Abstract
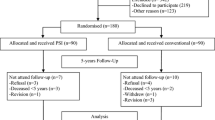
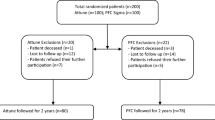
The purpose of this study was to determine if significant clinical differences exist in patient-reported outcome measures (PROMs) between PS and CR TKAs implanted using robotic-assisted technology. This was an IRB-approved retrospective study from an institutional database evaluating 214 knees in 190 patients. Inclusion criteria included: primary RA-TKA, age 22–89 at the time of surgery, preoperative coronal limb deformity within 15º of neutral alignment, and minimum 1-year follow-up. The PS cohort consisted of 103 patients with 107 RA-TKAs, whereas the CR cohort consisted of 87 patients with 107 RA-TKAs. Cohorts were compared on the basis of demographics and PROMs (KSS knee, KSS function, FJS-12, KOOS-JR, WOMAC, and 5-point satisfaction Likert scale) collected preoperatively and at 1-year follow-up. Statistical analyses comparing measures were conducted via Student’s t tests for continuous data and Chi-squared analyses for categorical data. There were no significant differences identified in short-term PROMs at 1-year follow-up between cohorts (all p values > 0.05). 93.1% of patients with CR knees and 94.7% of patients with PS knees reported a satisfaction level of “very satisfied” or “satisfied”. Revision arthroplasty occurred in six knees (2.8%, 3 knees in CR cohort, 3 knees in PS cohort) with no differences in overall complications between groups. The use of RA-TKA technology promoted high patient satisfaction scores within this study, independent of CR or PS implant type with no significant differences in PROMs, satisfaction, revisions, or complications between the two groups.


Similar content being viewed by others
Data availability
Unavailable.
References
Serna-Berna R, Lizaur-Utrilla A, Vizcaya-Moreno MF, Miralles Muñoz FA, Gonzalez-Navarro B, Lopez-Prats FA (2018) Cruciate-retaining vs posterior-stabilized primary total arthroplasty. Clinical outcome comparison With a minimum follow-up of 10 years. J Arthroplasty 33(8):2491–2495. https://doi.org/10.1016/j.arth.2018.02.094
Tria A (2002) Total knee arthroplasty. In: Scuderi G, Tria A (eds) Surgical techniques in total knee arthroplasty. Springer, New York, pp 177–185. https://doi.org/10.1007/0-387-21714-2_24
Ranawat CS, Insall J, Shine J (1975) Duo-condylar knee replacement. Curr Pract Orthop Surg 6:28–35
Insall J, Scott WN, Ranawat CS (1979) The total condylar knee prosthesis. A report of two hundred and twenty cases. J Bone Jt Surg 61(2):173–180 (American volume)
Shalhoub S, Lawrence JM, Keggi JM, Randall AL, DeClaire JH, Plaskos C (2019) Imageless, robotic-assisted total knee arthroplasty combined with a robotic tensioning system can help predict and achieve accurate postoperative ligament balance. Arthroplast Today 5(3):334–340. https://doi.org/10.1016/j.artd.2019.07.003
Kayani B, Haddad FS (2019) Robotic total knee arthroplasty: clinical outcomes and directions for future research. Bone Jt Res 8(10):438–442. https://doi.org/10.1302/2046-3758.810.Bjr-2019-0175
Parsley BS (2018) Robotics in orthopedics: a brave new world. J Arthroplasty 33(8):2355–2357. https://doi.org/10.1016/j.arth.2018.02.032
Song EK, Seon JK, Yim JH, Netravali NA, Bargar WL (2013) Robotic-assisted TKA reduces postoperative alignment outliers and improves gap balance compared to conventional TKA. Clin Orthop Relat Res 471(1):118–126. https://doi.org/10.1007/s11999-012-2407-3
Smith AF, Eccles CJ, Bhimani SJ et al (2019) Improved patient satisfaction following robotic-assisted total knee arthroplasty. J Knee Surg. https://doi.org/10.1055/s-0039-1700837
Nam D, Nunley RM, Barrack RL (2014) Patient dissatisfaction following total knee replacement: a growing concern? Bone Jt J 96-b(11 Supple A):96–100. https://doi.org/10.1302/0301-620x.96b11.34152
Canovas F, Dagneaux L (2018) Quality of life after total knee arthroplasty. Orthop Traumatol Surg Res 104(1S):S41–S46. https://doi.org/10.1016/j.otsr.2017.04.017
Bourne RB, Chesworth BM, Davis AM, Mahomed NN, Charron KD (2010) Patient satisfaction after total knee arthroplasty: who is satisfied and who is not? Clin Orthop Relat Res 468(1):57–63. https://doi.org/10.1007/s11999-009-1119-9
Kayani B, Konan S, Tahmassebi J, Oussedik S, Moriarty PD, Haddad FS (2020) A prospective double-blinded randomised control trial comparing robotic arm-assisted functionally aligned total knee arthroplasty versus robotic arm-assisted mechanically aligned total knee arthroplasty. Trials 21(1):194. https://doi.org/10.1186/s13063-020-4123-8
