Abstract
Purpose
To evaluate the refractive outcomes of scleral-sutured IOL 2 mm posterior to the limbus in post-traumatic eyes using SRK/T formula.
Methods
This single-center retrospective case series included 35 eyes from 35 post-traumatic patients undergoing scleral-suture of ErgomaX IOLs by a single experienced surgeon. Preoperative predicted refraction, procedure-related complications, and postoperative spherical equivalent (SE) at least 1 month after surgery were recorded. The prediction error (PE) was calculated as the difference between the postoperative SE and preoperative predicted refraction.
Results
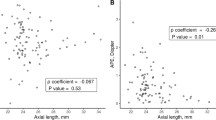
Of the 35 post-traumatic patients, 28 patients were aphakia without capsular support, and 7 patients were traumatic lens dislocation or subluxation. The mean age at surgery was 56.03 ± 14.56 years and 28 patients were men (80%). The mean postoperative spherical equivalent (SE) and postoperative astigmatism were − 1.23 ± 0.82 D and 1.57 ± 1.14 D, respectively. The mean prediction error (ME) of SRK/T formula was − 0.17 D. The mean absolute error (MAE) was 0.48D. The prediction accuracy was 60.0% for refractive errors of ± 0.50 D and 85.7% for refractive errors of ± 1.00D. Multiple linear regression analyses revealed that IOL power has positive correlation with PE.
Conclusion
Assumption of in-the-bag IOL position when calculating IOL (52501TY, ErgomaX) power for standardizing scleral-sutured IOL 2 mm posterior to the limbus demonstrates acceptable refractive outcomes. The accuracy of IOL power calculation using the SRK/T formula for eyes needing low IOL power or high IOL power may be affected by the uncertain position of postoperative IOL and further studies are needed.


Similar content being viewed by others
References
Khatry SK, Lewis AE, Schein OD, Thapa MD, Pradhan EK, Katz J (2004) The epidemiology of ocular trauma in rural Nepal. Br J Ophthalmol 88(4):456–460. https://doi.org/10.1136/bjo.2003.030700
Wittenborn JS, Zhang X, Feagan CW, Crouse WL, Shrestha S, Kemper AR, Hoerger TJ, Saaddine JB (2013) The economic burden of vision loss and eye disorders among the United States population younger than 40 years. Ophthalmology 120(9):1728–1735. https://doi.org/10.1016/j.ophtha.2013.01.068
Shah MA, Shah SM, Shah SB, Patel CG, Patel UA, Appleware A, Gupta A (2011) Comparative study of final visual outcome between open- and closed-globe injuries following surgical treatment of traumatic cataract. Graefes Arch Clin Exp Ophthalmol 249(12):1775–1781. https://doi.org/10.1007/s00417-011-1732-7
Kuhn F, Mester V (2002) Anterior chamber abnormalities and cataract. Ophthalmol Clin North Am 15(2):195–203. https://doi.org/10.1016/s0896-1549(02)00010-x
Tabatabaei SA, Soleimani M, Etesali H, Naderan M (2020) Accuracy of swept-source optical coherence tomography and ultrasound biomicroscopy for evaluation of posterior lens capsule in traumatic cataract. Am J Ophthalmol 216:55–58. https://doi.org/10.1016/j.ajo.2020.03.030
Tabatabaei A, Kiarudi MY, Ghassemi F, Moghimi S, Mansouri M, Mirshahi A, Kheirkhah A (2012) Evaluation of posterior lens capsule by 20-MHz ultrasound probe in traumatic cataract. Am J Ophthalmol 153(1):51–54. https://doi.org/10.1016/j.ajo.2011.05.038
Bausili Portabella MM, Nadal J, Alvarez de Toledo J, Fideliz de la Paz M, Barraquer RI (2020) Long-term outcome of scleral-sutured posterior chamber intraocular lens: a case series. Br J Ophthalmol 104(5):712–717. https://doi.org/10.1136/bjophthalmol-2019-314054
Su D, Stephens JD, Obeid A, Borkar D, Storey PP, Khan MA, Hsu J, Garg SJ, Gupta O (2019) Refractive outcomes after pars plana vitrectomy and scleral fixated intraocular lens with gore-tex suture. Ophthalmol Retina 3(7):548–552. https://doi.org/10.1016/j.oret.2019.02.012
Szurman P, Petermeier K, Aisenbrey S, Spitzer MS, Jaissle GB (2010) Z-suture: a new knotless technique for transscleral suture fixation of intraocular implants. Br J Ophthalmol 94(2):167–169. https://doi.org/10.1136/bjo.2009.162180
Hu XT, Zhang ZD, Zhou R, Pan QT (2013) Cauterization technique for suture erosion in transscleral fixation of intraocular lenses. Int J Ophthalmol 6(6):892–894. https://doi.org/10.3980/j.issn.2222-3959.2013.06.27
