Abstract
Tuberculosis (TB) is one of the leading cause of death worldwide, and the world is fighting with this global health emergency from the past 25 year. The current clinical interventions for the management of TB face a number of inherent challenges which includes low patient compliance due to the long therapy regimen, and emerging antimicrobial resistance. Therefore, there is an unmet need of new anti-TB therapeutic agent with enhanced safety profile, which can reduce the duration of therapy, enhanced bioavailability and efficacy against drug resistant forms of TB. Bacteriocins or anti microbial peptides (AMPs) occurring in microbes, human beings and other life forms have been investigated as host defense peptides. Structurally AMPs are short and ionized and play crucial role in innate immunity of host. Some AMPs can kill microbial infections directly while others function indirectly by altering the host defense mechanisms. Amidst rising issue of antibiotic resistance, AMPs are being tested in clinical research as potential antibiotics and novel therapeutics to fight against infections and non-infectious diseases. Studies have also highlighted the ability of AMPs to act against the bacteria spreading tuberculosis. The present review provides information on antimicrobial peptides, highlights their biological role, classification and mode of action in treatment and prevention of tuberculosis. It further mentions the prospects and challenges of developing peptides for their therapeutic applications against mycobacterium tuberculosis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Tuberculosis (TB) is an airborne disorder spread by the bacteria Mycobacterium tuberculosis (Mtb) and mostly affects lungs. TB is one of the leading cause of death worldwide, and for the past 25 years the world has been fighting this global health emergency (Furin et al. 2019). TB may exist as latent (bacteria is asleep or dormant) or active (bacteria is making the person sick) phase depending upon the immunity of infected person (Lin and Flynn 2010). The presence of conditions such as human immunodeficiency virus (HIV) infection, malnutrition, diabetes, may predispose the individual towards developing active TB (Narasimhan et al. 2013). Co-infection with HIV increases the pathogenicity of Mtb (Bruchfeld et al. 2015). World Health Organization (WHO) data shows that out of 10 million people diagnosed with TB in the year 2019, 1.2 million deaths were reported from HIV-negative individuals and 0.2 million additional deaths were reported from HIV-positive individuals (World Health Organization 2020). The active case load of TB is not uniform throughout the world. High rates of infection are observed in low to middle income countries of Africa and Southeast Asia (World Health Organization 2020). WHO reports suggest that the cumulative reduction in tuberculosis incidence worldwide was 9% from 2015–2019 (from 142 to 130 new cases per 100 000 population), including a reduction of 2.3% between 2018 and 2019. The incidences of TB in India as well as in Southeast Asian region has also seen a declining trend (Fig. 1). TB is mostly curable; however, it can cause death in case the patient does not get proper treatment. Reduced detection of cases results in lack of treatment for infected person, further posing a challenge for the medical community to control death toll. WHO reports that lockdown and restrictions imposed during COVID-19 may cause an additional 1.4 million deaths due to TB between 2020 and 2025 (World Health Organization, 2020).
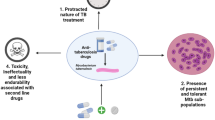
Research for treatment of TB has been going on from several decades, however till date, Bacille Calmette Guerin (BCG) is the only vaccine available. The vaccine consists of live attenuated strain of bacteria and is successful in controlling infection among children. The vaccine is not effective in adults and the routine treatment options for active TB include use of antibiotics as first line of treatment such as streptomycin, rifampicin, isoniazid, pyrazinamide etc. All these antibiotics have lengthy treatment period, ranging from months to year. Currently, the treatment includes administering cocktail of four different drugs, i.e., isoniazid, pyrazinamide, rifampicin, and ethambutol for 2 months followed by 4-month treatment with rifampicin and isoniazid (Silva et al. 2016a, b). Longer treatment months results in lack of patient compliance and adverse drug interactions which may cause the emergence of drug-resistant TB. Two types of drug resistant TB have been reported i.e., Multidrug resistant TB (MDR-TB) and extensively drug-resistant TB (XDR-TB) (Manjelievskaia et al. 2016). MDR-TB cases are treated with second line of treatment options such as fluoroquinolones or injectables (amikacin, capreomycin, and kanamycin) (Rendon et al., 2016). XDR-TB variant shows resistance to first line of drugs as well as to fluoroquinolone and at least one of the injectable of second line treatment (Chan and Iseman 2008) (Table 1). Central Asia and Eastern Europe reports the maximum number of MDR-TB cases (Seung et al. 2015). The 2021 report of WHO indicates that adult men are at highest risk for developing MDR-TB disease, and every year around 3.4% new MDR-TB cases are reported worldwide, while 18% cases are reported in previously treated patients (Shivekar et al. 2020). In 2019, there were 12,350 confirmed cases of XDR-TB (World Health Organization 2020). Drug resistant TB not only increases treatment cost but also causes adverse side-effects. The rise of multidrug-resistant Mtb strains has rendered routine treatment ineffective, underlining the need for novel targeted therapeutic methods (Kurz et al. 2016; Chan and Iseman 2008). AMPs (Antimicrobial peptides) are identified as potential alternative therapy against antimicrobial diseases, such as tuberculosis due to different mode of action (Usmani et al. 2018; Silva et al. 2016a, b; Fox 2013). AMPs participate in innate immunity and act along with cytokines and other host immune modulatory molecules to kill Mtb (Sow et al. 2011). AMPs are 20–60 amino acid biomolecules which play crucial role in innate immunity and can be administered alone or in combination with other drugs for treatment of tuberculosis. The chemical and physical properties of AMPs allow them to act against bacteria, fungi, and viruses (Table 2) (Arranz-Trullén et al. 2017).
This review provides an insight into challenges encountered in treatment of tuberculosis and highlights the need and use of AMPs as therapeutic agents in treating tuberculosis.
