Abstract
Purpose
Obstructive sleep apnea (OSA) during the rapid eye movement (REM) stage of the sleep cycle is associated with intense hypoxemia and cardiovascular instability. We characterized OSA during REM sleep in patients after percutaneous coronary intervention.
Methods
In this multicenter study, 204 patients who had undergone percutaneous coronary intervention in the prior 6 to 36 months were recruited for in-laboratory polysomnography. The primary measure was respiratory events during REM sleep. The patients were divided into 2 groups: (1) OSA during REM sleep (≥ 15 events/h) and (2) absence of OSA during REM sleep (< 15 events/h).
Results
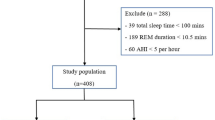
Based on the overall apnea-hypopnea index ≥ 15, 148 patients (74.0%) had OSA. After excluding patients with failed polysomnography or REM sleep < 30 min, 163 patients formed the cohort for this analysis. OSA during REM sleep was diagnosed in 132 patients (81%). Compared with the patients without OSA during REM sleep, those with OSA during REM sleep had a higher body mass index (p = 0.003) and systolic blood pressure (p = 0.041), and a higher prevalence of diabetes mellitus (p = 0.029). Logistic regression analysis, including age, sex, diabetes mellitus, indication for percutaneous coronary intervention, and indication for multi-vessel percutaneous coronary intervention, showed that diabetes mellitus was the only independent predictor of OSA during REM sleep (odds ratio 2.83; 95% CI, 1.17 to 6.83; p = 0.021).
Conclusion
In patients treated with percutaneous coronary intervention, there was a high prevalence of OSA during REM sleep. Diabetes mellitus was an independent predictor of OSA during REM sleep.

Similar content being viewed by others
References
Javaheri S, Barbe F, Campos-Rodriguez F, Dempsey JA, Khayat R et al (2017) Sleep apnea: types, mechanisms, and clinical cardiovascular consequences. J Am Coll Cardiol 69:841–848
Drager LF, McEvoy RD, Barbe F, Lorenzi-Filho G, Redline S, INCOSACT Initiative (International Collaboration of Sleep Apnea Cardiovascular Trialists) (2017) Sleep apnea and cardiovascular disease: lessons from recent trials and need for team science. Circulation. 136:1840–1850
Loo G, Tan AY, Koo CY, Tai BC, Richards M et al (2014) Prognostic implication of obstructive sleep apnea diagnosed by post-discharge sleep study in patients presenting with acute coronary syndrome. Sleep Med 15:631–636
Tan A, Hau W, Ho HH, Ghaem Maralani H, Loo G, Khoo SM, Tai BC, Richards AM, Ong P, Lee CH (2014) Obstructive sleep apnea and coronary plaque characteristics. Chest. 145:322–330
Lee CH, Sethi R, Li R, Ho HH, Hein T et al (2016) Obstructive sleep apnea and cardiovascular events after percutaneous coronary intervention. Circulation 133:2008–2017
Marin JM, Carrizo SJ, Vicente E, Agusti AG (2005) Long-term cardiovascular outcomes in men with obstructive sleep apnoea-hypopnoea with or without treatment with continuous positive airway pressure: an observational study. Lancet. 365:1046–1053
Campos-Rodriguez F, Martinez-Garcia MA, Reyes-Nuñez N, Caballero-Martinez I, Catalan-Serra P, Almeida-Gonzalez CV (2014) Role of sleep apnea and continuous positive airway pressure therapy in the incidence of stroke or coronary heart disease in women. Am J Respir Crit Care Med 189:1544–1550
McEvoy RD, Antic NA, Heeley E, Luo Y, Ou Q et al (2016) CPAP for prevention of cardiovascular events in obstructive sleep apnea. N Engl J Med 375:919–931
Peker Y, Glantz H, Eulenburg C, Wegscheider K, Herlitz J, Thunström E (2016) Effect of positive airway pressure on cardiovascular outcomes in coronary artery disease patients with nonsleepy obstructive sleep apnea. The RICCADSA randomized controlled trial. Am J Respir Crit Care Med 194:613–620
