Abstract
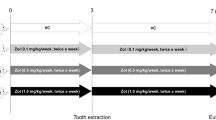
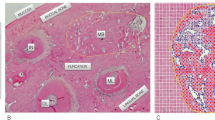
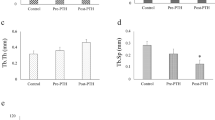
Bone metabolism and repair are directly regulated by arachidonic acid metabolites. At present, we analyzed the dose–response effects of a selective cysteinyl leukotriene receptor type-1 antagonist during bone repair after tooth extraction and on non-injured skeleton. Sixty-three 129 Sv/Ev male mice composed the groups: C—Control (saline solution); MTK2—2 mg/Kg of Montelukast (MTK) and MTK4–4 mg/Kg of MTK, daily administered by mouth throughout all experimental periods set at 7, 14, and 21 days post-operative. Dental sockets were analyzed by computed microtomography (microCT), histopathology, and immunohistochemistry. Femurs, L5 vertebra and organs were also removed for observation. Blood was collected for plasma bone and liver markers. Histopathology and microCT analysis revealed early socket repair of MTK2 and MTK4 animals, with significant increased BV/TV at days 14 and 21 compared to C. Higher plasma calcium was detected at days 7 and 21 in MTK4 in comparison to C, while phosphate was significantly increased in MTK2 in the same periods in comparison to C and MTK4. No significant differences were found regarding plasma ALP and TRAP, neither for local TRAP and Runx2 immunolabeling at the healing sockets. Organs did not present histological abnormalities. Increased AST levels have been detected in distinct groups and periods. In general, femur phenotype was improved in MTK treated animals. Collectively, MTK promoted early bone formation after tooth extraction and increased bone quality of femurs and vertebra in a time-dose-dependent manner, and should be considered as an alternative therapy when improved post-extraction socket repair or skeleton preservation is required.








Similar content being viewed by others
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Spector AA, Kim HY. Cytochrome P450 epoxygenase pathway of polyunsaturated fatty acid metabolism. Biochim Biophys Acta. 2015;1851:356–65.
Bennett M, Gilroy DW. Lipid mediators in inflammation. Microbiol Spectr. 2016. https://doi.org/10.1128/microbiolspec.MCHD-0035-2016.
Feuerstein G, Hallenbeck JM. Leukotrienes in health and disease. FASEB J. 1987;1:186–92.
Grosser T, Fries S, FitzGerald GA. Biological basis for the cardiovascular consequences of COX-2 inhibition: therapeutic challenges and opportunities. J Clin Invest. 2006;116:4–15.
Smyth EM, Grosser T, Wang M, Yu Y, FitzGerald GA. Prostanoids in health and disease. J Lipid Res. 2009;50(Suppl):S423–8.
Lisowska B, Kosson D, Domaracka K. Lights and shadows of NSAIDs in bone healing: the role of prostaglandins in bone metabolism. Drug Des Devel Ther. 2018;12:1753–8.
Saul D, Ninkovic M, Komrakova M, Wolff L, Simka P, Gasimov T, Menger B, Hoffmann DB, Rohde V, Sehmisch S. Effect of zileuton on osteoporotic bone and its healing, expression of bone, and brain genes in rats. J Appl Physiol. 2018;124:118–30.
White AE, Henry JK, Dziadosz D. The Effect of Nonsteroidal Anti-inflammatory Drugs and Selective COX-2 Inhibitors on Bone Healing. HSS J. 2021;17:231–4.
Kam PC, See AU. Cyclo-oxygenase isoenzymes: physiological and pharmacological role. Anaesthesia. 2000;55:442–9.
Zhang X, Schwarz EM, Young DA, Puzas JE, Rosier RN, O’Keefe RJ. Cyclooxygenase-2 regulates mesenchymal cell differentiation into the osteoblast lineage and is critically involved in bone repair. J Clin Invest. 2002;109:1405–15.
Simon AM, O’Connor JP. Dose and time-dependent effects of cyclooxygenase-2 inhibition on fracture-healing. J Bone Joint Surg Am. 2007;89:500–11.
Brock TG. Regulating leukotriene synthesis: the role of nuclear 5-lipoxygenase. J Cell Biochem. 2005;96:1203–11.
Peters-Golden M, Henderson WR Jr. Leukotrienes. N Engl J Med. 2007;357:1841–54.
Peters-Golden M. Cell biology of the 5-lipoxygenase pathway. Am J Respir Crit Care Med. 1998;157:S227–31.
Lee JM, Park H, Noh AL, Kang JH, Chen L, Zheng T, Lee J, Ji SY, Jang CY, Shin CS, Ha H, Lee ZH, Park HY, Lee DS, Yim M. 5-Lipoxygenase mediates RANKL-induced osteoclast formation via the cysteinyl leukotriene receptor 1. J Immunol. 2012;189:5284–92.
Offenbacher S, Odle BM, Van Dike TE. Endotoxin mediated leukotriene release from bone culture. J Den Res. 1986;65:351.
Gallwitz WE, Mundy GR, Lee CH, Qiao M, Roodman GD, Raftery M, Gaskell SJ, Bonewald LF. 5-Lipoxygenase metabolites of arachidonic acid stimulate isolated osteoclasts to resorb calcified matrices. J Biol Chem. 1993;268:10087–94.