Tuberculosis spread by inhaling infectious droplets released as a result of coughing, sneezing, or breathing by an infected active TB patient. The transmission probability depends on the bacterial load in infected sample, the closeness to the person as well as to the duration of exposure (Heemskerk et al. 2015). Once a person is exposed to the bacteria, the immune system of the body reacts to trap bacteria in tubercles or granulomas. Within two years after the primary encounter, the infection progresses to tuberculosis in about 5% of infected patients, while in 10% cases the dormant tubercles get reactivated over the course of several years and the latent infection becomes active TB later in their lifetime (Narasimhan et al. 2013). Studies suggest that one-third of world population suffers from latent TB infection and pose a serious challenge to disease elimination (Dye and Williams 2010). One of the major susceptibility factors of TB include innate and adaptive immune response i.e., alveolar macrophages and dendritic cells. Upon interaction with the pathogen, these immune cells bring about a cascade of signaling pathways activating other immune molecules such as toll-like receptors, heat shock proteins, or inflammatory cytokines (tumor necrosis factors, interleukins, or nitric oxide). However, mycobacterium tuberculosis may evade the macrophage mediated destruction (Sullivan et al. 2012). The local inflammatory milieu stimulates the release of chemokines and cytokines, involved in the mobilization of immune cells like lymphocytes, monocytes, neutrophils, and dendritic cells to the infection site, where they form a granuloma with infected macrophages at the center. Studies suggest that elevated levels of tumour necrosis factor alpha (TNF alpha) inhibit Mtb development and granuloma formation. The granuloma is a signature pathology of TB, which prevent multiplication of mycobacterium, trapping it inside the granuloma walls, thus leads to the prevention from spreading. The unique feature of this structure is the presence of foam cells formed by the differentiation of chronically activated macrophages (Beham et al. 2011; Szereday et al. 2003) (Fig. 2). Thus, the granuloma forms a necrotic zone at its center that helps the bacteria to emit its spread to different parts of the lungs, exhibiting its transmission via aerosols (Beham et al. 2011). People with HIV infection or those who are immune compromised are at a greater risk of developing active TB.
There are five major challenges to TB treatment; (a) lack of adequate treatment and diagnostic options, (b) lack of patient compliance due to long duration and complicated treatment options, (c) multi-drug resistant TB, (d) HIV co-infection (e) implementation of WHO’s Directly observed treatment short course (DOTS) (Murray, 2006).
Antimicrobial peptides (AMPs)
AMPs are cationic, amphipathic in nature, and possess bactericidal activity, which makes them the most effective therapeutic agent against tuberculosis. These anti-microbial peptides have the ability to disrupt normal mycobacterial cell wall function in a variety of ways, and then interact with intracellular targets as well as nucleic acids, enzymes, and organelles (AlMatar et al. 2018). The probability of antimicrobial resistance with AMPs is low due to several reasons i.e. (a) non-specific mode of killing by AMPs, (b) same molecule possess different killing mechanisms (c) mutations rendering bacteria resistant against AMPs are energy intensive and deleterious in some cases (Silva et al. 2016a, b).
Classification of AMPs
Produced by all life-forms, AMPs are 20–60 amino acid residues and are classified based on their source, activity, structural characteristics, and amino acid-rich species (Huan et al. 2020).
-
(1)
On the basis of source: Antimicrobial peptides can be derived from mammals, amphibians, microorganisms, and insects. Mammal derived AMPs include cathelicidins, defensins, casein, lactoferricin B. Mammalian AMPs are present in human, sheep, cattle, and dairy is one of the most important sources of AMPs (Huan et al. 2020). Among amphibians, frogs are the main source of AMP showing the presence of magainin and skin secretions from frog are also found to be rich source of AMPs (Varga et al. 2018). Another AMP reported from amphibians is cancrin. Examples of insect antimicrobial peptides include cecropin and Jellein, while those from microorganisms include nisin and gramicidin (Huan et al. 2020). Another interesting source of AMPs are the marine organisms (Falanga et al. 2016). As-CATH4 (Cathelicidin 4), Myticusin-beta and pardaxin are some of the AMPs obtained from marine environment showing potential immune activity (Huan et al. 2020).
-
(2)
On the basis of activity: AMPs can be classified based on the function i.e., antibacterial (nisin,cecropins, defensins), antiviral (Epi-1), anti-fungal (AurH1), antiparasitic (cathelicidin,temporins, Jellein), anti-human immunodeficiency virus (HIV) (defensins, LL-37, gramicidin D, caerin 1, maximin 3, magainin 2) or anti-tumor peptides (Tritpticin, indolicidin) (Huan et al., 2020).
-
(3)
On the basis of structure: Based on structure, AMPs can be classified as linear α-helical peptides, β-sheet peptides, linear extension structure, and both α-helix and β-sheet peptides (Lei et al. 2019).
-
(4)
On the basis of structural characteristics: AMPs can be divided into pole and carpet models based on their structural features. The pole model of AMP can be further divided into toroidal pore and barrel-stave model. In pole models the AMPs are arranged vertical over the cell membrane, whereas in carpet model they lie parallel to the cell membrane. Examples of pole model include magainin-2, lacticin Q, arenicin (Huan et al. 2020).
-
(5)
On the basis of amino-acid rich species: Some antimicrobial peptides are rich in amino acids such as proline (PrAMPs), tryptophan, arginine, histidine, glycine. Examples of amino acid rich AMPs include indolicidin, triptrpticin, octa-2, HV2, attacins, diptericins (Huan et al. 2020).
AMPs: Mechanism of Action
AMPs play a crucial role in innate immunity and modulate host defense. They possess broad spectrum anti-microbial activity with the ability to kill bacteria, virus, fungi, and parasites (Portell-Buj et al. 2019). Many AMPs have a direct and immediate antibacterial effect by disrupting the integrity of microbial membrane and entering into the cytoplasm of bacteria to react on intracellular targets (Hancock and Diamond 2000). These cationic molecules interact with the anionic surface of microbial membrane, resulting in accumulation of peptide molecules on the surface of membrane (Abedinzadeh et al. 2015). Later the AMPs interact with the cell-wall by forming pore, thinning, altering curvature, localized perturbations or modifying electrostatics (Jenssen et al. 2006; Nguyen et al. 2011; Yeung et al. 2011; Malmsten 2015). This interaction allows the peptide to translocate towards the cytoplasm and interact with intracellular targets i.e., nucleic acids, enzymes, organelles (Giuliani et al. 2007). Due to their amphipathic nature, as indicated in bacterial membrane, AMPs can interact in aqueous and lipid surroundings too (Sohlenkamp and Geiger 2015). AMPs show increased permeability to mycobacterial cell wall (Portell-Buj et al. 2019).
