Abstract
Background
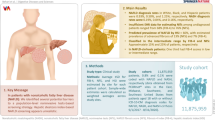
Nonalcoholic fatty liver disease (NAFLD) is the most common cause of chronic liver disease. Severe NAFLD with advanced fibrosis results in substantial morbidity and mortality. Associated with metabolic syndrome, NAFLD is often initially clinically silent, yet intensive lifestyle intervention with 7% or greater weight loss can improve or resolve NAFLD. Using a Veterans Health Administration (VHA) liver biopsy cohort, we evaluated simple noninvasive fibrosis scoring systems to identify NAFLD with advanced fibrosis (or severe disease) to assist providers.
Methods
In our retrospective study of a national VHA sample of patients with biopsy-proven NAFLD or normal liver (2005–2015), we segregated patients by fibrosis stage (0–4). Non-NAFLD liver disease was excluded. We evaluated the diagnostic accuracy of the NAFLD fibrosis score (NFS), fibrosis-4 calculator (FIB-4), aspartate aminotransferase-to-alanine aminotransferase ratio (AST/ALT ratio), AST-to-platelet ratio index (APRI), and body mass index, AST/ALT ratio, and diabetes (BARD) score by age groups.
Results
We included 329 patients with well-defined liver histology (296 NAFLD and 33 normal controls without fibrosis), in which 92 (28%) had advanced (stage 3–4) fibrosis. Across all age groups, NFS and FIB-4 best predicted advanced fibrosis (NFS with 0.676 threshold: AUROC 0.71–0.76, LR + 2.30–22.05, OR 6.00–39.58; FIB-4 with 2.67 threshold: AUROC of 0.62–0.80, LR + 4.70–27.45, OR 16.34–59.65).
Conclusions
While NFS and FIB-4 scores exhibit good diagnostic accuracy, FIB-4 is optimal in identifying NAFLD advanced fibrosis in the VHA. Easily implemented as a point-of-care clinical test, FIB-4 can be useful in directing patients that are most likely to have advanced fibrosis to GI/hepatology consultation and follow-up.
Similar content being viewed by others
Change history
24 July 2018
The original version of the article unfortunately contained errors in Table 3, Risk Factor column headings “Age > 50 (n = 115),” “Age > 50–64 (n = 154),” and “Age > 65 + (n = 60).”
Abbreviations
- AUROC:
-
Area under the ROC
- ALT:
-
Alanine aminotransferase
- AST:
-
Aspartate aminotransferase
- APRI:
-
AST-to-platelet ratio index
- BARD score:
-
Body mass index, AST/ALT ratio, and diabetes
- AUDIT-C:
-
Alcohol Use Disorders Identification Test Alcohol Consumption Questions
- BMI:
-
Body mass index
- FIB-4:
-
Fibrosis-4 calculator
- HCC:
-
Hepatocellular carcinoma
- NAFL:
-
Nonalcoholic fatty liver
- NAFLD:
-
Nonalcoholic fatty liver disease
- NFS:
-
NAFLD fibrosis score
- NASH:
-
Nonalcoholic steatohepatitis
- ROC:
-
Receiver operating characteristic curve
- VHA:
-
Veterans Health Administration
References
Chalasani N, Younossi Z, Lavine JE, et al. The diagnosis and management of nonalcoholic fatty liver disease: practice guidance from the American Association for the Study of Liver Diseases. Hepatology (Baltimore, Md). 2018;67:328–357.
Targher G, Byrne CD, Lonardo A, Zoppini G, Barbui C. Nonalcoholic fatty liver disease and risk of incident cardiovascular disease: a meta-analysis. J Hepatol. 2016;65:589–600.
EASL-EASD-EASO. Clinical practice guidelines for the management of nonalcoholic fatty liver disease. J Hepatol. 2016;64:1388–1402.
Rinella ME. Nonalcoholic fatty liver disease: a systematic review. Jama. 2015;313:2263–2273.
Angulo P, Hui JM, Marchesini G, et al. The NAFLD fibrosis score: a noninvasive system that identifies liver fibrosis in patients with NAFLD. Hepatology. 2007;45:846–854.
Angulo P, Kleiner DE, Dam-Larsen S, et al. Liver fibrosis, but no other histologic features, is associated with long-term outcomes of patients with nonalcoholic fatty liver disease. Gastroenterology. 2015;149:389–397.e310.
