Abstract
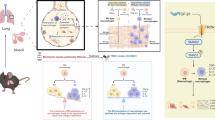
Proper lymphatic function is necessary for the transport of fluids, macromolecules, antigens and immune cells out of the interstitium. The lymphatic endothelium plays important roles in the modulation of lymphatic contractile activity and lymph transport, but it’s role as a barrier between the lymph and interstitial compartments is less well understood. Alterations in lymphatic function have long been associated with edema and inflammation although the integrity of the lymphatic endothelial barrier during inflammation is not well-defined. In this paper we evaluated the integrity of the lymphatic barrier in response to inflammatory stimuli commonly associated with increased blood endothelial permeability. We utilized in vitro assays of lymphatic endothelial cell (LEC) monolayer barrier function after treatment with different inflammatory cytokines and signaling molecules including TNF-α, IL-6, IL-1β, IFN-γ and LPS. Moderate increases in an index of monolayer barrier dysfunction were noted with all treatments (20–60 % increase) except IFN-γ which caused a greater than 2.5-fold increase. Cytokine-induced barrier dysfunction was blocked or reduced by the addition of LNAME, except for IL-1β and LPS treatments, suggesting a regulatory role for nitric oxide. The decreased LEC barrier was associated with modulation of both intercellular adhesion and intracellular cytoskeletal activation. Cytokine treatments reduced the expression of VE-cadherin and increased scavenging of β-catenin in the LECs and this was partially reversed by LNAME. Likewise the phosphorylation of myosin light chain 20 at the regulatory serine 19 site, which accompanied the elevated monolayer barrier dysfunction in response to cytokine treatment, was also blunted by LNAME application. This suggests that the lymphatic barrier is regulated during inflammation and that certain inflammatory signals may induce large increases in permeability.





Similar content being viewed by others
References
Casley-Smith JR (1968) How the lymphatic system works. Lymphology 1(3):77–80
Miteva DO, Rutkowski JM, Dixon JB, Kilarski W, Shields JD, Swartz MA (2010) Transmural flow modulates cell and fluid transport functions of lymphatic endothelium. Circ Res 106(5):920–931. doi:10.1161/CIRCRESAHA.109.207274
Angeli V, Ginhoux F, Llodra J, Quemeneur L, Frenette PS, Skobe M, Jessberger R, Merad M, Randolph GJ (2006) B cell-driven lymphangiogenesis in inflamed lymph nodes enhances dendritic cell mobilization. Immunity 24(2):203–215. doi:10.1016/j.immuni.2006.01.003
Angeli V, Randolph GJ (2006) Inflammation, lymphatic function, and dendritic cell migration. Lymphat Res Biol 4(4):217–228. doi:10.1089/lrb 2006.4406
Jakubzick C, Bogunovic M, Bonito AJ, Kuan EL, Merad M, Randolph GJ (2008) Lymph-migrating, tissue-derived dendritic cells are minor constituents within steady-state lymph nodes. J Exp Med 205(12):2839–2850. doi:10.1084/jem.20081430
Maruyama K, Ii M, Cursiefen C, Jackson DG, Keino H, Tomita M, Van Rooijen N, Takenaka H, D’Amore PA, Stein-Streilein J, Losordo DW, Streilein JW (2005) Inflammation-induced lymphangiogenesis in the cornea arises from CD11b-positive macrophages. J Clin Invest 115(9):2363–2372
Muller WA, Randolph GJ (1999) Migration of leukocytes across endothelium and beyond: molecules involved in the transmigration and fate of monocytes. J Leukoc Biol 66(5):698–704
Randolph GJ, Angeli V, Swartz MA (2005) Dendritic-cell trafficking to lymph nodes through lymphatic vessels. Nat Rev Immunol 5(8):617–628. doi:10.1038/nri1670
Skobe M, Detmar M (2000) Structure, function, and molecular control of the skin lymphatic system. J Investig Dermatol Symp Proc 5(1):14–19. doi:10.1046/j.1087-0024.2000.00001.x
