Abstract
Purpose
This study aims to investigate the effectiveness of the transtheoretical model (TTM)–based exercise training on TTM variables, exercise adherence, and physical function in patients in the early stages after bariatric surgery (BS).
Materials and Methods
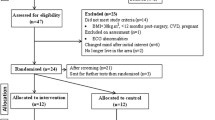
We conducted a single-blinded, prospective, randomized controlled trial (RCT) to evaluate the effects of TTM-based exercise training on BS patients immediately after surgery. Participants (n = 120) were randomized into a TTM-based exercise training group (n = 60) and a control group (n = 60). Main outcomes included TTM variables (measured by exercise stages of change (ESCs), exercise self-efficacy (ESE), and decisional balance), exercise adherence, and physical function (determined by the 6-min walk distance (6MWD)). Secondary outcomes were physical activity, anthropometrics, and body composition. We performed all analyses in accordance with the intention-to-treat principle.
Results
Retention rates for the interventions were 91.7% for the intervention group and 90.0% for the control group. Compared with the control group, the 12-week TTM-based intervention significantly helped participants advance through ESCs, demonstrate higher ESE, perceive more benefits and fewer barriers to exercise, and show higher exercise adherence and better physical function afterward (all P < 0.05). However, we observed no statistically significant difference between the two groups in anthropometric parameters or body composition after intervention.
Conclusion
The TTM-based exercise intervention had significant positive effects on the TTM variables, which could further help increase patients’ exercise adherence and physical function immediately after BS.
Trial Registration
This study was retrospectively registered at the Chinese Clinical Trial Registry (website: www.chictr.org.cn, registry number: ChiCTR2000039319).



Similar content being viewed by others
References
Global, regional, and national prevalence of overweight and obesity in children and adults during 1980-2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet. 2014;384(9945):766–81. https://doi.org/10.1016/S0140-6736(14)60460-8.
Wang Y, Wang L, Qu W. New national data show alarming increase in obesity and noncommunicable chronic diseases in China. Eur J Clin Nutr. 2017;71(1):149–50. https://doi.org/10.1038/ejcn.2016.171.
Angrisani L, Santonicola A, Iovino P, et al. Bariatric Surgery Worldwide 2013. Obes Surg. 2015;25(10):1822–32. https://doi.org/10.1007/s11695-015-1657-z.
Hui, Liang, Yun, et al. The effect of socioeconomic and individual factors on acceptance levels of bariatric surgery among Chinese patients. Surg Obes Relat Dis. 2014;10(2):361–5. https://doi.org/10.1016/j.soard.2013.07.016.
Adams TD, Davidson LE, Litwin SE, et al. Weight and metabolic outcomes 12 years after gastric bypass. N Engl J Med. 2017;377(12):1143–55. https://doi.org/10.1056/NEJMc1714001.
Velapati SR, Meera S, Kuchkuntla AR, et al. Weight regain after bariatric surgery: prevalence, etiology, and treatment. Curr Nutr Rep. 2018;7(4):329–34. https://doi.org/10.1007/s13668-018-0243-0.
Al-Najim W, Docherty NG, Le RCW. Food intake and eating behavior after bariatric surgery. Physiol Rev. 2018;98(3):1113–41. https://doi.org/10.1152/physrev.00021.2017.
Bellicha A et al. Effectiveness of exercise training after bariatric surgery-a systematic literature review and meta-analysis. Obes Rev. 2018;19(11):1544–56. https://doi.org/10.1111/obr.12740.
Ren ZQ, Lu GD, Zhang TZ, et al. Effect of physical exercise on weight loss and physical function following bariatric surgery: a meta-analysis of randomised controlled trials. BMJ Open. 2018;8(10):e023208. https://doi.org/10.1136/bmjopen-2018-023208.
Tabesh MR, Maleklou F, Ejtehadi F, et al. Nutrition, physical activity, and prescription of supplements in pre- and post-bariatric surgery patients: a practical guideline. Obes Surg. 2019;29(10):3385–400. https://doi.org/10.1007/s11695-019-04112-y.
