Abstract
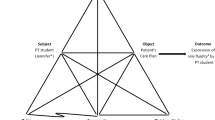
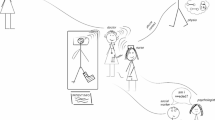
Practice based interprofessional education opportunities are proposed as a mechanism for health professionals to learn teamwork skills and gain an understanding of the roles of others. Primary care is an area of practice that offers a promising option for interprofessional student learning. In this study, we investigated what and how students from differing professions learn together. Our findings inform the design of future interprofessional education initiatives. Using activity theory, we conducted an ethnographic investigation of interprofessional education in primary care. During a 5 months period, we observed 14 clinic sessions involving mixed discipline student teams who interviewed people with chronic disease. Teams were comprised of senior medicine, nursing, occupational therapy, pharmacy and physiotherapy entry level students. Semi-structured interviews were also conducted with seven clinical educators. Data were analysed to ascertain the objectives, tools, rules and division of labour. Two integrated activity systems were identified: (1) student teams gathering information to determine patients’ health care needs and (2) patients either as health consumers or student educators. Unwritten rules regarding ‘shared contribution’, ‘patient as key information source’ and ‘time constraints’ were identified. Both the significance of software literacy on team leadership, and a pre-determined structure of enquiry, highlighted the importance of careful consideration of the tools used in interprofessional education, and the way they can influence practice. The systems of practice identified provide evidence of differing priorities and values, and multiple perspectives of how to manage health. The work reinforced the value of the patients’ voice in clinical and education processes.

Similar content being viewed by others
References
Australian Government Productivity Commission. (2011). Caring for older Australians: Overview, report no. 53. Canberra. Retrieved December 10, 2014, from http://www.pc.gov.au/inquiries/completed/aged-care/report/aged-care-overview-booklet.pdf
Australian Medical Council. (2010). Assessment and accreditation of medical schools: Standards and procedures, 2011. Australia.
Barr, H. (2013). Toward a theoretical framework for interprofessional education. Journal of Interprofessional Care, 27(1), 4–9.
Barr (2015). Interprofessional education: The genesis of a global movement. CAIPE. Retrieved November 20, 2015, from http://caipe.org.uk/silo/files/global-ipe-2015-corrected-hb-sept–2015pdf.pdf
Bleakley, A., Bligh, J., & Browne, J. (2011). In S. Hamstra (Ed.), Medical education for the future: Identity, power and location, Advances in Medical Education series (Vol. 1). New York: Springer.
CIHC. (2010). A national interprofessional competency framework. Retrieved December 10, 2014, from http://www.cihc.ca/files/CIHC_IPCompetencies_Feb1210.pdf
Colthart, I., Bagnall, G., Evans, A., Allbutt, H., Haig, A., Illing, J., & McKinstry, B. (2008). The effectiveness of self-assessment on the identification of learner needs, learner activity, and impact on clinical practice: BEME guide no. 10. Medical Teacher, 30(2), 124–145.
EBSCO Publishing. (2014). MIMS abbreviated. NSW: St Leonards.
Engestrom, Y. (2008). From teams to knots: Activity-theoretical studies of collaboration and learning at work. Cambridge: Cambridge University Press.
Engeström, Y. (2001). Expansive learning at work: Toward an activity theoretical reconceptualization. Journal of Education and Work, 14, 133–156.
Frenk, J., Chen, L., Bhutta, Z. A., Cohen, J., Crisp, N., Evans, T., & Zurayk, H. (2010). Health professionals for a new century: Transforming education to strengthen health systems in an interdependent world. The Lancet, 376(9756), 1923–1958.
Haddara, W., & Lingard, L. (2013). Are we all on the same page? A discourse analysis of interprofessional collaboration. Academic Medicine, 88(10), 1509–1515.
Haines, T. P., Kent, F., & Keating, J. L. (2014). Interprofessional student clinics: An economic evaluation of collaborative clinical placement education. Journal of Interprofessional Care, 28(4), 292–298.