Zawieja SD, Wang W, Wu X, Nepiyushchikh ZV, Zawieja DC, Muthuchamy M (2012) Impairments in the intrinsic contractility of mesenteric collecting lymphatics in a rat model of metabolic syndrome. Am J Physiol Heart Circ Physiol 302(3):H643–H653. doi:10.1152/ajpheart.00606.2011
Sessa WC (2009) Molecular control of blood flow and angiogenesis: role of nitric oxide. J Thromb Haemost 7(Suppl 1):35–37
Spyridopoulos I, Luedemann C, Chen D, Kearney M, Chen D, Murohara T, Principe N, Isner JM, Losordo DW (2002) Divergence of angiogenic and vascular permeability signaling by VEGF: inhibition of protein kinase C suppresses VEGF-induced angiogenesis, but promotes VEGF-induced, NO-dependent vascular permeability. Arterioscler Thromb Vasc Biol 22(6):901–906
Moncada S, Higgs EA (1991) Endogenous nitric oxide: physiology, pathology and clinical relevance. Eur J Clin Invest 21(4):361–374
Davenpeck KL, Gauthier TW, Lefer AM (1994) Inhibition of endothelial-derived nitric oxide promotes P-selectin expression and actions in the rat microcirculation. Gastroenterology 107(4):1050–1058
Krieglstein CF, Anthoni C, Cerwinka WH, Stokes KY, Russell J, Grisham MB, Granger DN (2007) Role of blood- and tissue-associated inducible nitric-oxide synthase in colonic inflammation. Am J Pathol 170(2):490–496
Gasheva OY, Zawieja DC, Gashev AA (2006) Contraction-initiated NO-dependent lymphatic relaxation: a self-regulatory mechanism in rat thoracic duct. J Physiol 575(Pt 3):821–832. doi:10.1113/jphysiol.2006.115212
Schmid-Schonbein GW (2012) Nitric oxide (NO) side of lymphatic flow and immune surveillance. Proc Natl Acad Sci U S A 109(1):3–4. doi:10.1073/pnas.1117710109
Wu TF, Carati CJ, Macnaughton WK, von der Weid PY (2006) Contractile activity of lymphatic vessels is altered in the TNBS model of guinea pig ileitis. Am J Physiol Gastrointest Liver Physiol 291(4):G566–G574. doi:10.1152/ajpgi.0 0058.2006
von der Weid PY, Muthuchamy M (2010) Regulatory mechanisms in lymphatic vessel contraction under normal and inflammatory conditions. Pathophysiology 17(4):263–276. doi: 10.1016
Hayes H, Kossmann E, Wilson E, Meininger C, Zawieja D (2003) Development and characterization of endothelial cells from rat microlymphatics. Lymphat Res Biol 1(2):101–119
Chakravortty D, Koide N, Kato Y, Sugiyama T, Kawai M, Fukada M, Yoshida T, Yokochi T (2000) Cytoskeletal alterations in lipopolysaccharide-induced bovine vascular endothelial cell injury and its prevention by sodium arsenite. Clin Diagn Lab Immunol 7(2):218–225
Dudek SM, Munoz NM, Desai A, Osan CM, Meliton AY, Leff AR (2011) Group V phospholipase A2 mediates barrier disruption of human pulmonary endothelial cells caused by LPS in vitro. Am J Respir Cell Mol Biol 44(3):361–368. doi:10.1165/rcmb.2009-0446OC
Chaitanya GV, Franks SE, Cromer W, Wells SR, Bienkowska M, Jennings MH, Ruddell A, Ando T, Wang Y, Gu Y, Sapp M, Mathis JM, Jordan PA, Minagar A, Alexander JS (2010) Differential cytokine responses in human and mouse lymphatic endothelial cells to cytokines in vitro. Lymphat Res Biol 8(3):155–164. doi:10.1089/lrb2010.0004
Puhlmann M, Weinreich DM, Farma JM, Carroll NM, Turner EM, Alexander HR Jr (2005) Interleukin-1beta induced vascular permeability is dependent on induction of endothelial tissue factor (TF) activity. J Transl Med 3:37. doi:10.1186/1479-5876-3-37
Bove K, Neumann P, Gertzberg N, Johnson A (2001) Role of ecNOS-derived NO in mediating TNF-induced endothelial barrier dysfunction. Am J Physiol Lung Cell Mol Physiol 280(5):L914–L922
Breslin JW, Yuan SY, Wu MH (2007) VEGF-C alters barrier function of cultured lymphatic endothelial cells through a VEGFR-3-dependent mechanism. Lymphat Res Biol 5(2):105–113. doi:10.1089/lrb2007.1004