Younossi ZM, Blissett D, Blissett R, et al. The economic and clinical burden of nonalcoholic fatty liver disease in the United States and Europe. Hepatology. 2016;64:1577–1586.
Younossi ZM, Stepanova M, Rafiq N, et al. Pathologic criteria for nonalcoholic steatohepatitis: interprotocol agreement and ability to predict liver-related mortality. Hepatology. 2011;53:1874–1882.
Goldberg D, Ditah IC, Saeian K, et al. Changes in the prevalence of hepatitis C virus infection, nonalcoholic steatohepatitis, and alcoholic liver disease among patients with cirrhosis or liver failure on the waitlist for liver transplantation. Gastroenterology. 2017;152:1090–1099.e1091.
Golabi P, Otgonsuren M, Cable R, et al. Nonalcoholic fatty liver disease (NAFLD) is associated with impairment of health related quality of life (HRQOL). Health Qual Outcomes. 2016;14:18.
Sayiner M, Otgonsuren M, Cable R, et al. Variables associated with inpatient and outpatient resource utilization among Medicare beneficiaries with nonalcoholic fatty liver disease with or without cirrhosis. J Clin Gastroenterol. 2017;51:254.
Bril F, Barb D, Portillo-Sanchez P, et al. Metabolic and histological implications of intrahepatic triglyceride content in nonalcoholic fatty liver disease. Hepatology. 2017;65:1132–1144.
Singh S, Allen AM, Wang Z, Prokop LJ, Murad MH, Loomba R. Fibrosis progression in nonalcoholic fatty liver vs nonalcoholic steatohepatitis: a systematic review and meta-analysis of paired-biopsy studies. Clin Gastroenterol Hepatol. 2015;13:643–654.e649.
Kleiner DE, Brunt EM, Van Natta M, et al. Design and validation of a histological scoring system for nonalcoholic fatty liver disease. Hepatology. 2005;41:1313–1321.
Bedossa P, Burt AD, Gouw A, et al. Utility and appropriateness of the FLIP algorithm and SAF score in the evaluation of biopsies of nonalcoholic fatty liver disease. Hepatology. 2014;60:565–567.
Vuppalanchi R, Ünalp A, Van Natta ML, et al. Effects of liver biopsy sample length and number of readings on sampling variability in nonalcoholic fatty liver disease. Clin Gastroenterol Hepatol. 2009;7:481–486.
Tapper EB, Lok AS-F. Use of liver imaging and biopsy in clinical practice New England. J Med. 2017;377:756–768.
Tapper EB, Sengupta N, Hunink MM, Afdhal NH, Lai M. Cost-effective evaluation of nonalcoholic fatty liver disease with NAFLD fibrosis score and vibration controlled transient elastography. Am J Gastroenterol. 2015;110:1298.
Cui J, Ang B, Haufe W, et al. Comparative diagnostic accuracy of magnetic resonance elastography vs. eight clinical prediction rules for non-invasive diagnosis of advanced fibrosis in biopsy-proven nonalcoholic fatty liver disease: a prospective study. Aliment Pharmacol Ther. 2015;41:1271–1280.
Sterling RK, Lissen E, Clumeck N, et al. Development of a simple noninvasive index to predict significant fibrosis in patients with HIV/HCV coinfection. Hepatology. 2006;43:1317–1325.
Harrison SA, Oliver D, Arnold HL, Gogia S, Neuschwander-Tetri BA. Development and validation of a simple NAFLD clinical scoring system for identifying patients without advanced disease. Gut. 2008;57:1441–1447.
Kanwal F, Kramer JR, Duan Z, Yu X, White D, El-Serag HB. Trends in the burden of nonalcoholic fatty liver disease in a United States cohort of veterans. Clin Gastroenterol Hepatol. 2016;14:301–308.e302.
Mittal S, El-Serag HB, Sada YH, et al. Hepatocellular carcinoma in the absence of cirrhosis in United States veterans is associated with nonalcoholic fatty liver disease. Clin Gastroenterol Hepatol. 2016;14:124–131.e121.
Patel YA, Gifford EJ, Glass LM, et al. Risk factors for biopsy-proven advanced nonalcoholic fatty liver disease in the Veterans Health Administration. Aliment Pharmacol Ther. 2017;47:268–278.
Shah AG, Lydecker A, Murray K, et al. Comparison of noninvasive markers of fibrosis in patients with nonalcoholic fatty liver disease. Clin Gastroenterol Hepatol. 2009;7:1104–1112.
