Abstract
Introduction
The objective of this study is to evaluate the outcomes for Staple Line Reinforcement (SLR) in RA-SG based on the Metabolic and Bariatric Surgery Accreditation and Quality Improvement Program (MBSAQIP) database for 2019.
Materials and Methods
We selected patients who underwent RA-SG in the MBSAQIP PUF (Public Utility File) for the year 2019 and grouped them based on their SLR status: Oversewing (OS), Buttressing (BR), both OS and BR and neither. Our primary outcomes were bleeding, organ space infection (OSI), and adverse events (AEs), and our secondary outcomes were operation length, hospital length of stay, readmissions, and conversion to open rates. We conducted separate chi square or one-way analysis of variance (ANOVA) as appropriate and multivariable direct logistic regression models for the categorical outcomes.
Results
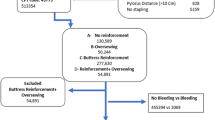
We found 115,621 patients with complete data of which there were 16,494 who underwent RA-SG. Our results did not show a statistically significant decrease in incidence of postoperative bleeding for BR and OS (Adjusted OR = 0.782, p = 0.2291 and Adjusted OR of 0.482, p = 0.054 for BR and OS respectively). There was a statistically significant effect for SLR status on operation length, with OS patients having the highest operative times (log-transformed mean = 2.03), followed by both BR + OS patients (log-transformed mean = 1.99). BR patients had the shortest operation length.
Conclusion
SLR did not result in any significant differences related to bleeding, OSI or AEs following RA-SG according to MBSAQIP for the year 2019. However, OS resulted in significantly longer operative time compared to BR alone.
Graphical Abstract

Similar content being viewed by others
References
Ng M, Fleming T, Robinson M, et al. Global, regional, and national prevalence of overweight and obesity in children and adults during 1980-2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet. 2014;384(9945):766-81. https://doi.org/10.1016/S0140-6736(14)60460-8. Erratum in: Lancet. 2014;384(9945):746.
Mingrone G, Panunzi S, De Gaetano A, et al. Bariatric-metabolic surgery versus conventional medical treatment in obese patients with type 2 diabetes: 5 year follow-up of an open-label, single-centre, randomised controlled trial. Lancet. 2015;386(9997):964–73. https://doi.org/10.1016/S0140-6736(15)00075-6.
Estimate of Bariatric Surgery Numbers, 2011–2020 [home-page on the Internet]. Gainesville: The American Society of Metabolic and Bariatric Surgeons; c2022 [updated 2022 Jun; accessed 2023 Apr 30]. Available at https://asmbs.org/resources/estimate-of-bariatric-surgery-numbers.
Mahawar KK, Omar I, Singhal R, et al. The first modified Delphi consensus statement on sleeve gastrectomy. Surg Endosc. 2021;35(12):7027–33. https://doi.org/10.1007/s00464-020-08216-w.
Morales-Marroquin E, Khatiwada S, Xie L, et al. Five year trends in the utilization of robotic bariatric surgery procedures, United States 2015–2019. Obes Surg. 2022;32(5):1539–45. https://doi.org/10.1007/s11695-022-05964-7.
Lin S, Jiang HG, Chen ZH, Zhou SY, Liu XS, Yu JR. Meta-analysis of robotic and laparoscopic surgery for treatment of rectal cancer. World J Gastroenterol. 2011;17(47):5214–20. https://doi.org/10.3748/wjg.v17.i47.5214.
Moser F, Horgan S. Robotically assisted bariatric surgery. Am J Surg. 2004;188(4A Suppl):38S-44S. https://doi.org/10.1016/j.amjsurg.2004.08.027.
Gagner M, Buchwald JN. Comparison of laparoscopic sleeve gastrectomy leak rates in four staple-line reinforcement options: a systematic review. Surg Obes Relat Dis. 2014;10(4):713–23. https://doi.org/10.1016/j.soard.2014.01.016.
Glaysher M, Khan OA, Mabvuure NT, et al. Staple line reinforcement during laparoscopic sleeve gastrectomy: does it affect clinical outcomes? Int J Surg. 2013;11(4):286–9. https://doi.org/10.1016/j.ijsu.2013.02.015.
Choi YY, Bae J, Hur KY, et al. Reinforcing the staple line during laparoscopic sleeve gastrectomy: does it have advantages? A meta-analysis. Obes Surg. 2012;22(8):1206–13. https://doi.org/10.1007/s11695-012-0674-4.