Yu J, Zhou Z, McEvoy RD, Anderson CS, Rodgers A, Perkovic V, Neal B (2017) Association of positive airway pressure with cardiovascular events and death in adults with sleep apnea: a systematic review and meta-analysis. JAMA. 318:156–166
Koo CY, Chua AP, Kristanto W, Koh EH, Tan ES et al (2019) Screening and treatment of obstructive sleep apnea in acute coronary syndrome. A randomized clinical trial. Int J Cardiol. https://doi.org/10.1016/j.ijcard.2019.07.003
Mokhlesi B, Ayas NT (2016) Cardiovascular events in obstructive sleep apnea – can CPAP therapy SAVE lives? N Engl J Med 375:994–996
Roder F, Wellmann B, Bitter T, Fox H, Türoff A et al (2020) Sleep duration and architecture during ASV for central sleep apnoea in systolic heart failure. Respir Physiol Neurobiol 271:103286
Alzoubaidi M, Mokhlesi B (2016) Obstructive sleep apnea during rapid eye movement sleep: clinical relevance and therapeutic implications. Curr Opin Pulm Med 22:545–554
Mokhlesi B, Finn LA, Hagen EW, Young T, Hla KM et al (2014) Obstructive sleep apnea during REM sleep and hypertension. Results of the Wisconsin Sleep Cohort. Am J Respir Crit Care Med 190:1158–1167
Appleton SL, Vakulin A, Martin SA, Lang CJ, Wittert GA et al (2016) Hypertension is associated with undiagnosed OSA during rapid eye movement sleep. Chest. 150:495–505
Ljunggren M, Lindberg E, Franklin KA, Öhagen P, Larsson M et al (2018) Obstructive sleep apnea during rapid eye movement sleep is associated with early signs of atherosclerosis in women. Sleep. 41. https://doi.org/10.1093/sleep/zsy099
Acosta-Castro P, Hirotsu C, Marti-Soler H, Marques-Vidal P, Tobback N, Andries D, Waeber G, Preisig M, Vollenweider P, Haba-Rubio J, Heinzer R (2018) REM-associated sleep apnoea: prevalence and clinical significance in the HypnoLaus cohort. Eur Respir J 52
Mokhlesi B, Hagen EW, Finn LA, Hla KM, Carter JR et al (2015) Obstructive sleep apnoea during REM sleep and incident non-dipping of nocturnal blood pressure: a longitudinal analysis of the Wisconsin Sleep Cohort. Thorax. 70:1062–1069
Aurora RN, Crainiceanu C, Gottlieb DJ, Kim JS, Punjabi NM (2018) Obstructive sleep apnea during REM sleep and cardiovascular disease. Am J Respir Crit Care Med 197:653–660
Tan LL, Ting J, Balakrishnan I, Seneviratna A, Gong L et al (2018) Sleep apnea evolution and left ventricular recovery after percutaneous coronary intervention for myocardial infarction. J Clin Sleep Med 14:1773–1781
Lemos PA, Cummins P, Lee CH, Degertekin M, Gardin M et al (2003) High-risk coronary intervention supported by percutaneous left ventricular assistance. Am J Cardiol 91:479–488
Fihn SD, Gardin JM, Abrams J, Berra K, Blankenship JC et al (2012) American College of Cardiology Foundation/American Heart Association Task Force. 2012 ACCF/AHA/ACP/AATS/PCNA/SCAI/STS guideline for the diagnosis and management of patients with stable ischemic heart disease: a report of the American College of Cardiology Foundation/American Heart Association task force on practice guidelines, and the American College of Physicians, American Association for Thoracic Surgery, Preventive Cardiovascular Nurses Association, Society for Cardiovascular Angiography and Interventions, and Society of Thoracic Surgeons. Circulation 126:e354–e471
Netzer NC, Stoohs RA, Netzer CM, Clark K, Strohl KP (1999) Using the Berlin questionnaire to identify patients at risk for the sleep apnea syndrome. Ann Intern Med 131:485–491
Johns MW (1991) A new method for measuring daytime sleepiness: the Epworth Sleepiness Scale. Sleep. 14:540–545
