Abstract
Purpose
There is a high incidence of abnormal sphenoid sinus changes in patients with pituitary apoplexy (PA). Their pathophysiology is currently unexplored and may reflect an inflammatory or infective process. In this preliminary study, we characterised the microbiota of sphenoid sinus mucosa in patients with PA and compared findings to a control group of surgically treated non-functioning pituitary adenomas (NFPAs).
Methods
In this prospective observational study of patients undergoing trans-sphenoidal surgery for PA or NFPA, sphenoid sinus mucosal specimens were microbiologically profiled through PCR-cloning of the 16S rRNA gene.
Results
Ten patients (five with PA and five with NFPAs) with a mean age of 51 years (range 23–71) were included. Differences in the sphenoid sinus microbiota of the PA and NFPA groups were observed. Four PA patients harboured Enterobacteriaceae (Enterobacter spp., N = 3; Escherichia coli, N = 1). In contrast, patients with NFPAs had a sinus microbiota more representative of health, including Staphylococcus epidermidis (N = 2) or Corynebacterium spp. (N = 2).
Conclusions
PA may be associated with an abnormal sphenoid sinus microbiota that is similar to that seen in patients with sphenoid sinusitis.
Similar content being viewed by others
Introduction
Pituitary apoplexy (PA) is an acute clinical syndrome secondary to haemorrhage and/or infarction of a pituitary adenoma [1]. Patients classically present with a sudden onset of headache, nausea/vomiting, visual disturbance and/or altered conscious level [1]. PA is presumed to be a spontaneous vascular event and risk factors include anticoagulant therapy, major surgery, dopamine agonist therapy, pregnancy and radiation therapy [1].
We and others have observed a high incidence of abnormal sphenoid sinus changes in PA [2]. In a recent study we noted that sphenoid sinus mucosal thickening (SSMT) was present in 62% of PA patients compared to just 6% of a control group of non-functioning pituitary adenomas (NFPAs) [2]. The aetiology of SSMT in PA is unknown and possibilities include inflammation or infection.
In this preliminary study, we sought to characterise the sphenoid sinus mucosal microbiota in patients with PA and compare them to a control group comprising surgically treated NFPAs.
Methods
This was a prospective, single-center observational study. Ethical approval was obtained from the Local Research Ethics Committee for the collection of sinus biopsies between 2008 and 2009 (08/H1012/50). Patient data on clinical presentation, preoperative magnetic resonance imaging findings, tumour histology, treatment and follow-up were collected from a prospective electronic database.
Patient cohorts
Patient cohorts were determined according to the following criteria:
-
(i)
Classical PA: as defined by the Society of Endocrinology, refers to a clinical syndrome, characterised by a sudden onset of headache, vomiting, visual impairment and decreased consciousness caused by haemorrhage and/or infarction of the pituitary gland [1]. Haemorrhage and/or infarction were confirmed using at least one or more of the following: imaging (T1/2 weighted magnetic resonance imaging), histopathology or intra-operative findings (i.e. evidence of pre-existing haemorrhage within the pituitary adenoma).
-
(ii)
Subclinical PA: defined as radiological and histopathological evidence of infarction or haemorrhage, without accompanying symptomatology.
-
(iii)
NFPA: surgically treated control group, with no evidence of pituitary apoplexy clinically, radiologically or on histopathology.
Tissue collection
Sphenoid sinus mucosal samples were collected during the approach for endoscopic trans-sphenoidal surgery for the treatment of PA or NFPAs, as described previously [3]. On induction of general anesthesia all patients received a perioperative dose of antibiotics (1.5 g cefuroxime and 500 mg metronidazole; iv). Following surgery, tissue samples were archived at −80 °C for further microbiological analyses.
