Abstract
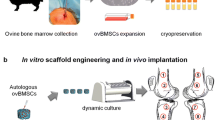
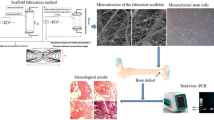
The aim of this study was to evaluate the effects of highly porous Biosilicate® scaffolds on bone healing in a tibial bone defect model in rats by means of histological evaluation (histopathological and immunohistochemistry analysis) of the bone callus and the systemic inflammatory response (immunoenzymatic assay). Eighty Wistar rats (12 weeks-old, weighing ±300 g) were randomly divided into 2 groups (n = 10 per experimental group, per time point): control group and Biosilicate® group (BG). Each group was euthanized 3, 7, 14 and 21 days post-surgery. Histological findings revealed a similar inflammatory response in both experimental groups, 3 and 7 days post-surgery. During the experimental periods (3–21 days post-surgery), it was observed that the biomaterial degradation, mainly in the periphery region, provided the development of the newly formed bone into the scaffolds. Immunohistochemistry analysis demonstrated that the Biosilicate® scaffolds stimulated cyclooxygenase-2, vascular endothelial growth factor and runt-related transcription factor 2 expression. Furthermore, in the immunoenzymatic assay, BG presented no difference in the level of tumor necrosis factor alpha in all experimental periods. Still, BG showed a higher level of interleukin 4 after 14 days post-implantation and a lower level of interleukin 10 in 21 days post-surgery. Our results demonstrated that Biosilicate® scaffolds can contribute for bone formation through a suitable architecture and by stimulating the synthesis of markers related to the bone repair.









Similar content being viewed by others
References
Phieffer LS, Goulet JA. Delayed unions of the Tibia. J Bone Joint Surg Am. 2006;88:205–16.
Axelrad TW, Kakar S, Einhorn TA. New technologies for the enhancement of skeletal repair. Injury. 2007;38:S49–62.
Välimäki V, Yrjans JJ, Vuorio E, Aro HT. Combined effect of bone morphogenetic protein-2 gene therapy and bioactive glass microspheres in enhancement of new bone formation. J Biomed Mater Res. 2005;75:501–9.
Drosse I, Volkmer E, Seitz S, Seitz H, Penzkofer R, Zahn K, Matis U, Mutschler W, Augat P, Schieker M. Validation of a femoral critical size defect model for orthotopic evaluation of bone healing: a biomechanical, veterinary and trauma surgical perspective. Tissue Eng Part C Methods. 2008;14:79–88.
Bhatt RA, Rozental TD. Bone graft substitutes. Hand Clin. 2012;28:457–68.
Nandi SK, Roy S, Mukherjee P, Kundu B, De DK, Basu D. Orthopaedic applications of bone graft and graft substitutes: a review. Indian J Med Res. 2010;132:15–30.
Dorozhkin S. Calcium orthophosphate-based biocomposites and hybrid biomaterials. J Mater Sci. 2009;44:2343–87.
Hutmacher DW, Schantz JT, Lam CX, Tan KC, Lim TC. State of the art and future directions of scaffold-based bone engineering from a biomaterials perspective. J Tissue Eng Regen Med. 2007;1:245–60.
Renno AC, Bossini PS, Crovace MC, Rodrigues AC, Zanotto ED, Parizotto NA. Characterization and in vivo biological performance of biosilicate. Biomed Res Int. 2013;. doi:10.1155/2013/141427.
De Long WG Jr, Einhorn TA, Koval K, McKee M, Smith W, Sanders R, Watson T. Bone grafts and bone graft substitutes in orthopaedic trauma surgery. A critical analysis. J Bone Joint Surg Am. 2007;89:649–58.
Hak DJ. The use of osteoconductive bone graft substitutes in orthopaedic trauma. J Am Acad Ortho Surg. 2007;15:525–36.
Ohtsuki C, Kamitakahara M, Miyazaki T. Bioactive ceramic-based materials with designed reactivity for bone tissue regeneration. J R Soc Interface. 2009;6:S349–60.
