Abstract
Purpose
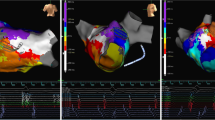
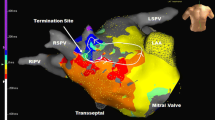
This study aims to describe a novel method of High Density Activation Sequence Mapping combined with Voltage Gradient Mapping Overlay (HD-VGM) to quickly localize and terminate atypical atrial flutter.
Methods
Twenty-one patients presenting with 26 different atypical atrial flutter circuits after a previous catheter or surgical AF ablation were studied. HD-VGM was performed with a commercially available impedance-based mapping system to locate and successfully ablate the critical isthmus of each tachycardia circuit. The results were compared to 21 consecutive historical control patients who had undergone an atypical flutter ablation without HD-VGM.
Results
Twenty-six different atypical flutter circuits were evaluated. An average 3D anatomic mapping time of 12.39 ± 4.71 min was needed to collect 2996 ± 690 total points and 1016 ± 172 used mapping points. A mean of 195 ± 75 s of radiofrequency (RF) energy was needed to terminate the arrhythmias. The mean procedure time was 135 ± 46 min. With a mean follow-up 16 ± 9 months, 90% are in normal rhythm. In comparison to the control cohort, the study cohort had a shorter procedure time (135 ± 46 vs. 210 ± 41 min, p = 0.0009), fluoroscopy time (8.5 ± 3.7 vs. 17.7 ± 7.7 min, p = 0.0021), and success in termination of the arrhythmia during the procedure (100 vs. 68.2%, p = 0.0230).
Conclusions
Ablation of atypical atrial flutter is challenging and time consuming. This case series shows that HD-VGM mapping can quickly localize and terminate an atypical flutter circuit.







Similar content being viewed by others
Abbreviations
- AF:
-
Atrial fibrillation
- PAF:
-
Paroxysmal atrial fibrillation
- pAF:
-
Persistent atrial fibrillation
- HD-VGM:
-
High Density Activation Sequence Mapping with Voltage Gradient Mapping Overlay
- aAFL:
-
Atypical atrial flutter
- LA:
-
Left atrium
- RA:
-
Right atrium
- CS:
-
Coronary Sinus
- LAT:
-
Local activation timing
- RAI:
-
Roving activation interval
- LVID:
-
Low-V ID
- ACT:
-
Activated clotting time
- ICE:
-
Intracardiac echo
- LSI:
-
Lesion size index
- FTI:
-
Force Time Integral
- RF:
-
Radiofrequency
- CAFÉ:
-
Complex atrial fractionated electrograms
References
Haissaguerre M, Jais P, Shah DC, Takahashi A, Hocini M, Quiniou G, et al. Spontaneous initiation of atrial fibrillation by ectopic beats originating in the pulmonary veins. NEJM. 1998;339:659–66.
Haissaguerre M, Shah DC, Jais P, Hocini M, Yamane T, Deisenhofer I, et al. Electrophysiological breakthroughs from the left atrium to the pulmonary veins. Circulation. 2000;102:2463–5.
Haissaguerre M, Jais P, Shah DC, Garrigue S, Takahashi A, Lavergne T, et al. Electrophysiological end point for catheter ablation of atrial fibrillation initiated from multiple pulmonary venous foci. Circulation. 2000;101:1409–17.
Papone C, Rosanio S, Oreto G, Tocchi M, Gugliotta F, et al. Circumferential radiofrequency ablation of pulmonary vein ostia: a new anatomic approach for curing atrial fibrillation. Circulation. 2000;102:2619–28.
Oral H, Scharf C, Chugh A, Hall B, Cheung P, et al. Catheter ablation for paroxysmal atrial fibrillation: segmental pulmonary vein ostial ablation versus left atrial ablation. Circulation. 2003;108:2355–60.
Haissaguerre M, Hocini M, Sanders P, Sacher P, Sacher F, et al. Catheter ablation of long-lasting persistent atrial fibrillation: clinical outcome and mechanisms of subsequent arrhythmias. J Cardiovasc Electrophysiol. 2005;16:1138–47.
Jais P, Sanders P, Hsu LF, Hocini M, Sacher F, Takahashi Y, et al. Flutter localized to the anterior left atrium after catheter ablation of atrial fibrillation. J Cardiovasc Electrophysiol. 2006;17:279–85.
Kobza R, Hindricks G, Tanner H, Schirdewahn P, Dorzewski A, et al. Late recurrent arrhythmias after ablation of atrial fibrillation: incidence, mechanisms and treatment. Heart Rhythm. 2004;1:676–83.
Gerstenfeld EP, Callans DJ, Dixit S, Russo AM, Nayak H, Lin D, et al. Mechanisms of organized left atrial tachycardias occurring after pulmonary vein isolation. Circulation. 2004;110:1351–7.
