Abstract
Background
It has been hypothesized that the metabolism of alcohol is altered following bariatric surgery. However, few studies have evaluated preoperative and postoperative alcohol use. The aims of the study were to characterize alcohol use in the preoperative period and 2 years postoperatively as well as to identify factors associated.
Methods
A study was conducted using data from the electronic charts of patients submitted to laparoscopic adjustable gastric banding (LAGB) and Roux-en-Y gastric bypass (RYGB) surgery in the city of Porto, Portugal. Associations with the following variables were analyzed: age, marital status, schooling, alcohol use, body mass index, binge eating disorder, and lifestyle habits.
Results
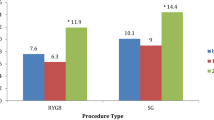
Among the 659 patients, 42.0 % completed the 2 years of follow-up. A total of 90.2 % were women; 67.4 % underwent LAGB, and 32.6 % underwent RYGB. The frequency of alcohol use was 24.2 % in the preoperative period and 9.4 % in the postoperative period (p = 0.000). Daily alcohol intake was two drinks in the preoperative period and 1.8 drinks in the postoperative period. Significant associations were found between postoperative alcohol use and the male gender (p = 0.001), age ≥45 years (p = 0.018), and preoperative BMI <40 kg/m2 (p = 0.028). No significant associations were found with the surgical technique. No previous nondrinkers became drinkers, and no patients increased the quantity or frequency of alcohol intake in the postoperative period.
Conclusions
The prevalence of alcohol use in the sample was low. Moreover, a lower prevalence rate was found in the postoperative period, independently of surgical technique, clinical factors, and percentage of weight loss.
Similar content being viewed by others
References
World Health Organization. Obesity and overweight. Fact sheet N°311, September 2006. http://www.who.int/mediacentre/factsheets/fs311/en/. Accessed November 19, 2011.
Buchwald H, Avidor Y, Braunwald E, et al. Bariatric surgery: a systematic review and meta-analysis. JAMA. 2004;292:1724–37.
Buchwald H, Estok R, Fahrbach K, et al. Weight and type 2 diabetes after bariatric surgery: systematic review and meta-analysis. Am J Med. 2009;122(3):248–56. doi:10.1016/j.amjmed.2008.09.041.PMID:19272486.
Sogg S. Alcohol misuse after bariatric surgery: epiphenomenon or “Oprah” phenomenon? Surg Obes Relat Dis. 2007;3(3):366–8.
Adams CE, Gabriele JM, Baillie LE. Tobacco use and substance use disorders as predictors of postoperative weight loss 2 years after bariatric surgery. Ann Behav Med. 2012;43:28–8. doi:10.1007/s11414-012-9277-z.
King WC, Chen JY, Mitchell JE, et al. Prevalence of alcohol use disorders before and after bariatric surgery. JAMA. 2012;307(23):2516–25. doi:10.1001/jama.2012.6147.PMID:22710289.
Conason A, Teixeira J, Hsu CH, et al. Substance use following bariatric weight loss surgery. JAMA. 2013;148(2):145–50.
Buffington CK. Alcohol use and health risks: Survey results. Bariatric Times. 2007; 4:21–23. http://bariatrictimes.com/2007/03/25/alcohol-use-and-health riskssurvey-results/. Accessed August 23, 2013.
Heinberg LJ, Ashton K, Coughlin J. Alcohol and bariatric surgery: review and suggested recommendations for assessment and management. Surg Obes Relat Dis. 2012;8(3):357–63. doi:10.1016/j.soard.2012.01.016.PMID:22425058.
Lent MR, Swencionis C. Addictive personality and maladaptive eating behaviors in adults seeking bariatric surgery. Eat Behav. 2012;13(1):67–70. doi:10.1016/j.eatbeh.2011.10.006.PMID:22177401.
Mechanick JI, Youdim A, Jones DB, et al. Clinical practice guidelines for the perioperative nutritional, metabolic and nonsurgical support of the bariatric surgery patient. Surg Obes Relat Dis. 2013;9(2):159–19. doi:10.1016/j.soard.2012.12.010.
Odom J, Zalesin KC, Washington TL, et al. Behavioral predictors of weight regain after bariatric surgery. Obes Surg. 2010;20(3):349–56. doi:10.1007/s11695-009-9895-6.PMID:19554382.
Hagedorn JC, Encarnacion B, Brat GA, et al. Does gastric bypass alter alcohol metabolism? Surg Obes Relat Dis. 2007;3(5):543–8.
Lieber CS. Metabolism of alcohol. Clin Liver Dis. 2005;9(1):1–35.
