Abstract
Purpose
Upgrade rates of conventional ADH are reported at 10–30%; however, rates for ADH bordering on DCIS (ADH-BD) are largely unknown. We examined the upgrade rate of ADH-BD and core needle biopsy (CNB) features associated with upgrade. Surgical management in patients with concurrent ipsilateral breast cancer (BC) was also examined.
Methods
From 2000 to 2018, women with CNB diagnosis of ADH-BD were prospectively identified. Women with pure ADH-BD and concurrent ipsilateral ADH-BD/BC were analyzed separately, and upgrade rates were calculated. CNB features associated with upgrade and type of surgery were examined in women with pure ADH-BD; CNB features and concurrent pathology associated with upgrade were examined in women with ipsilateral BC.
Results
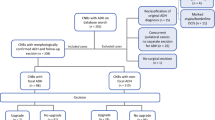
108/236 (46%) patients with pure ADH-BD on CNB had DCIS (40%) or invasive carcinoma (6%) on surgical excision. DCIS or invasive carcinoma was more frequently found on excision of a mass that yielded ADH-BD on biopsy than excision of calcifications (65% vs 38%; p < 0.001). The breast conservation success rate was high (80%) in patients who upgraded, despite a high re-excision rate of 46%. The upgrade rate of ADH-BD in women with concurrent ipsilateral BC was 41%. Most women (94%) with ADH-BD in the same quadrant as the BC were candidates for breast conserving surgery, with a success rate of 89%.
Conclusion
The upgrade rate for pure ADH-BD is significantly higher than that reported for women with conventional ADH, especially in women with a mass on imaging. The upgrade rate of concurrent ipsilateral ADH-BD and BC is similarly high. Excision with a margin of normal tissue and specimen inking should be routine to minimize the need for re-excision.


Similar content being viewed by others
References
Racz JM, Carter JM, Degnim AC (2017) Lobular neoplasia and atypical ductal hyperplasia on core biopsy: current surgical management recommendations. Ann Surg Oncol 24(10):2848–2854
Page DL, Dupont WD, Rogers LW, Rados MS (1985) Atypical hyperplastic lesions of the female breast. A long-term follow-up study. Cancer 55(11):2698–2708
Tavassoli FA, Norris HJ (1990) A comparison of the results of long-term follow-up for atypical intraductal hyperplasia and intraductal hyperplasia of the breast. Cancer 65(3):518–529
Rosai J (1991) Borderline epithelial lesions of the breast. Am J Surg Pathol 15(3):209–221
Tozbikian G, Brogi E, Vallejo CE et al (2017) Atypical ductal hyperplasia bordering on ductal carcinoma in situ. Int J Surg Pathol 25(2):100–107
Burak WE Jr, Owens KE, Tighe MB et al (2000) Vacuum-assisted stereotactic breast biopsy: histologic underestimation of malignant lesions. Arch Surg 135(6):700–703
Deshaies I, Provencher L, Jacob S et al (2011) Factors associated with upgrading to malignancy at surgery of atypical ductal hyperplasia diagnosed on core biopsy. Breast 20(1):50–55
Jackman RJ, Birdwell RL, Ikeda DM (2002) Atypical ductal hyperplasia: can some lesions be defined as probably benign after stereotactic 11-gauge vacuum-assisted biopsy, eliminating the recommendation for surgical excision? Radiology 224(2):548–554
Sohn V, Arthurs Z, Herbert G et al (2007) Atypical ductal hyperplasia: improved accuracy with the 11-gauge vacuum-assisted versus the 14-gauge core biopsy needle. Ann Surg Oncol 14(9):2497–2501
Winchester DJ, Bernstein JR, Jeske JM et al (2003) Upstaging of atypical ductal hyperplasia after vacuum-assisted 11-gauge stereotactic core needle biopsy. Arch Surg 138(6):619–622
Vandenbussche CJ, Khouri N, Sbaity E et al (2013) Borderline atypical ductal hyperplasia/low-grade ductal carcinoma in situ on breast needle core biopsy should be managed conservatively. Am J Surg Pathol 37(6):913–923
Kuhl CK, Keulers A, Strobel K, Schneider H, Gaisa N, Schrading S (2018) Not all false positive diagnoses are equal: on the prognostic implications of false-positive diagnoses made in breast MRI versus in mammography/digital tomosynthesis screening. Breast Cancer Res 20(1):13
Adrales G, Turk P, Wallace T, Bird R, Norton HJ, Greene F (2000) Is surgical excision necessary for atypical ductal hyperplasia of the breast diagnosed by Mammotome? Am J Surg 180(4):313–315