Herring LY, Stevinson C, Carter P, et al. The effects of supervised exercise training 12–24 months after bariatric surgery on physical function and body composition: a randomised controlled trial. Int J Obes. 2017;41(6):909–16. https://doi.org/10.1038/ijo.2017.60.
Coleman KJ, Caparosa SL, Jeanne F. Nichols, et al. Understanding the capacity for exercise in post-bariatric patients. Obes Surg. 2017;27(1):51–8. https://doi.org/10.1007/s11695-016-2240-y.
Campanha-Versiani L, Pereira DAG, Ribeiro-Samora GA, et al. The effect of a muscle weight-bearing and aerobic exercise program on the body composition, muscular strength, biochemical markers, and bone mass of obese patients who have undergone gastric bypass surgery. Obes Surg. 2017;27(8):2129–37. https://doi.org/10.1007/s11695-017-2618-5.
King WC, Hsu JY, Belle SH, et al. Pre- to postoperative changes in physical activity: report from the Longitudinal Assessment of Bariatric Surgery-2 (LABS-2). Surg Obes Relat Dis. 2012;8(5):522–32. https://doi.org/10.1016/j.soard.2011.07.018.
Meena, Shah, Peter, et al. High-volume exercise program in obese bariatric surgery patients: a randomized, controlled trial. Obesity (Silver Spring). 2011;19(9):1826–34. https://doi.org/10.1038/oby.2011.172.
Ryan E, Rhodes, et al. Theories of physical activity behaviour change: a history and synthesis of approaches. Psychol Sport Exerc. 2019;42:100–9. https://doi.org/10.1016/j.psychsport.2018.11.010.
Dikareva A, Harvey WJ, Cicchillitti MA, et al. Exploring perceptions of barriers, facilitators, and motivators to physical activity among female bariatric patients: implications for physical activity programming. Am J Health Promot. 2015;30(7):536–44. https://doi.org/10.4278/ajhp.140609-QUAL-270.
Zabatiero J, Hill K, Gucciardi DF, et al. Beliefs, barriers and facilitators to physical activity in bariatric surgery candidates. Obes Surg. 2015;26(5):1097–109. https://doi.org/10.1007/s11695-015-1867-4.
Prochaska J. The transtheoretical model of health behavior change. Am J Health Promot. 1997;12(1):38–48. https://doi.org/10.4278/0890-1171-12.1.38.
Reid AE, Aiken LS. Integration of five health behaviour models: common strengths and unique contributions to understanding condom use. Psychol Health. 2011;26(11):1499–520. https://doi.org/10.1080/08870446.2011.572259.
Glanz K, Bishop DB. The role of behavioral science theory in development and implementation of public health interventions. Annu Rev Public Health. 2010;31(1):399–418. https://doi.org/10.1146/annurev.publhealth.012809.103604.
Marcus BH, Eaton CA, Rossi JS, et al. Self-efficacy, decision-making, and stages of change: an integrative model of physical exercise1. J Appl Soc Psychol. 1994;24(6):489–508. https://doi.org/10.1111/j.1559-1816.1994.tb00595.x.
Marcus BH, Simkin LR. The transtheoretical model: applications to exercise behavior. Med Sci Sports Exerc. 1994;26(11):1400–4. https://doi.org/10.1249/00005768-199411000-00016.
Lippke S. Stages of change in physical exercise: a test of stage discrimination and nonlinearity. Am J Health Behav. 2006;30(3):290–301. https://doi.org/10.5555/ajhb.2006.30.3.290.
Aveyard P, Massey L, Parsons A, et al. The effect of transtheoretical model based interventions on smoking cessation. Soc Sci Med. 2009;68(3):397–403. https://doi.org/10.1016/j.socscimed.2008.10.036.
de Freitas PP, Menezes MCD, Santos LCD, et al. The transtheoretical model is an effective weight management intervention: a randomized controlled trial. BMC Public Health. 2020;20(1):652. https://doi.org/10.1186/s12889-020-08796-1.