The interaction of AMPs with mammalian cell membrane is quite different from the bacterial membranes. The reason lies in different composition and structure of the mammalian membrane. The mammalian phospholipids are primarily zwitter ionic resulting in net neutral charge, while bacterial membranes have negatively charged outer leaflets (Ebenhan et al. 2014). In mammalian membranes, phospholipids are distributed asymmetrically, with zwitterionic phospholipids in the outer leaflet and negatively charged phospholipids from cytoplasm in the inner leaflet (Lai and Gallo 2009; Zasloff 2002). As a result, interactions between AMPs and mammalian cell membranes are mostly mediated by hydrophobic contacts, which are weak in comparison to electrostatic interactions between AMPs and bacterial membranes. In addition, unlike microorganisms, mammalian cell membranes have significant cholesterol content which stabilizes the phospholipid bilayer and decrease the activity of AMPs (Lai and Gallo 2009).
Because of these structural differences between the membranes, the peptides selectively act on bacterial cells rather than human cells, making them a potential therapeutic to be used against microbes (Matsuzaki 2009) (Fig. 3). The following section discusses the role of AMPs in pathogenesis and elimination of tuberculosis.
Role of AMPs in Elimination of Tuberculosis
Till now, it has become quite clear to us as how AMPs attacks only bacterial cells. This section highlights the possible role of AMPs in tuberculosis.
AMPs interact with the host cells by penetrating in the cells or by modulating host immune response. Several studies show the efficacy of AMPs in inducing autophagy for bacterial death and clearance, e.g., three antimicrobial peptides including Indolicidin induced autophagy mediated cell death in the protozoa Leishmania together with disruption of cell membrane (Bera et al. 2003). The ability of autophagy induction and bacterial clearance makes AMP a potential therapeutic for treatment of tuberculosis.
In order for AMPs to be beneficial, it is crucial that they act at defined concentrations without affecting the host cells. A synthetic AMP, IP-1 (Iztli peptide 1) was reported to induce autophagy by sequestering ATP and helps in elimination of Mtb due to antimicrobial activity (Peláez et al. 2020). Vitamin-D induced AMP cathelicidin (LL-37) acts as anti-infective agent against Mtb (Chung et al. 2020). LL-37 is the active form of cationic AMP cathelicidin and is known to show activity against intra and extracellular Mtb (Deshpande et al. 2020). LL-37 is highly expressed in case of pulmonary tuberculosis and interacts with macrophages and Mtb. Mtb are phagocytosed by macrophages and prevents their degradation by inhibiting formation of acidic phagolysosomes. However, the super resolution microscopy study suggests that this inhibition may be suppressed by LL-37 (Deshpande et al. 2020). The results show that LL-37 is internalized in macrophages with the help of clathrin or lipid-raft. Once inside the infected macrophages, LL-37 enters the phagosomes and brings about degradation of Mtb via cell wall degradation or by inducing cellular degradation. In another study, in-silico analysis was carried out to understand the inhibitory effect of dermcidin AMP on bacterial cell wall component mycolic acid (Banerjee and Gohil, 2016). Mycolic acid is hydroxy fatty acids found in cell wall of Mycolata taxon including Mtb and are known to be crucial for the pathogenicity of bacteria and their existence. Dermcidin on the other hand is an AMP secreted by sweat glands and displays broad spectrum antimicrobial activity against both gram positive and gram-negative pathogenic bacteria. The results of the study show that dermcidin inhibits transfer of mycolic acid to cell wall and interferes with cell wall synthesis (Banerjee and Gohil 2016). Hepcidin is another AMP produced by human liver cells which shows broad spectrum antimicrobial activity (Sow et al. 2011). Studies have shown that hepcidin is localized to mycobacteria-containing phagosomes and shows antimicrobial activity against Mtb. Further, Mtb infection stimulates expression of hepcidin mRNA by innate immune cells in lungs (Sow et al. 2011). Hepcidin expression and induction in immune response highlights the role of AMP in clearing mycobacterium tuberculosis.
Microbial Resistance to AMPs
Antimicrobial peptides like any other protein structure are susceptible to proteases which may bring about their degradation. Certain features of AMPs prevent the microbes to develop resistance against them such as; (a) the concentration of AMPs at the infection site is strictly regulated by its expression, (b) secondly the production of various AMPs occur simultaneously, (c) thirdly the cost of developing resistance against AMPs is high for microbes, (d) fourthly lack of specific target epitopes in structure of AMPs make it difficult for microbes to degrade AMPs and (e) finally the AMPs belong to different structural classes of peptides and destroying single peptide will not result in resistance (Lai and Gallo 2009). There are other structural variations as well, i.e., the presence of disulphide bridges in AMPs such as defensins, protegrin’s, cryptidin-related sequence, make these peptides resistant to proteolysis (Peschel and Sahl 2006). Apart from the presence of disulphide bridges, other features such as thioether bridges, introduction of proline residues and amidation of protease-susceptible C terminal make antimicrobial peptides more resistant towards proteolysis. Further, considering that AMP’s major target is the bacterial cell membrane, it will be complicated for microorganisms to maintain its cell membrane’s functional and structural integrity, while evading AMPs' membrane-disrupting effects (Lai and Gallo 2009).
However, some studies do suggest that in due course of evolution, microbes can develop resistance to AMPs without added fitness cost and AMP resistant strains may even have competitive advantage over wild-type strains (Pränting et al. 2008; Lofton et al. 2013; Andersson et al. 2016). These possibilities may hinder the therapeutic application of AMPs against the microbes.
Clinical Relevance of AMPs
AMPs as the name suggest act as antibiotics killing the microorganisms. Interestingly, due to AMPs unique modus operandi, microbes rarely develop resistance against them. Thus, AMPs can be developed as antibiotic drugs without the problem of antibiotic resistance like the conventional antibiotics (Gallo et al. 2002). AMPs play a regulatory role in various autoimmune and inflammatory disorders, i.e., over-expression of AMPs is associated with dermatological conditions, whereas it is under-expressed in atopic dermatitis which increases infection (Pinheiro Da Silva and MacHado 2012). Use of AMPs as therapeutic in treatment of infected diabetic foot ulcers, oral mucositis, meningococcal meningitis, catheter infections, acne, cardiac ischemia, and fungal infections is currently under research (Gallo et al. 2002). Research suggests that the LL-37 AMP suppresses endotoxin-mediated lethality in rats and mice deficient in Cathelicidin-related Antimicrobial Peptide (CRAMP) and defensin are more susceptible to streptococcal and staphylococcal infections (Pinheiro Da Silva and MacHado 2012). The induction of AMPs (cathelicidin) by the active form of Vitamin D has shown role in cancer progression (Chen et al. 2018). However, the expression of LL-37 AMP shows contrasting effects with both pro-tumorigenic and anti-cancer effects. The expression of LL-37 is up-regulated in human breast cancer, and it promotes tumor growth in lung cancer, whereas LL-37 levels negatively regulate growth of gastric cancers. These findings indicate the probable role of AMPs in treatment of cancer. AMPs can also act as diagnostic markers for detection of various disorder (Pinheiro Da Silva and MacHado 2012).
