Abstract
Purpose
The purpose of this study is to investigate the association between obstructive sleep apnea (OSA) with middle ear acoustic transference and cochlear function.
Methods
Male individuals with and without mild, moderate, and severe OSA according to standard criteria of full polysomnography and no co-morbidities were studied. Subjects with BMI ≥40 kg/m2, present or past treatment for OSA, with heart failure, diabetes, hypertension, dyslipidemia, stroke, use of chronic medications, and previous history of risk for hearing loss were excluded. All subjects were submitted to full polysomnography, evaluation of wideband acoustic immittance by energy of absorbance (EA), and distortion product otoacoustic emissions (DPOAE).
Results
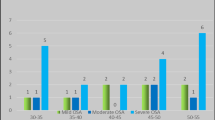
We studied 38 subjects (age 35.8 ± 7.2 years, BMI 28.8 ± 3.8 kg/m2) divided into no OSA (n = 10, age 33.6 ± 6.4 years, BMI 26.9 ± 4.1 kg/m2), mild (n = 11, age 32.8 ± 2.9 years, BMI 28.5 ± 3.5 kg/m2), moderate (n = 8, age 34.1 ± 6.8 years, BMI 29.6 ± 3.3 kg/m2), and severe OSA (n = 9, age 41.2 ± 9.2 years, BMI 30.5 ± 3.8 kg/m2). EA was similar between groups. In contrast, patients with severe OSA presented significantly lower DPOAE amplitudes when compared to the control, mild, and moderate OSA groups (p ≤ 0.03, for all comparisons).
Conclusions
Acoustic transference function of middle ear is similar in adults with and without OSA. Severe OSA is independently associated with cochlear function impairment in patients with no significant co-morbidities.




Similar content being viewed by others
References
Dempsey JA, Veasey SC, Morgan BJ, O'Donnell CP (2010) Pathophysiology of sleep apnea (vol 90, pg 47, 2010). Physiol Rev 90(2):797–798. doi:10.1152/physrev.z9j-2526-corr.2010
Peppard PE, Young T, Barnet JH, Palta M, Hagen EW, Hla KM (2013) Increased prevalence of sleep-disordered breathing in adults. Am J Epidemiol 177(9):1006–1014. doi:10.1093/aje/kws342
Makibara RR, Fukunaga JY, Gil D (2010) Eustachian tube function in adults with intact tympanic membrane. Brazilian journal of otorhinolaryngology 76(3):340–346
Sade J, Ar A (1997) Middle ear and auditory tube: middle ear clearance, gas exchange, and pressure regulation. Otolaryngol Head Neck Surg 116(4):499–524
Sivri B, Sezen OS, Akbulut S, Coskuner T (2013) The effect of continuous positive airway pressure on middle ear pressure. Laryngoscope 123(5):1300–1304. doi:10.1002/lary.23896
Thom JJ, Carlson ML, Driscoll CLW, St Louis EK, Ramar K, Olson EJ, Neff BA (2015) Middle ear pressure during sleep and the effects of continuous positive airway pressure. Am J Otolaryng 36(2):173–177. doi:10.1016/j.amjoto.2014.10.024
Shamsuzzaman AS, Gersh BJ, Somers VK (2003) Obstructive sleep apnea: implications for cardiac and vascular disease. JAMA 290(14):1906–1914. doi:10.1001/jama.290.14.1906
Mazurek B, Haupt H, Georgiewa P, Klapp BF, Reisshauer A (2006) A model of peripherally developing hearing loss and tinnitus based on the role of hypoxia and ischemia. Med Hypotheses 67(4):892–899. doi:10.1016/j.mehy.2006.03.040
Drager LF, Bortolotto LA, Lorenzi MC, Figueiredo AC, Krieger EM, Lorenzi-Filho G (2005) Early signs of atherosclerosis in obstructive sleep apnea. Am J Respir Crit Care Med 172(5):613–618. doi:10.1164/rccm.200503-340OC
Berry RB, Budhiraja R, Gottlieb DJ, Gozal D, Iber C, Kapur VK, Marcus CL, Mehra R, Parthasarathy S, Quan SF, Redline S, Strohl KP, Davidson Ward SL, Tangredi MM (2012) Rules for scoring respiratory events in sleep: update of the 2007 AASM Manual for the Scoring of Sleep and Associated Events. Deliberations of the Sleep Apnea Definitions Task Force of the American Academy of Sleep Medicine. Journal of clinical sleep medicine : JCSM: official publication of the American Academy of Sleep Medicine 8(5):597–619. doi:10.5664/jcsm.2172
Matsumura E, Matas CG, Magliaro FC, Pedreno RM, Lorenzi-Filho G, Sanches SG, Carvallo RM (2016) Evaluation of peripheral auditory pathways and brainstem in obstructive sleep apnea. Brazilian journal of otorhinolaryngology. doi:10.1016/j.bjorl.2016.10.014
Shanks JE (1984) Tympanometry. Ear Hear 5(5):268–280