Scruggs S, Mama SK, Carmack CL, et al. Randomized trial of a lifestyle physical activity intervention for breast cancer survivors: effects on transtheoretical model variables. Health Promot Pract. 2018;19(1):134–44. https://doi.org/10.1177/1524839917709781.
Mastellos N, Gunn LH, Felix LM, et al. Transtheoretical model stages of change for dietary and physical exercise modification in weight loss management for overweight and obese adults. Cochrane Database System Rev. 2014;2(2):CD008066. https://doi.org/10.1002/14651858.CD008066.pub3.
Hayotte M, Nègre V, Gray L, et al. The transtheoretical model (TTM) to gain insight into young women’s long-term physical activity after bariatric surgery: a qualitative study. Obes Surg. 2019;30(2):595–602. https://doi.org/10.1007/s11695-019-04220-9.
Wang L, Chen H, Lu H, et al. The effect of transtheoretical model-lead intervention for knee osteoarthritis in older adults: a cluster randomized trial. Arthritis Res Ther. 2020;22(1):134. https://doi.org/10.1186/s13075-020-02222-y.
Marinov B, Kostianev S, Turnovska T. Modified treadmill protocol for evaluation of physical fitness in pediatric age group--comparison with Bruce and Balke protocols. Acta Physiol Pharmacol Bulg. 2003;27(2-3):47.
De Souza SAF, Faintuch J, Fabris SM, et al. Six-minute walk test: functional capacity of severely obese before and after bariatric surgery. Surg Obes Relat Dis. 2009;5(5):540–3. https://doi.org/10.1016/j.soard.2009.05.003.
Castello V, Simes RP, Bassi D, et al. Impact of aerobic exercise training on heart rate variability and functional capacity in obese women after gastric bypass surgery. Obes Surg. 2010;21(11):1739–49. https://doi.org/10.1007/s11695-010-0319-4.
Machin D, Campbell MJ, Tan SB, et al. Sample size tables for clinical studies. Third Ed. 2011;21(11):1739–49. https://doi.org/10.1002/9781444300710.
Urbaniak, G.C.; Plous, S. Research Randomizer (Version 4.0) [Computer Software]. Available online: http://www.randomizer.org/.
Ren ZQ, Zhang TZ, Yang NL, et al. Construction of an exercise rehabilitation program for obese people after bariatric surgery. Chin Gen Prac. 2019;22(19):2332–9. https://doi.org/10.12114/j.issn.1007-9572.2019.00.240.
Burbank PM, Reibe D, Padula CA, et al. Exercise and older adults. Orthop Nurs. 2002;21(4):51–63. https://doi.org/10.3928/0098-9134-20000301-03.
Wang Y, Wang CC, Zhu SH, et al. Guidelines for surgical treatment of obesity and type 2 diabetes (2019). Chin J Prac Surg. 2019;39(4):301–6. https://doi.org/10.19538/j.cjps.issn1005-2208.2019.04.01.
Mechanick JI, Apovian C, Brethauer S, et al. Clinical practice guidelines for the perioperative nutrition, metabolic, and nonsurgical support of patients undergoing bariatric procedures - 2019 update: cosponsored by American Association of Clinical Endocrinologists/American College of Endocrinology, The Obesity Society, American Society for Metabolic and Bariatric Surgery, Obesity Medicine Association, and American Society of Anesthesiologists. Obesity (Silver Spring). 2020;28(4):1001–58. https://doi.org/10.1016/j.soard.2019.10.025.
Marcus BH, Selby VC, Niaura RS, et al. Self-efficacy and the stages of exercise behavior change. Res Q Exerc Sport. 1992;63(1):60–6. https://doi.org/10.1080/02701367.1992.10607557.
Yin B. The Transtheoretical model of change in health behavior change. Chin J Ment Health. 2007;21(3):194–9. https://doi.org/10.3321/j.issn:1000-6729.2007.03.015.
Ferguson B. ACSM’s guidelines for exercise testing and prescription 9th Ed. 2014. J Can Chiropr Assoc. 2014;58(3):328. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4139760
Bandura A, Freeman WH, Lightsey R. Self-efficacy: the exercise of control. J Cogn Psychother. 1997;13(2):158–64. https://doi.org/10.1891/0889-8391.13.2.158.
