Abstract
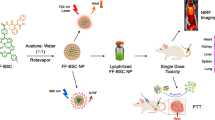
Under the inspiration of polydopamine melanin, a new dopamine-modified poly(aspartic acid) derivative, poly(α,β-(N-(3,4-dihydroxyphenylethyl)-l-aspartamide-co-α,β-N-(2-hydroxyethyl)-l-aspartamide) (PDAEA), was successfully synthesized by successive aminolysis reactions of polysuccinimide with dopamine and ethanolamine. The mixtures composed of PDAEA and FeCl3 exhibited an excellent photothermal property under the irradiation of near-infrared (NIR) laser. The interactions between PDAEA and FeCl3 were investigated by ultraviolet–visible (UV–Vis) spectroscopic, Fourier transformation infrared (FT-IR) spectroscopic, and visual colorimetric measurements. Additionally, PDAEA could interact with Fe3+ in water to form spherical nanostructures with a size of 116 nm, apt to aggregate at the tumor site via the enhanced permeability and retention effect (EPR effect), implying that toxic and side effects of traditional therapy might be reduced using this method. MTT assay demonstrated both PDAEA and the obtained complex products possessed good cytocompatibility to NIH-3T3 cells (more than 90 % cell viability). The effect of photothermal therapy in vitro was also evaluated qualitatively under certain conditions using an inverted fluorescence microscope. All the results indicated that the dopamine-modified poly(aspartic acid) derivative was a promising candidate as an efficient NIR photothermal therapeutic agent for cancer therapy.












Similar content being viewed by others
References
Parola P (2013) The return of the big three killers. Clin Microbiol Infec 19:887–888
Yoo D, Lee J, Shin T, Cheon J (2011) Theranostic magnetic nanoparticles. Acc Chem Res 44:863–874
American Cancer Society (2011) Global cancer facts & figures, 2nd edn. American Cancer Society, Atlanta
Kievit FM, Zhang M (2011) Surface engineering of iron oxide nanoparticles for targeted cancer therapy. Acc Chem Res 44:853–862
Vogel A, Venugopalan V (2003) Mechanisms of pulsed laser ablation of biological tissues. Chem Rev 103:577–644
Huang X, El-Sayed MA (2011) Plasmonic photo-thermal therapy (PPTT). Alex J Med 47:1–9
Liu J, Han J, Kang Z, Golamaully R, Xu N, Li H, Han X (2014) In vivo near-infrared photothermal therapy and computed tomography imaging of cancer cells using novel tungsten-based theranostic probe. Nanoscale 6:5770–5776
Yang K, Xu H, Cheng L, Sun C, Wang J, Liu Z (2012) In vitro and in vivo near-infrared photothermal therapy of cancer using polypyrrole organic nanoparticles. Adv Mater 24:5586–5592
Fitzgerald M, Hodgetts S, Heuvel CVD, Natoli R, Hart NS, Valter K, Harvey AR, Vink R, Provis J, Dunlop SA (2013) Red/near-infrared irradiation therapy for treatment of central nervous system injuries and disorders. Rev Neurosci 24:205–226
Chen S, Lin S, Lai M, Peng C, Lai C (2013) Therapeutic effects of near-infrared radiation on chronic neck pain. J Exp Clin Med 5:131–135
Huang P, Gao Y, Lin J, Hu H, Liao H, Yan X, Tang Y, Jin A, Song J, Niu G, Zhang G, Horkay F, Chen X (2015) Tumor-specific formation of enzyme-instructed supramolecular self-assemblies as cancer theranostics. ACS Nano 9:9517–9527
Choi WI, Kim J, Kang C, Byeon CC, Kim YH, Tae G (2011) Tumor regression in vivo by photothermal therapy based on gold-nanorod-loaded, functional nanocarriers. ACS Nano 5:1995–2003
Burke AR, Singh RN, Carroll DL, Wood JCS, D’Agostino RB Jr, Ajayan PM, Torti FM, Torti SV (2012) The resistance of breast cancer stem cells to conventional hyperthermia and their sensitivity to nanoparticle-mediated photothermal therapy. Biomaterials 33:2961–2970
