Abstract
Objective
Dyslipidemia is associated with an increased risk of cardiovascular disease, the major cause of death in an aging population. This study aimed to estimate the prevalence of dyslipidemia for the past decade among adults in Wuhan, China.
Methods
We performed a serial cross-sectional study that recruited 705 219 adults from the Health Management Center of Tongji Hospital, Tongji Medical College, Huazhong University of Science and Technology from 2010 to 2019. The diagnosis of dyslipidemia was based on the 2016 Chinese Guidelines for the Management of Dyslipidemia in Adults. Fixed effects and random effects models were applied to adjust the confounding variables (gender and age).
Results
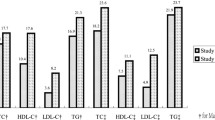
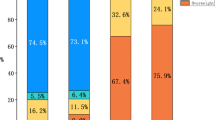
The overall prevalence of dyslipidemia was 33.1% (46.2% in men and 14.7% in women) in 2019. The prevalence of dyslipidemia was significantly increased over 10 years [from 28.6% (95% CI: 28.2%–29.1%) in 2010 to 32.8 % (95% CI:32.6%–33.1%) in 2019;. P–0.001], especially for hypo-high-density lipoprotein cholesterolemia [from 18.4% (95% CI: 18.0%–18.8%) in 2010 to 24.5% (95% CI: 24.3%–24.7%) in 2019; P–0.001]. In 2019, the prevalence of dyslipidemia was higher in participants with comorbidities, including overweight/obesity, hypertension, diabetes, hyperuricemia, or chronic kidney disease, and dyslipidemia was the most significant among participants aged 30–39 years.
Conclusion
This study demonstrated that dyslipidemia is on the rise in men, and more emphasis should be provided for the screening of dyslipidemia in young males for the primary prevention of cardiovascular and renal diseases.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Jiang Y, Ni W. Economic Evaluation of the 2016 Chinese Guideline and Alternative Risk Thresholds of Initiating Statin Therapy for the Management of Atherosclerotic Cardiovascular Disease. Pharmacoeconomics, 2019, 37(7): 943–952
Anderson TJ, Mancini GB, Genest J Jr, et al. The new dyslipidemia guidelines: what is the debate. Can J Cardiol, 2015, 31(5): 605–612
Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults. Executive Summary of The Third Report of The National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, And Treatment of High Blood Cholesterol In Adults (Adult Treatment Panel III). JAMA, 2001, 285(19): 2486–2497
Bauer UE, Briss PA, Goodman RA, et al. Prevention of chronic disease in the 21st century: elimination of the leading preventable causes of premature death and disability in the USA. Lancet, 2014, 384(9937): 45–52
Katsiki N, Mikhailidis DP, Mantzoros CS. Nonalcoholic fatty liver disease and dyslipidemia: An update. Metabolism, 2016, 65(8): 1109–1023
Maqbool M, Cooper ME, Jandeleit-Dahm KAM. Cardiovascular Disease and Diabetic Kidney Disease. Semin Nephrol, 2018, 38(3): 217–232
Zarvandi M, Rakhshandeh H, Abazari M, et al. Safety and efficacy of a polyherbal formulation for the management of dyslipidemia and hyperglycemia in patients with advanced-stage of type-2 diabetes. Biomed Pharmacother, 2017, 89: 69–75
Hager MR, Narla AD, Tannock LR. Dyslipidemia in patients with chronic kidney disease. Rev Endocr Metab Disord, 2017, 18(1): 29–40
Chávez-Talavera O, Tailleux A, Lefebvre P, et al. Bile Acid Control of Metabolism and Inflammation in Obesity, Type 2 Diabetes, Dyslipidemia, and Nonalcoholic Fatty Liver Disease. Gastroenterology, 2017, 152(7): 1679–1694
Gaggini M, Morelli M, Buzzigoli E, et al. Non-alcoholic fatty liver disease (NAFLD) and its connection with insulin resistance, dyslipidemia, atherosclerosis and coronary heart disease. Nutrients, 2013, 5(5): 1544–1560
Nepomuceno R, Vallerini BF, da Silva RL, et al. Systemic expression of genes related to inflammation and lipid metabolism in patients with dyslipidemia, type 2 diabetes mellitus and chronic periodontitis. Diabetes Metab Syndr, 2019, 13(4): 2715–2722
Zhou M, Wang H, Zeng X, et al. Mortality, morbidity, and risk factors in China and its provinces, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet, 2019, 394(10204): 1145–1158
Wang M, Liu M, Li F, et al. Gender heterogeneity in dyslipidemia prevalence, trends with age and associated factors in middle age rural Chinese. Lipids Health Dis, 2020, 19(1): 135
Song PK, Man QQ, Li H, et al. Trends in Lipids Level and Dyslipidemia among Chinese Adults, 2002–2015. Biomed Environ Sci, 2019, 32(8): 559–570
