Abstract
Purpose
To analyze the 100 most cited articles pertaining to endophthalmitis using bibliometric analysis.
Methods
An all-time Web of Science literature search and refined to peer-reviewed articles in the field of ophthalmology with the keyword “endophthalmitis” was completed. Total citation count of articles published pertaining to endophthalmitis, topic, incidence rate, publishing journals, year published, language, country of origin, number of authors, names of the first and last authors, study type, and number of patients/eyes studied.
Results
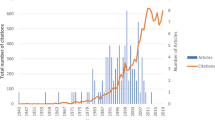
The top 100 most cited articles pertaining to endophthalmitis had a mean citation count of 362.92, with a range of 175 to 3583. They were published in 20 peer-reviewed journals, with Ophthalmology publishing the most (n = 42). Thirteen different countries were represented, with the majority (n = 77) originating from the USA. The most common study type was clinical experiences (n = 52), though eight of the top ten were clinical trials. The number of patients varied widely, represented by a mean of 9680, but with a median of only 229. The majority (n = 67) examined the incidence of endophthalmitis which included 24 articles after anti-vascular endothelial growth factor injections, 18 after ocular surgeries/procedures, 15 after intraocular steroid injections, eight after chemotoxic drug use, and three after ocular injuries.
Conclusion
This bibliographic study serves as a unique historical analysis of the top 100 cited scholarly articles pertaining to endophthalmitis with many of the articles related to post-procedural endophthalmitis.




Similar content being viewed by others
References
Durand ML (2013) Endophthalmitis. Clin Microbiol Infect 19:227–234
Taban M, Behrens A, Newcomb RL et al (2005) Acute endophthalmitis following cataract surgery: a systematic review of the literature. Arch Ophthalmol 123(5):613–620. https://doi.org/10.1001/archopht.123.5.613
Okada AA, Johnson RP, Liles WC, D’Amico DJ, Baker AS (1994) Endogenous bacterial endophthalmitis. Report of a ten-year retrospective study. Ophthalmol 101(5):832–838
Seal D, Reischl U, Behr A et al (2008) Laboratory diagnosis of endophthalmitis: comparison of microbiology and molecular methods in the European Society of Cataract & Refractive Surgeons multicenter study and susceptibility testing. J Cataract Refract Surg 34(9):1439–1450
Endophthalmitis Vitrectomy Study Group (1995) Results of the Endophthalmitis Vitrectomy Study. A randomized trial of immediate vitrectomy and of intravenous antibiotics for the treatment of postoperative bacterial endophthalmitis. Arch Ophthalmol 113(12):1479–1496
Weakley AL (1916) Metastatic endophthalmitis in a case of cerebro-spinal meningitis. Br Med J 1(2871):47–48. https://doi.org/10.1136/bmj.1.2871.47-a
Sacks D, Baxter B et al (2018) Multisociety consensus quality improvement revised consensus statement for endovascular therapy of acute ischemic stroke. Int J Stroke 13(6):612–632. https://doi.org/10.1177/1747493018778713
Simunovic MP, Rush RB, Hunyor AP, Chang AA (2012) Endophthalmitis following intravitreal injection versus endophthalmitis following cataract surgery: clinical features, causative organisms and post-treatment outcomes. Br J Ophthalmol 96:862–866
Rosenfeld PJ, Brown DM, Heier JS et al (2006) Ranibizumab for neovascular age-related macular degeneration. N Engl J Med 355(14):1419–1431. https://doi.org/10.1056/NEJMoa054481
Brown DM, Kaiser PK, Michels M et al (2006) Ranibizumab versus verteporfin for neovascular age-related macular degeneration. N Engl J Med 355(14):1432–1444. https://doi.org/10.1056/nejmoa062655
Gragoudas ES, Adamis AP, Cunningham ET, Feinsod M, Guyer DR (2004) Pegaptanib for neovascular age-related macular degeneration. N Engl J Med 351(27):2805–2816. https://doi.org/10.1056/nejmoa042760
Brown DM, Michels M, Kaiser PK et al (2009) Ranibizumab versus verteporfin photodynamic therapy for neovascular age-related macular degeneration: two-year results of the ANCHOR study. Ophthalmology 116(1):57-65.e5. https://doi.org/10.1016/j.ophtha.2008.10.018
Elman MJ, Aiello LP, Beck RW et al (2010) Randomized trial evaluating ranibizumab plus prompt or deferred laser or triamcinolone plus prompt laser for diabetic macular edema. Ophthalmology 117(6):1064-1077.e35. https://doi.org/10.1016/j.ophtha.2010.02.031