Philpotts LE, Lee CH, Horvath LJ, Lange RC, Carter D, Tocino I (2000) Underestimation of breast cancer with II-gauge vacuum suction biopsy. AJR Am J Roentgenol 175(4):1047–1050
Co M, Kwong A, Shek T (2018) Factors affecting the under-diagnosis of atypical ductal hyperplasia diagnosed by core needle biopsies—a 10-year retrospective study and review of the literature. Int J Surg 49:27–31
Khoury T, Chen X, Wang D et al (2015) Nomogram to predict the likelihood of upgrade of atypical ductal hyperplasia diagnosed on a core needle biopsy in mammographically detected lesions. Histopathology 67(1):106–120
Ko E, Han W, Lee JW et al (2008) Scoring system for predicting malignancy in patients diagnosed with atypical ductal hyperplasia at ultrasound-guided core needle biopsy. Breast Cancer Res Treat 112(1):189–195
Jang M, Cho N, Moon WK, Park JS, Seong MH, Park IA (2008) Underestimation of atypical ductal hyperplasia at sonographically guided core biopsy of the breast. AJR Am J Roentgenol 191(5):1347–1351
Mesurolle B, Perez JC, Azzumea F et al (2014) Atypical ductal hyperplasia diagnosed at sonographically guided core needle biopsy: frequency, final surgical outcome, and factors associated with underestimation. AJR Am J Roentgenol 202(6):1389–1394
Morrow M, Van Zee KJ, Solin LJ et al (2016) Society of Surgical Oncology-American Society for Radiation Oncology-American Society of Clinical Oncology Consensus Guideline on margins for breast-conserving surgery with whole-breast irradiation in ductal carcinoma in situ. Ann Surg Oncol 23(12):3801–3810
Mamtani A, Romanoff A, Baser R, Vincent A, Morrow M, Gemignani ML (2020) Adoption of SSO-ASTRO margin guidelines for ductal carcinoma in situ: what is the impact on use of additional surgery? Ann Surg Oncol. https://doi.org/10.1245/s10434-020-08610-7
Havel L, Naik H, Ramirez L, Morrow M, Landercasper J (2019) Impact of the SSO-ASTRO margin guideline on rates of re-excision after lumpectomy for breast cancer: a meta-analysis. Ann Surg Oncol 26(5):1238–1244
Rosenberger LH, Mamtani A, Fuzesi S et al (2016) Early adoption of the SSO-ASTRO consensus guidelines on margins for breast-conserving surgery with whole-breast irradiation in stage I and II invasive breast cancer: initial experience from memorial Sloan Kettering Cancer Center. Ann Surg Oncol 23(10):3239–3246
Rosenkranz KM, Ballman K, McCall L et al (2020) Cosmetic outcomes following breast-conservation surgery and radiation for multiple ipsilateral breast cancer: data from the alliance Z11102 study. Ann Surg Oncol. https://doi.org/10.1245/s10434-020-08893-w
Choi DX, Eaton AA, Olcese C, Patil S, Morrow M, Van Zee KJ (2013) Blurry boundaries: do epithelial borderline lesions of the breast and ductal carcinoma in situ have similar rates of subsequent invasive cancer? Ann Surg Oncol 20(4):1302–1310
Coopey SB, Mazzola E, Buckley JM et al (2012) The role of chemoprevention in modifying the risk of breast cancer in women with atypical breast lesions. Breast Cancer Res Treat 136(3):627–633
Funding
The preparation of this manuscript was funded in part by NIH/NCI Cancer Center Support Grant No. P30CA008748 to Memorial Sloan Kettering Cancer Center.
Author information
Authors and Affiliations
Contributions
Kate Pawloski, Nicole Christian, Andrea Knezevic, Hannah Y. Wen, Kimberly J. Van Zee, and Audree B. Tadros were involved in the conception and design of the study, acquisition of data, study supervision. All authors were involved in the analysis and interpretation of data and writing, review, and/or revision of this manuscript, and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
Dr. Monica Morrow declares the receipt of speaking honoraria from Genomic Health. Drs. Kate Pawloski, Nicole Christian, Andrea Knezevic, Hannah Y. Wen, Kimberly J. Van Zee, Audree B. Tadros declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. This article does not contain any studies with animals performed by any of the authors.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Pawloski, K.R., Christian, N., Knezevic, A. et al. Atypical ductal hyperplasia bordering on DCIS on core biopsy is associated with higher risk of upgrade than conventional atypical ductal hyperplasia. Breast Cancer Res Treat 184, 873–880 (2020). https://doi.org/10.1007/s10549-020-05890-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-020-05890-1