Thompson HR, Madsen KA. The Report Card on BMI Report Cards. Curr Obes Rep, 2017, 6(2): 163–167
Walsh EI, Shaw J, Cherbuin N. Trajectories of BMI change impact glucose and insulin metabolism. Nutr Metab Cardiovasc Dis, 2018, 28(3): 243–251
Vischer AS, Burkard T. Principles of Blood Pressure Measurement — Current Techniques, Office vs Ambulatory Blood Pressure Measurement. Adv Exp Med Biol, 2017, 956: 85–96
Petersmann A, Nauck M, Müller-Wieland D, et al. Definition, Classification and Diagnosis of Diabetes Mellitus. Exp Clin Endocrinol Diabetes, 2018, 126(7): 406–410
Liu H, Zhang XM, Wang YL, et al. Prevalence of hyperuricemia among Chinese adults: a national cross-sectional survey using multistage, stratified sampling. J Nephrol, 2014, 27(6): 653–658
Fernandez-Prado R, Castillo-Rodriguez E, Velez-Arribas FJ, et al. Creatinine Clearance Is Not Equal to Glomerular Filtration Rate and Cockcroft-Gault Equation Is Not Equal to CKD-EPI Collaboration Equation. Am J Med, 2016, 129(12): 1259–1263
Ko SH, Kim HS. Menopause-Associated Lipid Metabolic Disorders and Foods Beneficial for Post-menopausal Women. Nutrients, 2020, 12(1): 202
Klop B, Elte JW, Cabezas MC. Dyslipidemia in obesity: mechanisms and potential targets. Nutrients, 2013, 5(4): 1218–1240
Churilla JR, Johnson TM, Curls R, et al. Association between alcohol consumption patterns and metabolic syndrome. Diabetes Metab Syndr, 2014, 8(2): 119–123
Blum B, Wormack L, Holtel M, et al. Gender and thrombolysis therapy in stroke patients with incidence of dyslipidemia. BMC Womens Health, 2019, 19(1): 11
Franssen R, Monajemi H, Stroes ES, et al. Obesity and dyslipidemia. Med Clin North Am, 2011, 95(5): 893–902
Peters U, Dixon AE, Forno E. Obesity and asthma. J Allergy Clin Immunol. 2018,141(4):1169–1179
Broughton DE, Moley KH. Obesity and female infertility: potential mediators of obesity’s impact. Fertil Steril, 2017, 107(4): 840–847
McCracken E, Monaghan M, Sreenivasan S. Pathophysiology of the metabolic syndrome. Clin Dermatol, 2018, 36(1): 14–20
Gluvic Z, Zaric B, Resanovic I, et al. Link between Metabolic Syndrome and Insulin Resistance. Curr Vasc Pharmacol, 2017, 15(1): 30–39
Carrier A. Metabolic Syndrome and Oxidative Stress: A Complex Relationship. Antioxid Redox Signal, 2017, 26(9): 429–431
Vekic J, Zeljkovic A, Stefanovic A, et al. Obesity and dyslipidemia. Metabolism, 2019, 92: 71–81
Hirano T. Pathophysiology of Diabetic Dyslipidemia. J Atheroscler Thromb, 2018, 25(9): 771–778.
Radikova Z, Penesova A, Vlcek M, et al. LDL and HDL lipoprotein subfractions in multiple sclerosis patients with decreased insulin sensitivity. Endocr Regul, 2018, 52(3): 139–145
Ikezaki H, Furusyo N, Yokota Y, et al. Small Dense Low-Density Lipoprotein Cholesterol and Carotid Intimal Medial Thickness Progression. J Atheroscler Thromb, 2020, 27(10): 1108–1122
Gansevoort RT, Correa-Rotter R, Hemmelgarn BR, et al. Chronic kidney disease and cardiovascular risk: epidemiology, mechanisms, and prevention. Lancet, 2013, 382(9889): 339–352
Tietge UJ. Hyperlipidemia and cardiovascular disease: inflammation, dyslipidemia, and atherosclerosis. Curr Opin Lipidol, 2014, 25(1): 94–95
Ahn N, Kim K. High-density lipoprotein cholesterol (HDL-C) in cardiovascular disease: effect of exercise training. Integr Med Res, 2016, 5(3): 212–215
Koncsos P, Fülöp P, Juhász I, et al. Changes in triglyceride, HDL-C, and non-HDL-C levels in patients with acute coronary syndrome. Wien Klin Wochenschr, 2016, 128(23–24): 858–863
Haitao T, Vermunt JV, Abeykoon J, et al. COVID-19 and Sex Differences: Mechanisms and Biomarkers. Mayo Clin Proc, 2020, 95(10): 2189–2203
Enani S, Bahijri S, Malibary M, et al. The Association between Dyslipidemia, Dietary Habits and Other Lifestyle Indicators among Non-Diabetic Attendees of Primary Health Care Centers in Jeddah, Saudi Arabia. Nutrients, 2020, 12(8): 2441
Du D, Bruno R, Blizzard L, et al. The metabolomic signatures of alcohol consumption in young adults. Eur J Prev Cardiol, 2020, 27(8): 840–849
Acknowledgments
The authors declare that there is no conflict of interest with any financial organization or corporation or individual that can inappropriately influence this work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Zhang, M., Wan, Zc., Lv, Ym. et al. Ten-year Time-trend Analysis of Dyslipidemia Among Adults in Wuhan. CURR MED SCI 42, 1099–1105 (2022). https://doi.org/10.1007/s11596-022-2630-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11596-022-2630-4