Abstract
Purpose
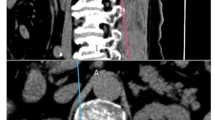
Percutaneous vertebroplasty (PVP) is a minimally invasive treatment for symptomatic vertebral compression fractures (VCFs). The aim of this study was to assess the effectiveness, complications and progress of results of PVP optimized in terms of technique, costs, time and strategic protocol after 3 years of procedures performed under fluoroscopic guidance alone.
Materials and methods
We treated 250 VCFs in 120 consecutive patients after assessing clinical and radiological indications. The effectiveness of the procedure was determined by statistical analysis of numerical scores for pain, mobility and drug consumption before and after treatment.
Results
No major complications and only three minor complications occurred. Clinically relevant improved mobility and reduction of pain and analgesics were observed, with overall significant results (p<0.0001) in all patients at 24 h after PVP and in 83 available patients at 6 months. A total of five asymptomatic refractures of cemented vertebrae and 14 new symptomatic vertebral fractures at different levels were observed between 1 and 10 months after the procedure.
Conclusions
PVP is a safe, rapid, effective and costeffective therapy for VCFs, requiring only brief hospital admission and with long-lasting clinical results, when performed under good-quality radiological guidance, when correct indications are respected and when it is associated with rehabilitation therapy in the follow-up. It is a valid alternative to conservative therapy, which is burdened by high healthcare costs and often requires long-term immobilisation of frail and elderly patients at risk of clinical complications.
Riassunto
Obiettivo
La vertebroplastica percutanea (VPP) è un trattamento mininvasivo per le fratture vertebrali sintomatiche da compressione (FVC). Scopo del presente lavoro è quello di valutare l’efficacia, le complicanze e la progressione dei risultati della VPP ottimizzata in termini di tecnica, costi, tempi e protocollo strategico dopo 3 anni di procedure effettuate sotto esclusiva guida fluoroscopica.
Materiali e metodi
Sono state trattate 250 FVC in 120 pazienti consecutivi dopo valutazione delle indicazioni cliniche e radiologiche. L’efficacia della procedura è stata determinata attraverso l’analisi statistica di score numerici per il dolore, la mobilità e l’uso di farmaci antalgici prima e dopo il trattamento.
Risultati
Non si sono verificate complicanze maggiori e solo 3 complicanze minori. È stato osservato un miglioramento della mobilità e riduzione del dolore e dell’uso di farmaci antalgici clinicamente rilevanti con risultati significativi (p<0,0001) in tutti i pazienti a 24 ore dalla VPP e, in 83 pazienti reperibili, a distanza di 6 mesi. Sono stati rilevati 5 nuovi cedimenti asintomatici in vertebre precedentemente trattate e 14 nuove fratture sintomatiche su livelli differenti da 1 a 10 mesi dopo la procedura.
Conclusioni
La VPP costituisce un trattamento sicuro, rapido, efficace, poco costoso, che richiede solo un ricovero breve e con risultati clinici duraturi qualora sia impiegato un sistema di guida radiologica di buona qualità, siano rispettate le corrette indicazioni e venga associata una terapia riabilitativa nel follow-up. Rappresenta una valida alternativa alla terapia conservativa, quest’ultima gravata da elevati costi sanitari e che richiede spesso l’immobilizzazione prolungata di pazienti fragili e anziani, a rischio di complicanze cliniche.
Similar content being viewed by others
References/Bibliografia
Anselmetti GC, Corrao G, Della Monica P et al (2007) Pain relief following percutaneous vertebroplasty: results of a series of 283 consecutive patients treated in a single institution. Cardiovasc Intervent Radiol 30:441–447
McGraw JK, Cardella J, Barr JD et al (2003) Society of Interventional Radiology quality improvement guidelines for percutaneous vertebroplasty. J Vasc Intervent Radiol 14:S311–S315
Kanis JA and Johnell O (2005) Requirements for DXA for the management of osteoporosis in Europe. Osteoporos Int 16:229
DaFonseca K, Baier M, Grafe I et al (2006) Balloon kyphoplasty in the therapy of vertebral fractures. Orthopade 35:1101–1109
Shen M, Kim Y (2007) Osteoporotic vertebral compression fractures: a review of current surgical management techniques. Am J Orthop 36:241–248
Kado DM, Browner WS, Palermo L et al (1999) Vertebral fractures and mortality in older women: a prospective study. Study of Osteoporotic Fractures Research Group. Arch Intern Med 159:1215–1220
Deen HG (2006) Current status of percutaneous vertebral augmentation techniques for vertebral compression fractures. Neurol Neurochir Pol 40:320–326
Ross P (1997) Clinical consequences of vertebral fractures. Am J Med 103:30S–43S
Gangi A, Sabharwal T, Irani FG et al (2006) Quality assurance guidelines for percutaneous vertebroplasty. Cardiovasc Intervent Radiol 29:173–178
Do HM, Kim BS, Marcellus ML et al (2005) Prospective analysis of clinical outcomes after percutaneous vertebroplasty for painful osteoporotic vertebral body fractures. AJNR Am J Neuroradiol 26:1623–1628