Mitchell P, Bandello F, Schmidt-Erfurth U et al (2011) The RESTORE Study. Ophthalmology 118(4):615–625. https://doi.org/10.1016/j.ophtha.2011.01.031
Nguyen QD, Brown DM, Marcus DM et al (2012) Ranibizumab for diabetic macular edema: results from 2 phase III randomized trials: RISE and RIDE. Ophthalmology 119(4):789–801. https://doi.org/10.1016/j.ophtha.2011.12.039
Spaide RF, Laud K, Fine HF et al (2006) Intravitreal bevacizumab treatment of choroidal neovascularization secondary to age-related macular degeneration. Retina 26(4):383–390. https://doi.org/10.1097/01.iae.0000238561.99283.0e
List of top 20 outpatient surgeries. Definitive healthcare website. Accessed May 23, 2020. https://blog.definitivehc.com/list-of-top-20-outpatient-surgical-procedures
Ohba N, Nakao K, Isashiki Y, Ohba A (2007) The 100 most frequently cited articles in ophthalmology journals. Arch Ophthalmol 125(7):952–960
Krauthammer M, Moisseiev E (2020 Apr) The 100 most cited articles on vitrectomy: a bibliographic perspective. Ophthalmol Retina 4(4):361–368
Heng Wong MY, Tan NYQ, Sabanayagam C (2019 Jan) Time trends, disease patterns and gender imbalance in the top 100 most cited articles in ophthalmology. Br J Ophthalmol 103(1):18–25
Dossarps D, Bron AM, Koehrer P, Aho-Glélé LS, Creuzot-Garcher C (2015) Endophthalmitis after intravitreal injections: Incidence, presentation, management, and visual outcome. Am J Ophthalmol 160(1):17-25.e1. https://doi.org/10.1016/j.ajo.2015.04.013
Martidis A, Duker JS, Greenberg PB et al (2002) Intravitreal triamcinolone for refractory diabetic macular edema. Ophthalmology 109(5):920–927. https://doi.org/10.1016/s0161-6420(02)00975-2
McCannel CA (2011) Meta-analysis of endophthalmitis after intravitreal injection of anti-vascular endothelial growth factor agents: causative organisms and possible prevention strategies. Retina 31(4):654–661. https://doi.org/10.1097/IAE.0b013e31820a67e4
Jonas JB, Kreissig I, Söfker A, Degenring RF (2003) Intravitreal injection of triamcinolone for diffuse diabetic macular edema. Arch Ophthalmol 121(1):57–61
Scott IU, Ip MS, VanVeldhuisen PC, et al. (2009) A randomized trial comparing the efficacy and safety of intravitreal triamcinolone with standard care to treat vision loss associated with macular Edema secondary to branch retinal vein occlusion: the Standard Care vs Corticosteroid for Retinal Vein Occlusion (SCORE) study report 6 [published correction appears in Arch Ophthalmol. 2009 Dec;127(12):1655]. Arch Ophthalmol 127(9):1115‐1128. https://doi.org/10.1001/archophthalmol.2009.233
Gillies MC, Sutter FK, Simpson JM, Larsson J, Ali H, Zhu M (2006) Intravitreal triamcinolone for refractory diabetic macular edema: two-year results of a double-masked, placebo-controlled, randomized clinical trial. Ophthalmology 113(9):1533–1538. https://doi.org/10.1016/j.ophtha.2006.02.065
Moshfeghi DM, Kaiser PK, Scott IU et al (2003) Acute endophthalmitis following intravitreal triamcinolone acetonide injection. Am J Ophthalmol 136(5):791–796. https://doi.org/10.1016/s0002-9394(03)00483-5
Kattan HM, Flynn HW Jr, Pflugfelder SC, Robertson C, Forster RK (1991) Nosocomial endophthalmitis survey. Current incidence of infection after intraocular surgery. Ophthalmology 98(2):227–238
Powe NR, Schein OD, Gieser SC, et al. (1994) Synthesis of the literature on visual acuity and complications following cataract extraction with intraocular lens implantation. Cataract Patient Outcome Research Team [published correction appears in Arch Ophthalmol 1994 Jul;112(7):889]. Arch Ophthalmol 112(2):239–252. https://doi.org/10.1001/archopht.1994.01090140115033
Jager RD, Aiello LP, Patel SC, Cunningham ET Jr (2004) Risks of intravitreous injection: a comprehensive review. Retina 24(5):676–698. https://doi.org/10.1097/00006982-200410000-00002
Aaberg TM Jr, Flynn HW Jr, Schiffman J, Newton J (1998) Nosocomial acute-onset postoperative endophthalmitis survey. A 10-year review of incidence and outcomes. Ophthalmology 105(6):1004–1010. https://doi.org/10.1016/S0161-6420(98)96000-6
Lundström M, Wejde G, Stenevi U, Thorburn W, Montan P (2007) Endophthalmitis after cataract surgery: a nationwide prospective study evaluating incidence in relation to incision type and location. Ophthalmology 114(5):866–870. https://doi.org/10.1016/j.ophtha.2006.11.025
