Abstract
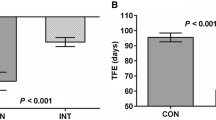
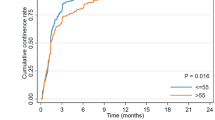
The objective of this study is to determine if the use of dehydrated human amnion/chorion membrane (dHACM) allograft wrapped around the NVB during a robotic-assisted radical prostatectomy (RARP) accelerates the return to potency. 940 patients with preoperative SHIM >20 underwent RARP with some degree of bilateral NS. Of these, 235 patients underwent RARP, with bilateral placement of dHACM graft around the NVBs. They were matched in a 1:3 proportion with a similar group of patients (n = 705) who did not receive the allograft (control group or group 2). Minimum follow-up was 12 months. Postoperative outcomes were analyzed between propensity-matched dHACM graft (group 1) and non-graft groups (group 2). Kaplan–Meier survival curves were compared across techniques using the log-rank test. There were no significant demographic differences between the two groups. Potency was defined as the ability to achieve and maintain satisfactory erections firm enough for sexual intercourse, with or without the use of PDE-5 inhibitors. The mean time to potency was significantly lower in group 1 (2.37 months) versus group 2 (3.94 months) (p < 0.0001). The potency recovery rates were superior for group 1 at all early time points measured except at 12 months. The time to potency was significantly shorter in the dHACM group with full NS, 2.19 ± 1.84 versus 2.78 ± 2.70 mo. in the non-dHACM with full NS (p = 0.029). In the dHACM group with partial NS, the mean time to potency was 3.05 ± 2.32 versus 3.92 ± 3.42 mo. in the non-dHACM with partial NS (p = 0.021). Patients who received the dHACM wrap around the NVB after RARP accelerates the return to potency when compared to a similar control group without the use of the allograft. We also demonstrated that this faster return to potency occurs regardless of the degree of the NS preservation. Younger patients (<55 years of age) had the highest overall advantage if they received the graft. Our results indicate that dHACM placement at the site of the prostatic NVB does not increase the risk of BCR after RARP, neither in the presence of PSM, extra-prostatic disease (≥pT3) nor high Gleason score (Gleason ≥8).






Similar content being viewed by others
Abbreviations
- dHACM:
-
Dehydrated human amnion/chorion membrane
- PCa:
-
Prostate cancer
- RARP:
-
Robotic-assisted radical prostatectomy
- NS:
-
Nerve spare
- RP:
-
Radical prostatectomy
- SHIM:
-
Sexual Health Inventory for Men
- y.o:
-
Years old
- mo.:
-
Months
References
Howlader N, Noone AM, Krapcho M, Garshell J, Miller D, Altekruse SF, Kosary CL, Yu M, Ruhl J, Tatalovich Z, Mariotto A, Lewis DR, Chen HS, Feuer EJ, Cronin KA (eds). SEER Cancer Statistics Review, 1975-2012, National Cancer Institute. Bethesda, MD, http://seer.cancer.gov/csr/1975_2012/, based on November 2014 SEER data submission, posted to the SEER web site, April 2015
NCCN Guidelines. Prostate cancer early detection. Vers2.2012. National Comprehensive Cancer Network Web site. http://www.nccn.org/professionals/physician_gls/pdf/prostate_detection.pdf. Accessed May 2012
Greene KL, Albertsen PC, Babaian RJ et al (2009) Prostate specific antigen best practice statement: 2009 update. J Urol 182:2232–2241
Heidenreich A, Bellmunt J, Bolla M et al (2011) EAU guidelines on prostate cancer. Part 1: screening, diagnosis, and treatment of clinically localised disease. EurUrol 59:61–71
Brett AS, Ablin RJ (2011) Prostate-cancer screening—what the US. Preventive Services Task Force left out. N Engl J Med 365:1949–1951
Walsh PC, Donker PJ (1982) Impotence following radical prostatectomy: insight into etiology and prevention. J Urol 128:492–497
Patel VR, Schatloff O, Chauhan S et al (2012) The role of the prostatic vasculature as a landmark for nerve sparing during robot-assisted radical prostatectomy. EurUrol 61:571–576
Kowalczyk KJ, Huang AC, Hevelone ND et al (2011) Stepwise approach for nerve sparing without countertraction during robot-assisted radical prostatectomy: technique and outcomes. EurUrol 60:536–547
Ko YH, Coelho RF, Sivaraman A et al (2013) Retrograde versus antegrade nerve sparing during robot-assisted radical prostatectomy: which is better for achieving early functional recovery? EurUrol 63:169–177
Menon M, Kaul S, Bhandari A, Shrivastava A, Tewari A, Hemal A (2005) Potency following robotic radical prostatectomy: a questionnaire based analysis of outcomes after conventional nerve sparing and prostatic fascia sparing techniques. J Urol 174:2291–2296
Finley DS, Osann K, Skarecty D, Ahlering TE (2009) Hypothermic nerver-sparing radical prostatectomy: rationale, feasibility, and effect on early continence. Urology 73(4):691–696
Fetterolf DE, Snyder RJ (2012) Scientific and clinical support for the use of dehydrated amniotic membrane in wound management. Wounds 24(10):299–307
MiMedx Research Report (2014) Effect of EpiFix on proliferation rates of PC3 and BOWE cells in vitro. MiMedx Group Inc, Marietta
Ricciardelli G, Ceccuzzi R, Raneri M et al (2014) Management of recurrent corneal ulcers: use of amniotic membrane. Eur J Ophthalmol 24:793–796