Maeda H, Wu J, Sawa T, Matsumura Y, Horic K (2000) Tumor vascular permeability and the EPR effect in macromolecular therapeutics: a review. J Control Release 65:271–284
Jaque D, Maestro LM, Rosal B, Haro-Gonzalez P, Benayas A, Plaza JL, Rodrigueza EM, Sole JG (2014) Nanoparticles for photothermal therapies. Nanoscale 6:9494–9530
Huang X, El-Sayed IH, Qian W, El-Sayed MA (2006) Cancer cell imaging and photothermal therapy in the near-infrared region by using gold nanorods. J Am Chem Soc 128:2115–2120
Tong L, Zhao Y, Huff TB, Hansen MN, Wei A, Cheng J (2007) Gold nanorods mediate tumor cell death by compromising membrane integrity. Adv Mater 19:3136–3141
Chen J, Wang D, Xi J, Au L, Siekkinen A, Warsen A, Li Z, Zhang H, Xia Y, Li X (2007) Immuno gold nanocages with tailored optical properties for targeted photothermal destruction of cancer cells. Nano Lett 7:1318–1322
Chen J, Glaus C, Laforest R, Zhang Q, Yang M, Gidding M, Welch MJ, Xia Y (2010) Gold nanocages as photothermal transducers for cancer treatment. Small 6:811–817
Boca SC, Potara M, Gabudean A, Juhem A, Baldeck PL, Astilean S (2011) Chitosan-coated triangular silver nanoparticles as a novel class of biocompatible, highly effective photothermal transducers for in vitro cancer cell therapy. Cancer Lett 311:131–140
Cheng L, Huang J, Chen HM, Lai T, Yang K, Liu R, Hsiao M, Chen C, Her L, Tsai DP (2012) Seedless, silver-induced synthesis of star-shaped gold/silver bimetallic nanoparticles as high efficiency photothermal therapy reagent. J Mater Chem 22:2244–2253
Huang X, Tang S, Mu X, Dai Y, Chen G, Zhou Z, Ruan F, Yang Z, Zheng N (2011) Freestanding palladium nanosheets with plasmonic and catalytic properties. Nat Nanotechnol 6:28–32
Zhou M, Zhang R, Huang M, Lu W, Song S, Melancon MP, Tian M, Liang D, Li C (2010) A chelator-free multifunctional [64Cu]CuS nanoparticle platform for simultaneous micro-PET/CT imaging and photothermal ablation therapy. J Am Chem Soc 132:15351–15358
Tian Q, Tang M, Sun Y, Zou R, Chen Z, Zhu M, Yang S, Wang J, Wang J, Hu J (2011) Hydrophilic flower-like CuS superstructures as an efficient 980 nm laser-driven photothermal agent for ablation of cancer cells. Adv Mater 23:3542–3547
Markovic ZM, Harhaji-Trajkovic LM, Todorovic-Markovic BM, Kepic DP, Arsikin KM, Jovanovic SP, Pantovic AC, Dramicanin MD, Trajkovic VS (2011) In vitro comparison of the photothermal anticancer activity of graphene nanoparticles and carbon nanotubes. Biomaterials 32:1121–1129
Yang K, Wan J, Zhang S, Tian B, Zhang Y, Liu Z (2012) The influence of surface chemistry and size of nanoscale graphene oxide on photothermal therapy of cancer using ultra-low laser power. Biomaterials 33:2206–2214
Robinson JT, Tabakman SM, Liang Y, Wang H, Casalongue HS, Vinh D, Dai H (2011) Ultrasmall reduced graphene oxide with high near-infrared absorbance for photothermal therapy. J Am Chem Soc 133:6825–6831
Sharifi S, Behzadi S, Laurent S, Forrest ML, Stroeve P, Mahmoudi M (2012) Toxicity of nanomaterials. Chem Soc Rev 41:2323–2343
Kvítek O, Siegel J, Hnatowicz V, ŠvorIík V (2013) Noble metal nanostructures influence of structure and environment on their optical properties. J Nanomater 2013:1–15
Li Y, Chen C (2011) Fate and toxicity of metallic and metal-containing nanoparticles for biomedical applications. Small 7:2965–2980
Yang S, Luo J, Zhou Q, Wang H (2012) Pharmacokinetics, metabolism and toxicity of carbon nanotubes for bio-medical purposes. Theranostics 2:271–282
Andrew TL, Swager TM (2008) Reduced photobleaching of conjugated polymer films through small molecule additives. Macromolecules 41:8306–8308