Heijden MMP et al. Psychometric properties of the exercise self-efficacy scale in Dutch primary care patients with type 2 diabetes mellitus. Int J Behav Med. 2014;21(2):394–401. https://doi.org/10.1007/s12529-013-9308-z.
Faghri WSC, Pouran D. The link between musculoskeletal pain, lifestyle behaviors, exercise self-efficacy, and quality of life in overweight and obese individuals. Int J Phys Med Rehabil. 2015;3(01):255. https://doi.org/10.4172/2329-9096.1000255.
Sechrist KR, Walker SN, Pender NJ. Development and psychometric evaluation of the exercise benefits/barriers scale. Res Nurs Health. 2010;10(6):357–65. https://doi.org/10.1002/nur.4770100603.
Tung WC, Gillett PA, Pattillo RE. Applying the transtheoretical model to physical activity in family caregivers in Taiwan. Public Health Nurs. 2005;22(4):299–310. https://doi.org/10.1111/j.0737-1209.2005.220405.x.
Marti CN, Georgiopoulou VV, Giamouzis G, et al. Patient-reported selective adherence to heart failure self-care recommendations: a prospective cohort study: The Atlanta Cardiomyopathy Consortium. Congest Heart Fail. 2013;19(1):16–24. https://doi.org/10.1111/j.1751-7133.2012.00308.x.
Vella CA, Taylor K, Drummer D. High-intensity interval and moderate-intensity continuous training elicit similar enjoyment and adherence levels in overweight and obese adults. Eur J Sport Sci. 2017;17(9):1203–11. https://doi.org/10.1080/17461391.2017.1359679.
Crapo RO, Casaburi R, Coates AL, et al. ATS Statement: guidelines for the six-minute walk test. Am J Respir Crit Care Med. 2002;166(1):111–7. https://doi.org/10.1164/ajrccm.166.1.at1102.
Patterson E. Guidelines for data processing and analysis of the International Physical Activity Questionnaire (IPAQ)-short and long forms. 2005.
Macfarlane D, Chan A, Cerin E. Examining the validity and reliability of the Chinese version of the International Physical Activity Questionnaire, long form (IPAQ-LC). Public Health Nutr. 2011;14(3):443–50. https://doi.org/10.1017/S1368980010002806.
Sevil J, Práxedes A, Abarca-Sos A, et al. Levels of physical activity, motivation and barriers to participation in university students. J Sports Med Phys Fitness. 2015;56(10):1239–48. https://pubmed.ncbi.nlm.nih.gov/26554859
Lee DH, Park K, Ahn S, et al. Comparison of abdominal visceral adipose tissue area measured by computed tomography with that estimated by bioelectrical impedance analysis method in Korean subjects. Nutrients. 2015;7(12):10513–24. https://doi.org/10.3390/nu7125548.
Hamer RM, Simpson PM. Last observation carried forward versus mixed models in the analysis of psychiatric clinical trials. Am J Psychiatr. 2009;166(6):639–41. https://doi.org/10.1176/appi.ajp.2009.09040458.
Ham OK, Sung KM, Lee BG, et al. Transtheoretical model based exercise counseling combined with music skipping rope exercise on childhood obesity. Asian Nurs Res (Korean Soc Nurs Sci). 2016;10(2):116–22. https://doi.org/10.1016/j.anr.2016.03.003.
Selukmilosun A, Zincir H. The effect of a transtheoretical model–based motivational interview on self efficacy, metabolic control, and health behaviour in adults with type 2 diabetes mellitus: A randomized controlled trial. Int J Nurs Pract. 2019;25(4):e12742. https://doi.org/10.1111/ijn.12742.
Zhu LX, Ho SC, Sit JWH, et al. The effects of a transtheoretical model-based exercise stage-matched intervention on exercise behavior in patients with coronary heart disease: a randomized controlled trial. Patient Educ Couns. 2014;95(3):384–92. https://doi.org/10.1016/j.pec.2014.03.013.
