Abstract
Purpose
To evaluate the diagnostic value of MRI-guided contrast-enhanced ultrasound (CEUS) for prostate cancer (PCa) diagnosis, and characteristics of PCa in qualitative and quantitative CEUS.
Material and methods
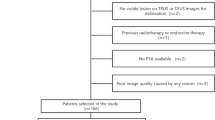
This prospective and multicenter study included 250 patients (133 in the training cohort, 57 in the validation cohort and 60 in the test cohort) who underwent MRI, MRI-guided CEUS and prostate biopsy between March 2021 and February 2023. MRI interpretation, qualitative and quantitative CEUS analysis were conducted. Multitree extreme gradient boosting (XGBoost) machine learning-based models were applied to select the eight most important quantitative parameters. Univariate and multivariate logistic regression models were constructed to select independent predictors of PCa. Diagnostic value was determined for MRI, qualitative and quantitative CEUS using the area under receiver operating characteristic curve (AUC).
Results
The performance of quantitative CEUS was superior to that of the qualitative CEUS and MRI in predicting PCa. The AUC was 0.779 (95%CI 0.70–0.849), 0.756 (95%CI 0.638–0.874) and 0.759 (95%CI 0.638–0.879) of qualitative CEUS, and 0.885 (95%CI 0.831–0.940), 0.802 (95%CI 0.684–0.919) and 0.824 (95%CI 0.713–0.936) of quantitative CEUS in training, validation and test cohort, respectively. Compared with quantitative CEUS, MRI achieved less well performance for AUC 0.811 (95%CI 0.741–0.882, p = 0.099), 0.748 (95%CI 0.628–0.868, p = 0.539) and 0.737 (95%CI 0.602–0.873, p = 0.029), respectively. Moreover, the highest specificity of 80.6% was obtained by quantitative CEUS.
Conclusion
We developed a reliable method of MRI-guided CEUS that demonstrated enhanced performance compared to MRI. The qualitative and quantitative CEUS characteristics will contribute to improved diagnosis of PCa.






Similar content being viewed by others
Abbreviations
- AUC:
-
Area under the curve
- CEUS:
-
Contrast-enhanced ultrasound
- csPCa:
-
Clinically significant prostate cancer
- DCA:
-
Decision curve analysis
- mp-MRI:
-
Multiparameter magnetic resonance imaging
- nsPCa:
-
Non-clinically significant prostate cancer
- PCa:
-
Prostate cancer
- PI-RADS:
-
Prostate imaging reporting and data system
- ROC:
-
Receiver operating curve
- ROI:
-
Region of interest
- TTP:
-
Time to peak
- US:
-
Ultrasound
- WoR:
-
Washout rate
References
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, Bray F (2021) Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 71(3):209–249
Kiebish MA, Tekumalla P, Ravipaty S, Dobi A, Srivastava S, Wu W, Patil S, Friss T, Klotz A, Srinivasan A, Cullen J, Rosner IL, Ali A, Laszlo S, Petrovic M, Fleshner N, Garren J, Miller G, Mahaveer Chand N, Rodrigues LO, Granger E, Kellogg MD, Luan S, Diamandis E, Akmaev VR, Sarangarajan R, Bountra C, Freedland SJ, McLeod DG, Narain NR (2021) Clinical utility of a serum biomarker panel in distinguishing prostate cancer from benign prostate hyperplasia. Sci Rep 11(1):15052
Butler SS, Muralidhar V, Zhao SG, Sanford NN, Franco I, Fullerton ZH, Chavez J, D’Amico AV, Feng FY, Rebbeck TR, Nguyen PL, Mahal BA (2020) Prostate cancer incidence across stage, NCCN risk groups, and age before and after USPSTF grade D recommendations against prostate-specific antigen screening in 2012. Cancer 126(4):717–724
Ahdoot M, Wilbur AR, Reese SE, Lebastchi AH, Mehralivand S, Gomella PT, Bloom J, Gurram S, Siddiqui M, Pinsky P, Parnes H, Linehan WM, Merino M, Choyke PL, Shih JH, Turkbey B, Wood BJ, Pinto PA (2020) MRI-targeted, systematic, and combined biopsy for prostate cancer diagnosis. N Engl J Med 382(10):917–928