Lovell JF, Jin CS, Huynh E, Jin H, Kim C, Rubinstein JL, Chan WCW, Cao W, Wang LV, Zheng G (2011) Porphysome nanovesicles generated by porphyrin bilayers for use as multimodal biophotonic contrast agents. Nat Mater 10:324–332
Lovell JF, Jin CS, Huynh E, MacDonald TD, Cao W, Zheng G (2012) Enzymatic regioselection for the synthesis and biodegradation of porphysome nanovesicles. Angew Chem Int Ed 51:2429–2433
Simon JD (2000) Spectroscopic and dynamic studies of the epidermal chromophores trans-urocanic acid and eumelanin. Accounts Chem Res 33:307–313
Liu Y, Ai K, Lu L (2014) Polydopamine and its derivative materials: synthesis and promising applications in energy, environmental, and biomedical fields. Chem Rev 114:5057–5115
Liu Y, Ai K, Liu J, Deng M, He Y, Lu L (2013) Dopamine-melanin colloidal nanospheres: an efficient near-infrared photothermal therapeutic agent for in vivo cancer therapy. Adv Mater 25:1353–1359
Black KC, Yi J, Rivera JG, Zelasko-Leon DC, Messersmith PB (2013) Polydopamine-enabled surface functionalization of gold nanorods for cancer cell-targeted imaging and photothermal therapy. Nanomedicine (Lond) 8:17–28
Zheng R, Wang S, Tian Y, Jiang X, Fu D, Shen S, Yang W (2015) Polydopamine-coated magnetic composite particles with an enhanced photothermal effect. ACS Appl Mater Interfaces 7:15876–15884
Zhang R, Su S, Hu K, Shao L, Deng X, Sheng W, Wu Y (2015) Smart micelle@polydopamine core-shell nanoparticles for highly effective chemo–photothermal combination therapy. Nanoscale 7:19722–19731
Wang X, Zhang J, Wang Y, Wang C, Xiao J, Zhang Q, Cheng Y (2016) Multi-responsive photothermal-chemotherapy with drug-loaded melanin-like nanoparticles for synergetic tumor ablation. Biomaterials 81:114–124
Hu Z, Zhao F, Wang Y, Huang Y, Chen L, Li N, Li J, Li Z, Yi G (2014) Facile fabrication of a C60–polydopamine-graphene nanohybrid for single light induced photothermal and photodynamic therapy. Chem Commun 50:10815–10818
Lin L, Cong Z, Cao J, Ke K, Peng Q, Gao J, Yang H, Liu G, Chen X (2014) Multifunctional Fe3O4@polydopamine coreshell nanocomposites for intracellular mRNA detection and imaging-guided photothermal therapy. ACS Nano 8:3876–3883
Kang HS, Yang SR, Kim J, Han S, Chang I (2001) Effects of grafted alkyl groups on aggregation behavior of amphiphilic poly(aspartic acid). Langmuir 17:7501–7506
Huang S, Yang L, Liu M, Phua SL, Yee WA, Liu W, Zhou R, Lu X (2013) Complexes of polydopamine-modified clay and ferric ions as the framework for pollutant-absorbing supramolecular hydrogels. Langmuir 29:1238–1244
Hou S, Ma PX (2015) Stimuli-responsive supramolecular hydrogels with high extensibility and fast self-healing via precoordinated mussel-inspired chemistry. Chem Mater 27:7627–7635
Choi YC, Choi JS, Junga YJ, Cho YW (2014) Human gelatin tissue-adhesive hydrogels prepared by enzyme-mediated biosynthesis of DOPA and Fe3+ ion crosslinking. J Mater Chem B 2:201–209
Guo Z, Ni K, Wei D, Ren Y (2015) Fe3+-induced oxidation and coordination crosslinking in catechol-chitosan hydrogels under acidic pH conditions. RSC Adv 5:37377–37384
Funding
This study was funded by NSFC (51203079), the Natural Science Foundation of Tianjin (14JCYBJC18100), and PCSIRT (IRT1257).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Gong, C., Lu, C., Li, B. et al. Dopamine-modified poly(amino acid): an efficient near-infrared photothermal therapeutic agent for cancer therapy. J Mater Sci 52, 955–967 (2017). https://doi.org/10.1007/s10853-016-0391-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10853-016-0391-9