Hench LL, Xynos ID, Polak JM. Bioactive glasses for in situ tissue regeneration. J Biomater Sci Polym Ed. 2004;15:543–62.
Hu YC, Zhong JP. Osteostimulation of bioglass. Chin Med J. 2009;122:2386–9.
Xin R, Zhang Q, Gao J. Identification of the wollastonite phase in sintered 45S5 bioglass and its effect on in vitro bioactivity. J Non Cryst Solids. 2010;356:1180–4.
Hench LL, Polak JM. Third-generation biomedical materials. Science. 2002;295:1014–7.
Peitl Filho O, LaTorre GP, Hench LL. Effect of crystallization on apatite-layer formation of bioactive glass 45S5. J Biomed Mater Res. 1996;30:509–14.
Kido HW, Oliveira P, Parizotto NA, Crovace MC, Zanotto ED, Peitl-Filho O, Fernandes KP, Mesquita-Ferrari RA, Ribeiro DA, Renno AC. Histopathological, cytotoxicity and genotoxicity evaluation of Biosilicate® glass-ceramic scaffolds. J Biomed Mater Res A. 2013;101:667–73.
Moura J, Teixeira LN, Ravagnani C, Peitl O, Zanotto ED, Beloti MM, Panzeri H, Rosa AL, De Oliveira PT. In vitro osteogenesis on a highly bioactive glass–ceramic (Biosilicate®). J Biomed Mater Res A. 2007;82:545–57.
Bossini PS, Rennó AC, Ribeiro DA, Fangel R, Peitl O, Zanotto ED, Parizotto NA. Biosilicate® and low-level laser therapy improve bone repair in osteoporotic rats. J Tissue Eng Regen Med. 2011;5:229–37.
Granito RN, Renno AC, Ravagnani C, Bossini PS, Mochiuti D, Jorgetti V, Driusso P, Peitl O, Zanotto ED, Parizotto NA, Oishi J. In vivo biological performance of a novel highly bioactive glass-ceramic (Biosilicate®): a biomechanical and histomorphometric study in rat tibial defects. J Biomed Mater Res B Appl Biomater. 2011;97:139–47.
Wu C, Zhu Y, Chang J, Zhang Y, Xiao Y. Bioactive inorganic-materials/alginate composite microspheres with controllable drug-delivery ability. J Biomed Mater Res B Appl Biomater. 2010;94:32–43.
Sachot N, Castaño O, Mateos-Timoneda MA, Engel E, Planell JA. Hierarchically engineered fibrous scaffolds for bone regeneration. J R Soc Interface. 2013;10:20130684.
Paşcu EI, Stokes J, McGuinness GB. Electrospun composites of PHBV, silk fibroin and nano-hydroxyapatite for bone tissue engineering. Mater Sci Eng C Mater Biol Appl. 2013;33:4905–16.
Pinto KN, Tim CR, Crovace MC, Matsumoto MA, Parizotto NA, Zanotto ED, Peitl O, Renno AC. Effects of Biosilicate® scaffolds and low-level laser therapy on the process of bone healing. Photomed Laser Surg. 2013;31:252–60.
Schieker M, Seitz H, Drosse I, Seitz S, Mutschler W. Biomaterials as scaffold for bone tissue engineering. Eur J Trau ma. 2006;32:114–24.
Zanotto ED, Ravagnani C, Peitl O, Panzeri H, Lara EH. Process and compositions for preparing particulate, bioactive or resorbable biosilicates for use in the treatment of oral ailments. Sao Carlos: Universidade Federal de Sao Carlos, Universidade de Sao Paulo; 2004. International Classification C03C10/00, WO 2004/074199 (INPI 03006441).
Crovace MC. Obtencão de estruturas porosas altamente bioativas via sinterização do Biosilicate®. Dissertation (MSc in Materials Engineering), Post-Graduate Program in Science and Materials Engineering, Federal University of Sao Carlos, Sao Carlos; 2009.