Only a few AMPs have been approved for clinical usage to date, including polymyxins, which were first introduced in the 1950s (Falagas and Kasiakou 2005; Zavascki et al. 2007; Landman et al. 2008). Polymyxins are administered as topical treatment in the prevention and treatment of local infections. Gram-negative infections caused by drug- resistant microorganisms often require their use as last alternative for intravenous medications (Zavascki et al. 2007). A variety of AMPs are being developed for the treatment of diverse bacterial infections, including pexiganan and omiganan, produced from animal immunological components, and synthetic LTX-109, respectively. Two of the phase III clinical studies, confirmed that Pexiganan can treat bacterial infections associated with diabetic foot ulcers (NCT00563394, NCT00563433) (Lamb and Wiseman 1998; Lipsky et al. 2008), The topical gel for catheter infections (NCT00231153) and rosacea (NCT01784133) has been tested as a derivative of indolicidin, a bovine neutrophil-derived AMP. LTX-109 is a synthetic antimicrobial peptidomimetic that has been tested for local use in moderate Gram- positive skin infections (NCT01223222), impetigo (NCT01803035), and in those with Staphylococcus aureus (S. aureus) nasal colonisation (NCT01158235) (Nilsson et al. 2015). The majority of AMPs such as pexiganan, omiganan, and LTX-109, are designed for indigenous use and a very few are designed for systemic delivery. Additionally, hLF1-11 known as the cationic fraction of human lactoferricin is used as intravenous formulation to treat bacterial and fungal infections in immuno- compromised stem cell transplant recipients (NCT00509938) (Van der Velden et al. 2009). In addition to hLF1-11, a variety of other AMPs are under development for treatment of fungal diseases (Table 3). For example, novexatin, a highly cationic peptide generated from defensins, is used in the treatment of obstinate fungal infections in toes, while CZEN-002, a dimeric peptide extracted from melanocyte-stimulating hormone (MSH), is used to get relief from vaginal candidiasis.
Development of AMPs: Challenges and Clinical Applications
Despite the increasing number of clinical trials on AMPs, there is still lack of literature and studies highlighting the potential use of AMPs as therapeutic agents (Kosikowska and Lesner 2016). Till date, only seven AMPs have been approved by Food and Drug Administration (FDA) for therapeutic uses, though more than 3000 have been discovered. These findings indicate that development and use of AMPs as therapeutic agents is a cumbersome task full of challenges (Chen and Lu 2020).
The screening of identified clusters or expected peptide sequences for antimicrobial and/or fungicidal properties is the first step in the design and optimization of therapeutic AMPs for the treatment of infectious diseases using standard minimal inhibitory concentration (MIC) or minimal microbicidal concentration (MMC) assays (Fjell et al. 2012). However, the anti-fungal and antibacterial activity of AMPs vary with varying environmental conditions making it difficult for researchers to corroborate their in-vivo findings against in-vitro results. This fact poses a major challenge in the use of AMPs as therapeutic agent. The most successful formulation of AMPs are the topical ones as the metabolic stability of AMPs is fairly low, and peptide drugs show low oral bioavailability rendering the oral formulation of AMPs highly difficult (Vlieghe et al. 2010). In addition, the intravenous formulation also suffers from short half-life due to degradation by proteolytic enzymes in blood and liver. Therefore, there is a dire need to enhance the stability of AMPs for their wide use in pharmaceutical companies. Another major drawback in large-scale production of AMPs is the high cost of production which makes it difficult to scale-up the products and market them. Further, AMPs development suffers from lack of toxicology studies and may even face regulatory hindrances due to less clinical data (Vlieghe et al. 2010). Thus, AMPs development and production needs much research and studies in order to be used as an alternative to regular antibiotics.
Conclusion and Future Prospective
Antibiotic resistance as we all know has boggled the scientific community to find alternative solutions. Antimicrobial peptides and inability of most microorganisms to develop resistance against them, shows hope in the future for the use of AMPs as therapeutic agent. The ever-rising cases of tuberculosis with less control measures urges the medical community to find innovative and sustainable ways for using AMPs’ therapeutic potential in treatment and cure of the deadly diseases. Based on review reports, antimicrobial host defense peptides have been proven in various investigations to act against mycobacterium tuberculosis. Natural peptides, as discussed in this paper, are amazing scaffolds for future drug discoveries due to their distinct structural topologies. Exploring the relationship between peptide structure, function as well as the molecular mechanism of action can provide a more thorough understanding of the peptides. This information will be helpful in the development of new molecules with desired properties.