Baluk P, Fuxe J, Hashizume H, Romano T, Lashnits E, Butz S, Vestweber D, Corada M, Molendini C, Dejana E, McDonald DM (2007) Functionally specialized junctions between endothelial cells of lymphatic vessels. J Exp Med 204(10):2349–2362. doi:10.1084/jem.20062596
Leak LV, Burke JF (1968) Electron microscopic study of lymphatic capillaries in the removal of connective tissue fluids and particulate substances. Lymphology 1(2):39–52
Chaitanya GV, Cromer W, Wells S, Jennings M, Mathis JM, Minagar A, Alexander JS (2012) Metabolic modulation of cytokine-induced brain endothelial adhesion molecule expression. Microcirculation 19(2):155–165. doi:10.1111/j.1549-8719.2011.00141.x
Barbieri SS, Weksler BB (2007) Tobacco smoke cooperates with interleukin-1beta to alter beta-catenin trafficking in vascular endothelium resulting in increased permeability and induction of cyclooxygenase-2 expression in vitro and in vivo. Faseb J 21(8):1831–1843. doi:10.1096/fj.06-7557com
Sola-Villa D, Camacho M, Sola R, Soler M, Diaz JM, Vila L (2006) IL-1beta induces VEGF, independently of PGE2 induction, mainly through the PI3-K/mTOR pathway in renal mesangial cells. Kidney Int 70(11):1935–1941
Alexander JS, Chaitanya GV, Grisham MB, Boktor M (2010) Emerging roles of lymphatics in inflammatory bowel disease. Ann N Y Acad Sci 1207(Suppl 1):E75–E85. doi:10.1111/j.1749-6632.2010.05757.x
Breslin JW, Gaudreault N, Watson KD, Reynoso R, Yuan SY, Wu MH (2007) Vascular endothelial growth factor-C stimulates the lymphatic pump by a VEGF receptor-3-dependent mechanism. Am J Physiol Heart Circ Physiol 293(1):H709–H718. doi:10.1152/ajpheart.00102.2007
Chatterjee V, Gashev AA (2012) Aging-associated shifts in functional status of mast cells located by adult and aged mesenteric lymphatic vessels. Am J Physiol Heart Circ Physiol 303(6):H693–H702. doi:10.1152/ajpheart.00378.2012
Breslin JW (2011) ROCK and cAMP promote lymphatic endothelial cell barrier integrity and modulate histamine and thrombin-induced barrier dysfunction. Lymphat Res Biol 9(1):3–11. doi:10.1089/lrb2010.0016
Nooteboom A, Van Der Linden CJ, Hendriks T (2002) Tumor necrosis factor-alpha and interleukin-1beta mediate endothelial permeability induced by lipopolysaccharide-stimulated whole blood. Crit Care Med 30(9):2063–2068. doi:10.1097/01.CCM.0000021522.67956.E6
Hunziker T, Brand CU, Kapp A, Waelti ER, Braathen LR (1992) Increased levels of inflammatory cytokines in human skin lymph derived from sodium lauryl sulphate-induced contact dermatitis. Br J Dermatol 127(3):254–257
Olszewski WL, Pazdur J, Kubasiewicz E, Zaleska M, Cooke CJ, Miller NE (2001) Lymph draining from foot joints in rheumatoid arthritis provides insight into local cytokine and chemokine production and transport to lymph nodes. Arthritis Rheum 44(3):541–549. doi:10.1002/1529-0131(200103)44:3<541:AID-ANR102>3.0.CO;2-6
Glass CA, Harper SJ, Bates DO (2006) The anti-angiogenic VEGF isoform VEGF165b transiently increases hydraulic conductivity, probably through VEGF receptor 1 in vivo. J Physiol 572(Pt 1):243–257
Cromer W, Jennings MH, Odaka Y, Mathis JM, Alexander JS (2010) Murine rVEGF164b, an inhibitory VEGF reduces VEGF-A-dependent endothelial proliferation and barrier dysfunction. Microcirculation 17(7):536–547
Wu F, Han M, Wilson JX (2009) Tripterine prevents endothelial barrier dysfunction by inhibiting endogenous peroxynitrite formation. Br J Pharmacol 157(6):1014–1023. doi:10.1111/j.1476-5381.2009.00292.x
Sawa Y, Ueki T, Hata M, Iwasawa K, Tsuruga E, Kojima H, Ishikawa H, Yoshida S (2008) LPS-induced IL-6, IL-8, VCAM-1, and ICAM-1 expression in human lymphatic endothelium. J Histochem Cytochem 56(2):97–109. doi:10.1369/jhc.7A 7299.2007
Ghoshal S, Witta J, Zhong J, de Villiers W, Eckhardt E (2009) Chylomicrons promote intestinal absorption of lipopolysaccharides. J Lipid Res 50(1):90–97. doi:10.1194/jlr.M800156-JLR200