Wang L, Chen H, Lu H, et al. The effect of transtheoretical model-lead intervention for knee osteoarthritis in older adults: a cluster randomized trial. Arthritis Res Ther. 2020;22(1):134–48. https://doi.org/10.1186/s13075-020-02222-y.
Richert J, Lippke S, Ziegelmann JP. Intervention-engagement and its role in the effectiveness of stage-matched interventions promoting physical exercise. Res Sports Med. 2011;19(3):145–61. https://doi.org/10.1080/15438627.2011.583164.
Vilela DB, Andrioni F. Jungerman, et al. The transtheoretical model and substance dependence: theoretical and practical aspects. Rev Bras Psiquiatr. 2009;31(4):362–8. https://doi.org/10.1590/s1516-44462009005000010.
Aoike DT, Baria F, Kamimura MA, et al. Impact of home-based aerobic exercise on the physical capacity of overweight patients with chronic kidney disease. Int Urol Nephrol. 2015;47(2):359–67. https://doi.org/10.1007/s11255-014-0894-8.
Jansons P, Robins L, O’Brien L, et al. Gym-based exercise was more costly compared with home-based exercise with telephone support when used as maintenance programs for adults with chronic health conditions: cost-effectiveness analysis of a randomised trial. Aust J Phys. 2017;64(1):48–54.
Babu AS, Padmakumar R, Nayak K, et al. Effects of home-based exercise training on functional outcomes and quality of life in patients with pulmonary hypertension: a randomized clinical trial. Indian Heart J. 2019;71(2):161–5. https://doi.org/10.1016/j.ihj.2019.03.002.
Park S, Gu MO. Development and Effects of Combined Exercise Program for Older Adults with Sarcopenia Based on Transtheoretical Model. J Korean Acad Nurs. 2018;48(6):656–68. https://doi.org/10.4040/jkan.2018.48.6.656.
Pirzadeh A, Mostafavi F, Ghofranipour F, et al. Applying transtheoretical model to promote physical activities among women. Iran J Psych Behav Sci. 2015;9(4):e1580. https://doi.org/10.17795/ijpbs-1580.
Stacie, Scruggs, Scherezade, et al. Randomized trial of a lifestyle physical activity intervention for breast cancer survivors: effects on transtheoretical model variables. Health Promot Pract. 2017;19(1):134–44. https://doi.org/10.1177/1524839917709781.
Bernardine MP, Carolyn R, Shira D, et al. Home-based exercise among cancer survivors: adherence and its predictors. Psychooncology. 2009;18(4):369–76. https://doi.org/10.1002/pon.1465.
Gremeaux V, Troisgros O, Benaïm S, et al. Determining the minimal clinically important difference for the six-minute walk test and the 200-meter fast-walk test during cardiac rehabilitation program in coronary artery disease patients after acute coronary syndrome. Arch Phys Med Rehabil. 2011;92(4):611–9. https://doi.org/10.1016/j.apmr.2010.11.023.
Holland AE, Hill CJ, Rasekaba T, et al. Updating the minimal important difference for six-minute walk distance in patients with chronic obstructive pulmonary disease. Arch Phys Med Rehabil. 2010;91(2):221–5. https://doi.org/10.1016/j.apmr.2009.10.017.
Stegen S, Derave W, Calders P, et al. Physical fitness in morbidly obese patients: effect of gastric bypass surgery and exercise training. Obes Surg. 2011;21(1):61–70. https://doi.org/10.1007/s11695-009-0045-y.
Maïmoun L, Lefebvre P, Jaussent A, et al. Body composition changes in the first month after sleeve gastrectomy based on gender and anatomic site. Surg Obes Relat Dis. 2018;13(5):1–7. https://doi.org/10.1016/j.soard.2017.01.017.
Mundbjerg LH, Stolberg CR, Cecere S, et al. Supervised physical training improves weight loss after roux-en-y gastric bypass surgery: a randomized controlled trial. Obesity (Silver Spring, Md). 2018;26(5):828–37. https://doi.org/10.1002/oby.22143.
