Thorac Surg. 2004;78:216–21.
Choi SH, Kim YT, Kim SK, Kang KW, Goo JM, Kang CH, et al. Positron emission tomography-computed tomography for postoperative surveillance in non-small cell lung cancer. Ann Thorac Surg. 2011;92:1826–32 (discussion 1832).
Dane B, Grechushkin V, Plank A, Moore W, Bilfinger T. PET/CT vs. non-contrast CT alone for surveillance 1-year post lobectomy for stage I non-small-cell lung cancer. Am J Nucl Med Mol Imaging. 2013;3:408–16.
Antoniou AJ, Marcus C, Tahari AK, Wahl RL, Subramaniam RM. Follow-up or surveillance 18F-FDG PET/CT and survival outcome in lung cancer patients. J Nucl Med. 2014;28:1062–8.
Aokage K, Yoshida J, Nishimura M, Nishiwaki Y, Nagai K. Annual abdominal ultrasonographic examination after curative NSCLC resection. Lung Cancer. 2007;57:334–8.
Yanagawa N, Shiono S, Abiko M, Ogata SY, Sato T, Tamura G. New IASLC/ATS/ERS classification and invasive tumor size are predictive of disease recurrence in stage I lung adenocarcinoma. J Thorac Oncol. 2013;8:612–8.
Warth A, Muley T, Meister M, Stenzinger A, Thomas M, Schirmacher P, et al. The novel histologic International Association for the Study of Lung Cancer/American Thoracic Society/European Respiratory Society classification system of lung adenocarcinoma is a stage-independent predictor of survival. J Clin Oncol. 2012;30:1438–46.
Asamura H, Goya T, Koshiishi Y, Sohara Y, Eguchi K, Mori M, et al. A Japanese Lung Cancer Registry study: prognosis of 13,010 resected lung cancers. J Thorac Oncol. 2008;3:46–52.
McCunney RJ, Li J. Radiation risks in lung cancer screening programs: a comparison with nuclear industry workers and atomic bomb survivors. Chest. 2014;145:618–24.
Little MP. Cancer after exposure to radiation in the course of treatment for benign and malignant disease. Lancet Oncol. 2001;2:212–20.
Bach PB, Mirkin JN, Oliver TK, et al. Benefits and harms of ct screening for lung cancer: a systematic review. JAMA. 2012;307:2418–29.
Winton T, Livingston R, Johnson D, Rigas J, Johnston M, Butts C, et al. Vinorelbine plus cisplatin vs. observation in resected non-small-cell lung cancer. N Engl J Med. 2005;352:2589–97.
Douillard JY, Rosell R, De Lena M, Carpagnano F, Ramlau R, Gonzales-Larriba JL, et al. Adjuvant vinorelbine plus cisplatin versus observation in patients with completely resected stage IB-IIIA non-small-cell lung cancer (Adjuvant Navelbine International Trialist Association [ANITA]): a randomised controlled trial. Lancet Oncol. 2006;7:719–27.
Butts CA, Ding K, Seymour L, Twumasi-Ankrah P, Graham B, Gandara D, et al. Randomized phase III trial of vinorelbine plus cisplatin compared with observation in completely resected stage IB and II non-small-cell lung cancer: updated survival analysis of JBR-10. J Clin Oncol. 2010;28:29–34.
Arriagada R, Dunant A, Pignon JP, Bergman B, Chabowski M, Grunenwald D, et al. Long-term results of the international adjuvant lung cancer trial evaluating adjuvant Cisplatin-based chemotherapy in resected lung cancer. J Clin Oncol. 2010;28:35–42.
Borgelt B, Gelber R, Kramer S, Brady LW, Chang CH, Davis LW, et al. The palliation of brain metastases: final results of the first two studies by the Radiation Therapy Oncology Group. Int J Radiat Oncol Biol Phys. 1980;6:1–9.
Coia LR, Aaronson N, Linggood R, Loeffler J, Priestman TJ. A report of the consensus workshop panel on the treatment of brain metastases. Int J Radiat Oncol Biol Phys. 1992;23:223–7.
Nieder C, Grosu AL, Astner S, Thamm R, Molls M. Integration of chemotherapy into current treatment strategies for brain metastases from solid tumors. Radiat Oncol. 2006;1:19.
Conflict of interest
None of the authors has any financial or other potential conflicts of interests to declare.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sawada, S., Shiono, S., Yamashita, Y. et al. A proposal of postoperative follow-up pathways for lung cancer. Gen Thorac Cardiovasc Surg 63, 231–238 (2015). https://doi.org/10.1007/s11748-014-0506-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11748-014-0506-7