Khan MA, Samara WA, Gerstenblith AT, Chiang A, Mehta S, Garg SJ, Hsu J, Gupta OP (2018) Combined pars plana vitrectomy and scleral fixation of an intraocular lens using gore-tex suture: one-year outcomes. Retina 38(7):1377–1384. https://doi.org/10.1097/iae.0000000000001692
Abbey AM, Hussain RM, Shah AR, Faia LJ, Wolfe JD, Williams GA (2015) Sutureless scleral fixation of intraocular lenses: outcomes of two approaches. The 2014 Yasuo Tano Memorial Lecture. Graefes Arch Clin Exp Ophthalmol 253(1):1–5. https://doi.org/10.1007/s00417-014-2834-9
Lee R, Govindaraju V, Farley ND, Abbey AM, Stem MS, Shields RA, Wa CA, Williams GA, Faia LJ, Hassan TS, Wolfe JD (2021) Refractive outcomes after sutureless intrascleral fixation of intraocular lens with pars plana vitrectomy. Retina 41(4):822–826. https://doi.org/10.1097/iae.0000000000002916
Kane JX, Chang DF (2021) Intraocular lens power formulas, biometry, and intraoperative aberrometry: a review. Ophthalmology 128(11):e94–e114. https://doi.org/10.1016/j.ophtha.2020.08.010
Retzlaff JA, Sanders DR, Kraff MC (1990) Development of the SRK/T intraocular lens implant power calculation formula. J Cataract Refract Surg 16(3):333–340. https://doi.org/10.1016/s0886-3350(13)80705-5
Botsford BW, Williams AM, Conner IP, Martel JN, Eller AW (2019) Scleral fixation of intraocular lenses with gore-tex suture: refractive outcomes and comparison of lens power formulas. Ophthalmol Retina 3(6):468–472. https://doi.org/10.1016/j.oret.2019.02.005
Ohr MP, Wisely CE (2020) Refractive outcomes and accuracy of IOL power calculation with the SRK/T formula for sutured, scleral-fixated Akreos AO60 intraocular lenses. Graefes Arch Clin Exp Ophthalmol 258(10):2125–2129. https://doi.org/10.1007/s00417-020-04721-9
Li Z, Lian Z, Young CA, Zhao J, Jin G, Zheng D (2021) Accuracy of intraocular lens calculation formulas for eyes with insufficient capsular support. Ann Transl Med 9(4):324. https://doi.org/10.21037/atm-20-3290
Gao S, Qin T, Wang S, Lu Y (2015) Sulcus fixation of foldable intraocular lenses guided by ultrasound biomicroscopy. J Ophthalmol 2015:520418. https://doi.org/10.1155/2015/520418
Erickson P (1990) Effects of intraocular lens position errors on postoperative refractive error. J Cataract Refract Surg 16(3):305–311. https://doi.org/10.1016/s0886-3350(13)80699-2
Melles RB, Holladay JT, Chang WJ (2018) Accuracy of intraocular lens calculation formulas. Ophthalmology 125(2):169–178. https://doi.org/10.1016/j.ophtha.2017.08.027
Norrby S, Bergman R, Hirnschall N, Nishi Y, Findl O (2017) Prediction of the true IOL position. Br J Ophthalmol 101(10):1440–1446. https://doi.org/10.1136/bjophthalmol-2016-309543
Muzyka-Wozniak M, Ogar A (2016) Anterior chamber depth and iris and lens position before and after phacoemulsification in eyes with a short or long axial length. J Cataract Refract Surg 42(4):563–568. https://doi.org/10.1016/j.jcrs.2015.12.050
Olsen T (2007) Calculation of intraocular lens power: a review. Acta Ophthalmol Scand 85(5):472–485. https://doi.org/10.1111/j.1600-0420.2007.00879.x
Hoffer KJ, Savini G (2021) Update on intraocular lens power calculation study protocols: the better way to design and report clinical trials. Ophthalmology 128(11):e115–e120. https://doi.org/10.1016/j.ophtha.2020.07.005
Acknowledgements
Not applicable.
Funding
This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Wenlong Wei declares that he has no conflict of interest. Haishuang Lin declares that she has no conflict of interest. Xuanli Zheng declares that she has no conflict of interest. Siyi Wang declares that he has no conflict of interest. Shengsheng Bai declares that he has no conflict of interest. Zhenquan Zhao declares that he has no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wei, W., Lin, H., Zheng, X. et al. Refractive outcomes of scleral-sutured posterior chamber intraocular lenses in post-traumatic eyes. Int Ophthalmol 43, 423–429 (2023). https://doi.org/10.1007/s10792-022-02439-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-022-02439-7