Abstract
Objectives
Night-shift work exposure is proposed to link to a wide range of health issues, especially cancer incidence, cancer-specific death, and all-cause death. However, the epidemiological associations among night-shift work exposure, breast cancer, breast cancer-specific death, and all-cause mortality remain inconclusive.
Methods
We performed an updated systematic review and meta-analysis to confirm potential associations among night-shift work exposure, breast cancer, and all-cause mortality.
Results
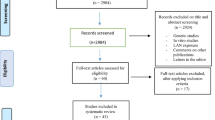
A total of 31 prospective cohort studies, involving 9.3 million participants, 31,244 incident breast cancer cases, 12,728 cancer-related deaths, 7882 cardiovascular deaths, and 30,807 all-cause mortalities were included. Overall, the summary RR of incident breast cancer in females for an increase of night-shift work was 1.029 (95% CI 1.003–1.055). Compared with standard day workers, night-shift workers had a statistically significantly increased RR (1.086, 95% CI 1.032–1.142) for breast cancer incidence in the subgroup of > 10 years exposure. Furthermore, a positive association was revealed in subgroup studies of rotating night-shift work (RR = 1.053, 95% CI 1.018–1.090). A significant increased risk of cardiovascular mortality was demonstrated in the night-shift work group (RR = 1.031; 95% CI 1.006–1.057).
Conclusion
Our systematic review and meta-analysis provided convincing evidence supporting positive associations among night-shift work exposure, breast cancer incidence, and cardiovascular mortality. Taken together, night-shift work exposure significantly increased the risk of breast cancer morbidity by 2.9% for total, 8.6% for the subgroup of more than 10 years night-shift work, and 5.3% for rotating night-shift work. In addition, night-shift work increased the risk of cardiovascular mortality by 3.1%.





Similar content being viewed by others
References
Wei T, Li C, Heng Y, Gao X, Zhang G, Wang H, Zhao X, Meng Z, Zhang Y, Hou H (2020) Association between night-shift work and level of melatonin: systematic review and meta-analysis. Sleep Med 75:502–509
Booker LA, Magee M, Rajaratnam SMW, Sletten TL, Howard ME (2018) Individual vulnerability to insomnia, excessive sleepiness and shift work disorder amongst healthcare shift workers A systematic review. Sleep Med Rev 41:220–233
Megdal SP, Kroenke CH, Laden F, Pukkala E, Schernhammer ES (2005) Night work and breast cancer risk: a systematic review and meta-analysis. Eur J Cancer 41:2023–2032
Jia Y, Lu Y, Wu K, Lin Q, Shen W, Zhu M, Huang S, Chen J (2013) Does night work increase the risk of breast cancer? A systematic review and meta-analysis of epidemiological studies. Cancer Epidemiol 37:197–206
Wang F, Yeung KL, Chan WC, Kwok CC, Leung SL, Wu C, Chan EY, Yu IT, Yang XR, Tse LA (2013) A meta-analysis on dose-response relationship between night shift work and the risk of breast cancer. Ann Oncol 24:2724–2732
Benabu JC, Stoll F, Gonzalez M, Mathelin C (2015) Night work, shift work: breast cancer risk factor? Gynecol Obstet Fertil 43:791–799
He C, Anand ST, Ebell MH, Vena JE, Robb SW (2015) Circadian disrupting exposures and breast cancer risk: a meta-analysis. Int Arch Occup Environ Health 88:533–547
Liu W, Zhou Z, Dong D, Sun L, Zhang G (2018) Sex differences in the association between night shift work and the risk of cancers: a meta-analysis of 57 articles. Dis Markers 2018:7925219