Scott RD, Volatile TB (1986) Twelve years’ experience with posterior cruciate-retaining total knee arthroplasty. Clin Orthop Relat Res 205:100–107
Zhang X, Zhu C, Shang X (2020) Letter to the editor on “does recession of the posterior cruciate ligament influence outcome in total knee arthroplasty?” J Arthroplasty 35(4):1162-1164.e1161. https://doi.org/10.1016/j.arth.2019.12.031
Broberg JS, Ndoja S, MacDonald SJ, Lanting BA, Teeter MG (2020) Comparison of contact kinematics in posterior-stabilized and cruciate-retaining total knee arthroplasty at long-term follow-up. J Arthroplasty 35(1):272–277. https://doi.org/10.1016/j.arth.2019.07.046
Kayani B, Konan S, Horriat S, Ibrahim MS, Haddad FS (2019) Posterior cruciate ligament resection in total knee arthroplasty: the effect on flexion-extension gaps, mediolateral laxity, and fixed flexion deformity. Bone Jt J 101-b(10):1230–1237. https://doi.org/10.1302/0301-620x.101b10.Bjj-2018-1428.R2
Murakami K, Hamai S, Okazaki K et al (2017) Kinematic analysis of stair climbing in rotating platform cruciate-retaining and posterior-stabilized mobile-bearing total knee arthroplasties. Arch Orthop Trauma Surg 137(5):701–711. https://doi.org/10.1007/s00402-017-2662-6
Longo UG, Ciuffreda M, Mannering N et al (2018) Outcomes of posterior-stabilized compared with cruciate-retaining total knee arthroplasty. J Knee Surg 31(4):321–340. https://doi.org/10.1055/s-0037-1603902
Dorr LD, Ochsner JL, Gronley J, Perry J (1988) Functional comparison of posterior cruciate-retained versus cruciate-sacrificed total knee arthroplasty. Clin Orthop Relat Res 236:36–43
Becker MW, Insall JN, Faris PM (1991) Bilateral total knee arthroplasty. One cruciate retaining and one cruciate substituting. Clin Orthop Relat Res 271:122–124
Migliorini F, Eschweiler J, Tingart M, Rath B (2019) Posterior-stabilized versus cruciate-retained implants for total knee arthroplasty: a meta-analysis of clinical trials. Eur J Orthop Surg Traumatol 29(4):937–946. https://doi.org/10.1007/s00590-019-02370-1
Sires JD, Craik JD, Wilson CJ (2019) Accuracy of bone resection in MAKO total knee robotic-assisted surgery. J Knee Surg. https://doi.org/10.1055/s-0039-1700570
Rivière C, Harman C, Boughton O, Cobb J (2020) The kinematic alignment technique for total knee arthroplasty. Springer International Publishing, Cham, pp 175–195
Almaawi AM, Hutt JRB, Masse V, Lavigne M, Vendittoli PA (2017) The impact of mechanical and restricted kinematic alignment on knee anatomy in total knee arthroplasty. J Arthroplasty 32(7):2133–2140. https://doi.org/10.1016/j.arth.2017.02.028
Scuderi GR, Bourne RB, Noble PC, Benjamin JB, Lonner JH, Scott WN (2012) The new Knee Society knee scoring system. Clin Orthop Relat Res 470(1):3–19. https://doi.org/10.1007/s11999-011-2135-0
Giesinger JM, Behrend H, Hamilton DF, Kuster MS, Giesinger K (2019) Normative values for the forgotten joint score-12 for the US general population. J Arthroplasty 34(4):650–655. https://doi.org/10.1016/j.arth.2018.12.011
Lyman S, Lee YY, Franklin PD, Li W, Cross MB, Padgett DE (2016) Validation of the KOOS, JR: a short-form knee arthroplasty outcomes survey. Clin Orthop Relat Res 474(6):1461–1471. https://doi.org/10.1007/s11999-016-4719-1
Park SH, Kang BH, Kim MJ et al (2020) Validation of the Western Ontario and McMaster Universities arthritis index short form (WOMAC-SF) and its relevance to disability and frailty. Yonsei Med J 61(3):251–256. https://doi.org/10.3349/ymj.2020.61.3.251
Lyman S, Lee YY, McLawhorn AS, Islam W, MacLean CH (2018) What are the minimal and substantial improvements in the HOOS and KOOS and JR versions after total joint replacement? Clin Orthop Relat Res 476(12):2432–2441. https://doi.org/10.1097/corr.0000000000000456
Holtz N, Hamilton DF, Giesinger JM, Jost B, Giesinger K (2020) Minimal important differences for the WOMAC osteoarthritis index and the forgotten joint score-12 in total knee arthroplasty patients. BMC Musculoskelet Disord 21(1):401. https://doi.org/10.1186/s12891-020-03415-x
Lee WC, Kwan YH, Chong HC, Yeo SJ (2017) The minimal clinically important difference for Knee Society Clinical Rating System after total knee arthroplasty for primary osteoarthritis. Knee Surg Sports Traumatol Arthrosc 25(11):3354–3359. https://doi.org/10.1007/s00167-016-4208-9
Behrend H, Zdravkovic V, Giesinger J, Giesinger K (2016) Factors predicting the forgotten joint score after total knee arthroplasty. J Arthroplasty 31(9):1927–1932. https://doi.org/10.1016/j.arth.2016.02.035