Liu YW, Sanford CA, Ellison JC, Fitzpatrick DF, Gorga MP, Keefe DH (2008) Wideband absorbance tympanometry using pressure sweeps: system development and results on adults with normal hearing. J Acoust Soc Am 124(6):3708–3719. doi:10.1121/1.3001712
Greenhouse SW, Geisser S (1959) On methods in the analysis of profile data. Psychometrika 24(2):95–112. doi:10.1007/bf02289823
Holm S (1979) A simple sequentially rejective multiple test procedure. Scand J Stat 6(2):65–70
Casale M, Vesperini E, Potena M, Pappacena M, Bressi F, Baptista PJ, Salvinelli F (2012) Is obstructive sleep apnea syndrome a risk factor for auditory pathway? Sleep & breathing = Schlaf & Atmung 16(2):413–417. doi:10.1007/s11325-011-0517-x
Sheu JJ, Wu CS, Lin HC (2012) Association between obstructive sleep apnea and sudden sensorineural hearing loss: a population-based case-control study. Arch Otolaryngol Head Neck Surg 138(1):55–59. doi:10.1001/archoto.2011.227
Ballacchino A, Salvago P, Cannizzaro E, Costanzo R, Di Marzo M, Ferrara S, La Mattina E, Messina G, Mucia M, Mule A, Plescia F, Sireci F, Rizzo S, Martines F (2015) Association between sleep-disordered breathing and hearing disorders. Clinical observation in Sicilian patients Acta Medica Mediterr 31(3):607–614
Deniz M, Ciftci Z, Ersozlu T, Gultekin E, Alp R (2016) The evaluation of auditory system in obstructive sleep apnea syndrome (OSAS) patients. Am J Otolaryngol 37(4):299–303. doi:10.1016/j.amjoto.2016.03.004
Martines F, Ballacchino A, Sireci F, Mucia M, La Mattina E, Rizzo S, Salvago P (2016) Audiologic profile of OSAS and simple snoring patients: the effect of chronic nocturnal intermittent hypoxia on auditory function. European archives of oto-rhino-laryngology : official journal of the European Federation of Oto-Rhino-Laryngological Societies (EUFOS): affiliated with the German Society for Oto-Rhino-Laryngology-Head and Neck Surgery 273(6):1419–1424. doi:10.1007/s00405-015-3714-6
Terzi S, Ozgur A, Erdivanli OC, Coskun ZO, Ogurlu M, Demirci M, Dursun E (2015) Diagnostic value of the wideband acoustic absorbance test in middle-ear effusion. J Laryngol Otol 129(11):1078–1084. doi:10.1017/s0022215115002339
Taiji H, Kanzaki J (2016) Detection of the presence of middle-ear effusion with wideband absorbance tympanometry. Nihon Jibiinkoka Gakkai kaiho 119(5):727–733
Ellison JC, Gorga M, Cohn E, Fitzpatrick D, Sanford CA, Keefe DH (2012) Wideband acoustic transfer functions predict middle-ear effusion. Laryngoscope 122(4):887–894. doi:10.1002/lary.23182
Nakajima HH, Rosowski JJ, Shahnaz N, Voss SE (2013) Assessment of ear disorders using power reflectance. Ear Hear 34(Suppl 1):48s–53s. doi:10.1097/AUD.0b013e31829c964d
Feeney MP, Grant IL, Marryott LP (2003) Wideband energy reflectance measurements in adults with middle-ear disorders. J Speech Lang Hear Res 46(4):901–911
Bernath I, McNamara P, Szternak N, Szakacs Z, Koves P, Terray-Horvath A, Vida Z (2009) Hyperviscosity as a possible cause of positive acoustic evoked potential findings in patients with sleep apnea: a dual electrophysiological and hemorheological study. Sleep Med 10(3):361–367. doi:10.1016/j.sleep.2008.03.012
Mazurek B, Winter E, Fuchs J, Haupt H, Gross J (2003) Susceptibility of the hair cells of the newborn rat cochlea to hypoxia and ischemia. Hear Res 182(1–2):2–8
Kim SH, Won YS, Kim MG, Baek YJ, Oh IH, Yeo SG (2016) Relationship between obesity and hearing loss. Acta Otolaryngol 136(10):1046–1050. doi:10.1080/00016489.2016.1179787
Nagaoka J, Anjos MF, Takata TT, Chaim RM, Barros F, Penido Nde O (2010) Idiopathic sudden sensorineural hearing loss: evolution in the presence of hypertension, diabetes mellitus and dyslipidemias. Brazilian journal of otorhinolaryngology 76(3):363–369
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Funding information
This study was supported by Fundação de Amparo à Pesquisa do Estado de São Paulo (FAPESP process number 2013/10281-7).
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Matsumura, E., Matas, C.G., Sanches, S.G.G. et al. Severe obstructive sleep apnea is associated with cochlear function impairment. Sleep Breath 22, 71–77 (2018). https://doi.org/10.1007/s11325-017-1530-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-017-1530-5