Microbiological profiling
Bacterial genomic DNA was extracted from tissue biopsy samples (<25 mg) using a Qiagen DNA Blood and Tissue Kit (Qiagen Ltd, UK), according to the manufacturing protocol. Polymerase chain reaction of extracted bacterial DNA was performed using the 806R/8FLP primer set [4] and amplified products purified using a Qiagen PCR purification kit (Qiagen Ltd, UK). Amplicons were ligated into a pDrive cloning vector (Qiagen Ltd, UK) and transformed into competent Escherichia coli as per the manufacturer’s protocol. Negative controls comprised PCR grade water alone in the absence of amplicon product. Transformants were plated onto Luria–Bertani media (supplemented 0.1 mg/ml ampicillin; 0.05 mM IPTG; 0.08 mg/ml X-gal) and successful transformants identified using blue/white screening. Plasmid DNA purification was performed using the QIAprep Miniprep kit (Qiagen Ltd, UK) and inserts screened by PCR using the vector specific primers M13 forward (5′ GTTTTCCCAGTCACGAC 3′) and M13 reverse (5′ AACAGCTATGACCATG 3′). Inserts were sequenced using M13-vector primers at the University of Manchester Sanger sequencing facility. Consensus sequences were identified following a BLAST search of the GenBank nucleotide database (http://blast.ncbi.nlm.nih.gov/Blast.cgi). Isolates exhibiting >98% homology to database sequences were delineated to the species level.
Results
Ten patients were included in this pilot study, five with PA (four classical and one subclinical) and five with NFPAs (Table 1). The mean age was 51 years (range 23–71). There were four males and six females. The typical MRI scan of a patient with PA (Case A1) and NFPA (Case N3) are shown in Fig. 1.
Sagittal T1 (a and c) and coronal T2-weighted (b and d) MRI from a patient presenting with PA (a and b) and NFPA (c and d). The patient with PA (a and b; Case A1, Table 1) was a 24 year old male, with no significant past medical history, who presented with acute confusion, headaches and hyponatraemia. MRI revealed a pituitary lesion with evidence of bleed and sphenoid sinus mucosal thickening (green arrows). The patient with NFPA (c and d; Case N3, Table 1) was a 54 year old female who presented with a homonymous hemianopia. MRI revealed a pituitary lesion abutting the optic chiasm and with no evidence of sphenoid sinus mucosal thickening and a relatively empty sinus (white arrows)
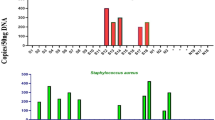
Two hundred and fifty bacterial clones were subjected to plasmid purification and PCR screening. Overall, differences were observed between the sphenoid sinus microbiota of the PA and NFPA groups (Table 1). Four of the five PA patients harboured atypical respiratory bacterial taxa, including Enterobacter sp. and Escherichia coli. In contrast, clonal libraries generated from 4 patients with NFPAs comprised predominantly of sequences representative of Corynebacterium spp., Staphylococcus spp. and Prevotella spp. One NFPA patient (Case N4) was found to harbour Streptococcus pneumoniae only and had evidence of asymptomatic sphenoid sinus disease preoperatively.
Discussion
Compositional differences in the sinus microbiota between patients with and without PA have not been reported previously. Our main finding is the presence of Enterobacter and Escherichia bacterial DNA, from the sphenoid sinuses of PA patients. Bacteria representative of these genera were not identified in non-apoplectic controls.
Investigations of the sinonasal tract have shown members of the corynebacteria, staphylococci and propionibacteria to be well represented in health [5,6,7]. In the present study, clonal libraries generated from the sinuses of NFPA patients were generally representative of such findings with either Staphylococcus epidermidis or Corynebacterium spp. predominating following sequencing. In contrast, atypical respiratory pathogens are rarely reported in the context of the heathy upper airways. For example, a recent survey of the nares (n = 1878) reported E. coli and Enterobacter aerogenes are carried by less than 6.1 and 2.6% of healthy adults, respectively [8]. With regards the sinuses, microbiota studies are generally more limited in terms of sample size, but typically report recovery of these bacterial taxa in less than 5% healthy individuals [7, 9]. Rather, these bacteria are typically associated with infradiaphragmatic sources and have been implicated as potential pathogens in rhinosinusitis following their isolation in symptomatic individuals [10,11,12]. The clinical significance of Leuconostoc carriage by PA patients is unclear and, to the authors knowledge, has not been described in the context of this body site. In the clinical setting, members of this genus are considered recalcitrant to standard microbiological identification, but have been described in the context of opportunistic infection in immunocompromised individuals [13,14,15].
