Abstract
Purpose
The aim of the study was to examine the outcomes of transepithelial photorefractive keratectomy (Trans-PRK) and Femtosecond Laser-assisted in situ keratomileusis (Z-LASIK) for the correction of high myopia.
Methods
A retrospective cohort study design was used. The study group included 792 eyes with high-grade myopia (− 6.0 diopters or higher) or high-grade myopia with astigmatism that were treated with Z-LASIK or Trans-PRK in 2013 through 2014 in an optical outpatient clinic of a large private medical service. The Trans-PRK group comprised of 674 eyes with a spherical equivalent (SE) of − 7.87 ± 1.46 and the Z-LASIK group comprised of 118 eyes with a SE of − 7.19 ± 0.81 (P < 0.001).
Results
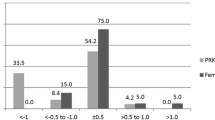
The mean postoperative SE in the Trans-PRK group was − 0.06 and − 0.02 in the Z-LASIK group (P = 0.545). Efficacy index values were 0.92 in the Trans-PRK group and 0.95 in the Z-LASIK group (P = 0.083), and corresponding safety index values were 0.95 and 0.97 (P = 0.056). An UCVA of 20/40 or better was achieved in 94.20% of eyes in the Trans-PRK group, and 98.31% in the Z-LASIK group (P = 0.063). The majority of eyes in both the Trans-PRK and Z-LASIK groups were within ± 0.5D of attempted correction: 59.35 and 64.71%, respectively (P = 0.271).
Conclusions
Both Trans-PRK and Z-LASIK demonstrated excellent efficacy, safety and predictability profiles, with results comparable and in some cases superior to the current literature. Results of Z-LASIK were slightly better than those of Trans-PRK, though the preoperative SE of the latter was higher.







Similar content being viewed by others


References
Hori-Komai Y, Toda I, Asano-Kato N, Tsubota K (2002) Reasons for not performing refractive surgery. J Cataract Refract Surg 28(5):795–797
Bamashmus M, Saleh MF, Abdulrahman M, Al-Kershy N (2010) Reasons for not performing LASIK in refractive surgery candidates in Yemen. Eur J Ophthalmol 20(5):858–864
Loewenstein A, Lipshitz I, Varssano D, Lazar M (1997) Complications of excimer laser photorefractive keratectomy for myopia. J Cataract Refract Surg 23(8):1174–1176
Alio JL, Artola A, Claramonte PJ, Ayala MJ, Sanchez SP (1998) Complications of photorefractive keratectomy for myopia: two year follow-up of 3000 cases. J Cataract Refract Surg 24(5):619–626
Luger MH, Ewering T, Arba-Mosquera S (2012) Consecutive myopia correction with transepithelial versus alcohol-assisted photorefractive keratectomy in contralateral eyes: one-year results. J Cataract Refract Surg 38(8):1414–1423. https://doi.org/10.1016/j.jcrs.2012.03.028
Fadlallah A, Fahed D, Khalil K, Dunia I, Menassa J, El Rami H, Chlela E, Fahed S (2011) Transepithelial photorefractive keratectomy: clinical results. J Cataract Refract Surg 37(10):1852–1857. https://doi.org/10.1016/j.jcrs.2011.04.029
Wang DM, Du Y, Chen GS, Tang LS, He JF (2012) Transepithelial photorefractive keratectomy mode using SCHWIND-ESIRIS excimer laser: initial clinical results. Int J Ophthalmol 5(3):334–337. https://doi.org/10.3980/j.issn.2222-3959.2012.03.16
Ambrosio R Jr, Wilson S (2003) LASIK vs LASEK vs PRK: advantages and indications. Semin Ophthalmol 18(1):2–10
Shortt AJ, Bunce C, Allan BD (2006) Evidence for superior efficacy and safety of LASIK over photorefractive keratectomy for correction of myopia. Ophthalmology 113(11):1897–1908. https://doi.org/10.1016/j.ophtha.2006.08.013
Melki SA, Azar DT (2001) LASIK complications: etiology, management, and prevention. Surv Ophthalmol 46(2):95–116
Schallhorn SC, Amesbury EC, Tanzer DJ (2006) Avoidance, recognition, and management of LASIK complications. Am J Ophthalmol 141(4):733–739. https://doi.org/10.1016/j.ajo.2005.11.036
Wang B, Naidu RK, Chu R, Dai J, Qu X, Zhou H (2015) Dry eye disease following refractive surgery: a 12-month follow-up of SMILE versus FS-LASIK in high myopia. J Ophthalmol 2015:132417. https://doi.org/10.1155/2015/132417
Meyer CH, Mennel S, Schmidt JC (2009) Acute keratoconus-like hydrops after laser in situ keratomileusis. J Ophthalmol 2009:363482. https://doi.org/10.1155/2009/363482
Wu W, Wang Y (2015) The correlation analysis between corneal biomechanical properties and the surgically induced corneal high-order aberrations after small incision lenticule extraction and femtosecond laser in situ keratomileusis. J Ophthalmol 2015:758196. https://doi.org/10.1155/2015/758196
Sutton G, Lawless M, Hodge C (2014) Laser in situ keratomileusis in 2012: a review. Clin Exp Optom 97(1):18–29. https://doi.org/10.1111/cxo.12075
Kymionis GD, Kounis GA, Grentzelos MA, Panagopoulou SI, Kandarakis SA, Krasia MS (2011) Interface corneal stromal irregularities after flap creation using femtosecond laser. Eur J Ophthalmol 21(2):207–209