Ijaz S, Verbeek J, Seidler A, Lindbohm M-L, Ojajarvi A, Orsini N, Costa G, Neuvonen K (2013) Night-shift work and breast cancer - a systematic review and meta-analysis. Scand J Work Environ Health 39:431–447
Kamdar BB, Tergas AI, Mateen FJ, Bhayani NH, Oh J (2013) Night-shift work and risk of breast cancer: a systematic review and meta-analysis. Breast Cancer Res Treat 138:291–301
Pahwa M, Labreche F, Demers PA (2018) Night shift work and breast cancer risk: what do the meta-analyses tell us? Scand J Work Environ Health 44:432–435
Salamanca-Fernandez E, Rodriguez-Barranco M, Guevara M, Ardanaz E, de Labry O, Lima A, Sanchez MJ (2018) Night-shift work and breast and prostate cancer risk: updating the evidence from epidemiological studies. An Sist Sanit Navar 41:211–226
Dun A, Zhao X, Jin X, Wei T, Gao X, Wang Y, Hou H (2020) Association between night-shift work and cancer risk: updated systematic review and meta-analysis. Front Oncol 10:1006–1020
Lin X, Chen W, Wei F, Ying M, Wei W, Xie X (2015) Night-shift work increases morbidity of breast cancer and all-cause mortality: a meta-analysis of 16 prospective cohort studies. Sleep Med 16:1381–1387
Schernhammer ES, Laden F, Speizer FE, Willett WC, Hunter DJ, Kawachi I, Colditz GA (2001) Rotating night shifts and risk of breast cancer in women participating in the Nurses’ Health Study. J Natl Cancer Inst 93:1563–1568
Schernhammer ES, Kroenke CH, Laden F, Hankinson SE (2006) Night work and risk of breast cancer. Epidemiology 17:108–111
Pronk A, Ji BT, Shu XO, Xue S, Yang G, Li HL, Rothman N, Gao YT, Zheng W, Chow WH (2010) Night-shift work and breast cancer risk in a cohort of Chinese women. Am J Epidemiol 171:953–959
Knutsson A, Alfredsson L, Karlsson B, Akerstedt T, Fransson EI, Westerholm P, Westerlund H (2013) Breast cancer among shift workers: results of the WOLF longitudinal cohort study. Scand J Work Environ Health 39:170–177
Koppes LL, Geuskens GA, Pronk A, Vermeulen RC, de Vroome EM (2014) Night work and breast cancer risk in a general population prospective cohort study in The Netherlands. Eur J Epidemiol 29:577–584
Schernhammer E (2014) 0359 Nighshift work and breast cancer risk - good news, bad news ? Occup Environ Med 71(Suppl 1):A121
Travis RC, Balkwill A, Fensom GK, Appleby PN, Reeves GK, Wang XS, Roddam AW, Gathani T, Peto R, Green J et al (2016) Night shift work and breast cancer incidence: three prospective studies and meta-analysis of published studies. J Natl Cancer Inst 108:djw169
Fritschi L, Valerie Gross J, Wild U, Heyworth JS, Glass DC, Erren TC (2018) Shift work that involves circadian disruption and breast cancer: a first application of chronobiological theory and the consequent challenges. Occup Environ Med 75:231–234
Yang W, Shi Y, Ke X, Sun H, Guo J, Wang X (2019) Long-term sleep habits and the risk of breast cancer among Chinese women: a case-control study. Eur J Cancer Prev 28:323–329
James P, Bertrand KA, Hart JE, Schernhammer ES, Tamimi RM, Laden F (2017) Outdoor light at night and breast cancer incidence in the Nurses’ Health Study II. Environ Health Perspect 125:087010–087020
Vistisen HT, Garde AH, Frydenberg M, Christiansen P, Hansen AM, Andersen J, Bonde JP, Kolstad HA (2017) Short-term effects of night shift work on breast cancer risk: a cohort study of payroll data. Scand J Work Environ Health 43:59–67
Wegrzyn LR, Tamimi RM, Rosner BA, Brown SB, Stevens RG, Eliassen AH, Laden F, Willett WC, Hankinson SE, Schernhammer ES (2017) Rotating night-shift work and the risk of breast cancer in the Nurses’ Health Studies. Am J Epidemiol 186:532–540
