Abstract
Purpose
The purpose of this study is to investigate whether individual response of anti-Mullerian hormone (AMH) to gonadotropin-releasing hormone (GnRH) treatment is associated with difference in ovarian stimulation outcomes.
Methods
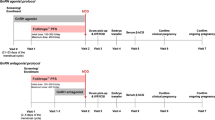
The retrospective study included 1058 non-polycystic ovary syndrome (PCOS) women undergoing long agonist protocol in a single in vitro fertilization unit from January 1, 2016, through December 31, 2016. Patients were grouped according to AMH changes from day 3 to the day of stimulation (group 1, change < 1 ng/ml, n = 714; group 2, decrease ≥ 1 ng/ml, n = 143; group 3, increase ≥ 1 ng/ml, n = 201). A generalized linear model including Poisson distribution and log link function was used to evaluate the association between AMH response and the number of oocytes retrieved.
Results
Group 2 was characterized by higher basal AMH level and increased AMH to AFC ratio in comparison with two other groups. However, the number of oocytes and ovarian sensitivity index in group 2 was significantly lower than group 3. Adjusted for age, BMI, ovarian reserve markers, and stimulation parameters, the population marginal means (95% confidence interval) of oocyte number in groups 1 through 3 were 9.51 (9.17, 9.86), 8.04 (7.54, 8.58), and 10.65 (10.15, 11.18), respectively. For patients from group 2 and group 3, basal AMH is no longer significantly associated with oocyte yield.
Conclusions
AMH change in response to GnRH agonist varies among individuals; for those undergoing significant changes in AMH following GnRH agonist treatment, basal AMH may not be a reliable marker for ovarian response in long agonist protocol.

Similar content being viewed by others
References
Iliodromiti S, Anderson RA, Nelson SM. Technical and performance characteristics of anti-Mullerian hormone and antral follicle count as biomarkers of ovarian response. Hum Reprod Update. 2015;21(6):698–710. https://doi.org/10.1093/humupd/dmu062.
La Marca A, Sunkara SK. Individualization of controlled ovarian stimulation in IVF using ovarian reserve markers: from theory to practice. Hum Reprod Update. 2014;20(1):124–40. https://doi.org/10.1093/humupd/dmt037.
Broer SL, Broekmans FJM, Laven JSE, Fauser BCJM. Anti-Mullerian hormone: ovarian reserve testing and its potential clinical implications. Hum Reprod Update. 2014;20(5):688–701. https://doi.org/10.1093/humupd/dmu020.
Jayaprakasan K, Campbell BK, Hopkisson JF, Clewes JS, Johnson IR, Raine-Fenning NJ. Effect of pituitary desensitization on the early growing follicular cohort estimated using anti-Mullerian hormone. Hum Reprod. 2008;23(11):2577–83. https://doi.org/10.1093/humrep/den282.
Su HI, Maas K, Sluss PM, Chang RJ, Hall JE, Joffe H. The impact of depot GnRH agonist on AMH levels in healthy reproductive-aged women. J Clin Endocr Metab. 2013;98(12):E1961–E6. https://doi.org/10.1210/jc.2013-2410.
Fauser BCJM, Chang J, Azziz R, Legro R, Dewailly D, Franks S, et al. Revised 2003 consensus on diagnostic criteria and long-term health risks related to polycystic ovary syndrome (PCOS). Hum Reprod. 2004;19(1):41–7. https://doi.org/10.1093/humrep/deh098.
Ren JZ, Sha AG, Han DM, Li P, Geng J, Ma CH. Does prolonged pituitary down-regulation with gonadotropin-releasing hormone agonist improve the live-birth rate in in vitro fertilization treatment? Fertil Steril. 2014;102(1):75–81. https://doi.org/10.1016/j.fertnstert.2014.03.030.
Martin-Johnston M, Beltsos AN, Grotjan HE, Uhler ML. Adding human menopausal gonadotrophin to antagonist protocols - is there a benefit? Reprod Biomed Online. 2007;15(2):161-168
Madani T, Yeganeh LM, Ezabadi Z,Hasani F, Chehrazi M. Comparing the efficacy of urinary and recombinant hCG on oocyte/follicle ratio to trigger ovulation in women undergoing intracytoplasmic sperm injection cycles: a randomized controlled trial. J Assist Reprod Gen. 2012;30(2):239-245
D'Arpe S, Di Feliciantonio M, Candelieri M, Franceschetti S, Piccioni MG, Bastianelli C. Ovarian function during hormonal contraception assessed by endocrine and sonographic markers: a systematic review. Reprod BioMed Online. 2016;33(4):436–48. https://doi.org/10.1016/j.rbmo.2016.07.010.
Huang JL, Wang XY, Li ZL, Ma RW, Xiao WF. Effects of GnRH agonists on the expression of developmental follicular anti-Mullerian hormone in varying follicular stages in cyclic mice in vivo. Mol Med Rep. 2015;12(3):4305–13. https://doi.org/10.3892/mmr.2015.3993.
Singh P, Krishna A. Effects of GnRH agonist treatment on steroidogenesis and folliculogenesis in the ovary of cyclic mice. J Ovarian Res. 2010;3:26. https://doi.org/10.1186/1757–2215–3-26.
Hagen CP, Sorensen K, Anderson RA, Juul A. Serum levels of antimullerian hormone in early maturing girls before, during, and after suppression with GnRH agonist. Fertil Steril. 2012;98(5):1326–30. https://doi.org/10.1016/j.fertnstert.2012.07.1118.