Sjaak, Pouwels, Marjon, et al. Aspects of exercise before or after bariatric surgery: a systematic review. Obes Facts. 2015;8(2):132–46. https://doi.org/10.1159/000381201.
Egberts K, Brown WA, Brennan L, et al. Does exercise improve weight loss after bariatric surgery? A systematic review. Obes Surg. 2012;22(2):335–41. https://doi.org/10.1007/s11695-011-0544-5.
Hassannejad A, Khalaj A, Mansournia MA, et al. The effect of aerobic or aerobic-strength exercise on body composition and functional capacity in patients with BMI ≥35 after bariatric surgery: a randomized control trial. Obes Surg. 2017;27(11):2792–801. https://doi.org/10.1007/s11695-017-2717-3.
Coen PM, Tanner CJ, Helbling NL, et al. Clinical trial demonstrates exercise following bariatric surgery improves insulin sensitivity. J Clin Investig. 2015;125(1):248–57. https://doi.org/10.1172/JCI78016.
García-Ruiz-De-Gordejuela A, Agüera Z, Granero R, et al. Weight loss trajectories in bariatric surgery patients and psychopathological correlates. Eur Eat Disord Rev. 2017;25(6):586–94. https://doi.org/10.1002/erv.2558.
Conceição E, Bastos AP, Brandão I, et al. Loss of control eating and weight outcomes after bariatric surgery: a study with a Portuguese sample. Eat Weight Disord. 2014;19(1):103–9. https://doi.org/10.1007/s40519-013-0069-0.
Sheets CS, Peat CM, Berg KC, et al. Post-operative psychosocial predictors of outcome in bariatric surgery. Obes Surg. 2015;25(2):330–45. https://doi.org/10.1007/s11695-014-1490-9.
Acknowledgements
We would like to thank Guangdong Lu (Department of Interventional Radiology, The First Affiliated Hospital of Nanjing Medical University) for statistical advice. We thank Dongmei Ai (Department of Rehabilitation Medicine, Nanjing Drum Tower Hospital) for administering the exercise assessment and guidance. We thank Donglian Xu (Department of Clinical Nutrition, The First Affiliated Hospital of Nanjing Medical University) for nutrition guidance. We thank LetPub (www.letpub.com) for its linguistic assistance during the revision of this manuscript.
Funding
This research was funded by the project “The exploration of trajectories and intervention program of frailty for gastric cancer survivors based on the health ecology theory (82073407)” (supported by NSFC).
Author information
Authors and Affiliations
Contributions
Ziqi Ren contributed to conception, design, acquisition, analysis, and interpretation; drafted and critically revised the manuscript; gave final approval; and took responsibility for the integrity of the data and the accuracy of the data analysis. Hanfei Zhu contributed to conception, design, acquisition, analysis, and interpretation and drafted and critically revised the manuscript. Tianzi Zhang, Hongxia Hua, and Kang Zhao were responsible for the conception, design, participants’ recruitment, data collection, interpretation, and manuscript revision. Ningli Yang and Hui Liang were responsible for participants’ recruitment, data interpretation, and manuscript revision. Qin Xu was responsible for the conception, study design, manuscript drafting, and study supervision.
Corresponding author
Ethics declarations
Ethics Approval
This study was approved by the ethics committee of the First Affiliated Hospital of Nanjing Medical University (2018-SR-057). All procedures performed in studies involving human participants followed the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Key Points
1. Exercise training for BS patients was conducted immediately after surgery.
2. The TTM-based exercise intervention is effective in motivating BS patients to exercise regularly.
3. The TTM-based exercise intervention following bariatric surgery improves physical function.
4. A structured home-based exercise program for BS patients based on TTM is proposed.
Supplementary Information
ESM 1
(DOCX 37 kb)
Rights and permissions
About this article
Cite this article
Ren, Z., Zhu, H., Zhang, T. et al. Effects of a 12-Week Transtheoretical Model–Based Exercise Training Program in Chinese Postoperative Bariatric Patients: a Randomized Controlled Trial. OBES SURG 31, 4436–4451 (2021). https://doi.org/10.1007/s11695-021-05607-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-021-05607-3