Zelen CM, Serena TE, Denoziere G, Fetterolf DE (2013) A prospective randomized comparative parallel study of amniotic membrane wound graft in the management of diabetic foot ulcers. [Randomized control study]. Int Wound J 10:502–507
Serena TE, Carter MC, Le LT et al (2014) A multi-center randomized controlled clinical trial evaluating the use of dehydrated human amnion/chorion membrane allografts and multi-layer compression therapy vs. multi-layer compression therapy alone in the treatment of venous leg ulcers. Wound Repair Regen. doi:10.1111/wrr.12227
Zelen CM, Gould L, Serena TE et al (2015) A prospective, randomised, controlled, multi-centre comparative effectiveness study of healing using dehydrated human amnion/chorion membrane allograft, bioengineered skin substitute or standard of care for treatment of chronic lower extremity diabetic ulcers. Int Wound J. doi:10.1111/iwj.12395
Patel VR, Samavedi S, Bates AS et al (2015) Dehydrated human amniotic membrane allograft nerve wrap around the prostatic neurovascular bundle accelerates early return to continence and potency following robot-assisted radical prostatectomy: propensity score–matched analysis. EurUrol 67:977–980
Patel VR, Schatloff O, Chauhan S et al (2012) The role of the prostatic vasculature as a landmark for nerve sparing during robot-assisted radical prostatectomy. Eur Urol 61(3):571–576
Ko YH, Coelho RF, Sivaraman A et al (2013) Retrograde versus antegrade nerve sparing during robot-assisted radical prostatectomy: which is better for achieving early functional recovery? Eur Urol 63(1):169–177
Patel VR, Coelho RF, Palmer KJ et al (2009) Periurethral suspension stitch during robot-assisted laparoscopic radical prostatectomy: description of the technique and continence outcomes. Eur Urol 56(3):472–478
Ou YC, Yang CK, Wang J et al (2013) The trifecta outcome in 300 consecutive cases of robotic-assisted laparoscopic radical prostatectomy according to D’Amico risk criteria. EJSO 39:107–113
Thompson I at el (2007 ) Guideline for the management of clinically localized prostate cancer. American Urological Association. 2007 Update
Sexual dysfunction after radical prostatectomy. Rev Urol. 2005; 7(Suppl 2): S3–S10
Parolini O, Solomon A, Evangelista M, Soncini M (2010) Human term placenta as a therapeutic agent: from the first clinical applications to future perspectives. In: Berven E (ed) Human placenta: structure and development. Nova Science, Hauppauge, pp 1–48
Zelen CM, Poka A, Andrews J (2013) A prospective, randomized, blinded comparative study of injectable dehydrated human amniotic/chorionic membrane (dHACM) in the treatment of recalcitrant plantar fasciitis a feasibility study. [Randomized control study]. Foot Ankle. doi:10.1177/1071100713502179
Koob TJ, Rennert R, Zabek N, Massee M, Lim JJ, Temenoff JS et al (2013) Biological properties of dehydrated human amnion/chorion composite graft: implications for chronic wound healing. Int Wound J 10:493–500
Koob TJ, Lied JJ, Massee M et al (2014) Properties of dehydrated human amnion/chorion composite grafts: Implications for wound repair and soft tissue regeneration. J Bio Mater. Research Part B Applied Biomaterials
Zelen CM, Serena TE, Denoziere G, Fetterolf DE (2013) A prospective randomized comparative parallel study of amniotic membrane wound graft in the management of diabetic foot ulcers. [Randomized control study]. Int Wound J 10(5):502–507
Serena TE, Carter MC, Le LT, Sabo MJ, DiMarco DT (2014) A Multi-center randomized controlled clinical trial evaluating the use of dehydrated human amnion/chorion membrane allografts and multi-layer compression therapy vs. multi-layer compression therapy alone in the treatment of venous leg ulcers. Wound Repair Regen. doi:10.1111/wrr.12227
Willett NJ, Thote T, Lin A, Moran S, Raji Y, Sridaran S, Stevens HY, Guldberg RE (2014) Intra-articular injection of micronized dehydrated human amnion/chorion membrane attenuates osteoarthritis development. Arthr Res Ther 16(10):R47
Hsu GS (2014) Utilizing dehydrated human amnion/chorion membrane allograft in transcanal tympanoplasty. Otolaryngology 4:161. doi:10.4172/2161-119X.1000161
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
The study was partially funded by MiMedx® (Marietta, GA, USA) who provided the grafts. Author Patel is a medical consultant for MiMedx®.
Conflict of interest
Ogaya-Pinies, Palayapalam-Ganapathi, Rogers, Hernandez-Cardona, Rocco, Coelho, Jenson, declare that they have no conflicts of interest.
Ethical approval
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2000 (5).
Informed consent
Informed consent was obtained from all patients for being included in the study.
Rights and permissions
About this article
Cite this article
Ogaya-Pinies, G., Palayapalam-Ganapathi, H., Rogers, T. et al. Can dehydrated human amnion/chorion membrane accelerate the return to potency after a nerve-sparing robotic-assisted radical prostatectomy? Propensity score-matched analysis. J Robotic Surg 12, 235–243 (2018). https://doi.org/10.1007/s11701-017-0719-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11701-017-0719-8