Abstract
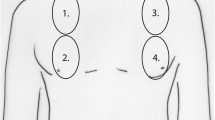
Chest ultrasonography is a useful tool to assess extravascular lung water at bedside. In presence of interstitial-alveolar imbibition, vertical artifacts arising from the pleura are detected; these are called B-lines. Although a positive linear correlation between B-lines and extravascular lung water has been shown in symptomatic heart failure patients, the subclinical phase of pulmonary imbibition and the clearance of B-lines after rapid body fluid removal have been less investigated. The aim of this study was to assess if chest ultrasound could detect lung water imbibition and its variations induced by dialysis, an experimental model of controlled rapid fluid loss. Forty-one patients undergoing hemodialysis were studied. Total number of B-lines from ultrasound chest scanning and vena cava diameters were measured before and after treatment. Before dialysis, most of the patients presented ultrasound signs of pulmonary imbibition despite the absence of dyspnea; the number of B-lines was associated with the accumulated weight before treatment (p < 0.05) as well as with the residual weight after dialysis (p < 0.01); B-lines and end-inspiratory and end-expiratory vena cava diameters were also significantly reduced after dialysis. Moreover, B-lines reduction was significantly related to weight loss. Ultrasound performed at the bedside can detect lung water and intravascular overload and their reduction after dialysis in yet asymptomatic patients. These observations add further evidence regarding the use of lung ultrasound and inferior vena cava measurement in estimating volume overload and monitoring the response to therapy both in hemodialysis and congestive heart failure patients.



Similar content being viewed by others
References
Jambrik Z, Monti S, Coppola V, Agricola E, Mottola G, Miniati M et al (2004) Usefulness of ultrasound lung comets as a nonradiologic sign of extravascular lung water. Am J Cardiol 93:1265–12770
Lichtenstein D, Meziere G (1998) A lung ultrasound sign allowing bedside distinction between pulmonary edema and COPD: the comet-tail artifact. Intensive Care Med 24:1331–1334
Lichtenstein D, Meziere G, Biderman P, Gepner A, Barre O (1997) The comet-tail artifact. An ultrasound sign of alveolar-interstitial syndrome. Am J Respir Crit Care Med 156:1640–1646
Agricola E, Bove T, Oppizzi M, Marino G, Zangrillo A, Margonato A et al (2005) “Ultrasound comet-tail images”: a marker of pulmonary edema: a comparative study with wedge pressure and extravascular lung water. Chest 127:1690–1695
Soldati G, Copetti R, Sher S (2009) Sonographic interstitial syndrome: the sound of lung water. J Ultrasound Med 28:163–174
Gargani L, Frassi F, Soldati G, Tesorio P, Gheorghiade M, Picano E (2008) Ultrasound lung comets for the differential diagnosis of acute cardiogenic dyspnoea: a comparison with natriuretic peptides. Eur J Heart Fail 10:70–77
Lichtenstein DA, Meziere GA (2008) Relevance of lung ultrasound in the diagnosis of acute respiratory failure: the BLUE protocol. Chest 134:117–125
Agricola E, Picano E, Oppizzi M, Pisani M, Meris A, Fragasso G et al (2006) Assessment of stress-induced pulmonary interstitial edema by chest ultrasound during exercise echocardiography and its correlation with left ventricular function. J Am Soc Echocardiogr 19:457–463
Volpicelli G, Caramello V, Cardinale L, Mussa A, Bar F, Frascisco MF (2008) Bedside ultrasound of the lung for the monitoring of acute decompensated heart failure. Am J Emerg Med 26:585–591
Noble VE, Murray AF, Capp R, Sylvia-Reardon MH, Steele DJ, Liteplo A (2009) Ultrasound assessment for extravascular lung water in patients undergoing hemodialysis. Time course for resolution. Chest 135:1433–1439
Mallamaci F, Benedetto FA, Tripepi R, Rastelli S, Castellino P, Tripepi G, Picano E, Zoccali C (2010) Detection of pulmonary congestion by chest ultrasound in dialysis patients. JACC Cardiovasc Imaging 3:586–594
Alwall N, Lunderquist A, Olsson O (1953) Studies on electrolyte-fluid retention. I. Uremic lung, fluid lung? On pathogenesis and therapy; a preliminary report. Acta Med Scand 146:157–163
Kooman JP, van der Sande FM, Leunissen KM (2009) Wet or dry in dialysis—can new technologies help? Semin Dial 22:9–12
Reissig A, Kroegel C (2003) Transthoracic sonography of diffuse parenchymal lung disease: the role of comet tail artifacts. J Ultrasound Med 22:173–180
Gargani L, Doveri M, D’Errico L, Frassi F, Bazzichi ML, DelleSedie A, Scali MC, Monti S, Mondillo S, Bombardieri S, Caramella D, Picano E (2009) Ultrasound lung comets in systemic sclerosis: a chest sonography hallmark of pulmonary interstitial fibrosis. Rheumatology 48:1382–1387
Soldati G, Copetti R (2006) Ecografia toracica. Edizioni medico scientifiche, Torino, Italy
Volpicelli G, Cardinale L, Mussa A, Valeria C (2009) Diagnosis of cardiogenic pulmonary edema by sonography limited to the anterior lung. Chest 135:883
Kalantar-Zadeh K, Regidor DL, Kovesdy CP, Van Wyck D, Bunnapradist S, Horwich TB et al (2009) Fluid retention is associated with cardiovascular mortality in patients undergoing long-term hemodialysis. Circulation 119:671–679
Ando Y, Yanagiba S, Asano Y (1995) The inferior vena cava diameter as a marker of dry weight in chronic hemodialyzed patients. Artif Organs 19:1237–1242
Krause I, Birk E, Davidovits M, Cleper R, Blieden L, Pinhas L, Gamzo Z, Eisenstein B (2001) Inferior vena cava diameter: a useful method for estimation of fluid status in children on haemodialysis. Nephrol Dial Transplant 16:1203
Acknowledgment
We would like to acknowledge Dr. S. Guzzetti for statistical advice.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Trezzi, M., Torzillo, D., Ceriani, E. et al. Lung ultrasonography for the assessment of rapid extravascular water variation: evidence from hemodialysis patients. Intern Emerg Med 8, 409–415 (2013). https://doi.org/10.1007/s11739-011-0625-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11739-011-0625-4