Galibert P, Deramond H, Rosat P et al (1987) Preliminary note on the treatment of vertebral angioma by percutaneous acrylic vertebroplasty. Neurochirurgie 33:166–168
Wu CC, Lin MH, Yang SH et al (2007) Surgical removal of extravasated epidural and neuroforaminal polymethylmethacrylate after percutaneous vertebroplasty in the thoracic spine. Eur Spine J 16(Suppl 3):326–331
Freitag M, Gottschalk A, Schuster M et al (2006) Pulmonary embolism caused by polymethylmethacrylate during percutaneous vertebroplasty in orthopaedic surgery. Acta Anaesthesiol Scand. 50:248–251
Hoffmann RT, Jakobs TF, Trumm C et al (2007) Vertebroplasty in the treatment of osteoporotic vertebral body fracture. Eur Radiol 17:2656–2662
Layton KF, Thielen KR, Koch CA et al (2007) Vertebroplasty, first 1000 levels of a single center: evaluation of the outcomes and complications. AJNR Am J Neuroradiol 28:683–689
Mathis JM, Barr JD, Belkoff SM et al (2001) Percutaneous vertebroplasty: a developing standard of care for vertebral compression fractures. AJNR Am J Neuroradiol 22:373–381
Website of the Ministry of Health www.ministerosalute.it/dispositivi/paginainterna.jsp?id=88&menu=commissione
Cotten A, Boutry N, Cortet B et al (1998) Percutaneous vertebroplasty: state of the art. RadioGraphics 18:311–320
Syed MI, Jan S, Patel NA et al (2006) Fatal fat embolism after vertebroplasty: identification of the high-risk patient. AJNR Am J Neuroradiol 27:343–345
Syed MI, Shaikh A (2007) Vertebroplasty: a systematic approach. Pain Physician 10:367–380
Muto M, Perrotta V, Guarnieri G et al (2008) Vertebroplasty and kyphoplasty: friends or foes? Radiol Med (Torino) 113:1171–1184
Kaufmann TJ, Jensen ME, Schweickert PA et al (2001) Age of fracture and clinical outcomes of percutaneous vertebroplasty. AJNR Am J Neuroradiol 22:1860–1863
Kobayashi K, Shimoyama K, Nakamura K et al (2005) Percutaneous vertebroplasty immediately relieves pain of osteoporotic vertebral compression fractures and prevents prolonged immobilization of patients. Eur Radiol 15:360–367
Syed MI, Patel NA, Jan S et al (2005) New symptomatic vertebral compression fractures within a year following vertebroplasty in osteoporotic women. AJNR Am J Neuroradiol 26:1601–1604
Tanigawa N, Komemushi A, Kariya S et al (2006) Radiological follow-up of new compression fractures following percutaneous vertebroplasty. Cardiovasc Intervent Radiol 29:92–96
Lindsay R, Silverman LS, Cooper C et al (2001) Risk of new vertebral fracture in the year following a fracture. JAMA 285:320–323
Kim SH, Kang HS, Choi JA et al (2004) Risk factors of new compression fractures in adjacent vertebrae after percutaneous vertebroplasty. Acta Radiol 45:440–445
Komemushi A, Tanigawa N, Kariya S et al (2006) Percutaneous vertebroplasty for osteoporotic compression fracture: multivariate study of predictors of new vertebral body fracture. Cardiovasc Intervent Radiol 29:580–585
Lin WC, Lee YC, Lee CH et al (2008) Refractures in cemented vertebrae after percutaneous vertebroplasty: a retrospective analysis. Eur Spine J 17:592–599
Baroud G, Bohner M (2006) Biomechanical impact of vertebroplasty. Postoperative biomechanics of vertebroplasty. Joint Bone Spine 73:144–150
Barbero S, Casorzo I, Durando M et al (2008) Percutaneous vertebroplasty: the follow-up. Radiol Med (Torino) 113:101–113
Jasiak-Tyrkalska B, Czerwifski E (2006) Physiotherapeutical management after osteoporotic fractures. Ortop Traumatol Rehabil 8:388–394
Huntoon EA, Schmidt CK, Sinaki M (2008) Significantly fewer refractures after vertebroplasty in patients who engage in back-extensor-strengthening exercises. Mayo Clin Proc 83:54–57
Caudana R, Renzi Brivio L, Ventura L et al (2008) CT-guided percutaneous vertebroplasty: personal experience in the treatment of osteoporotic fractures and dorsolumbar metastases. Radiol Med (Torino) 113:114–133
Diamond TH, Bryant C, Browne L et al (2006) Clinical outcomes after acute osteoporotic vertebral fractures: a 2-year non-randomised trial comparing percutaneous vertebroplasty with conservative therapy. Med J Aust 184:113–117
Nakano M, Hirano N, Ishihara H et al (2006) Calcium phosphate cementbased vertebroplasty compared with conservative treatment for osteoporotic compression fractures: a matched case-control study. J Neurosurg Spine 4:110–117
Voormolen MH, Mali WP, Lohle PN et al (2007) Percutaneous vertebroplasty compared with optimal pain medication treatment: short-term clinical outcome of patients with subacute or chronic painful osteoporotic vertebral compression fractures. The VERTOS study. AJNR Am J Neuroradiol 28:555–560
Farrar JT, Young JP, LaMoreaux L et al (2001) Clinical importance of changes in chronic pain intensity measured on an 11-point numerical pain rating scale. Pain 94:149–158
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Pedicelli, A., Rollo, M., Piano, M. et al. Percutaneous vertebroplasty: optimizing the procedure after treatment of 250 vertebral levels under fluoroscopic guidance. Radiol med 114, 1141–1158 (2009). https://doi.org/10.1007/s11547-009-0448-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11547-009-0448-9