Abbreviations
- TB:
-
Tuberculosis
- AMPs:
-
Antimicrobial peptides
- Mtb:
-
Mycobacterium tuberculosis
- HIV:
-
Human immunodeficiency virus
- WHO:
-
World Health Organization
- Covid-19:
-
Coronavirus disease
- MDR-TB:
-
Multidrug-resistant TB
- XDR-TB:
-
Extensively drug-resistant TB
- EMB:
-
Ethambutol
- PZA:
-
Pyrazinamide
- DNA:
-
Deoxyribonucleic acid
- CATH-4:
-
Cathelicidin 4
- DHPS:
-
Di-hydropteroate synthase
- DHPS:
-
Di-hydrofolate synthase
- TNF:
-
Alpha tumour necrosis factor alpha
- DOTS:
-
Directly observed treatment Short course
- NETs:
-
Neutrophil extracellular traps
- IP-1:
-
Iztli peptide 1
- CRAMP:
-
Cathelicidin-related Antimicrobial Peptide
- FDA:
-
Food and Drug Administration
- MIC:
-
Minimal inhibitory concentration
- MMC:
-
Minimal microbicidal concentration
References
Abedinzadeh M, Gaeini M, Sardari S (2015) Natural antimicrobial peptides against Mycobacterium tuberculosis. J Antimicrob Chemothe 70(5):1285–1289. https://doi.org/10.1093/jac/dku570
AlMatar M, Makky EA, Yakıcı G, Var I, Kayar B, Köksal F (2018) Antimicrobial peptides as an alternative to anti-tuberculosis drugs. Pharmacol Res 128:288–305. https://doi.org/10.1016/j.phrs.2017.10.011
Andersson DI, Hughes D, Kubicek-Sutherland JZ (2016) Mechanisms and consequences of bacterial resistance to antimicrobial peptides. Drug Resist Updates 26:43–57. https://doi.org/10.1016/j.drup.2016.04.002
Arranz-Trullén, J., Lu, L., Pulido, D., Bhakta, S., & Boix, E (2017) Host antimicrobial peptides: The promise of new treatment strategies against tuberculosis. Front Immunol 8:1499 https://doi.org/10.3389/fimmu.2017.01499
Banerjee DI, Gohil TP (2016) Interaction of antimicrobial peptide with mycolyl transferase in Mycobacterium tuberculosis. Int J Mycobacteriology 5(1):83–88. https://doi.org/10.1016/j.ijmyco.2015.07.002
Beham AW, Puellmann K, Laird R, Fuchs T, Streich R, Breysach C, Raddatz D, Oniga S, Peccerella T, Findeisen P, Kzhyshkowska J, Gratchev A, Schweyer S, Saunders B, Wessels JT, Möbius W, Keane J, Becker H, Ganser A, Neumaier M, Kaminski WE (2011) A TNF-regulated recombinatorial macrophage immune receptor implicated in granuloma formation in tuberculosis. PLoS Pathog 7(11):e1002375. https://doi.org/10.1371/journal.ppat.1002375
Bera A, Singh S, Nagaraj R, Vaidya T (2003) Induction of autophagic cell death in Leishmania donovani by antimicrobial peptides. Mol Biochem Parasitol 127(1):23–35. https://doi.org/10.1016/s0166-6851(02)00300-6
Bjerkedal T, Palmer CE (1962) Effect of isoniazid prophylaxis in experimental tuberculosis in guinea pigs. Action of isoniazid in vivo. Am J Hyg 76(2):89–123. https://doi.org/10.1093/oxfordjournals.aje.a120274
Bruchfeld J, Correia-Neves M, Kallenius G (2015) Tuberculosis and HIV coinfection. Cold Spring Harb Perspect Med 5(7):1–15. https://doi.org/10.1101/cshperspect.a017871
Caminero JA, Sotgiu G, Zumla A, Migliori GB (2010) Best drug treatment for multidrug-resistant and extensively drug-resistant tuberculosis. Lancet Infect Dis 10(9):621–629. https://doi.org/10.1016/S1473-3099(10)70139-0
Chan ED, Iseman MD (2008) Multidrug-resistant and extensively drug-resistant tuberculosis: A review. Curr Opin Infect Dis 21(6):587–595. https://doi.org/10.1097/QCO.0b013e328319bce6
Chaturvedi P, Dhanik M, Pande A (2014) Characterization and structural analysis of hepcidin like antimicrobial peptide from schizothorax richardsonii (Gray). Pro J 33(1):1–10. https://doi.org/10.1007/s10930-013-9530-1
Chen CH, Lu TK (2020) Development and challenges of antimicrobial peptides for therapeutic applications. Antibiotics. https://doi.org/10.3390/antibiotics9010024
Chen X, Zou X, Qi G, Tang Y, Guo Y, Si J, Liang L (2018) Roles and mechanisms of human cathelicidin LL-37 in cancer. Cell Physiol Biochem 47(3):1060–1073. https://doi.org/10.1159/000490183
Cherkasov A, Hilpert K, Jenssen H, Fjell CD, Waldbrook M, Mullaly SC, Volkmer R, Hancock RE (2009) Use of artificial intelligence in the design of small peptide antibiotics effective against a broad spectrum of highly antibiotic-resistant superbugs. ACS Chem Biol 4(1):65–74. https://doi.org/10.1021/cb800240j
Chingaté S, Delgado G, Salazar LM, Soto CY (2015) The ATPase activity of the mycobacterial plasma membrane is inhibited by the LL37-analogous peptide LLAP. Peptides 71:222–228. https://doi.org/10.1016/j.peptides.2015.07.021
Chung C, Silwal P, Kim I, Modlin RL, Jo EK (2020) Vitamin D-cathelicidin axis: at the crossroads between protective immunity and pathological inflammation during infection. Immune Netw. https://doi.org/10.4110/in.2020.20.e12
Clarke GBM, O'Hea AJ (1961) Chronic pulmonary tuberculosis treatment with ethionamide combined with cycloserine or oxytetracycline. Br Med J 1:636–8. https://www.jstor.org/stable/20352486
Coxon GD, Craig D, Corrales RM, Vialla E, Gannoun-zaki L, Kremer L (2013) Synthesis antitubercular activity and mechanism of resistance of highly effective thiacetazone analogues. PLoS ONE. https://doi.org/10.1371/journal.pone.0053162
Cuthbert J, Bruce LG (1964) Treatment of pulmonary tuberculosis by capreomycin and pas: a small preliminary trial. Tubercle 45:205–210. https://doi.org/10.1016/s0041-3879(64)80007-6
Deshpande D, Grieshober M, Wondany F, Gerbl F, Noschka R, Michaelis J, Stenger S (2020) Super-resolution microscopy reveals a direct interaction of intracellular mycobacterium tuberculosis with the antimicrobial peptide LL-37. Int J Mol Sci 21(18):6741. https://doi.org/10.3390/ijms21186741
