Abstract
Introduction
Morbidly obese patients have lower quality of life (QOL) when compared to the general population. So far, no studies have compared gender and procedural differences in gastrointestinal QOL after sleeve gastrectomy (SG) and Roux-en-Y gastric bypass (RYGB).
Methods
Patients before and after bariatric surgery completed the gastrointestinal quality of life index (GIQLI), a 36-item questionnaire with five subscores. Differences between SG and RYGB were analyzed, as were gender differences.
Results
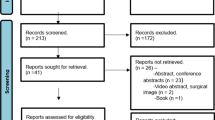
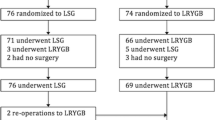
Some 186 patients completed the questionnaire, 75 before surgery, 56 within 6 months, and 55 within 24 months after surgery. Total GIQLI score and all subscores were significantly better within 24 months after surgery (80.9 ± 19.2 vs. 109.2 ± 17.7, p < 0.001). The specific gastrointestinal items ‘feeling of fullness’, ‘eating pleasure’, ‘slow speed of eating’, and ‘diarrhea’ were also significantly better after surgery whereas many other gastrointestinal items were not different. Total GIQLI score was significantly higher for SG than for RYGB within 6 months, while there were no significant differences within 24 months after surgery. There were also no significant differences in specific gastrointestinal items between SG and RYGB within 24 months after surgery and in total GIQLI score between female and male patients.
Conclusion
Total GIQLI score and all subscores were higher within 24 months after bariatric surgery. Total GIQLI score was significantly higher after SG when compared to RYGB within 6 months, but not different within 24 months after surgery. There was no difference in total GIQLI score between female and male patients.

Similar content being viewed by others
Abbreviations
- BMI:
-
Body mass index
- DMII:
-
Diabetes mellitus type II
- EWL:
-
Excess weight loss
- GERD:
-
Gastroesophageal reflux disease
- GIQLI:
-
Gastrointestinal quality of life index
- QOL:
-
Quality of life
- RCT:
-
Randomized controlled trial
- RYGB:
-
Roux-Y gastric bypass
- SG:
-
Sleeve gastrectomy
References
Gellner R, Domschke W. Epidemiology of obesity. Chirurg. 2008;79(9):807–10. 812-6, 818
Ogden CL et al. Prevalence of childhood and adult obesity in the United States, 2011-2012. JAMA. 2014;311(8):806–14.
Fruhbeck G et al. Obesity: the gateway to ill health—an EASO position statement on a rising public health, clinical and scientific challenge in Europe. Obes Facts. 2013;6(2):117–20.
Guh DP et al. The incidence of co-morbidities related to obesity and overweight: a systematic review and meta-analysis. BMC Public Health. 2009;9:88.
Kuk JL et al. Edmonton Obesity Staging System: association with weight history and mortality risk. Appl Physiol Nutr Metab. 2011;36(4):570–6.
Andersen JR et al. Health-related quality of life after bariatric surgery: a systematic review of prospective long-term studies. Surg Obes Relat Dis. 2015;11(2):466–73.
Jia H, Lubetkin EI. The impact of obesity on health-related quality-of-life in the general adult US population. J Public Health (Oxf). 2005;27(2):156–64.
Kolotkin RL, Meter K, Williams GR. Quality of life and obesity. Obes Rev. 2001;2(4):219–29.
Clements RH et al. Gastrointestinal symptoms are more intense in morbidly obese patients and are improved with laparoscopic Roux-en-Y gastric bypass. Obes Surg. 2003;13(4):610–4.
Yu P-J. Impairment of gastrointestinal quality of life in severely obese patients. World J Gastroenterol. 2014;20(22):7027.
Poves I et al. Gastrointestinal quality of life after laparoscopic Roux-en-Y gastric bypass. Obes Surg. 2006;16(1):19–23.
Mingrone G et al. Bariatric–metabolic surgery versus conventional medical treatment in obese patients with type 2 diabetes: 5 year follow-up of an open-label, single-centre, randomised controlled trial. Lancet. 2015;386(9997):964–73.
Sjostrom L. Review of the key results from the Swedish Obese Subjects (SOS) trial—a prospective controlled intervention study of bariatric surgery. J Intern Med. 2013;273(3):219–34.
Sjostrom L. Bariatric surgery and reduction in morbidity and mortality: experiences from the SOS study. Int J Obes. 2008;32(Suppl 7):S93–7.
Buchwald H, Oien DM. Metabolic/bariatric surgery worldwide 2011. Obes Surg. 2013;23(4):427–36.
Sarwer DB, Steffen KJ. Quality of life, body image and sexual functioning in bariatric surgery patients. Eur Eat Disord Rev. 2015;23(6):504–8.
Overs SE et al. Food tolerance and gastrointestinal quality of life following three bariatric procedures: adjustable gastric banding, Roux-en-Y gastric bypass, and sleeve gastrectomy. Obes Surg. 2011;22(4):536–43.
Hachem A, Brennan L. Quality of life outcomes of bariatric surgery: a systematic review. Obes Surg. 2015; doi:10.1007/s11695-015-1940-z.
Eypasch E et al. Gastrointestinal quality of life index: development, validation and application of a new instrument. Br J Surg. 1995;82(2):216–22.
Lee YC et al. Gastrointestinal quality of life following bariatric surgery in Asian patients. Hepato-Gastroenterology. 2013;60(124):759–61.
Lee WJ et al. Gastro-intestinal quality of life after metabolic surgery for the treatment of type 2 diabetes mellitus. Obes Surg. 2015;25(8):1371–9.
Ser KH et al. Experience in laparoscopic sleeve gastrectomy for morbidly obese Taiwanese: staple-line reinforcement is important for preventing leakage. Surg Endosc. 2010;24(9):2253–9.
Forgione A et al. Prospective evaluation of functional outcome after laparoscopic sigmoid colectomy. Ann Surg. 2009;249(2):218–24.
Mathus-Vliegen EM. Long-term weight loss after bariatric surgery in patients visited at home outside the study environment. Obes Surg. 2006;16(11):1508–19.
Acknowledgements
We would like to thank Mr. Jonathan D. Hendrie for proofreading of the manuscript, and we would like to thank Ms. Marion Link for helping with the organization of the study.
Author Contributions
Study conception and design: LF, FN, HGK, BPM; acquisition of data: FN, LS, ATB, HGK, LF; analysis and interpretation of data: LF, FN, ATB, LS, TB; drafting of manuscript: FN, LS; critical revision: LF, TB, HGK, BPM.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no competing interests.
Ethical Statement
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent Statement
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Nickel, F., Schmidt, L., Bruckner, T. et al. Gastrointestinal Quality of Life Improves Significantly After Sleeve Gastrectomy and Roux-en-Y Gastric Bypass—a Prospective Cross-Sectional Study Within a 2-Year Follow-up. OBES SURG 27, 1292–1297 (2017). https://doi.org/10.1007/s11695-016-2464-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-016-2464-x