Hammick, M., Freeth, D., Koppel, I., Reeves, S., & Barr, H. (2007). A best evidence systematic review of interprofessional education: BEME guide no. 9. Medical Teacher, 29, 735–751.
Health Workforce Australia. (2011). National health workforce Innovation and reform strategic framework for action 2011–2015. Retrieved December 10, 2014, from http://www.hwa.gov.au/sites/uploads/hwa-wir-strategic-framework-for-action-201110.pdf
Holmqvist, M., Courtney, C., Meilli, R., & Dick, A. (2012). Student-run clinics: Opportunities for interprofessional education and increasing social accountability. Journal of Research in Interprofessional Practice and Education, 2, 264–277.
Kent, F., Drysdale, P., Martin, N., & Keating, J. L. (2014). The mixed discipline aged care student clinic: An authentic interprofessional learning initiative. Journal of Allied Health, 43(1), 51–56.
Kent, F., & Keating, J. (2013). Patient outcomes from a student-led interprofessional clinic in primary care. Journal of Interprofessional Care, 27(4), 336–338.
Kent, F., & Keating, J. L. (2015). Interprofessional education in primary care for entry level students—A systematic literature review. Nurse Education Today, 35(12), 1221–1231.
Lai, F., Kent, F., & Dodic, M. (2015). Student-led interprofessional clinics may improve health management in patients with chronic disease. Medical Journal Australia, 203(10), 402.
Leucht, R., Madsen, M., Taugher, M., & Petterson, B. (1990). Interprofessional education perception scale. Journal of Allied Health, 19(2), 181–191.
Lingard, L., McDougall, A., Levstik, M., Chandok, N., Spafford, M. M., & Schryer, C. (2012a). Representing compexity well: A story about teamwork, with implications for how we teach collaboration. Medical Education, 46, 869–877.
Lingard, L., Vanstone, M., Durrant, M., Fleming-Carroll, B., Lowe, M., Rashotte, J., & Tallett, S. (2012b). Conflicting messages: Examining the dynamics of leadership on interprofessional teams. Academic Medicine, 87(12), 1762–1767.
Miles, M., & Huberman, A. M. (1994). Qualitative data analysis: An expanded sourcebook (2nd ed.). Thousand Oaks: Sage Publications.
Parsell, G., & Bligh, J. (1999). The development of a questionnaire to assess the readiness of health care students for interprofessional learning (ripls). Medical Education, 33(2), 95–100.
Reeves, S., & Lewin, S. (2004). Interprofessional collaboration in the hospital: Strategies and meanings. Journal of Health Services & Research Policy, 9(4), 218–225.
Reeves, S., Perrier, L., Goldman, J., Freeth, D., & Zwarenstein, M. (2013). Interprofessional education: Effects on professional practice and healthcare outcomes (update) (review). Cochrane Database of Systematic Reviews, 3.
The Commonwealth of Australia. (2015). 2015 Intergenerational report Australia in 2055.
The Interprofessional Curriculum Renewal Consortium. (2014). Curriculum renewal for interprofessional education in health. Australia: Commonwealth of Australia, Office for Learning and Teaching.
Towle, A., Bainbridge, L., Godolphin, W., Katz, A., Kline, C., Lown, B., & Thistlethwaite, J. (2010). Active patient involvement in the education of health professionals. Medical Education, 44(1), 64–74.
Varpio, L., Hall, P., Lingard, L., & Schryer, C. F. (2008). Interprofessional communication and medical error: A reframing of research questions and approaches. Academic Medicine, 83(10 Suppl), S76–S81.
World Health Organisation. (2010). Framework for action on interprofessional education and collaborative practice. Geneva.
Acknowledgments
This project received funding from the Australian Government and the Department of Health, Victoria.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kent, F., Francis-Cracknell, A., McDonald, R. et al. How do interprofessional student teams interact in a primary care clinic? A qualitative analysis using activity theory. Adv in Health Sci Educ 21, 749–760 (2016). https://doi.org/10.1007/s10459-015-9663-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10459-015-9663-4