Abstract
Objectives
To describe the innovative intraoperative technologies emerging to aid surgeons during minimally invasive robotic-assisted laparoscopic prostatectomy.
Methods
We searched multiple electronic databases reporting on intraoperative imaging and navigation technologies, robotic surgery in combination with 3D modeling and 3D printing used during laparoscopic or robotic-assisted laparoscopic prostatectomy. Additional searches were conducted for articles that considered the role of artificial intelligence and machine learning and their application to robotic surgery. We excluded studies using intraoperative navigation technologies during open radical prostatectomy and studies considering technology to visualize lymph nodes.
Summary of findings
Intraoperative imaging using either transrectal ultrasonography or augmented reality was associated with a potential decrease in positive surgical margins rates. Improvements in detecting capsular involvement may be seen with augmented reality. The benefit, feasibility and applications of other imaging modalities such as 3D-printed models and optical imaging are discussed.
Conclusion
The application of image-guided surgery and robotics has led to the development of promising new intraoperative imaging technologies such as augmented reality, fluorescence imaging, optical coherence tomography, confocal laser endomicroscopy and 3D printing. Currently challenges regarding tissue deformation and automatic tracking of prostate movements remain and there is a paucity in the literature supporting the use of these technologies. Urologic surgeons are encouraged to improve and test these advanced technologies in the clinical arena, preferably with comparative, randomized, trials.

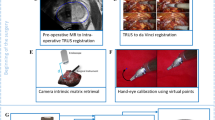
Reproduced with permission from Elsevier Inc [11]

Reproduced with permission from Elsevier Inc [11]

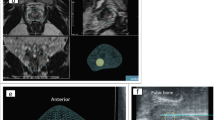
Reproduced with permission from Elsevier Inc [23]

Reproduced with permission from Elsevier Inc [23]

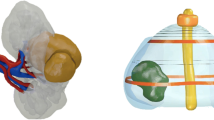
Reproduced with permission from Springer Nature [27]

Reproduced with permission from Mary Ann Liebert Inc [29]

Reproduced with permission from Mary Ann Liebert Inc [34]