PA is characterised by a sudden onset of headache and other neurological symptoms and in many patients this is the first sign of a pre-existing pituitary adenoma. Despite the significant patient morbidity associated with this syndrome, the pathophysiology of PA remains poorly understood with a significant proportion of patients presenting with no recognised risk factors [16]. The identification of known respiratory pathogens from the sinuses of PA patients could be indicative of an infective aetiology. In support of this is the observation of increased prevalence of sphenoid sinus mucosal thickening in patients presenting with PA, most notably within the first week of the onset of symptoms [2, 17, 18]. Infection is also a known risk factor for other cerebral vascular phenomena, such as cavernous sinus syndrome [19]. Given the proximity of the sphenoid sinus to the pituitary gland, it is tempting to speculate an infective aetiology for some patients with PA.
On the other hand, it must be noted that in this preliminary study, the patients undergoing pituitary surgery for PA did not exhibit preoperative evidence of sinusitis. Moreover we acknowledge that we did not attempt to culture the bacteria as from previous experience, this can be difficult, in part due to the administration of peri-operative broad-spectrum antibiotics during trans-sphenoidal surgery. Further work is warranted in a larger patient cohort, utilizing next generation sequencing platforms to achieve better microbiota profiling, together with histological analyses of explanted sphenoid sinus and pituitary tissue.
Conclusion
In this preliminary study, we characterised the sphenoid sinus mucosal microbiota in patients with PA and compared findings to a control group comprising of surgically treated NFPAs. PA patients harboured atypical sinus bacteria, including Enterobacteriaceae. In contrast, NFPA patients had a sinus microbiota more representative of health. The abnormal microbiota in PA patients was similar to reported cases of sphenoid sinusitis. Future prospective studies are warranted in order to explore this observation.
References
Rajasekaran S, Vanderpump M, Baldeweg S, Drake W, Reddy N, Lanyon M, Markey A., Plant G, Powell M, Sinha S, Wass J (2011) UK guidelines for the management of pituitary apoplexy. Clin Endocrinol 74(1):9–20. doi:10.1111/j.1365-2265.2010.03913.x
Waqar M, McCreary R, Kearney T, Karabatsou K, Gnanalingham KK (2017) Sphenoid sinus mucosal thickening in the acute phase of pituitary apoplexy. Pituitary. doi:10.1007/s11102-017-0804-z
Zador Z, Gnanalingham K (2013) Endoscopic transnasal approach to the pituitary–operative technique and nuances. Br J Neurosurg 27(6):718–726. doi:10.3109/02688697.2013.798862
Humphreys GJ, McBain AJ (2013) Continuous culture of sessile human oropharyngeal microbiotas. J Med Microbiol 62:906–916
Ramakrishnan VR, Feazel LM, Gitomer SA, Ir D, Robertson CE, Frank DN (2013) The microbiome of the middle meatus in healthy adults. PLoS ONE 8(12):e85507. doi:10.1371/journal.pone.0085507
Boase S, Foreman A, Cleland E, Tan L, Melton-Kreft R, Pant H, Hu FZ, Ehrlich GD, Wormald PJ (2013) The microbiome of chronic rhinosinusitis: culture, molecular diagnostics and biofilm detection. BMC Infect Dis 13:210
Shibao S, Toda M, Tomita T, Ogawa K, Yoshida K (2014) Analysis of the bacterial flora in the nasal cavity and the sphenoid sinus mucosa in patients operated on with an endoscopic endonasal transsphenoidal approach. Neurol Med Chir 54(Suppl 3):1009–1013