Tzima E, Irani-Tehrani M, Kiosses WB, Dejana E, Schultz DA, Engelhardt B, Cao G, DeLisser H, Schwartz MA (2005) A mechanosensory complex that mediates the endothelial cell response to fluid shear stress. Nature 437(7057):426–431. doi:10.1038/nature03952
Tharakan B, Hellman J, Sawant DA, Tinsley JH, Parrish AR, Hunter FA, Smythe WR, Childs EW (2011) beta-Catenin Dynamics in the Regulation of Microvascular Endothelial Cell Hyperpermeability. Shock. doi:10.1097/SHK.0b013e318240b564
Ding H, Keller KC, Martinez IK, Geransar RM, zur Nieden KO, Nishikawa SG, Rancourt DE, zur Nieden NI (2012) NO-beta-catenin crosstalk modulates primitive streak formation prior to embryonic stem cell osteogenic differentiation. J Cell Sci 125(Pt 22):5564–5577. doi:10.1242/jcs.081703
Kang DE, Soriano S, Frosch MP, Collins T, Naruse S, Sisodia SS, Leibowitz G, Levine F, Koo EH (1999) Presenilin 1 facilitates the constitutive turnover of beta-catenin: differential activity of Alzheimer’s disease-linked PS1 mutants in the beta-catenin-signaling pathway. J Neurosci 19(11):4229–4237
Soriano S, Kang DE, Fu M, Pestell R, Chevallier N, Zheng H, Koo EH (2001) Presenilin 1 negatively regulates beta-catenin/T cell factor/lymphoid enhancer factor-1 signaling independently of beta-amyloid precursor protein and notch processing. J Cell Biol 152(4):785–794
Strawitz JG, Eto K, Mitsuoka H, Olney C, Pairent FW, Howard JM (1968) Molecular weight dependence of lymphatic permeability: the concept of regional cancer chemotheraphy by lymphatic perfusion. Microvasc Res 1(1):58–67
Rigor RR, Shen Q, Pivetti CD, Wu MH, Yuan SY (2012) Myosin Light Chain Kinase Signaling in Endothelial Barrier Dysfunction. Med Res Rev. doi:10.1002/med.21270
Yoshikawa H, Takada K, Muranishi S (1984) Molecular weight dependence of permselectivity to rat small intestinal blood-lymph barrier for exogenous macromolecules absorbed from lumen. J Pharmacobiodyn 7(1):1–6
Scallan JP, Huxley VH (2010) In vivo determination of collecting lymphatic vessel permeability to albumin: a role for lymphatics in exchange. J Physiol 588(Pt 1):243–254. doi:10.1113/jphysiol.2009.179622
Dunworth WP, Fritz-Six KL, Caron KM (2008) Adrenomedullin stabilizes the lymphatic endothelial barrier in vitro and in vivo. Peptides 29(12):2243–2249. doi:10.1016/j.peptides.2008.09.009
Price GM, Chrobak KM, Tien J (2008) Effect of cyclic AMP on barrier function of human lymphatic microvascular tubes. Microvasc Res 76(1):46–51. doi:10.1016/j.mvr.2008.02.003
Hou WH, Liu IH, Tsai CC, Johnson FE, Huang SS, Huang JS (2011) CRSBP-1/LYVE-1 ligands disrupt lymphatic intercellular adhesion by inducing tyrosine phosphorylation and internalization of VE-cadherin. J Cell Sci 124(Pt 8):1231–1244. doi:10.1242/jcs.078154
Acknowledgments
Supported by NIH grants HL070308, DK099221, HL094269, CA140732 and the Scott & White Wigley award.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
10456_2013_9393_MOESM1_ESM.tif
Supplementary Fig 1 Dose response curves of cytokines tested on RLEC monolayer permeability. Each graph is a single experiment with n = 3. These data along with the literature was used to determine which doses to use for further experiments. (TIFF 23578 kb)
10456_2013_9393_MOESM2_ESM.tif
Supplementary Fig 2 Western blots representative data for β-catenin, VE-cadherin and pMLC20/MLC20 ratios from TNF-α, IL-6, IL-1β, LPS and IFN-γ treated RLECs at 1 hour. (TIFF 12587 kb)
Rights and permissions
About this article
Cite this article
Cromer, W.E., Zawieja, S.D., Tharakan, B. et al. The effects of inflammatory cytokines on lymphatic endothelial barrier function. Angiogenesis 17, 395–406 (2014). https://doi.org/10.1007/s10456-013-9393-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10456-013-9393-2