Kudsi OY, Huskey K, Grove S, et al. Prevalence of preoperative alcohol abuse among patients seeking weight-loss surgery. Surg Endosc. 2013;27(4):1093–7. doi:10.1007/s00464-012-2568-x.
Pinhão S, Poinhos R, Franchini B, et al. Nutritional intake of Portuguese population: energy, macronutrient and ethanol intake. Obes Facts. 2013;6(1):141–2. doi:10.1159/000170983.
Hasin DS, Stinson FS, Ogburn E, et al. Prevalence, correlates, disability and comorbidity of DSM-IV alcohol abuse and dependence in the United States: results from the National Epidemiologic Survey on Alcohol and Related Conditions. Arch Gen Psychiatry. 2007;64(7):830–42.
Naimi TS, Brewer RD, Mokdad A, et al. Binge drinking among US adults. JAMA. 2003;289(1):70–5.
Substance Abuse and Mental Health Services Administration. Results from the 2010 National Survey on Drug Use and Health: Summary of National Findings. Rockville, MD: Substance Abuse and Mental Health Services Administration, 2011.http://oas.samhsa.gov/NSDUH/. Accessed May 30, 2013.
Kleiner KD, Gold MS, Frost-Pineda K, et al. Body mass index and alcohol use. J Addict Dis. 2004;23(3):105–18.
Klockhoff H, Naslund I, Jones AW. Faster absorption of ethanol and higher peak concentration in women after gastric bypass surgery. J Clin Pharmacol. 2002;54(6):587–91.
Deitel M, Gawdat K, Melissa J. Reporting weight loss. Obes Surg. 2007;17(5):565–8.
Deitel M, Greenstein RJ. Recommendations for reporting weight loss. Obes Surg. 2003;13(2):159–60.
Reinhold RB. Critical analysis of long-term weight loss following gastric bypass. Surg Gynecol Obstet. 1982;155(3):385–64.
National Institute on Alcohol Abuse and Alcoholism. Patients who drink too much: Clinicians Guide 2005. Bethesda; 2005.www.niaaa.nih.gov/guide.Helping.Acessed August 20, 2013.
Wee CC, Mukamal KJ, Huskey KW, et al. Surg Obes Relat Dis. 2014;S1550-7289(14):6–9. doi:10.1016/j.soard.2013.12.014.
Ertelt TW, Mitchell JE, Lancaster K, et al. Alcohol abuse and dependence before and after bariatric surgery: a review of the literature and report of a new data set. Surg Obes Relat Dis. 2008;4(5):647–50. doi:10.1016/j.soard.2008.01.004.
Suzuki J, Haimovici F, Chang G. Alcohol use disorders after bariatric surgery. Obes Surg. 2012;22(2):201–7. doi:10.1007/s11695-010-0346-1.PMID:21188544.
Mitchell JE, Lancaster KL, Burgard MA, et al. Long-term follow-up of patients’ status after gastric bypass. Obes Surg. 2001;11(4):464–8.
Clark MM, Balsiger BM, Sletten CD, et al. Psychosocial factors and 2-year outcome following bariatric surgery for weight loss. Obes Surg. 2003;13(5):739–45.
Dixon JB, Dixon ME, O’Brien PE. Pre-operative predictors of weight loss at 1-year after lap-band surgery. Obes Surg. 2001;11(2):200–7.
Burgos MGPA, Medeiros MC, Bion FM, Pessoa DCNP. The effect of alcoholic beverages in nursing mothers and their impact on children. Rev Bras Saude Mater Infant. 2002;2(2):129–35. doi:10.1590/S1519-38292002000200005.
Burgos MGPA, Bion FM, Campos F. Lactação e álcool: efeitos clínicos e nutricionais. Arch Latino Am Nutr. 2004;54(1):25–35.
Conflict of Interest
All authors (Maria Goretti Pessoa de Araujo Burgos; Poliana Coelho Cabral; Regiane Maio; Bruno M. P. M. Oliveira; Margarida Sarmento Oliveira Dias; Diva Bizarro de Figueiredo Melim; and Maria Flora Correia) confirm that they have no conflict of interest.
Statement of Informed Consent
Informed consent was obtained from all individual participants included in the study.
Statement of Human Rights
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the Helsinki Declaration and its later amendments or comparable ethical standards.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
de Araujo Burgos, M.P., Cabral, P.C., Maio, R. et al. Prevalence of Alcohol Abuse Before and After Bariatric Surgery Associated With Nutritional and Lifestyle Factors: A Study Involving a Portuguese Population. OBES SURG 25, 1716–1722 (2015). https://doi.org/10.1007/s11695-015-1609-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-015-1609-7