Kock R, Werner P, Friedrich AW, Fegeler C, Becker K, Prevalence of Multiresistant Microorganisms Study G, Prevalence of Multiresistant Microorganisms PMMSG (2016) Persistence of nasal colonization with human pathogenic bacteria and associated antimicrobial resistance in the German general population. New Microb New Infect 9:24–34. doi:10.1016/j.nmni.2015.11.004
Niederfuhr A, Kirsche H, Riechelmann H, Wellinghausen N (2009) The bacteriology of chronic rhinosinusitis with and without nasal polyps. Arch Otolaryngol Head Neck Surg 135(2):131–136
Bhattacharyya N, Kepnes LJ (1999) The microbiology of recurrent rhinosinusitis after endoscopic sinus surgery. Arch Otolaryngol Head Neck Surg 125(10):1117–1120
Brook I (2002) Bacteriology of acute and chronic sphenoid sinusitis. Ann Otol Rhinol Laryngol 111(11):1002–1004. doi:10.1177/000348940211101109
Massoubre J, Saroul N, Vokwely JE, Lietin B, Mom T, Gilain L (2016) Results of transnasal transostial sphenoidotomy in 79 cases of chronic sphenoid sinusitis. Eur Ann Otorhinolaryngol Head Neck Dis 133(4), 231–236. doi:10.1016/j.anorl.2016.02.002
Albanese A, Spanu T, Sali M, Novegno F, D’Inzeo T, Santangelo R, Mangiola A, Anile C, Fadda G (2006) Molecular identification of Leuconostoc mesenteroides as a cause of brain abscess in an immunocompromised patient. J Clin Microbiol 44(8):3044–3045. doi:10.1128/JCM.00448-06
Bou G, Luis Saleta J, Saez Nieto JA, Tomas M, Valdezate S, Sousa D, Lueiro F, Villanueva R, Jose Pereira M, Llinares P (2008) Nosocomial outbreaks caused by Leuconostoc mesenteroides subsp. mesenteroides. Emerg Infect Dis 14(6):968–971. doi:10.3201/eid1406.071095
Ferrer S, de Miguel G, Domingo P, Pericas R, Prats G (1995) Pulmonary infection due to Leuconostoc species in a patient with AIDS. Clin Infect Dis 21(1):225–226
Sibal L, Ball SG, Connolly V, James RA, Kane P, Kelly WF, Kendall-Taylor P, Mathias D, Perros P, Quinton R, Vaidya B (2004) Pituitary apoplexy: a review of clinical presentation, management and outcome in 45 cases. Pituitary 7(3):157–163. doi:10.1007/s11102-005-1050-3
Liu JK, Couldwell WT (2006) Pituitary apoplexy in the magnetic resonance imaging era: clinical significance of sphenoid sinus mucosal thickening. J Neurosurg 104(6):892–898
Arita K, Kurisu K, Tominaga A, Sugiyama K, Ikawa F, Yoshioka H, Sumida M, Kanou Y, Yajin K, Ogawa R (2001) Thickening of sphenoid sinus mucosa during the acute stage of pituitary apoplexy. J Neurosurg 95(5):897–901
Komatsu H, Matsumoto F, Kasai M, Kurano K, Sasaki D, Ikeda K (2013) Cavernous sinus thrombosis caused by contralateral sphenoid sinusitis: a case report. Head Face Med. doi:10.1186/1746-160X-9-9
Acknowledgements
The authors would like to thank colleagues in the departments of endocrinology (Dr Tara Kearney), neuro-radiology (Dr David Hughes) and Neuropathology (Drs Daniel Du Plessis and Piyali Pal) at Salford Royal Foundation Trust for their clinical input in the management of these patients:
Funding
This work was not supported by specific grant funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors have no potential conflicts of interest to disclose.
Ethical approval
This study received ethical approval (reference 08/H1012/50).
Informed consent
Informed consent was taken from all participants in this study.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Humphreys, G.J., Waqar, M., McBain, A.J. et al. Sphenoid sinus microbiota in pituitary apoplexy: a preliminary study. Pituitary 20, 619–623 (2017). https://doi.org/10.1007/s11102-017-0823-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11102-017-0823-9