Bhide P, Dilgil M, Gudi A, Shah A, Akwaa C, Homburg R. Each small antral follicle in ovaries of women with polycystic ovary syndrome produces more antimullerian hormone than its counterpart in a normal ovary: an observational cross-sectional study. Fertil Steril. 2015;103(2):537–41. https://doi.org/10.1016/j.fertnstert.2014.10.033.
Alebic MS, Stojanovic N, Duhamel A, Dewailly D. The phenotypic diversity in per-follicle anti-Mullerian hormone production in polycystic ovary syndrome. Hum Reprod. 2015;30(8):1927–33. https://doi.org/10.1093/humrep/dev131.
Nardo LG, Yates AP, Roberts SA, Pemberton P, Laing I. The relationships between AMH, androgens, insulin resistance and basal ovarian follicular status in non-obese subfertile women with and without polycystic ovary syndrome. Hum Reprod. 2009;24(11):2917–23. https://doi.org/10.1093/humrep/dep225.
Dewailly D, Robin G, Peigne M, Decanter C, Pigny P, Catteau-Jonard S. Interactions between androgens, FSH, anti-Mullerian hormone and estradiol during folliculogenesis in the human normal and polycystic ovary. Hum Reprod Update. 2016;22(6):709–24. https://doi.org/10.1093/humupd/dmw027.
Pierre A, Peigne M, Grynberg M, Arouche N, Taieb J, Hesters L, et al. Loss of LH-induced down-regulation of anti-Mullerian hormone receptor expression may contribute to anovulation in women with polycystic ovary syndrome. Hum Reprod. 2013;28(3):762–9. https://doi.org/10.1093/humrep/des460.
Cimino I, Casoni F, Liu XH, Messina A, Parkash J, Jamin SP, et al. Novel role for anti-Mullerian hormone in the regulation of GnRH neuron excitability and hormone secretion. Nat Commun. 2016;7:10055. https://doi.org/10.1038/ncomms10055.
Cui LL, Qin YY, Gao X, Lu J, Geng L, Ding LL, et al. Antimullerian hormone: correlation with age and androgenic and metabolic factors in women from birth to postmenopause. Fertil Steril. 2016;105(2):481. https://doi.org/10.1016/j.fertnstert.2015.10.017.
Ashrafi M, Hemat M, Arabipoor A, Salman Yazdi R, Bahman-Abadi A, Cheraghi R. Predictive values of anti-Mullerian hormone, antral follicle count and ovarian response prediction index (ORPI) for assisted reproductive technology outcomes. Journal of Obstetrics and Gynaecology : the Journal of the Institute of Obstetrics and Gynaecology. 2017;37(1):82–8. https://doi.org/10.1080/01443615.2016.1225025.
Kunicki M, Lukaszuk K, Jakiel G, Liss J. Serum dehydroepiandrosterone sulphate concentration is not a predictive factor in IVF outcomes before the first cycle of GnRH agonist administration in women with normal ovarian reserve. PLoS One. 2015;10(3):e0118570. https://doi.org/10.1371/journal.pone.0118570.
Knez J, Kovacic B, Medved M, Vlaisavljevic V. What is the value of anti-Mullerian hormone in predicting the response to ovarian stimulation with GnRH agonist and antagonist protocols? Reproductive Biology and Endocrinology: RB&E. 2015;13:58. https://doi.org/10.1186/s12958-015-0049-5.
Heidar Z, Bakhtiyari M, Mirzamoradi M, Zadehmodarres S, Sarfjoo FS, Mansournia MA. Prediction of different ovarian responses using anti-Mullerian hormone following a long agonist treatment protocol for IVF. J Endocrinol Investig. 2015;38(9):1007–15. https://doi.org/10.1007/s40618-015-0297-4.
Aydin T, Kara M, Aran T, Turktekin N, Ozdemir B. The association between anti-Mullerian hormone and IVF-ICSI outcome in poor responder patients performing long protocol. Clinical and Experimental Obstetrics & Gynecology. 2015;42(5):663–5.
Anckaert E, Smitz J, Schiettecatte J, Klein BM, Arce JC. The value of anti-Mullerian hormone measurement in the long GnRH agonist protocol: association with ovarian response and gonadotrophin-dose adjustments. Hum Reprod. 2012;27(6):1829–39. https://doi.org/10.1093/humrep/des101.
McLennan IS, Pankhurst MW. Is the understanding of AMH being confounded by study designs that do not adequately reflect that it is an atypical hormone? Hum Reprod. 2017;32(1):14–7. https://doi.org/10.1093/humrep/dew305.
Acknowledgements
The authors would like to thank all the staff, nurses, and physicians at the Reproductive Medicine Center for their support in generating this manuscript. This work was supported by the National Natural Science Foundation of China [grant number 81302454], the Science and Technology Project funding in Xiamen City [grant number 3502Z20144039], and the Natural Science Foundation of Fujian Province [grant numbers 2016D025 and 2015D016].
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Cai, J., Liu, L., Zheng, J. et al. Differential response of AMH to GnRH agonist among individuals: the effect on ovarian stimulation outcomes. J Assist Reprod Genet 35, 467–473 (2018). https://doi.org/10.1007/s10815-017-1095-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-017-1095-z