Gagner M, Deitel M, Erickson AL, Crosby RD. Survey on laparoscopic sleeve gastrectomy (LSG) at the Fourth International Consensus Summit on Sleeve Gastrectomy. Obes Surg. 2013;23(12):2013–7. https://doi.org/10.1007/s11695-013-1040-x.
Bennett WC, Park J, Mostellar M, et al. Comparison of robot-assisted sleeve gastrectomy outcomes in multiple staple line treatment modalities from 2015 to 2019: a 5-year propensity score-adjusted MBSAQIP® analysis. Surg Endosc. 2023;37(2):1401–11. https://doi.org/10.1007/s00464-022-09366-9.
Lundberg PW, Stoltzfus J, El Chaar M. 30-day outcomes of robot-assisted versus conventional laparoscopic sleeve gastrectomy: first analysis based on MBSAQIP. Surg Obes Relat Dis. 2019;15(1):1–7. https://doi.org/10.1016/j.soard.2018.10.015.
Aboueisha MA, Freeman M, Allotey JK, et al. Battle of the buttress: 5-year propensity-matched analysis of staple-line reinforcement techniques from the MBSAQIP database. Surg Endosc. 2023;37(4):3090–102. https://doi.org/10.1007/s00464-022-09452-y.
El Chaar M, Stoltzfus J, Gersin K, Thompson K. A novel risk prediction model for 30-day severe adverse events and readmissions following bariatric surgery based on the MBSAQIP database. Surg Obes Relat Dis. 2019;15(7):1138–45. https://doi.org/10.1016/j.soard.2019.03.005.
Gonzalez-Heredia R, Patel N, Sanchez-Johnsen L, et al. Does age influence bariatric surgery outcomes? Bariatr Surg Pract Patient Care. 2015;10(2):74–8. https://doi.org/10.1089/bari.2015.0004.
Petrick AT, Rosenthal RJ, Wood GC. Understanding the causes of conflicting outcomes reported using the same cohorts from the MBASQIP PUF data registry. Surg Obes Relat Dis. 2021;17(9):e42–5. https://doi.org/10.1016/j.soard.2021.05.005.
Gagner M, Kemmeter P. Comparison of laparoscopic sleeve gastrectomy leak rates in five staple-line reinforcement options: a systematic review. Surg Endosc. 2020;34(1):396–407. https://doi.org/10.1007/s00464-019-06782-2.
Moon RC, Teixeira AF, Jawad MA. To oversew or not to oversew in robotic sleeve gastrectomy: a case against oversewing the staple line. Langenbecks Arch Surg. 2021;406(4):1023–7. https://doi.org/10.1007/s00423-020-02073-w.
Barreto TW, Kemmeter PR, Paletta MP, Davis AT. A comparison of a single center’s experience with three staple line reinforcement techniques in 1,502 laparoscopic sleeve gastrectomy patients. Obes Surg. 2015;25(3):418–22. https://doi.org/10.1007/s11695-014-1432-6.
Moon RC, Stephenson D, Royall NA, et al. Robot-assisted versus laparoscopic sleeve gastrectomy: learning curve, perioperative, and short-term outcomes. Obes Surg. 2016;26(10):2463–8. https://doi.org/10.1007/s11695-016-2131-2.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Informed Consent
Informed Consent does not apply. For this type of study formal consent is not required.
Disclosures
Dr. Maher El Chaar is a paid faculty for Intuitive surgical and also received honoraria from WL Gore, none of the other authors have any disclosures.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The MBSAQIP program the hospitals participating in the MBSAQIP are the source of the data used herein; they have not verified and are not responsible for the statistical validity of the data analysis or the conclusions derived by the authors.
Social media: Agree to share on social media.
Twitter: @MaherElChaar
IG: dr_maher.elchaar
Key points
1. The use of Staple Line Reinforcement (SLR) in Robotic Assisted (RA-) surgery in the field of Metabolic and Bariatric Surgery MBS) is controversial because of lack of outcome data and cost concerns.
2. The analysis of the outcomes of various SLR techniques following RA-SG based on MBSAQIP PUF for 2019 showed that SLR does not result in any statistically significant differences in relation to bleeding, organ space infection or adverse events.
3. Use of buttressing material or oversewing of the staple line result in lower albeit non-significant bleeding rates following RA-SG.
4. Oversewing of the staple line results in significantly longer operative times compared to buttressing.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Faugno-Fusci, D., Perrone, J., Michaud, A. et al. Outcomes of Staple Line Reinforcement Following Robotic Assisted Sleeve Gastrectomy Based on MBSAQIP Database. OBES SURG 33, 2662–2670 (2023). https://doi.org/10.1007/s11695-023-06740-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-023-06740-x