Deisenhofer I, Estner H, Zrenner B, Schreieck J, et al. Left atrial tachycardia after circumferential pulmonary vein ablation for atrial fibrillation: incidence, electrophysiological characteristic, and results of radiofrequency ablation. Europace. 2006;8:573–82.
Veenhuysen GD, Knecht S, O’Neill Phil D, Wright M, Nault I, Weerasooriya R, et al. Atrial tachycardias encountered during and after catheter ablation for atrial fibrillation: part I: classification, incidence, management. Pacing Clin Electrophysiol. 2009;32:393–8.
Sawhney N, Anousheh R, Chen W, Feld GK. Circumferential pulmonary vein ablation with additional linear ablation results in an increased incidence of left atrial flutter compared with segmental pulmonary vein isolation as an initial approach to ablation of paroxysmal atrial fibrillation. Circa Arrhythmia Electrophysiol. 2010;3:243–8.
Chugh A, Oral H, Lemola K, Hall B, Cheung P, et al. Prevalence, mechanisms, and clinical significance of macroreentrant atrial tachycardia during and following left atrial ablation for atrial fibrillation. Heart Rhythm. 2005;2:464–71.
Wazni OM, Saliba W, Fahmy T, Lakkireddy D, Thal S, et al. Atrial arrhythmias after surgical maze: findings during catheter ablation. J Am Coll Cardiol. 2006;48:1405–9.
Weerasooriya R, Jais P, Wright M, Matsuo KS, et al. Catheter ablation of atrial tachycardia following atrial fibrillation ablation. J Cardiovasc Electrophysiol. 2009;20:833–8.
Eitel C, Hindricks G, Dagres N, Sommer P, Piorkowski C. Ensite Velocity cardiac mapping system: a new platform for 3D mapping of cardiac arrhythmias. Expert Rev Med Devices. 2010;7(2):185–92.
Ballin SJ, Korthas MA, Weers NJ, Hoffman CJ. Direct visualization of the slow pathway using voltage gradient mapping: a novel approach for successful ablation of atrioventricular nodal reentry tachycardia. Europace. 2011;13(8):1188–94.
January CT, Wann LS, Alpert JS, Calkins H, Cigarroa JE, Cleveland JC Jr, Conti JB, Ellinor PT, Ezekowitz MD, Field ME, Murray KT, Sacco RL, Stevenson WG, Tchou PJ, Tracy CM, Yancy CW. AHA/ACC/HRS guideline for the management of patients with atrial fibrillation: executive summary: a report of the American College of Cardiology/American Heart Association Task Force on practice guidelines and the Heart Rhythm Society Circulation. 2014;130(23):2071–104.
Coffey JO, d’Avila A, Dukkipati S, Danik SB, Gangireddy SR, et al. Catheter ablation of scar-related atypical atrial flutter. Europace. 2013;15:414–9.
Patel AM, d’Avila A, Neuzil P, Kim SJ, Mela T, et al. Atrial tachycardia after ablation of persistent atrial fibrillation: identification of the critical isthmus with a combination of multielectrode activation mapping and targeted entrainment mapping. Circ Arrhythmia Electrophysiol. 2008;1:14–22.
Casella M, Perna F, Russo AD, Pelargonio G, et al. Right ventricular substrate mapping using the Ensite Navx system: accuracy of high-density voltage map obtained by automatic point acquisition during geometry reconstruction. Heart Rhythm. 2006:1598–605.
Winkle RA, Moskovitz R, Mead RH, Engel G, Kong MH, Fleming W, Patrawala RA. Ablation of atypical atrial flutter using ultra high density-activation sequence mapping. J Interv Card Electrophysiol. 2017;48(2):177–184.
Jais P, Matsuo S, Knecht S, Weerasooriya R, Hocini M, et al. A deductive mapping strategy for atrial tachycardia following atrial fibrillation ablation: importance of localized reentry. J Cardiovasc Electrophysiol. 2009;20:480–91.
Acknowledgments
The authors thank Ms. Kim Oaks for the editorial assistance and Ms. Manya Harsch for the statistical assistance.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
This study was approved by our local institutional review board.
Conflict of interest
Drs. Sundaram and Choe are on the speaker’s bureau for St. Jude Medical. In addition, Drs. Sundaram and Choe have received a research grant from St. Jude Medical, Asia Division, to study the genetic basis of Brugada Syndrome in Cambodia. This conflict is not relevant to the article. N. Mullins and C. Boorman receive salary support from St. Jude Medical.
Rights and permissions
About this article
Cite this article
Sundaram, S., Choe, W., Ryan Jordan, J. et al. Catheter ablation of atypical atrial flutter: a novel 3D anatomic mapping approach to quickly localize and terminate atypical atrial flutter. J Interv Card Electrophysiol 49, 307–318 (2017). https://doi.org/10.1007/s10840-017-0269-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-017-0269-z