Abstract
Purpose
One of the key areas of delivery of the ‘Action Plan for Health Research 2019–2029’, for the Health Service Executive (HSE) in Ireland, is adding value and using data and knowledge, including health-related quality of life (HRQoL), for improved health care, service delivery and better population health and wellbeing. The development of governance, management and support framework and mechanisms will provide a structure for ensuring research is relevant to the organisation’s service plan, well designed, has a clear plan for dissemination and translation of knowledge, and minimises research waste. Developing a process for the translation, dissemination and impact of research is part of the approach to improving translation of research into practice and aligning it with knowledge gaps. A project was undertaken to develop a clear, unified, universally applicable approach for the translation, dissemination, and impact of research undertaken by HSE staff and commissioned, sponsored, or hosted by the organisation. This included the development of guidance, training, and information for researchers.
Methods
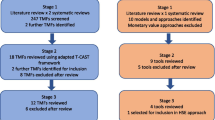
Through an iterative process, an interdisciplinary working group of experts in knowledge translation (KT), implementation science, quality improvement and research management, identified KT frameworks and tools to form a KT, dissemination, and impact process for the HSE. This involved a literature review, screening of 247 KT theories, models, and frameworks (TMFs), review of 18 TMFs selected as usable and applicable to the HSE, selection of 11 for further review, and final review of 6 TMFs in a consensus workshop. An anonymous online survey of HSE researchers, consisting of a mixture of multiple choice and free text questions, was undertaken to inform the development of the guidance and training.
Results
A pilot of the KT process and guidance, involving HSE researchers testing its use at various stages of their research, demonstrated the need to guide researchers through planning, stakeholder engagement, and disseminating research knowledge, and provide information that could easily be understood by novice as well as more experienced researchers. A survey of all active researchers across the organisation identified their support and knowledge requirements and led to the development of accompanying guidance to support researchers in the use of the process. Researchers of all levels reported that they struggled to engage with stakeholders, including evidence users and policy makers, to optimise the impact of their research. They wanted tools that would support better engagement and maximise the value of KT. As a result of the project a range of information, guidance, and training resources have been developed.
Conclusion
KT is a complex area and researchers need support to ensure they maximise the value of their research. The KT process outlined enables the distilling of a clear message, provides a process to engage with stakeholders, create a plan to incorporate local and political context, and can show a means to evaluate how much the findings are applied in practice. This is a beneficial application of KT in the field of patient reported outcomes. In implementing this work, we have reinforced the message that stakeholder engagement is crucial from the start of the research study and increases engagement in, and ownership of, the research knowledge.



Similar content being viewed by others
Data availability
Data is available from the authors.
References
Terres, A. (2019a). Health Service Executive Action Plan for Health Research 2019–2029. Health Service Executive. Retrieved December 21, 2021, from https://hseresearch.ie/publications/
Damschroder, L. J., Aron, D. C., Keith, R. E., Kirsh, S. R., Alexander, J. A., & Lowery, J. C. (2009). Fostering implementation of health services research findings into practice: A consolidated framework for advancing implementation science. Implementation Science, 4, 15.
Prihodova, L., Guerin, S., Tunney, C., & Kernohan, W. G. (2019). Key components of knowledge transfer and exchange in health services research: Findings from a systematic scoping review. Journal of Advanced Nursing, 75(2), 313–326. https://doi.org/10.1111/jan.13836(Epub2018Oct7)
Ellen, M. E., Lavis, J. N., Horowitz, E., et al. (2018). How is the use of research evidence in health policy perceived? A comparison between the reporting of researchers and policy-makers. Health Research Policy System, 16, 64. https://doi.org/10.1186/s12961-018-0345-6
Chalmers, I., & Glasziou, P. (2016) Is 85% of health research really ‘wasted’. The BMJ, BMJ Blogs. https://www.bmj.com/content/369/bmj.m1847
Moher, D., Glasziou, P., Chalmers, I., Nasser, M., Bossuyt, P. M., Korevaar, A., Graham, I. D., Ravaud, P., & Boutron, I. (2016). Increasing value and reducing waste in biomedical research: Who’s listening? Lancet, 387(10027), 1573–1586.
Al-Shahi Salman, R., Beller, E., Kagan, J., Hemminki, E., Phillips, R. S., Savulescu, J., Macleod, M., Wisely, J., & Chalmers, I. (2014). Increasing value and reducing waste in biomedical research regulation and management. Lancet, 383(9912), 176–185. https://doi.org/10.1016/S0140-6736(13)62297-7 Epub 2014 Jan 8.
Royal College of Physicians. (2020). Research for all? An analysis of clinical participation in research. Royal College of Physicians.