Reproduced with permission from Wolters Kluwer Health Inc [36]
Similar content being viewed by others
Availability of data and material
The authors confirm that the data supporting the findings of this study are openly available within this article or those referenced.
Code availability
Not applicable.
References
Ferlay J et al (2015) Cancer incidence and mortality worldwide: sources, methods and major patterns in GLOBOCAN 2012. Int J Cancer 136(5):E359–E386
Chang SL et al (2015) The impact of robotic surgery on the surgical management of prostate cancer in the USA. BJU Int 115(6):929–936
Coughlin GD et al (2018) Robot-assisted laparoscopic prostatectomy versus open radical retropubic prostatectomy: 24-month outcomes from a randomised controlled study. Lancet Oncol 19(8):1051–1060
Tosoian JJ, Loeb S (2012) Radical retropubic prostatectomy: comparison of the open and robotic approaches for treatment of prostate cancer. Rev Urol 14(1–2):20–27
Ou YC et al (2013) The trifecta outcome in 300 consecutive cases of robotic-assisted laparoscopic radical prostatectomy according to D’Amico risk criteria. Eur J Surg Oncol 39(1):107–113
Walz J et al (2016) A critical analysis of the current knowledge of surgical anatomy of the prostate related to optimisation of cancer control and preservation of continence and erection in candidates for radical prostatectomy: an update. Eur Urol 70(2):301–311
Bianco Jr FJ, Scardino PT, Eastham JA (2005) Radical prostatectomy: long-term cancer control and recovery of sexual and urinary function (“trifecta”). Urology 66(5 Suppl):83–94
Ukimura O, Gill IS (2006) Real-time transrectal ultrasound guidance during nerve sparing laparoscopic radical prostatectomy: pictorial essay. J Urol 175(4):1311–1319
Sauvain JL et al (2003) Value of power Doppler and 3D vascular sonography as a method for diagnosis and staging of prostate cancer. Eur Urol 44(1):21–30 (discussion 30–1)
Ukimura O, Magi-Galluzzi C, Gill IS (2006) Real-time transrectal ultrasound guidance during laparoscopic radical prostatectomy: impact on surgical margins. J Urol 175(4):1304–1310
Han M et al (2011) Tandem-robot assisted laparoscopic radical prostatectomy to improve the neurovascular bundle visualization: a feasibility study. Urology 77(2):502–506
Long JA et al (2012) Real-time robotic transrectal ultrasound navigation during robotic radical prostatectomy: initial clinical experience. Urology 80(3):608–613
Hung AJ et al (2012) Robotic transrectal ultrasonography during robot-assisted radical prostatectomy. Eur Urol 62(2):341–348
Matsuoka Y et al (2014) Integrated image navigation system using head-mounted display in “RoboSurgeon” endoscopic radical prostatectomy. Wideochir Inne Tech Maloinwazyjne 9(4):613–618
Mohareri O et al (2015) Intraoperative registered transrectal ultrasound guidance for robot-assisted laparoscopic radical prostatectomy. J Urol 193(1):302–312
van der Poel HG et al (2008) Peroperative transrectal ultrasonography-guided bladder neck dissection eases the learning of robot-assisted laparoscopic prostatectomy. BJU Int 102(7):849–852
Shoji S et al (2014) Intraoperative ultrasonography with a surgeon-manipulated microtransducer during robotic radical prostatectomy. Int J Urol 21(7):736–739
Tang SL et al (1998) Augmented reality systems for medical applications. IEEE Eng Med Biol Mag 17(3):49–58
Thompson S et al (2013) Design and evaluation of an image-guidance system for robot-assisted radical prostatectomy. BJU Int 111(7):1081–1090
Simpfendörfer T et al (2011) Augmented reality visualization during laparoscopic radical prostatectomy. J Endourol 25(12):1841–1845
Rassweiler J et al (2014) Surgical navigation in urology: European perspective. Curr Opin Urol 24(1):81–97
Ukimura O et al (2014) Three-dimensional surgical navigation model with TilePro display during robot-assisted radical prostatectomy. J Endourol 28(6):625–630
Porpiglia F et al (2018) Augmented reality robot-assisted radical prostatectomy: preliminary experience. Urology 115:184
Porpiglia F et al (2019) Three-dimensional elastic augmented-reality robot-assisted radical prostatectomy using hyperaccuracy three-dimensional reconstruction technology: a step further in the identification of capsular involvement. Eur Urol 76(4):505–514
Ebbing J et al (2018) Comparison of 3D printed prostate models with standard radiological information to aid understanding of the precise location of prostate cancer: a construct validation study. PLoS ONE 13(6):e0199477
Shin T, Ukimura O, Gill IS (2016) Three-dimensional printed model of prostate anatomy and targeted biopsy-proven index tumor to facilitate nerve-sparing prostatectomy. Eur Urol 69(2):377–379
Porpiglia F et al (2018) Development and validation of 3D printed virtual models for robot-assisted radical prostatectomy and partial nephrectomy: urologists’ and patients’ perception. World J Urol 36(2):201–207
Weissleder R, Nahrendorf M (2015) Advancing biomedical imaging. Proc Natl Acad Sci U S A 112(47):14424–14428
Ganzer R et al (2009) Intraoperative photodynamic evaluation of surgical margins during endoscopic extraperitoneal radical prostatectomy with the use of 5-aminolevulinic acid. J Endourol 23(9):1387–1394
Schaafsma BE et al (2011) The clinical use of indocyanine green as a near-infrared fluorescent contrast agent for image-guided oncologic surgery. J Surg Oncol 104(3):323–332
Porpiglia F et al (2018) Selective clamping during laparoscopic partial nephrectomy: the use of near infrared fluorescence guidance. Minerva Urol Nefrol 70(3):326–332
Mangano MS et al (2018) Robot-assisted nerve-sparing radical prostatectomy using near-infrared fluorescence technology and indocyanine green: initial experience. Urologia 85(1):29–31
Huang D et al (1991) Optical coherence tomography. Science 254(5035):1178–1181
Aron M et al (2007) Second prize: preliminary experience with the Niris optical coherence tomography system during laparoscopic and robotic prostatectomy. J Endourol 21(8):814–818
Chen SP, Liao JC (2014) Confocal laser endomicroscopy of bladder and upper tract urothelial carcinoma: a new era of optical diagnosis? Curr Urol Rep 15(9):437
Lopez A et al (2016) Intraoperative optical biopsy during robotic assisted radical prostatectomy using confocal endomicroscopy. J Urol 195(4 Pt 1):1110–1117
Navaratnam A, Abdul-Muhsin H, Humphreys M (2018) Updates in urologic robot assisted surgery. F1000Res 7:1948
Aruni G, Amit G, Dasgupta P (2018) New surgical robots on the horizon and the potential role of artificial intelligence. Investig Clin Urol 59(4):221–222
Panesar S et al (2019) Artificial intelligence and the future of surgical robotics. Ann Surg 270(2):223–226
Shademan A et al (2016) Supervised autonomous robotic soft tissue surgery. Sci Transl Med 8(337):337ra64
Kassahun Y et al (2016) Surgical robotics beyond enhanced dexterity instrumentation: a survey of machine learning techniques and their role in intelligent and autonomous surgical actions. Int J Comput Assist Radiol Surg 11(4):553–568
Hughes-Hallett A et al (2015) The current and future use of imaging in urological robotic surgery: a survey of the European Association of Robotic Urological Surgeons. Int J Med Robot 11(1):8–14
Acknowledgements
We also would like to acknowledge Riccardo Bertolo in assisting in the initial design of this review article.
Funding
The authors did not receive support from any organization for the submitted work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethics approval
This a review article and evidence synthesis of existing, ethically approved data, thus no dedicated ethical approval is required for this study.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Makary, J., van Diepen, D.C., Arianayagam, R. et al. The evolution of image guidance in robotic-assisted laparoscopic prostatectomy (RALP): a glimpse into the future. J Robotic Surg 16, 765–774 (2022). https://doi.org/10.1007/s11701-021-01305-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11701-021-01305-5