Ahmed HU, El-Shater Bosaily A, Brown LC, Gabe R, Kaplan R, Parmar MK, Collaco-Moraes Y, Ward K, Hindley RG, Freeman A, Kirkham AP, Oldroyd R, Parker C, Emberton M (2017) Diagnostic accuracy of multi-parametric MRI and TRUS biopsy in prostate cancer (PROMIS): a paired validating confirmatory study. Lancet 389(10071):815–822
Pagniez MA, Kasivisvanathan V, Puech P, Drumez E, Villers A, Olivier J (2020) Predictive factors of missed clinically significant prostate cancers in men with negative magnetic resonance imaging: a systematic review and meta-analysis. J Urol 204(1):24–32
Annamalai A, Fustok JN, Beltran-Perez J, Rashad AT, Krane LS, Triche BL (2022) Interobserver agreement and accuracy in interpreting mpMRI of the prostate: a systematic review. Curr Urol Rep 23(1):1–10
Borofsky S, George AK, Gaur S, Bernardo M, Greer MD, Mertan FV, Taffel M, Moreno V, Merino MJ, Wood BJ, Pinto PA, Choyke PL, Turkbey B (2018) What are we missing? False-negative cancers at multiparametric MR imaging of the prostate. Radiology 286(1):186–195
Zhang J, Xu L, Zhang G, Zhang X, Bai X, Sun H, Jin Z (2023) Effects of dynamic contrast enhancement on transition zone prostate cancer in prostate imaging reporting and data system version 2.1. Radiol Oncol
Salib A, Halpern E, Eisenbrey J, Chandrasekar T, Chung PH, Forsberg F, Trabulsi EJ (2022) The evolving role of contrast-enhanced ultrasound in urology: a review. World J Urol
Yang G, Ruan L (2022) Imaging findings of prostate tuberculosis by transrectal contrast-enhanced ultrasound and comparison with 2D ultrasound and pathology. Br J Radiol 95(1129):20210713
Jung EM, Wertheimer T, Putz FJ, Jung F, Kammerer S, Pregler B, Luerken L, Stroszczynski C, Beyer L (2020) Contrast enhanced ultrasound (CEUS) with parametric imaging and time intensity curve analysis (TIC) for evaluation of the success of prostate arterial embolization (PAE) in cases of prostate hyperplasia. Clin Hemorheol Microcirc 76(2):143–153
Wink M, Frauscher F, Cosgrove D, Chapelon JY, Palwein L, Mitterberger M, Harvey C, Rouvière O, de la Rosette J, Wijkstra H (2008) Contrast-enhanced ultrasound and prostate cancer; a multicentre European research coordination project. Eur Urol 54(5):982–992
Sidhu PS, Cantisani V, Dietrich CF, Gilja OH, Saftoiu A, Bartels E, Bertolotto M, Calliada F, Clevert DA, Cosgrove D, Deganello A, D’Onofrio M, Drudi FM, Freeman S, Harvey C, Jenssen C, Jung EM, Klauser AS, Lassau N, Meloni MF, Leen E, Nicolau C, Nolsoe C, Piscaglia F, Prada F, Prosch H, Radzina M, Savelli L, Weskott HP, Wijkstra H (2018) The EFSUMB guidelines and recommendations for the clinical practice of contrast-enhanced ultrasound (CEUS) in non-hepatic applications: update 2017 (Long Version). Ultraschall Med 39(2):e2–e44
Turkbey B, Rosenkrantz AB, Haider MA, Padhani AR, Villeirs G, Macura KJ, Tempany CM, Choyke PL, Cornud F, Margolis DJ, Thoeny HC, Verma S, Barentsz J, Weinreb JC (2019) Prostate imaging reporting and data system version 2.1: 2019 update of prostate imaging reporting and data system version 2. Eur Urol 76(3):340–351
Epstein JI, Egevad L, Amin MB, Delahunt B, Srigley JR, Humphrey PA (2016) The 2014 international society of urological pathology (ISUP) consensus conference on gleason grading of prostatic carcinoma: definition of grading patterns and proposal for a new grading system. Am J Surg Pathol 40(2):244–252
Sano F, Terao H, Kawahara T, Miyoshi Y, Sasaki T, Noguchi K, Kubota Y, Uemura H (2011) Contrast-enhanced ultrasonography of the prostate: various imaging findings that indicate prostate cancer. BJU Int 107(9):1404–1410
