Abstract
Background
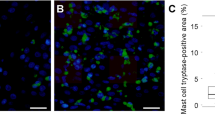
Eosinophilic esophagitis (EoE) is a chronic disease characterized histologically by > 15 eosinophils per high-power field (eos/hpf). Esophageal mucosal mast cells have been implicated in EoE pathogenesis. The association of atopy with EoE has been established but has not been correlated with levels of serum tryptase. The lack of concurrent atopy in some patients suggests the possibility that atopy may either be the related subtype of EoE or may be a sign of comorbidities. No study has looked at whether patients present with different phenotypes/comorbid disease when they have evidence of elevated serum tryptase. We hypothesized that these patients differ with respect to presentation and comorbidities with more refractory GI disease.
Aims
To examine whether elevations of serum tryptase associate with different, more severe clinical presentations in EoE patients which may be explained via mast cell activation.
Materials and Methods
Retrospective chart review identified 72 patients with EoE with results for serum tryptase between 2015 and 2016. Patients were classified as TryptaseHI (tryptase > 10.9 µg/l) and TryptaseLO (< 10.9 µg/l). Clinical characteristics and treatment response were compared using univariate analysis and multivariate regression between the groups.
Results
Out of 72 patients, 12 were tested as TryptaseHI (16.7%, 95% CI 8.1–25.3%). TryptaseHI was associated frequently with asthma (P = 0.0003), urticaria (P = 0.002), arthralgia (P = 0.005), sinusitis (P = 0.03), nausea/vomiting (P = 0.046), and eosinophilic gastrointestinal disease (P = 0.001). Asthma and arthralgia were found to be significantly associated with TryptaseHI (P = 0.0013, P = 0.0098, respectively). Mucosal eosinophil counts and tryptase levels were not correlated (R2 0.095, P = 0.77). Tryptase did not resolve with resolution of esophageal eosinophilia.
Conclusions
We found that EoE patients with elevated tryptase levels more commonly presented with asthma, urticaria, arthralgia, nausea/vomiting, sinusitis, and more distal eosinophilia. This indicates that atopy in EoE patients warrants further exploration. The lack of correlation between histologic remission and reduction of serum tryptase levels post-treatment suggests that mast cell activation may be an independent, yet associated disease. More study into this unique association is warranted.
Similar content being viewed by others
References
Furuta GT, Liacouras CA, Collins MH, et al. Eosinophilic esophagitis in children and adults: a systematic review and consensus recommendations for diagnosis and treatment. Gastroenterology. 2007;133:1342–1363.
Liacouras CA, Furuta GT, Hirano I, et al. Eosinophilic esophagitis: updated consensus recommendations for children and adults. J Allergy Clin Immunol. 2011;128:3–20.
Dellon ES, Gonsalves N, Hirano I, et al. ACG clinical guideline: evidenced based approach to diagnosis and management of esophageal eosinophilia and eosinophilic esophagitis (EoE). Am J Gastroenterol. 2013;108:679–692.
Zimmerman SL, Levine MS, Rubesin SE, et al. Idiopathic eosinophilic esophagitis in adults: the ringed esophagus. Radiology. 2005;236:159–165.
Straumann A, Spichtin HP, Grize L, et al. Natural history of primary eosinophilic esophagitis: a follow-up of 30 adult patients for up to 11.5 years. Gastroenterology. 2003;125:1660–1669.
Straumann A, Kristl J, Conus S, et al. Cytokine expression in healthy and inflamed mucosa: probing the role of eosinophils in the digestive tract. Inflamm Bowel Dis. 2005;11:720–726.
Aceves SS, Chen D, Newbury RO, et al. Mast cells infiltrate the esophageal smooth muscle in patients with eosinophilic esophagitis, express TGF-beta1, and increase esophageal smooth muscle contraction. J Allergy Clin Immunol. 2010;126:1198–1204. (e4).
Straumann A, Bauer M, Fischer B, Blaser K, Simon HU. Idiopathic eosinophilic esophagitis is associated with a T(H)2-type allergic inflammatory response. J Allergy Clin Immunol. 2001;108:954–961.
Chehade M, Sampson HA, Morotti RA, Magid MS. Esophageal subepithelial fibrosis in children with eosinophilic esophagitis. J Pediatr Gastroenterol Nutr. 2007;45:319–328.
Blanchard C, Wang N, Stringer KF, et al. Eotaxin-3 and a uniquely conserved gene-expression profile in eosinophilic esophagitis. J Clin Invest. 2006;116:536–547.
Abonia JP, Blanchard C, Butz BB, et al. Involvement of mast cells in eosinophilic esophagitis. J Allergy Clin Immunol. 2010;126:140–149.
Wang Y-H, Hogan SP, Fulkerson PC, Abonia JP, Rothenberg ME. Expanding the paradigm of eosinophilic esophagitis: mast cells and IL-9. J Allergy Clin Immunol. 2013;131:1583–1585. https://doi.org/10.1016/j.jaci.2013.04.010.
Schwartz LB, Metcalfe DD, Miller JS, Earl H, Sullivan T. Tryptase levels as an indicator of mast-cell activation in systemic anaphylaxis and mastocytosis. N Engl J Med. 1987;316:1622–1626.
Aceves SS, Newbury RO, Dohil R, et al. Esophageal remodeling in pediatric eosinophilic esophagitis. J Allergy Clin Immunol. 2007;119:206–212.
Kagalwalla AF, Akhtar N, Woodruff SA, et al. Eosinophilic esophagitis: epithelial mesenchymal transition contributes to esophageal remodeling and reverses with treatment. J Allergy Clin Immunol. 2012;129:1387–1396. (e7).
Lucendo AJ, Arias Á, De Rezende LC, et al. Subepithelial collagen deposition, profibrogenic cytokine gene expression, and changes after prolonged fluticasone propionate treatment in adult eosinophilic esophagitis: a prospective study. J Allergy Clin Immunol. 2011;128:1037–1046.
Cheng E, Souza RF, Spechler SJ. Tissue remodeling in eosinophilic esophagitis. Am J Physiol Gastrointest Liver Physiol. 2012;303:G1175–G1187.
Branton MH, Kopp JB. TGF-β and fibrosis. Microbes Infect. 1999;1:1349–1365.
Dellon ES, Liacouras CA, Molina-Infante J, Furuta GT. Updated international consensus diagnostic criteria for eosinophilic esophagitis: proceedings of the AGREE conference. Gastroenterology. 2018;. https://doi.org/10.1053/j.gastro.2018.07.009.
Acknowledgments
Portions of this study have been presented in abstract form at the Annual Symposium of Digestive Disease Week (DDW) 2017, Chicago, IL, on May 6–9, 2017.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The authors confirm that due consideration was given to the protection of intellectual property associated with this work and that there are no impediments to publication, including the timing of publication, with respect to intellectual property. In doing so, the authors have followed the regulations of our institutions concerning intellectual property. The authors confirm that no aspect of the work covered in this manuscript has involved either experimental animals or human patients or required use of informed consent. This study was approved through the Utah Institutional Review Board (IRB #00061947).
Rights and permissions
About this article
Cite this article
Kutty, G.R., Downs-Kelly, E., Crispin, H.T. et al. Elevated Tryptase in EoE Is an Independent Phenomenon Associated with Extra-Esophageal Symptoms. Dig Dis Sci 64, 152–157 (2019). https://doi.org/10.1007/s10620-018-5298-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-018-5298-7