Brownson, R. C., Kreuter, M. W., Arrington, B. A., & True, W. R. (2006). Translating scientific discoveries into public health action: How can schools of public health move us forward? Public Health Reports, 121(1), 97–103. https://doi.org/10.1177/003335490612100118
Minogue, V., Cooke, M., Donskoy, A. L., Vicary, P., & Wells, B. (2018). Patient and public involvement in reducing health and care waste. Research Involvement and Engagement, 2018(4), 5.
Minogue, V., & Wells, B. (2019, August 9). Patients and the public are essential to reducing research waste. BMJ Opinion. https://blogs.bmj.com/bmj/2019/08/09/virginia-minogue-and-bill-wells-patients-and-the-public-are-essential-to-reducing-research-waste/
Brundage, M., Bass, B., Jolie, R., & Foley, K. (2011). A knowledge translation challenge: Clinical use of quality of life data from cancer clinical trials. Quality of Life Research: An International Journal of Quality of Life Aspects of Treatment, Care and Rehabilitation, 20(7), 979–985. https://doi.org/10.1007/s11136-011-9848-0
Minogue, V., & Wells, B. (2018). Adding value, reducing research waste, the role of the NHS Research and Development Management Community. International Journal of Health Governance, 23(2), 160–177.
Health Service Executive. (2021, September). HSE National Framework for the Governance, Management and Support of Health Research. Health Service Executive. Retrieved December 21, 2021, from https://hseresearch.ie/publications/
Terres, A., O’Hara, M. C., Fleming, P., Cole, N., O’Hanlon, D., & Manning, P. (2019b). Research Activity in the HSE and its funded organisations: A report of staff engaged in research, research studies undertaken, publication output and research networks. Health Service Executive. Retrieved December 21, 2021, from https://hseresearch.ie/publications/
Strifler, L., Cardoso, R., McGowan, J., Cogo, E., Nincic, V., Khan, P., Scott, A., Ghassemi, M., MacDonald, H., Lai, Y., Treister, V., Tricco, A., & Straus, S. (2018). Scoping review identifies significant number of knowledge translation theories, models, and frameworks with limited use. Journal of Clinical Epidemiology, 100(2018), 92–102.
Payne, C., Brown, M. J., Guerin, S., & Kernohan, W. G. (2019). EMTReK: An evidence-based model for the transfer and exchange of research knowledge—Five case studies in palliative care. SAGE Open Nursing. https://doi.org/10.1177/2377960819861854
Birken, S. A., Rohweder, C. L., Powell, B. J., Shea, C. M., Scott, J., Leeman, J., Grewe, M. E., Kirk, M. A., Damschroder, L., Aldridge, W. A., Haines, E. R., Straus, S., & Presseau, J. (2018). T-CaST: An implementation theory comparison and selection tool. Implementation Science, 2018(13), 143.
Department of Health. (2018). NCEC Implementation Guide and Toolkit. Department of Health. Retrieved December 21, 2021, from https://health.gov.ie/national-patient-safety-office/ncec/
Health Service Executive Research and Development. (2021). Knowledge Translation, Dissemination, and Impact; A Practical Guide for Researchers. Guide No 2: Planning your knowledge Translation activity (version 5). Research and Development. Health Service Executive. https://hseresearch.ie/wp-content/uploads/2021/09/Guide-no-2-Planning-your-knowledge-translation-activity.pdf
Esmail, R., Hanson, H. M., Holroyd-Leduc, J., Brown, S., Strifler, L., Straus, S. E., Niven, D. J., & Clement, F. M. (2020). A scoping review of full-spectrum knowledge translation theories, models, and frameworks. Implementation Science, 15, 11. https://doi.org/10.1186/s13012-020-0964-5
Shelton, R. C., Rhoades-Cooper, B., & Wiltsey-Stirman, S. (2018). The sustainability of evidence-based interventions and practices in public health and health care. Annual Review of Public Health, 9, 55–76.
Barwick, M. (2008). Knowledge Translation Planning Template. The Hospital for Sick Children. Retrieved December 21, 2021, from https://www.sickkids.ca/en/learning/continuing-professional-development/knowledge-translation-training/knowledge-translation-planning-template-form/
Abad-Corpa, E., Cabrero-Garcia, J., Delgado-Hito, P., Carrillo-Alcaraz, A., Meseguer-Liza, C., & Martinez-Corbalan, J. T. (2012). Effectiveness of participatory-action-research to put in practice evidence at a nursing Onco-haematology Unit. Revista latino-americana de enfermagem, 2012(20), 59–67.
Abed, J., Reilley, B., Butler, M. O., Kean, T., Wong, F., & Hohman, K. (2000). Comprehensive Cancer Control Initiative of the Centers for Disease Control and Prevention: An example of participatory innovation diffusion. Journal of Public Health Management and Practice, 2000(6), 79–92.
Moullin, J. C., Dickson, K. S., Stadnick, N. A., Rakin, B., & Aarons, G. A. (2019). Systematic Review of the Exploration, Preparation, Implementation, Sustainment (EPIS) Framework. Implementation Science, 2019(14), 1.