Dada T, Pangtey MS, Sharma N, Vajpayee RB, Jhanji V, Sethi HS (2006) Hyeropic shift after LASIK induced diffuse lamellar keratitis. BMC Ophthalmol 6:19. https://doi.org/10.1186/1471-2415-6-19
Tatar MG, Aylin Kantarci F, Yildirim A, Uslu H, Colak HN, Goker H, Gurler B (2014) Risk factors in post-LASIK corneal ectasia. J Ophthalmol 2014:204191. https://doi.org/10.1155/2014/204191
Khoramnia R, Salgado JP, Lohmann CP, Kobuch KA, von Mohrenfels CW (2012) Precision, morphology, and histology of corneal flap cuts using a 200-kHz femtosecond laser. Eur J Ophthalmol 22(2):161–167. https://doi.org/10.5301/EJO.2011.8376
Vestergaard A, Ivarsen A, Asp S, Hjortdal JO (2013) Femtosecond (FS) laser vision correction procedure for moderate to high myopia: a prospective study of ReLEx((R)) flex and comparison with a retrospective study of FS-laser in situ keratomileusis. Acta Ophthalmol 91(4):355–362. https://doi.org/10.1111/j.1755-3768.2012.02406.x
Ang M, Mehta JS, Rosman M, Li L, Koh JC, Htoon HM, Tan D, Chan C (2013) Visual outcomes comparison of 2 femtosecond laser platforms for laser in situ keratomileusis. J Cataract Refract Surg 39(11):1647–1652. https://doi.org/10.1016/j.jcrs.2013.04.044
Tomita M, Watabe M, Yukawa S, Nakamura N, Nakamura T, Magnago T (2014) Safety, efficacy, and predictability of laser in situ keratomileusis to correct myopia or myopic astigmatism with a 750 Hz scanning-spot laser system. J Cataract Refract Surg 40(2):251–258. https://doi.org/10.1016/j.jcrs.2013.07.043
Kulkamthorn T, Silao JN, Torres LF, Lim JN, Purcell TL, Tantayakom T, Schanzlin DJ (2008) Wavefront-guided laser in situ keratomileusis in the treatment of high myopia by using the CustomVue wavefront platform. Cornea 27(7):787–790. https://doi.org/10.1097/ICO.0b013e31816a3554
Kojima T, Hallak JA, Azar DT (2008) Control-matched analysis of laser in situ keratomileusis outcomes in high myopia. J Cataract Refract Surg 34(4):544–550. https://doi.org/10.1016/j.jcrs.2007.11.031
Stonecipher KG, Kezirian GM, Stonecipher M (2010) LASIK for − 6.00 to − 12.00 D of myopia with up to 3.00 D of cylinder using the ALLEGRETTO WAVE: 3- and 6-month results with the 200- and 400-Hz platforms. J Refract Surg 26(10):S814–S818. https://doi.org/10.3928/1081597X-20100921-08
Alio JL, Vega-Estrada A, Pinero DP (2011) Laser-assisted in situ keratomileusis in high levels of myopia with the amaris excimer laser using optimized aspherical profiles. American journal of ophthalmology 152(6):954–963. https://doi.org/10.1016/j.ajo.2011.05.009
Hashmani N, Hashmani S, Ramesh P, Rajani H, Ahmed J, Kumar J, Kumar A, Jamali M (2017) A comparison of visual outcomes and patient satisfaction between photorefractive keratectomy and femtosecond laser-assisted in situ keratomileusis. Cureus 9(9):e1641. https://doi.org/10.7759/cureus.1641
Ghadhfan F, Al-Rajhi A, Wagoner MD (2007) Laser in situ keratomileusis versus surface ablation: visual outcomes and complications. J Cataract Refract Surg 33(12):2041–2048. https://doi.org/10.1016/j.jcrs.2007.07.026
Aslanides IM, Georgoudis PN, Selimis VD, Mukherjee AN (2015) Single-step transepithelial ASLA (SCHWIND) with mitomycin-C for the correction of high myopia: long term follow-up. Clin Ophthalmol 9:33–41. https://doi.org/10.2147/OPTH.S73424
Gazieva L, Beer MH, Nielsen K, Hjortdal J (2011) A retrospective comparison of efficacy and safety of 680 consecutive lasik treatments for high myopia performed with two generations of flying-spot excimer lasers. Acta Ophthalmol 89(8):729–733. https://doi.org/10.1111/j.1755-3768.2009.01830.x
Alio JL, Muftuoglu O, Ortiz D, Perez-Santonja JJ, Artola A, Ayala MJ, Garcia MJ, de Luna GC (2008) Ten-year follow-up of laser in situ keratomileusis for myopia of up to − 10 diopters. Am J Ophthalmol 145(1):46–54. https://doi.org/10.1016/j.ajo.2007.09.010
Chamon W, Alleman N (2008) Refractive surgery outcomes and frequency of complications in management of complications in refractive surgery. Springer, Berlin
Sekundo W, Bonicke K, Mattausch P, Wiegand W (2003) Six-year follow-up of laser in situ keratomileusis for moderate and extreme myopia using a first-generation excimer laser and microkeratome. J Cataract Refract Surg 29(6):1152–1158
Kymionis GD, Tsiklis NS, Astyrakakis N, Pallikaris AI, Panagopoulou SI, Pallikaris IG (2007) Eleven-year follow-up of laser in situ keratomileusis. J Cataract Refract Surg 33(2):191–196. https://doi.org/10.1016/j.jcrs.2006.11.002
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gershoni, A., Mimouni, M., Livny, E. et al. Z-LASIK and Trans-PRK for correction of high-grade myopia: safety, efficacy, predictability and clinical outcomes. Int Ophthalmol 39, 753–763 (2019). https://doi.org/10.1007/s10792-018-0868-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-018-0868-4