Berry RB, Budhiraja R, Gottlieb DJ, Gozal D, Iber C, Kapur VK, Marcus CL, Mehra R, Parthasarathy S, Quan SF, Redline S, Strohl KP, Davidson Ward SL, Tangredi MM, American Academy of Sleep Medicine (2012) American Academy of Sleep Medicine. Rules for scoring respiratory events in sleep: update of the 2007 AASM manual for the scoring of sleep and associated events. Deliberations of the Sleep Apnea Definitions Task Force of the American Academy of Sleep Medicine. J Clin Sleep Med 8:597–619
Sharma S, Fox H, Aguilar F, Mukhtar U, Willes L et al (2019) Auto positive airway pressure therapy reduces pulmonary pressures in adults admitted for acute heart failure with pulmonary hypertension and obstructive sleep apnea. The ASAP-HF pilot trial. Sleep 42
Spiesshoefer J, Aries J, Giannoni A, Emdin M, Fox H, Boentert M et al (2019) APAP therapy does not improve impaired sleep quality and sympatho-vagal balance: a randomized trial in patients with obstructive sleep apnea and systolic heart failure. Sleep Breath. https://doi.org/10.1007/s11325-019-01868-6
Sterz U, Buchner S, Hetzenecker A, Satzl A, Debl K et al (2018) Resolution of ST deviation after myocardial infarction in patients with and without sleep-disordered breathing. Somnologie (Berl) 22:130
Oldenburg O, Fox H, Wellmann B, Thiem U, Horstkotte D, Bitter T (2017) Automatic positive airway pressure for treatment of obstructive sleep apnea in heart failure. Somnologie 21:273–280
Azarbarzin A, Sands SA, Stone KL, Taranto-Montemurro L, Messineo L, Terrill PI, Ancoli-Israel S, Ensrud K, Purcell S, White DP, Redline S, Wellman A (2019) The hypoxic burden of sleep apnoea predicts cardiovascular disease-related mortality: the Osteoporotic Fractures in Men Study and the Sleep Heart Health Study. Eur Heart J 40:1149–1157
Oldenburg O, Wellmann B, Buchholz A, Bitter T, Fox H, Thiem U, Horstkotte D, Wegscheider K (2016) Nocturnal hypoxaemia is associated with increased mortality in stable heart failure patients. Eur Heart J 37:1695–1703
Fox H, Purucker HC, Holzhacker I, Tebtmann U, Bitter T et al (2016) Prevalence of sleep-disordered breathing and patient characteristics in a coronary artery disease cohort undergoing cardiovascular rehabilitation. J Cardiopulm Rehabil Prev 36:421–429
Reuter H, Herkenrath S, Treml M, Halbach M, Steven D (2018) Sleep-disordered breathing in patients with cardiovascular diseases cannot be detected by ESS, STOP-BANG, and Berlin questionnaires. Clin Res Cardiol 107:1071–1078
Acknowledgments
The authors are grateful to Easmed Pte Ltd. for their support in polysomnography.
Funding
This study was supported by a Collaborative Centre Grant and a Clinician Scientist Award from the National Medical Research Council of Singapore (award number: NMRC/CG/C006/2017 NMRC/CSA–INV/002/2015).
Author information
Authors and Affiliations
Contributions
ATA: study design, analysis, and interpretation of data; drafting and revising manuscript; and final approval. WK, MJT, CYK, CWC, and PK: concept, design, analysis, and interpretation of data; revising manuscript; and final approval. SPC: statistical analysis and interpretation of data; revising manuscript; and final approval. PQX, GR, ATT, and FB: analysis and interpretation of data; drafting and revising manuscript; and final approval. APC and CHL: concept, design, analysis, and interpretation of data; drafting and revising manuscript; and final approval.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 19 kb)
Rights and permissions
About this article
Cite this article
Aung, AT., Kristanto, W., Tan, M.JI. et al. Obstructive sleep apnea during rapid eye movement sleep in patients after percutaneous coronary intervention: a multicenter study. Sleep Breath 25, 125–133 (2021). https://doi.org/10.1007/s11325-020-02057-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-020-02057-6