Thienpont E, VandenBerghe A, Schwab PE, Forthomme JP, Cornu O (2016) Joint awareness in osteoarthritis of the hip and knee evaluated with the ‘forgotten joint’ score before and after joint replacement. Knee Surg Sports Traumatol Arthrosc 24(10):3346–3351. https://doi.org/10.1007/s00167-015-3970-4
Marchand RC, Sodhi N, Anis HK et al (2019) One-year patient outcomes for robotic-arm-assisted versus manual total knee arthroplasty. J Knee Surg 32(11):1063–1068. https://doi.org/10.1055/s-0039-1683977
Marchand RC, Sodhi N, Khlopas A et al (2017) Patient satisfaction outcomes after robotic arm-assisted total knee arthroplasty: a short-term evaluation. J Knee Surg 30(9):849–853. https://doi.org/10.1055/s-0037-1607450
Kayani B, Konan S, Pietrzak JRT, Haddad FS (2018) Iatrogenic bone and soft tissue trauma in robotic-arm assisted total knee arthroplasty compared with conventional jig-based total knee arthroplasty: a prospective cohort study and validation of a new classification system. J Arthroplasty 33(8):2496–2501. https://doi.org/10.1016/j.arth.2018.03.042
Siebert W, Mai S, Kober R, Heeckt PF (2002) Technique and first clinical results of robot-assisted total knee replacement. Knee 9(3):173–180. https://doi.org/10.1016/s0968-0160(02)00015-7
Tibbo ME, Limberg AK, Salib CG et al (2019) Acquired idiopathic stiffness after total knee arthroplasty: a systematic review and meta-analysis. The J Bone Jt Surg 101(14):1320–1330. https://doi.org/10.2106/jbjs.18.01217 (American volume)
Acknowledgements
Harry M. King, Jr.—assistance with data collection and analysis.
Funding
The authors did not receive support from any organization for the submitted work. No funding was received to assist with the preparation of this manuscript. No funding was received for conducting this study. No funds, grants, or other support was received.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by JAR, MW, NG, LS and JK. The first draft of the manuscript was written by JAR and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript. Please note that Dr. JW was added to the list of co-authors during the manuscript revision stage. Dr. Whitaker’s contribution included statistical analysis of the data.
Corresponding author
Ethics declarations
Conflict of interest
Author Jarod A. Richards declares that he has no conflict of interest. Author Mark D. Williams declares that he has no conflict of interest. Author Neil A. Gupta declares that he has no conflict of interest. Author Joseph M. Kitchen declares that he has no conflict of interest. Author John E. Whitaker declares that he has no conflict of interest. Author Langan S. Smith declares that he has no conflict of interest. Author Arthur L. Malkani declares he has received IP royalties, speaker and consultant honoraria, and research support from Stryker Orthopedics. He serves as a reviewer for Journal of Arthroplasty, Bone and Joint Journal, Journal of Knee Surgery and Journal of Hip Surgery.
Ethical approval
This research study was conducted retrospectively from data obtained for clinical purposes. We consulted extensively with the IRB of University of Louisville who determined that our study did not need ethical approval. No human subjects were enrolled or consented. No animals were involved. An IRB official waiver of ethical approval was granted from the IRB of University of Louisville (IRB# 20.0848).
Research involving human and animal participants
This article does not contain any studies with human or animal subjects performed by any of the authors.
Informed consent
This research study was conducted retrospectively from data obtained for clinical purposes. No identifying information about the patients are included. We consulted extensively with the IRB of University of Louisville who determined that our study did not need require informed consent from the subjects. This study was reviewed by the University of Louisville Institutional Review Board (IRB# 20.0848) and determined by the Chair/Vice-Chair of the IRB that the study is exempt according to 45 CFR 46.101(b) under Category 4: Secondary research for which consent is not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Richards, J.A., Williams, M.D., Gupta, N.A. et al. No difference in PROMs between robotic-assisted CR versus PS total knee arthroplasty: a preliminary study. J Robotic Surg 16, 1209–1217 (2022). https://doi.org/10.1007/s11701-021-01352-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11701-021-01352-y