Dye C, Williams BG (2010) The population dynamics and control of tuberculosis. Science 328(5980):856–861. https://doi.org/10.1126/science.1185449
Ebenhan T, Gheysens O, Kruger HG, Zeevaart JR, Sathekge MM (2014) Antimicrobial Peptides Their Role as Infection-Selective Tracers for Molecular Imaging. Internatl, BioMed Res. https://doi.org/10.1155/2014/867381
Falagas ME, Kasiakou SK (2005) Colistin: The revival of polymyxins for the management of multidrug-resistant gram-negative bacterial infections. Clin Infect Dis 40(9):1333–1341. https://doi.org/10.1086/429323
Falanga A, Lombardi L, Franci G, Vitiello M, Iovene MR, Morelli G, Galdiero M, Galdiero S (2016) Marine antimicrobial peptides: Nature provides templates for the design of novel compounds against pathogenic bacteria. Int J Mol Sci. https://doi.org/10.3390/ijms17050785
Finland M (1958) Summary of the monograph on the basic and clinical research of the new antibiotic, kanamycin. Ann N Y Acad Sci. https://doi.org/10.1111/j.1749-6632.1958.tb54725.x
Fjell CD, Hiss JA, Hancock REW, Schneider G (2012) Designing antimicrobial peptides: Form follows function. Nat Rev Drug Discov 11(1):37–51. https://doi.org/10.1038/nrd3591
Fox JL (2013) Antimicrobial peptides stage a comeback. Nat Biotechnol 31(5):379–382. https://doi.org/10.1038/nbt.2572
Furin J, Cox H, Pai M (2019) Tuberculosis. The Lancet 393(10181):1642–1656. https://doi.org/10.1016/S0140-6736(19)30308-3
Gallo RL, Murakami M, Ohtake T, Zaiou M (2002) Biology and Clinical relevance of naturally occurring antimicrobial peptides. J Allergy Clin Immunol 110(6):823–831. https://doi.org/10.1067/mai.2002.129801
Ghobrial O, Derendorf H, Hillman JD (2010) Pharmacokinetic and pharmacodynamic evaluation of the lantibiotic MU1140. J Pharma Sci 99(5):2521–2528. https://doi.org/10.1002/jps
Gilbert DN (1991) Once-daily aminoglycoside therapy. Antimicrob Agents Chemother 35(3):399–405. https://doi.org/10.1128/aac.35.3.399
Gillespie SH, Kennedy N. (1998) Fluoroquinolones: a new treatment for tuberculosis? Int J Tuberc Lung Dis 2: 265–71. https://pubmed.ncbi.nlm.nih.gov/9559396/
Giuliani A, Pirri G, Nicoletto SF (2007) Antimicrobial peptides: An overview of a promising class of therapeutics. Eur. J. Biol, Cent. https://doi.org/10.2478/s11535-007-0010-5
Grumbach F, Rist N (1967) Experimental antitubercular activity of rifampicin, a derivative of rifamycin SV. Rev Tuberc Pneumol 31(6):749–762. https://doi.org/10.2174/157489110790112572
Hancock REW, Diamond G (2000) The role of cationic antimicrobial peptides in innate host defences. Trend Microbiol 8(9):402–410. https://doi.org/10.1016/S0966-842X(00)01823-0
Heemskerk D, Caws M, Marais B, Farrar J (2015). Tuberculosis in Children and Adults. https://doi.org/10.1016/S0140-6736(00)45122-6
Hinshaw HC, Pyle MM, Feldman WH (1947) Streptomycin in tuberculosis. Am J Med 2(5):429–435. https://doi.org/10.1016/0002-9343(47)90087-9
Huan Y, Kong Q, Mou H, Yi H (2020) Antimicrobial peptides: classification, design, application and research progress in multiple fields. Front Microbiol 11:1–21. https://doi.org/10.3389/fmicb.2020.582779
Jenssen H, Hamill P, Hancock REW (2006) Peptide antimicrobial agents. Clin Microbiol Rev 19(3):491–511. https://doi.org/10.1128/CMR.00056-05
Kapoor R, Eimerman PR, Hardy JW, Cirillo JD, Contag CH, Barron AE (2011) Efficacy of antimicrobial peptoids against Mycobacterium tuberculosis. Antimicrob Agents Chemother 55(6):3058–3062. https://doi.org/10.1128/AAC.01667-10
Khara JS, Priestman M, Uhía I, Hamilton MS, Krishnan N, Wang Y, Yang YY, Langford PR, Newton SM, Robertson BD, Ee PLR (2016) Unnatural amino acid analogues of membrane-active helical peptides with anti-mycobacterial activity and improved stability. J Antimicrob Chemother 71(8):2181–2191. https://doi.org/10.1093/jac/dkw107
Kosikowska P, Lesner A (2016) Antimicrobial peptides (AMPs) as drug candidates: a patent review (2003–2015). Expert Opin Ther Pat 26(6):689–702. https://doi.org/10.1080/13543776.2016.1176149
Kurz SG, Furin JJ, Bark CM (2016) Drug-Resistant Tuberculosis: Challenges and Progress. Infect Dis Clin North Am 30(2):509–522. https://doi.org/10.1016/j.idc.2016.02.010
Lai Y, Gallo RL (2009) AMPed up immunity: how antimicrobial peptides have multiple roles in immune defense. Trend Immunol 30(3):131–141. https://doi.org/10.1016/j.it.2008.12.003
Lamb HM, Wiseman LR (1998) Pexiganan acetate. Drugs 56(6):1047–1052. https://doi.org/10.2165/00003495-199856060-00011
Lan Y, Lam JT, Siu GKH, Yam WC, Mason AJ, Lam JKW (2014) Cationic amphipathic D-enantiomeric antimicrobial peptides with in vitro and ex vivo activity against drug-resistant Mycobacterium tuberculosis. Tuberculosis 94(6):678–689. https://doi.org/10.1016/j.tube.2014.08.001
Landman D, Georgescu C, Martin DA, Quale J (2008) Polymyxins revisited. Clin Microbiol Rev 21(3):449–465. https://doi.org/10.1128/CMR.00006-08
Lei J, Sun LC, Huang S, Zhu C, Li P, He J, Mackey V, Coy DH, & He QY (2019). The antimicrobial peptides and their potential clinical applications. Am J Transl Res, 11(7): 3919–3931. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6684887/
Ling LP, Flynn JL (2010) Understanding latent tuberculosis: a moving target. J Immunol 185(1):15–22. https://doi.org/10.4049/jimmunol.0903856