Titler, M. G., Kleiber, C., Steelman, V. J., Rakel, B. A., Budreau, G., Everett, L. Q., & Goode, C. J. (2001). The Iowa Model of evidence-based practice to promote quality care. Critical Care Nursing Clinicians of North America, 13, 497–509.
Graham, I., Logan, J., Harrison, M., Straus, S., Tetroe, J., Caswell, W., & Robinson, N. (2006). Lost in knowledge translation: Time for a map? Journal of Continuing Education in the Health Professions, 2006(26), 13–24.
Schroy, P. C., III., Emmons, K., Peters, E., Glick, J. T., Robinson, P. A., Lydotes, M. A., Mylvanaman, S., Evans, S., Chaisson, C., Pignone, M., Prout, M., Davidson, P., & Heeren, T. C. (2011). The impact of a novel computer-based decision aid on shared decision making for colorectal cancer screening: A randomized trial. Medical Decision Making, 31(1), 93–107. https://doi.org/10.1177/0272989X10369007 Epub 2010 May 18.
Agurto, I., Sandoval, J., De La Rosa, M., & Guardado, M. E. (2006). Improving cervical cancer prevention in a developing country. International Journal for Quality in Health Care: Journal of the International Society for Quality in Health Care/ISQua, 18, 81–86.
Porter, C. M. (2015). Revisiting Precede–Proceed: A leading model for ecological and ethical health promotion. Health Education Journal, 75(6), 753–764. https://doi.org/10.1177/0017896915619645
Harvey, G., & Kitson, A. (2016). PARIHS revisited: From heuristic to integrated framework for the successful implementation of knowledge into practice. Implementation Science, 11, 33.
Feldstein, A. C., & Glasgow, R. E. (2008). A Practical, Robust Implementation and Sustainability Model (PRISM) for Integrating Research Findings into Practice. The Joint Commission Journal on Quality and Patient Safety, 34(4), 228–243.
Glasgow, R. E., Vogt, T. M., & Boles, S. M. (1999). Evaluating the public health impact of health promotion interventions: The RE-AIM Framework. American Journal of Public Health, 89(9), 1322.
Burnette, J. L., O’Boyle, E. H., VanEpps, E. M., Pollock, J. M., & Finkel, E. J. (2013). Mind-sets matter: A meta-analytic review of implicit theories and self-regulation. Psychological Bulletin, 139(3), 655–701.
Bandura, A. (2001). Social cognitive theory: An agentic perspective. Annual Review of Psychology., 52, 1–26. https://doi.org/10.1146/annurev.psych.52.1.1
Berkowitz, J. M., Huhman, M., Heitzler, C. D., Potter, L. D., Nolin, M. J., & Banspach, S. W. (2008). Overview of formative, process, and outcome evaluation methods used in the VERB™ Campaign. American Journal of Preventive Medicine, 34, 222–229.
Adams, M. A., Norman, G. J., Hovell, M. F., Sallis, J. F., & Patrick, K. (2009). Reconceptualizing decisional balance in an adolescent sun protection intervention: Mediating effects and theoretical interpretations. Health Psychology: Official Journal of the Division of Health Psychology, American Psychological Association, 2009(28), 217–225.
Van Calster, B., Wynants, L., Riley, R. D., Van Smeden, M., & Collins, G. S. (2021). Methodology over metrics: Current scientific standards are a disservice to patients and society. Journal of Clinical Epidemiology, 138(2021), 219–226. https://doi.org/10.1016/j.jclinepi.2021.05.018
Weldring, T., & Smith, S. M. (2013). Patient-Reported Outcomes (PROs) and Patient-Reported Outcome Measures (PROMs). Health Service Insights, 6, 61–68. https://doi.org/10.4137/HSI.S11093 Published 2013 Aug 4.
Acknowledgements
The authors are grateful to all members of the Knowledge Translation, Dissemination and Impact Project Working Group and implementation group who are responsible for the delivery and oversight of the project. They would also like to acknowledge the input of the Patient and Public Involvement Knowledge Translation Sub-group.
Funding
No external funding was sought for this project.
Author information
Authors and Affiliations
Contributions
VM, MM, AT contributed to the development of the research study and design. VM and MM drafted the manuscript, and all authors critically reviewed each version of the manuscript and read and approved the final version. VM and MM are the HSE leads for the knowledge translation, dissemination and impact project which is part of the HSE Action Plan for Health Research. AT is the lead for the implementation of the plan and oversees the work of the KT workstream.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest or competing interests.
Consent for publication
Not applicable.
Ethical approval
Not applicable.
Informed consent
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Minogue, V., Morrissey, M. & Terres, A. Supporting researchers in knowledge translation and dissemination of their research to increase usability and impact. Qual Life Res 31, 2959–2968 (2022). https://doi.org/10.1007/s11136-022-03122-1
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-022-03122-1