Abstract
Purpose
The aim of this study was to evaluate the testicular parenchyma in pediatric patients with testicular microlithiasis by shear wave elastography (SWE) and compare the values with normal control subjects.
Methods
Twenty-three patients previously diagnosed with testicular microlithiasis under follow-up for 20 ± 11 months were included in the study group. In the control group, 31 patients with no medical history that could affect testicular tissue were prospectively included. Forty-six testes in the study group and 62 testes in the control group were evaluated with gray-scale ultrasound and SWE.
Results
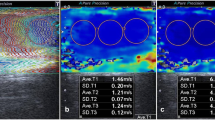
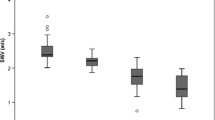
There were no differences in age and testes volume between the study and control groups. The mean SWE values of all testes based on elasticity and speed parameters in the study group were 8.84 ± 2.86 kPa and 1.66 ± 0.26 m/s, respectively. In the control group, mean SWE values were 5.26 ± 1.17 kPa and 1.31 ± 0.14 m/s, respectively. Elasticity values were significantly higher in testes with microlithiasis as compared with the control group (p < 0.001).
Conclusions
SWE evaluation demonstrates the effects of ultrastructural changes in elasticity that are not detected on gray-scale ultrasound. SWE is a more reliable method in follow-up examinations for pediatric testicular microlithiasis.



Similar content being viewed by others
References
Shanmugasundaram R, Singh JC, Kekre NS. Testicular microlithiasis: is there an agreed protocol? Indian J Urol. 2007;23:234–9.
Bennett HF, Middleton WD, Bullock AD, et al. Testicular microlithiasis: US follow-up. Radiology. 2001;218:359–63.
Goede J, Hack WW, van der Voort-Doedens LM, et al. Prevalence of testicular microlithiasis in asymptomatic males 0 to 19 years old. J Urol. 2009;182:1516–20.
Kim B, Winter TC, Ryu JA. Testicular microlithiasis: clinical significance and review of the literature. Eur Radiol. 2003;13:2567–76.
Derogee M, Bevers RF, Prins HJ, et al. Testicular microlithiasis, a premalignant condition: prevalence, histopathologic findings, and relation to testicular tumor. Urology. 2001;57:1133–7.
Bach AM, Hann LE, Hadar O, et al. Testicular microlithiasis: what is its association with testicular cancer? Radiology. 2001;220:70–5.
Backus ML, Mack LA, Middleton WD, et al. Testicular microlithiasis: imaging appearances and pathologic correlation. Radiology. 1994;192:781–5.
Cast JE, Nelson WM, Early AS, et al. Testicular microlithiasis: prevalence and tumor risk in a population referred for scrotal sonography. AJR Am J Roentgenol. 2000;175:1703–6.
Emberton P, Moody AR. Testicular microlithiasis. AJR Am J Roentgenol. 1994;162:1002–3.
Winter TC, Kim B, Lowrance WT, et al. Testicular microlithiasis: what should you recommend? AJR Am J Roentgenol. 2016;206:1164–9.
Guibal A, Renosi G, Rode A, et al. Shear wave elastography: an accurate technique to stage liver fibrosis in chronic liver diseases. Diagn Interv Imaging. 2016;97:91–9.
Samir AE, Allegretti AS, Zhu Q, et al. Shear wave elastography in chronic kidney disease: a pilot experience in native kidneys. BMC Nephrol. 2015;16:119.
Magri F, Chytiris S, Capelli V, et al. Shear wave elastography in the diagnosis of thyroid nodules: feasibility in the case of coexistent chronic autoimmune Hashimoto’s thyroiditis. Clin Endocrinol. 2012;76:137–41.
Trottmann M, Marcon J, D’Anastasi M, et al. Shear-wave elastography of the testis in the healthy man—determination of standard values. Clin Hemorheol Microcirc. 2016;62:273–81.
Trottmann M, Marcon J, D’Anastasi M, et al. The role of VTIQ as a new tissue strain analytics measurement technique in testicular lesions. Clin Hemorheol Microcirc. 2014;58:195–209.
Zhang X, Lv F, Tang J. Shear wave elastography (SWE) is reliable method for testicular spermatogenesis evaluation after torsion. Int J Clin Exp Med. 2015;8:7089.
Dede O, Teke M, Daggulli M, et al. Elastography to assess the effect of varicoceles on testes: a prospective controlled study. Andrologia. 2016;48:257–61.
Ucar AK, Alis D, Samanci C, et al. A preliminary study of shear wave elastography for the evaluation of unilateral palpable undescended testes. Eur J Radiol. 2017;86:248–51.
Richenberg J, Belfield J, Ramchandani P, et al. Testicular microlithiasis imaging and follow-up: guidelines of the ESUR scrotal imaging subcommittee. Eur Radiol. 2015;25:323–30.
Renshaw AA. Testicular calcifications: incidence, histology and proposed pathological criteria for testicular microlithiasis. J Urol. 1998;160:1625–8.
Drut R, Drut RM. Testicular microlithiasis: histologic and immunohistochemical findings in 11 pediatric cases. Pediatr Dev Pathol. 2002;5:544–50.
Holm M, Lenz S, De Meyts ER, et al. Microcalcifications and carcinoma in situ of the testis. BJU Int. 2001;87:144–9.
Sun Z, Xie M, Xiang F, et al. Utility of real-time shear wave elastography in the assessment of testicular torsion. PLoS One. 2015;10:e0138523.
Marte A, Pintozzi L, Creti G, et al. Long-term follow-up of testicular microlithiasis in children and adolescents: multicenter prospective cohort study of the Italian Society of Pediatric Urology. Eur J Pediatr Surg. 2017;27:155–60.
Goddi A, Sacchi A, Magistretti G, et al. Real-time tissue elastography for testicular lesion assessment. Eur Radiol. 2012;22:721–30.
Aigner F, De Zordo T, Pallwein-Prettner L, et al. Real-time sonoelastography for the evaluation of testicular lesions. Radiology. 2012;263:584–9.
Rocher L, Criton A, Gennisson JL, et al. Testicular Shear wave elastography in normal and infertile men: a prospective study on 601 patients. Ultrasound Med Biol. 2017;43:782–9.
Pedersen MR, Osther PJ, Rafaelsen SR. Testicular microlithiasis and preliminary experience of acoustic radiation force impulse imaging. Acta radiol Open. 2016;5:2058460116658686.
Marcon J, Trottmann M, Rubenthaler J, et al. Three-dimensional vs. two-dimensional shear-wave elastography of the testes—preliminary study on a healthy collective. Clin Hemorheol Microcirc. 2016;64:447–56.
Cooper ML, Kaefer M, Fan R, et al. Testicular microlithiasis in children and associated testicular cancer. Radiology. 2014;270:857–63.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical statement
The study was approved by the institutional review committee.
Financial disclosure
The authors have no relevant financial interest in this article.
Conflict of interest
The authors declare that they have all participated in the design, execution, and analysis of the paper, and that they have approved the final version. Additionally, there are no conflicts of interest in connection with this paper, and the material described is not under publication or consideration for publication elsewhere. No financial support was received while the paper was prepared.
About this article
Cite this article
Bayramoglu, Z., Kandemirli, S.G., Comert, R.G. et al. Shear wave elastography evaluation in pediatric testicular microlithiasis: a comparative study. J Med Ultrasonics 45, 281–286 (2018). https://doi.org/10.1007/s10396-017-0837-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10396-017-0837-y