Lipsky BA, Holroyd KJ, Zasloff M (2008) Topical versus systemic antimicrobial therapy for treating mildly infected diabetic foot ulcers: A randomized, controlled, double-blinded, multicenter trial of pexiganan cream. Clin Infect Dis 47(12):1537–1545. https://doi.org/10.1086/593185
Llamas-González YY, Pedroza-Roldán C, Cortés-Serna MB, Márquez-Aguirre AL, Gálvez-Gastélum FJ, Flores-Valdez MA (2013) The synthetic cathelicidin HHC-10 inhibits mycobacterium bovis BCG in vitro and in C57BL/6 mice. Microb Drug Resist 19(2):124–129. https://doi.org/10.1089/mdr.2012.0149
Lofton H, Pränting M, Thulin E, Andersson DI (2013) Mechanisms and fitness costs of resistance to antimicrobial Peptides LL-37, CNY100HL and wheat germ histones. PLoS ONE. https://doi.org/10.1371/journal.pone.0068875
Lucchesi M (1970) The antimycobacterial activity of capreomycin. Antibiot Chemother 16:27–31
Malmsten M (2015) Interactions of antimicrobial peptides with bacterial membranes and membrane components. Curr Top Med Chem 16(1):16–24. https://doi.org/10.2174/1568026615666150703121518
Manjelievskaia J, Erck D, Piracha S, Schrager L (2016) Drug-resistant TB: deadly, costly and in need of a vaccine. Trans R Soc Trop Med Hyg 110(3):186–191. https://doi.org/10.1093/trstmh/trw006
Mansour SC, De La Fuente-Núñez C, Hancock REW (2015) Peptide IDR-1018: Modulating the immune system and targeting bacterial biofilms to treat antibiotic-resistant bacterial infections. J Pept Sci 21(5):323–329. https://doi.org/10.1002/psc.2708
Matsuzaki K (2009) Control of cell selectivity of antimicrobial peptides. Biochim Biophys Acta Biomembrane 1788(8):1687–1692. https://doi.org/10.1016/j.bbamem.2008.09.013
Murray S (2006) Challenges of Tuberculosis Control. CMAJ 174(1):33–34. https://doi.org/10.1503/cmaj.051504
Narasimhan P, Wood J, Macintyre CR, Mathai D (2013) Risk factors for tuberculosis. Pulm Med. https://doi.org/10.1155/2013/828939
Nguyen LT, Haney EF, Vogel HJ (2011) The expanding scope of antimicrobial peptide structures and their modes of action. Trend Biotechnol 29(9):464–472. https://doi.org/10.1016/j.tibtech.2011.05.001
Nilsson AC, Janson H, Wold H, Fugelli A, Andersson K, Håkangård C, Olsson P, Olsen WM (2015) Ltx-109 is a novel agent for nasal decolonization of methicillin-resistant and -sensitive staphylococcus aureus. Antimicrob Agents Chemother 59(1):145–151. https://doi.org/10.1128/AAC.03513-14
Palomino JC, Martin A (2014) Drug resistance mechanisms in Mycobacterium tuberculosis. Antibiotics 3(3):317–340. https://doi.org/10.3390/antibiotics3030317
Peláez Coyotl EA, Barrios Palacios J, Muciño G, Moreno-Blas D, Costas M, Montiel Montes T, Diener C, Uribe-Carvajal S, Massieu L, Castro-Obregón S, Espinosa OR (2020) Antimicrobial Peptide against Mycobacterium Tuberculosis That Activates Autophagy Is an Effective Treatment for Tuberculosis. Pharmaceutics. https://doi.org/10.3390/pharmaceutics12111071
Peschel A, Sahl HG (2006) The co-evolution of host cationic antimicrobial peptides and microbial resistance. Nat Rev Microbiol 4(7):529–536. https://doi.org/10.1038/nrmicro1441
Pinheiro Da Silva F, MacHado MCC (2012) Antimicrobial peptides: Clinical relevance and therapeutic implications. Peptides 36(2):308–314. https://doi.org/10.1016/j.peptides.2012.05.014
Portell-Buj E, Vergara A, Alejo I, López-Gavín A, Rosa Montè M, San Nicolàs L, Gonzàlez-Martín J, Tudó G (2019) In vitro activity of 12 antimicrobial peptides against mycobacterium tuberculosis and mycobacterium avium clinical isolates. J Med Microbiol 68(2):211–215. https://doi.org/10.1099/jmm.0.000912
Pränting M, Negrea A, Rhen M, Andersson DI (2008) Mechanism and fitness costs of PR-39 resistance in Salmonella enterica serovar typhimurium LT2. Antimicrob Agents Chemother 52(8):2734–2741. https://doi.org/10.1128/AAC.00205-08
Pulido D, Torrent M, Andreu D, Nogues MV, Boix E (2013) Two human host defense ribonucleases against mycobacteria, the eosinophil cationic protein (RNase 3) and RNase 7. Antimicrob Agents Chemother 57(8):3797–3805. https://doi.org/10.1128/AAC.00428-13
Ramón-García S, Mikut R, Ng C, Ruden S, Volkmer R, Reischl M, Hilpert K, Thompson CJ (2013) Targeting mycobacterium tuberculosis and other microbial pathogens using improved synthetic antibacterial peptides. Antimicrob Agents Chemother 57(5):2295–2303. https://doi.org/10.1128/AAC.00175-13
Rendon A, Tiberi S, Scardigli A, D’Ambrosio L, Centis R, Caminero JA, Migliori GB (2016) Classification of drugs to treat multidrug-resistant tuberculosis (MDR-TB) Evidence and perspectives. J Thorac Dis 8(10):2666–2671. https://doi.org/10.21037/jtd.2016.10.14
Rivas-Santiago B, Castañeda-Delgado JE, Rivas Santiago CE, Waldbrook M, González-Curiel I, León-Contreras JC, Enciso-Moreno JA, Villar V.del, Mendez-Ramos, J, Hancock, REW, & Hernandez-Pando R, (2013a) Ability of innate defence regulator peptides IDR-1002, IDR-HH2 and IDR-1018 to protect against mycobacterium tuberculosis infections in animal models. PLoS ONE. https://doi.org/10.1371/journal.pone.0059119
Rivas-Santiago B, Rivas Santiago CE, Castañeda-Delgado JE, León-Contreras JC, Hancock REW, Hernandez-Pando R (2013b) Activity of LL-37, CRAMP and antimicrobial peptide-derived compounds E2, E6 and CP26 against Mycobacterium tuberculosis. Int J Antimicrob Agents 41(2):143–148. https://doi.org/10.1016/j.ijantimicag.2012.09.015