Oliveira P, Ribeiro DA, Pipi EF, Driusso P, Parizotto NA, Renno AC. Low-level laser therapy does not modulate the outcomes of a highly bioactive glassceramic (Biosilicate®) on bone consolidation in rats. J Mater Sci Mater Med. 2010;21:1379–84.
Pape HC, Marcucio R, Humphrey C, Colnot C, Knobe M, Harvey EJ. Trauma-induced inflammation and fracture healing. J Orthop Trauma. 2010;24:522–5.
Gauthier O, Müller R, von Stechow D, Lamy B, Weiss P, Bouler JM, Aguado E, Daculsi G. In vivo bone regeneration with injectable calcium phosphate biomaterial: a three-dimensional micro-computed tomographic, biomechanical and SEM study. Biomaterials. 2005;26:5444–53.
Link DP, Van den dolder J, Van den Beucken JJJP, Cuijpers VM, Wolke JGC, Mikos AG, Jansen JA. Evaluation of the biocompatibility of calcium phosphate cement/PLGA microparticle composites. J Biomed Mater Res A. 2008;87:760–9.
Xynos ID, Edgar AJ, Buttery LDK, Hench LL, Polak JM. Ionic products of bioactive glass dissolution increase proliferation of human osteoblasts and induce insulin-like growth factor II mRNA expression and protein synthesis. Biochem Biophys Res Commun. 2000;276:461–5.
Anderson JM, Mcnally AK. Biocompatibility of implants: lymphocyte/macrophage interactions. Semin Immunopathol. 2011;33:221–33.
Granito RN, Ribeiro DA, Rennó AC, Ravagnani C, Bossini PS, Peitl-Filho O, Zanotto ED, Parizotto NA, Oishi J. Effects of biosilicate and bioglass 45S5 on tibial bone consolidation on rats: a biomechanical and a histological study. J Mater Sci Mater Med. 2009;20:2521–6.
Matsumoto MA, Holgado LA, Renno ACM, Caviquioli G, Biguetti CC, Saraiva PP, Kawakami RY. A novel bioactive vitroceramic presents similar biological responses as autogenous bone grafts. J Mater Sci Mater Med. 2012;23:1447–56.
Karageorgiou V, Kaplan D. Porosity of 3D biomaterial scaffolds and osteogenesis. Biomaterials. 2005;26:5474–91.
Salgado AJ, Coutinho OP, Reis RL. Bone tissue engineering: state of the art and future trends. Macromol Biosci. 2004;4:743–65.
Zhang X, Schwarz EM, Young DA, Puzas E, Rosier RN, O’keefe RJ. Cyclo-oxygenase-2 regulates mesenchymal cell differentiation into the osteoblast lineage and is critically involved in bone repair. J. Clin. Invest. 2002;109:1405–15.
Komori T. Regulation of skeletal development by the Runx family of transcription factors. J Cell Biochem. 2005;95:445–53.
Keramarisa NC, Calorib GM, Nikolaoua VS, Schemitschc EH, Giannoudisa PV. Fracture vascularity and bone healing: a systematic review of the role of VEGF. Injury. 2008;39:S45–57.
Hallab NJ, Jacobs JJ. Biologic Effects of Implant Debris. Bull NYU Joint Dis. 2009;67:182–8.
Shioi A, Teitelbaum SL, Ross FP, Welgus HG, Suzuki H, Ohara J, Lacey DL. Interleukin 4 inhibits murine osteoclast formation in vitro. J Cell Biochem. 1991;47:272–7.
Acknowledgments
The authors thank FAPESP (Fundação de Amparo à Pesquisa do Estado de São Paulo) for their financial support.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kido, H.W., Tim, C.R., Bossini, P.S. et al. Porous bioactive scaffolds: characterization and biological performance in a model of tibial bone defect in rats. J Mater Sci: Mater Med 26, 74 (2015). https://doi.org/10.1007/s10856-015-5411-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10856-015-5411-9