Pershing S, Lum F, Hsu S et al (2020) Endophthalmitis after cataract surgery in the united states: a report from the intelligent research in sight registry, 2013–2017. Ophthalmol 127(2):151–158. https://doi.org/10.1016/j.ophtha.2019.08.026
Ciulla TA, Starr MB, Masket S (2002) Bacterial endophthalmitis prophylaxis for cataract surgery: an evidence-based update. Ophthalmology 109(1):13–24. https://doi.org/10.1016/s0161-6420(01)00899-5
Speaker MG, Menikoff JA (1991) Prophylaxis of endophthalmitis with topical povidone-iodine. Ophthalmology 98(12):1769–1775. https://doi.org/10.1016/s0161-6420(91)32052-9
Endophthalmitis Study Group, European Society of Cataract & Refractive Surgeons (2007) Prophylaxis of postoperative endophthalmitis following cataract surgery: results of the ESCRS multicenter study and identification of risk factors. J Cataract Refract Surg 33(6):978–988. https://doi.org/10.1016/j.jcrs.2007.02.032
Doshi RR, Leng T, Fung AE (2012) Reducing oral flora contamination of intravitreal injections with face mask or silence. Retina 32(3):473–476. https://doi.org/10.1097/IAE.0B013E31822C2958
Kresloff MS, Castellarin AA, Zarbin MA (1998) Endophthalmitis. Surv Ophthalmol 43(3):193–224. https://doi.org/10.1016/s0039-6257(98)00036-8
Barry P, Seal DV, Gettinby G, et al. (2006) ESCRS study of prophylaxis of postoperative endophthalmitis after cataract surgery: preliminary report of principal results from a European multicenter study [published correction appears in J Cataract Refract Surg. 2006 May;32(5):709]. J Cataract Refract Surg 32(3):407–410. https://doi.org/10.1016/j.jcrs.2006.02.021
Fang CT, Lai SY, Yi WC, Hsueh PR, Liu KL, Chang SC (2007) Klebsiella pneumoniae genotypeK1: an emerging pathogen that causes septic ocular or central nervous system complications from pyogenic liver abscess. Clin Infect Dis 45(3):284–293. https://doi.org/10.1086/519262
Han DP, Wisniewski SR, Wilson LA et al (1996) Spectrum and susceptibilities of microbiologicisolates in the Endophthalmitis Vitrectomy Study [published correction appears in Am JOphthalmol 1996 Dec; 122(6):920. Am J Ophthalmol 122(1):1–17. https://doi.org/10.1016/s0002-9394(14)71959-2
Speaker MG, Milch FA, Shah MK, Eisner W, Kreiswirth BN (1991) Role of external bacterial flora in the pathogenesis of acute postoperative endophthalmitis. Ophthalmology 98(5):639–650. https://doi.org/10.1016/s0161-6420(91)32239-5
Jackson TL, Eykyn SJ, Graham EM, Stanford MR (2003) Endogenous bacterial endophthalmitis: a 17-year prospective series and review of 267 reported cases. Surv Ophthalmol 48(4):403–423. https://doi.org/10.1016/s0039-6257(03)00054-7
Wong JS, Chan TK, Lee HM, Chee SP (2000) Endogenous bacterial endophthalmitis: an East Asian experience and a reappraisal of a severe ocular affliction. Ophthalmology 107(8):1483–1491. https://doi.org/10.1016/s0161-6420(00)00216-5
Martín-Martín A, Thelwall M, Orduna-Malea E, Delgado L-Cózar E (2020 Sep) Google Scholar, Microsoft Academic, Scopus, Dimensions, Web of Science, and OpenCitations’ COCI: a multidisciplinary comparison of coverage via citations. Scientometrics 21:1–3
Kulkarni AV, Aziz B, Shams I, Busse JW (2009 Sep 9) Comparisons of citations in Web of Science, Scopus, and Google Scholar for articles published in general medical journals. JAMA 302(10):1092–1096
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
No conflicting relationship exists for any author.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Disclaimer: The view(s) expressed herein are those of the author(s) and do not reflect the official policy or position of the Madigan Army Medical Center, the San Antonio Military Medical Center, the Walter Reed Military Medical Center, the U.S. Army Medical Department, the U.S. Army Office of the Surgeon General, the Department of the Air Force, the Department of the Army, Department of Defense, the Defense Health Agency, or any other agency of the U.S. Government.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Wade, C.I., Whitescarver, T.D., Ashcroft, C.R. et al. Endophthalmitis: a bibliographic review. Int Ophthalmol 41, 4151–4161 (2021). https://doi.org/10.1007/s10792-021-01967-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-021-01967-y