Rodríguez A, Villegas E, Montoya-Rosales A, Rivas-Santiago B, Corzo G (2014) Characterization of antibacterial and hemolytic activity of synthetic pandinin 2 variants and their inhibition against Mycobacterium tuberculosis. PLoS ONE 9(7):101742. https://doi.org/10.1371/journal.pone.0101742
Ross KF, Herzberg MC (2001) Calprotectin expression by gingival epithelial cells. Infect Immun 69:3248–3254. https://doi.org/10.1128/IAI.69.5.3248-3254.2001
Santos P, Gordillo A, Osses L, Salazar LM, Soto CY (2012) Effect of antimicrobial peptides on ATPase activity and proton pumping in plasma membrane vesicles obtained from mycobacteria. Peptides 36(1):121–128. https://doi.org/10.1016/j.peptides.2012.04.018
Schluger NW (2013) Fluoroquinolones in The treatment of tuberculosis: Which is best? Am J Respir Crit Care Med 188(7):768–769. https://doi.org/10.1164/rccm.201308-1446ED
Seung KJ, Keshavjee S, Rich ML (2015) Multidrug-resistant tuberculosis and extensively drug-resistant tuberculosis. Cold Spring Harb Perspect Med 5(9):a017863
Sharma A, Pohane AA, Bansal S, Bajaj A, Jain V, Srivastava A (2015) Cell penetrating synthetic antimicrobial peptides (SAMPs) exhibiting potent and selective killing of Mycobacterium by targeting its DNA. Chem Eur J 21(9):3540–3545. https://doi.org/10.1002/chem.201404650
Shi W, Zhang X, Jiang X, Yuan H, Lee JS, Barry CE, Wang H, Zhang W, Zhang Y (2011) Pyrazinamide inhibits trans-translation in Mycobacterium tuberculosis. Science 333(6049):1630–1632. https://doi.org/10.1126/science.1208813
Shivekar SS, Kaliaperumal V, Brammacharry U, Sakkaravarthy A, Raj CKV, Alagappan C, Muthaiah M (2020) Prevalence and factors associated with multidrug-resistant tuberculosis in South India. Sci Rep 10(1):1–11. https://doi.org/10.1038/s41598-020-74432-y
Silva JP, Appelberg R, Gama FM (2016a) Antimicrobial peptides as novel anti-tuberculosis therapeutics. Biotechnol Adv 34(5):924–940. https://doi.org/10.1016/j.biotechadv.2016.05.007
Silva JP, Gonçalves C, Costa C, Sousa J, Silva-Gomes R, Castro AG, Pedrosa J, Appelberg R, Gama FM (2016b) Delivery of LLKKK18 loaded into self-assembling hyaluronic acid nanogel for tuberculosis treatment. J Control Release 235:112–124. https://doi.org/10.1016/j.jconrel.2016.05.064
Sohlenkamp C, Geiger O (2015) Bacterial membrane lipids: diversity in structures and pathways. FEMS Microbiol Rev 40(1):133–159. https://doi.org/10.1093/femsre/fuv008
Sow FB, Nandakumar S, Velu V, Kellar KL, Schlesinger LS, Amara RR, Lafuse WP, Shinnick TM, Sable SB (2011) Mycobacterium tuberculosis components stimulate production of the antimicrobial peptide hepcidin. Tuberculosis 91(4):314–321. https://doi.org/10.1016/j.tube.2011.03.003
Sullivan JT, Young EF, Mccann JR, Braunstein M (2012) The mycobacterium tuberculosis SecA2 system subverts phagosome maturation to promote growth in macrophages. Infect Immun 80(3):996–1006. https://doi.org/10.1128/IAI.05987-11
Szereday L, Baliko Z, Szekeres-Bartho J (2003) Gamma/delta T cell subsets in patients with active Mycobacterium tuberculosis infection and tuberculin anergy. Clin Exp Immunol 131(2):287–291. https://doi.org/10.1046/j.1365-2249.2003.02063.x
Usmani SS, Kumar R, Kumar V, Singh S, Raghava GPS (2018) AntiTbPdb: A knowledgebase of anti-tubercular peptides. Database 2018:1–8. https://doi.org/10.1093/database/bay025
Van der Velden WJFM, van Iersel TMP, Blijlevens NMA, Donnelly JP (2009) Safety and tolerability of the antimicrobial peptide human lactoferrin 1–11 (hLF1-11). BMC Med 7:44. https://doi.org/10.1186/1741-7015-7-44
Varga JFA, Bui-Marinos MP, Katzenback BA (2018) Frog skin innate immune defences: sensing and surviving pathogens. Front Immunol 9:3128
Vlieghe P, Lisowski V, Martinez J, Khrestchatisky M (2010) Synthetic therapeutic peptides: science and market. Drug Discov Today 15(1–2):40–56. https://doi.org/10.1016/j.drudis.2009.10.009
Wiesner J, Vilcinskas A (2010) Antimicrobial peptides: The ancient arm of the human immune system. In Virulence 1(5):440–464. https://doi.org/10.4161/viru.1.5.12983
World Health Organization (2020) Tuberculosis Report. In Baltimore Health News: XLIX (Issues 9–10–11)
Yeager R, Munroe W, Dessau F. Pyrazinamide (1952) (Aldinamide) in the treatment of pulmonary tuberculosis. Am Rev Tuberc 65,523–534. https://pubmed.ncbi.nlm.nih.gov/14924175/
Yeung ATY, Gellatly SL, Hancock REW (2011) Multifunctional cationic host defence peptides and their clinical applications. Cell Mol Life Sci 68(13):2161–2176. https://doi.org/10.1007/s00018-011-0710-x
Yew WW, Lee J, Chan CY, Cheung SW, Wong PC, Kwan SY (1991) Ofloxacin penetration into tuberculous pleural effusion. Antimicrob Agents Chemother 35(10):2159–2160. https://doi.org/10.1128/aac.35.10.2159
Zasloff M (2002) Antimicrobial peptides of multicellular organisms. Nature 415:389–395. https://doi.org/10.3138/9781487589684-006
Zavascki AP, Goldani LZ, Li J, Nation RL (2007) Polymyxin B for the treatment of multidrug-resistant pathogens: A critical review. J Antimicrob Chemother 60(6):1206–1215. https://doi.org/10.1093/jac/dkm357
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Mehta, K., Sharma, P., Mujawar, S. et al. Role of Antimicrobial Peptides in Treatment and Prevention of Mycobacterium Tuberculosis: A Review. Int J Pept Res Ther 28, 132 (2022). https://doi.org/10.1007/s10989-022-10435-9
Accepted:
Published:
DOI: https://doi.org/10.1007/s10989-022-10435-9