Wildeboer RR, Mannaerts CK, van Sloun RJG, Budäus L, Tilki D, Wijkstra H, Salomon G, Mischi M (2020) Automated multiparametric localization of prostate cancer based on B-mode, shear-wave elastography, and contrast-enhanced ultrasound radiomics. Eur Radiol 30(2):806–815
Liu G, Wu S, Huang L (2020) Contrast-enhanced ultrasound evaluation of the prostate before transrectal ultrasound-guided biopsy can improve diagnostic sensitivity: a STARD-compliant article. Medicine 99(19):e19946
Grey ADR, Scott R, Shah B, Acher P, Liyanage S, Pavlou M, Omar R, Chinegwundoh F, Patki P, Shah TT, Hamid S, Ghei M, Gilbert K, Campbell D, Brew-Graves C, Arumainayagam N, Chapman A, McLeavy L, Karatziou A, Alsaadi Z, Collins T, Freeman A, Eldred-Evans D, Bertoncelli-Tanaka M, Tam H, Ramachandran N, Madaan S, Winkler M, Arya M, Emberton M, Ahmed HU (2022) Multiparametric ultrasound versus multiparametric MRI to diagnose prostate cancer (CADMUS): a prospective, multicentre, paired-cohort, confirmatory study. Lancet Oncol 23(3):428–438
Kunz P, Kiesl S, Groß S, Kauczor HU, Schmidmaier G, Fischer C (2020) Intra-observer and device-dependent inter-observer reliability of contrast-enhanced ultrasound for muscle perfusion quantification. Ultrasound Med Biol 46(2):275–285
Postema AW, Frinking PJ, Smeenge M, De Reijke TM, De la Rosette JJ, Tranquart F, Wijkstra H (2016) Dynamic contrast-enhanced ultrasound parametric imaging for the detection of prostate cancer. BJU Int 117(4):598–603
Weinreb JC, Barentsz JO, Choyke PL, Cornud F, Haider MA, Macura KJ, Margolis D, Schnall MD, Shtern F, Tempany CM, Thoeny HC, Verma S (2016) PI-RADS prostate imaging-reporting and data system: 2015, Version 2. Eur Urol 69(1):16–40
Pang X, Zhang J, Chen L, Yuan Y, Xu D (2022) Study on the diagnostic value of contrast-enhanced ultrasound and magnetic resonance imaging in prostate cancer. Evid Based Complement Alternat Med 2022:7983530
Sato T, Isoda H, Fujimoto K, Furuta A, Fujimoto M, Ito K, Kobayashi T, Nakamoto Y (2021) Evaluation of weighted diffusion subtraction for detection of clinically significant prostate cancer. J Magn Reson Imag 54(6):1979–1988
Maxeiner A, Fischer T, Schwabe J, Baur ADJ, Stephan C, Peters R, Slowinski T, von Laffert M, Marticorena Garcia SR, Hamm B, Jung EM (2019) Contrast-enhanced ultrasound (CEUS) and quantitative perfusion analysis in patients with suspicion for prostate cancer. Ultraschall Med 40(3):340–348
Jung EM, Wiggermann P, Greis C, Eder F, Ehrich J, Jung W, Schreyer AG, Stroszczynski C, Ganzer R (2012) First results of endocavity evaluation of the microvascularization of malignant prostate tumors using contrast enhanced ultrasound (CEUS) including perfusion analysis: first results. Clin Hemorheol Microcirc 52(2–4):167–177
Acknowledgements
We thank all the participants in this study.
Funding
This study has received funding by National Natural Science Foundation of China (Grants No. 82171942, 82371971, 82202153 and 82202154) and the foundations of National Key R&D Program of China (Grant No. 2022YFF0606304).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors disclose no conflicts of interest.
Ethical approval
Institutional Review Board approval was obtained.
Informed consent
Written informed consent was only obtained from prospectively enrolled patients in this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Liu, Y., Lu, D., Xu, G. et al. Diagnostic accuracy of qualitative and quantitative magnetic resonance imaging-guided contrast-enhanced ultrasound (MRI-guided CEUS) for the detection of prostate cancer: a prospective and multicenter study. Radiol med 129, 585–597 (2024). https://doi.org/10.1007/s11547-024-01758-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11547-024-01758-2