White AJ, Weinberg CR, Park YM (2017) Sleep characteristics, light at night and breast cancer risk in a prospective cohort. Int J Cancer 141:2204–2214
Andersen ZJ, Jorgensen JT, Elsborg L, Lophaven SN, Backalarz C, Laursen JE, Pedersen TH, Simonsen MK, Brauner EV, Lynge E (2018) Long-term exposure to road traffic noise and incidence of breast cancer: a cohort study. Breast Cancer Res 20:119–131
Jones ME, Schoemaker MJ, McFadden EC, Wright LB, Johns LE, Swerdlow AJ (2019) Night shift work and risk of breast cancer in women: the Generations Study cohort. Br J Cancer 121:172–179
Sweeney MR, Sandler DP, Niehoff NM, White AJ (2020) Shift work and working at night in relation to breast cancer incidence. Cancer Epidemiol Biomarkers Prev 29:687–689
Gu F, Han J, Laden F, Pan A, Caporaso NE, Stampfer MJ, Kawachi I, Rexrode KM, Willett WC, Hankinson SE et al (2015) Total and cause-specific mortality of U.S. nurses working rotating night shifts. Am J Prev Med 48:241–252
Dickerman BA, Markt SC, Koskenvuo M, Hublin C, Pukkala E, Mucci LA, Kaprio J (2016) Sleep disruption, chronotype, shift work, and prostate cancer risk and mortality: a 30-year prospective cohort study of Finnish twins. Cancer Causes Control 27:1361–1370
Trudel-Fitzgerald C, Zhou ES, Poole EM, Zhang X, Michels KB, Eliassen AH, Chen WY, Holmes MD, Tworoger SS, Schernhammer ES (2017) Sleep and survival among women with breast cancer: 30 years of follow-up within the Nurses’ Health Study. Br J Cancer 116:1239–1246
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ 339:b2535-2539
Li W, Ray RM, Thomas DB, Davis S, Yost M, Breslow N, Gao DL, Fitzgibbons ED, Camp JE, Wong E et al (2015) Shift work and breast cancer among women textile workers in Shanghai, China. Cancer Causes Control 26:143–150
Akerstedt T, Knutsson A, Narusyte J, Svedberg P, Kecklund G, Alexanderson K (2015) Night work and breast cancer in women: a Swedish cohort study. BMJ Open 5:e008127
Kawachi I, Colditz GA, Stampfer MJ, Willett WC, Manson JE, Speizer FE, Hennekens CH (1995) Prospective study of shift work and risk of coronary heart disease in women. Circulation 92:3178–3182
Boggild H, Suadicani P, Hein HO, Gyntelberg F (1999) Shift work, social class, and ischaemic heart disease in middle aged and elderly men; a 22 year follow up in the Copenhagen Male Study. Occup Environ Med 56:640–645
Akerstedt T, Fredlund P, Gillberg M, Jansson B (2002) A prospective study of fatal occupational accidents - relationship to sleeping difficulties and occupational factors. J Sleep Res 11:69–71
Virtanen SV, Notkola V (2002) Socioeconomic inequalities in cardiovascular mortality and the role of work: a register study of Finnish men. Int J Epidemiol 31:614–621
Fujino Y, Iso H, Tamakoshi A, Inaba Y, Koizumi A, Kubo T, Yoshimura T (2006) A prospective cohort study of shift work and risk of ischemic heart disease in Japanese male workers. Am J Epidemiol 164:128–135
Hublin C, Partinen M, Koskenvuo K, Silventoinen K, Koskenvuo M, Kaprio J (2010) Shift-work and cardiovascular disease: a population-based 22-year follow-up study. Eur J Epidemiol 25:315–323
Natti J, Anttila T, Oinas T, Mustosmaki A (2012) Night work and mortality: prospective study among Finnish employees over the time span 1984 to 2008. Chronobiol Int 29:601–609
Lin Y, Ueda J, Yagyu K, Kurosawa M, Tamakoshi A, Kikuchi S (2013) A prospective cohort study of shift work and the risk of death from pancreatic cancer in Japanese men. Cancer Causes Control 24:1357–1361