McPherson S, Hardy T, Dufour J-F, et al. Age as a confounding factor for the accurate non-invasive diagnosis of advanced NAFLD fibrosis. Am J Gastroenterol. 2017;112:740.
Wai CT, Greenson JK, Fontana RJ, et al. A simple noninvasive index can predict both significant fibrosis and cirrhosis in patients with chronic hepatitis C. Hepatology. 2003;38:518–526.
Williams AL, Hoofnagle JH. Ratio of serum aspartate to alanine aminotransferase in chronic hepatitis relationship to cirrhosis. Gastroenterology. 1988;95:734–739.
Eusebi P. Diagnostic accuracy measures. Cerebrovasc Dis. 2013;36:267–272.
Seed P. DIAGT: Stata module to report summary statistics for diagnostic tests compared to true disease status. EconPapers: 2010. Available at: https://econpapers.repec.org/software/bocbocode/s423401.htm. Accessed 30 Mar 2018.
National Center for Veterans Analysis and Statistics. Profile of Veterans (2016). Data from the American Community Survey; 2018. Available at: https://www.va.gov/vetdata/docs/SpecialReports/Profile_of_Veterans_2016.pdf. Accessed 10 Mar 2018.
Vilar-Gomez E, Martinez-Perez Y, Calzadilla-Bertot L, et al. Weight loss through lifestyle modification significantly reduces features of nonalcoholic steatohepatitis. Gastroenterology. 2015;149:367–378.e365.
Del Re AC, Maciejewski ML, Harris AH. MOVE: weight management program across the veterans health administration: patient-and facility-level predictors of utilization. BMC Health Serv Res. 2013;13:511.
Batch BC, Goldstein K, Yancy WS Jr, et al. Outcome by gender in the veterans health administration motivating overweight/obese veterans everywhere weight management program. J Women’s Health (Larchmt). 2018;27:32–39.
Knowler WC, Barrett-Connor E, Fowler SE, et al. Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. N Engl J Med. 2002;346:393–403.
Haw JS, Galaviz KI, Straus AN, et al. Long-term sustainability of diabetes prevention approaches: a systematic review and meta-analysis of randomized clinical trials. JAMA Intern Med. 2017;177:1808–1817.
Brito JP, Montori VM, Davis AM. Metabolic surgery in the treatment algorithm for type 2 diabetes: a joint statement by international diabetes organizations. Jama. 2017;317:635–636.
Lassailly G, Caiazzo R, Buob D, et al. Bariatric surgery reduces features of nonalcoholic steatohepatitis in morbidly obese patients. Gastroenterology. 2015;149:379–388.
Saab S, Mallam D, Cox GA, Tong MJ. Impact of coffee on liver diseases: a systematic review. Liver Int. 2014;34:495–504.
Molloy JW, Calcagno CJ, Williams CD, Jones FJ, Torres DM, Harrison SA. Association of coffee and caffeine consumption with fatty liver disease, nonalcoholic steatohepatitis, and degree of hepatic fibrosis. Hepatology.. 2012;55:429–436.
Armstrong MJ, Gaunt P, Aithal GP, et al. Liraglutide safety and efficacy in patients with nonalcoholic steatohepatitis (LEAN): a multicentre, double-blind, randomised, placebo-controlled phase 2 study. Lancet. 2016;387:679–690.
Neuschwander-Tetri BA, Clark JM, Bass NM, et al. Clinical, laboratory and histological associations in adults with nonalcoholic fatty liver disease. Hepatology. 2010;52:913–924.
Funding
This work was supported in part by resources from the Veterans Affairs (VA) Cooperative Studies Program Epidemiology Center, Durham, and the VA Ann Arbor Healthcare Systems.
Author information
Authors and Affiliations
Contributions
All authors had access to the data and a role in writing/preparing the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The views expressed in this paper are those of the authors and do not necessarily represent the policies or position of, nor imply endorsement from, the Department of Veterans Affairs, or US Government. Christine M. Hunt has received consultancy fees from Otsuka and Indivior.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Patel, Y.A., Gifford, E.J., Glass, L.M. et al. Identifying Nonalcoholic Fatty Liver Disease Advanced Fibrosis in the Veterans Health Administration. Dig Dis Sci 63, 2259–2266 (2018). https://doi.org/10.1007/s10620-018-5123-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-018-5123-3