Carter BD, Diver WR, Hildebrand JS, Patel AV, Gapstur SM (2014) Circadian disruption and fatal ovarian cancer. Am J Prev Med 46:S34–S41
Gapstur SM, Diver WR, Stevens VL, Carter BD, Teras LR, Jacobs EJ (2014) Work schedule, sleep duration, insomnia, and risk of fatal prostate cancer. Am J Prev Med 46:S26-33
Gu F, Zhang H, Hyland PL, Berndt S, Gapstur SM, Wheeler W, Ellipse Consortium T, Amos CI, Bezieau S, Bickeböller H et al (2017) Inherited variation in circadian rhythm genes and risks of prostate cancer and three other cancer sites in combined cancer consortia. Int J Cancer 141:1794–1802
Yu F, Zhang T, Zhou C, Xu H, Guo L, Chen M, Wu B (2019) The circadian clock gene bmal1 controls intestinal exporter MRP2 and drug disposition. Theranostics 9:2754–2767
Zou Y, Lin X, Bu J, Lin Z, Chen Y, Qiu Y, Mo H, Tang Y, Fang W, Wu Z (2020) Timeless-stimulated miR-5188-FOXO1/β-catenin-c-jun feedback loop promotes stemness via ubiquitination of β-catenin in breast cancer. Mol Ther 28:313–327
Manodpitipong A, Saetung S, Nimitphong H, Siwasaranond N, Wongphan T, Sornsiriwong C, Luckanajantachote P, Mangjit P, Keesukphan P, Crowley SJ et al (2017) Night-shift work is associated with poorer glycaemic control in patients with type 2 diabetes. J Sleep Res 26:764–772
Proietti S, Cucina A, Reiter RJ, Bizzarri M (2013) Molecular mechanisms of melatonin’s inhibitory actions on breast cancers. Cell Mol Life Sci 70:2139–2157
Kubatka P, Zubor P, Busselberg D, Kwon TK, Adamek M, Petrovic D, Opatrilova R, Gazdikova K, Caprnda M, Rodrigo L et al (2018) Melatonin and breast cancer: evidences from preclinical and human studies. Crit Rev Oncol Hematol 122:133–143
Borniger JC, Walker Ii WH, Surbhi EKM, Zhang N, Zalenski AA, Muscarella SL, Fitzgerald JA, Smith AN, Braam CJ et al (2018) A role for hypocretin/orexin in metabolic and sleep abnormalities in a mouse model of non-metastatic breast cancer. Cell Metab 28:118-129.e115
Chen L, Zheng J, Zhang Y, Yang L, Wang J, Ni J, Cui D, Yu C, Cai Z (2011) Tumor-specific expression of microRNA-26a suppresses human hepatocellular carcinoma growth via cyclin-dependent and -independent pathways. Mol Ther 19:1521–1528
Ndoye A, Dolivet G, Høgset A, Leroux A, Fifre A, Erbacher P, Berg K, Behr JP, Guillemin F, Merlin JL (2006) Eradication of p53-mutated head and neck squamous cell carcinoma xenografts using nonviral p53 gene therapy and photochemical internalization. Mol Ther 13:1156–1162
Li H, Tu J, Zhao Z, Chen L, Qu Y, Li H, Yao H, Wang X, Lee DF, Shen J et al (2020) Molecular signatures of BRCAness analysis identifies PARP inhibitor Niraparib as a novel targeted therapeutic strategy for soft tissue Sarcomas. Theranostics 10:9477–9494
Ramraj SK, Elayapillai SP, Pelikan RC, Zhao YD, Isingizwe ZR, Kennedy AL, Lightfoot SA, Benbrook DM (2020) Novel ovarian cancer maintenance therapy targeted at mortalin and mutant p53. Int J Cancer 147:1086–1097
Funding
No funding was received for this research.
Author information
Authors and Affiliations
Contributions
Informed consent each of the authors has contributed to read and approved this manuscript
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Research involving human participants and/or animals
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Wei, F., Chen, W. & Lin, X. Night-shift work, breast cancer incidence, and all-cause mortality: an updated meta-analysis of prospective cohort studies. Sleep Breath 26, 1509–1526 (2022). https://doi.org/10.1007/s11325-021-02523-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-021-02523-9