Garcia C, Boyce BF, Gilles J, Dallas M, Qiao M, Mundy GR, Bonewald LF. Leukotriene B4 stimulates osteoclastic bone resorption both in vitro and in vivo. J Bone Miner Res. 1996;11:1619–27.
Bonewald LF, Flynn M, Qiao M, Dallas MR, Mundy GR, Boyce BF. Mice lacking 5-lipoxygenase have increased cortical bone thickness. Adv Exp Med Biol. 1997;433:299–302.
Manigrasso MB, O’Connor JP. Accelerated fracture healing in mice lacking the 5-lipoxygenase gene. Acta Orthop. 2010;81:748–55.
Biguetti CC, Couto MCR, Silva ACR, Shindo JVTC, Rosa VM, Shinohara AL, Andreo JC, Duarte MAH, Wang Z, Brotto M, Matsumoto MA. New surgical model for bone-muscle injury reveals age and gender-related healing patterns in the 5 lipoxygenase (5LO) knockout mouse. Front Endocrinol. 2020;11:484.
Wixted JJ, Fanning PJ, Gaur T, O’Connell SL, Silva J, Mason-Savas A, Ayers DC, Stein GS, Lian JB. Enhanced fracture repair by leukotriene antagonism is characterized by increased chondrocyte proliferation and early bone formation: a novel role of the cysteinyl LT-1 receptor. J Cell Physiol. 2009;221:31–9.
Cottrell JA, Keshav V, Mitchell A, O’Connor JP. Local inhibition of 5-lipoxygenase enhances bone formation in a rat model. Bone Joint Res. 2013;2:41–50.
Simionato GB, da Silva ACR, Oliva AH, de Abreu Furquim EM, Couto MCR, Shinohara AL, Biguetti CC, Matsumoto MA. Lack of 5-lipoxygenase in intramembranous and endochondral 129Sv mice skeleton and intramembranous healing. Arch Oral Biol. 2021;131: 105266.
Mahmoud RH, Biguetti CC, Simionato GB, Custódio IC, Silva RBP, Duarte MAH, Faverani LP, Ervolino E, Fakhouri WD, Matsumoto MA. Alveolar socket healing in 5-lipoxygenase knockout aged female mice treated or not with high dose of zoledronic acid. Sci Rep. 2021;11:19535.
Bousquet J, Demoly P, Humbert M. Montelukast in guidelines and beyond. Adv Ther. 2009;26:575–87.
Krishnamoorthy M, Mohd Noor N, Mat Lazim N, Abdullah B. Efficacy of Montelukast in Allergic Rhinitis Treatment: A systematic review and meta-analysis. Drugs. 2020;80:1831–51.
Zheng C, Shi X. Cysteinyl leukotriene receptor 1 (cysLT1R) regulates osteoclast differentiation and bone resorption. Artif Cells Nanomed Biotechnol. 2018;46(sup3):S64–70.
Wei J, Chen S, Huang C, Guo W, Yang S, Feng B, Chu J. Antagonism of cysteinyl leukot-riene receptor 1 (cysLT1R) by montelukast regulates differentiation of MC3T3-E1 cells under overloaded mechanical environment. Biochem Biophys Res Commun. 2018;495:995–1001.
Sabbah W, Slade GD, Sanders AE, Bernabé E. Denture wearing and mortality risk in edentulous American adults: A propensity score analysis. J Dent. 2020;100: 103360.
Bhattacharyya S, Choudhury S, Datta P, Pal AK, Roy S, Chatterjee R, De R, Chakraborty A, Saha S, Chowdhury AR. Assessment of jaw bone quality for designing patient-specific dental implant using computed tomography data. J Long Term Eff Med Implants. 2021;31:49–58.
Scarano A, Bernardi S, Rastelli C, Mortellaro C, Vittorini P, Falisi G. Soft tissue augmentation by means of silicon expanders prior to bone volume increase: a case series. J Biol Regul Homeost Agents. 2019;33(6 Suppl. 2):77–84.
Bernardi S, Macchiarelli G, Bianchi S. Autologous materials in regenerative dentistry: harvested bone, platelet concentrates and dentin derivates. Molecules. 2020;25:5330.
Bianchi S, Mancini L, Torge D, Cristiano L, Mattei A, Varvara G, Macchiarelli G, Marchetti E, Bernardi S. Bio-morphological reaction of human periodontal ligament fibroblasts to different types of dentinal derivates in vitro study. Int J Mol Sci. 2021;22:8681.
Bianchi S, Bernardi S, Mattei A, Cristiano L, Mancini L, Torge D, Varvara G, Macchiarelli G, Marchetti E. Morphological and biological evaluations of human periodontal ligament fibroblasts in contact with different bovine bone grafts treated with low-temperature deproteinisation protocol. Int J Mol Sci. 2022;23:5273.
Bianchi S, Torge D, Rinaldi F, Piattelli M, Bernardi S, Varvara G. Platelets’ role in dentistry: from oral pathology to regenerative potential. Biomedicines. 2022;10:218.
Percie du Sert N, Ahluwalia A, Alam S, Avey MT, Baker M, Browne WJ, Clark A, Cuthill IC, Dirnagl U, Emerson M, Garner P, Holgate ST, Howells DW, Hurst V, Karp NA, Lazic SE, Lidster K, MacCallum CJ, Macleod M, Pearl EJ, Petersen OH, Rawle F, Reynolds P, Rooney K, Sena ES, Silberberg SD, Steckler T, Würbel H. Reporting animal research: Explanation and elaboration for the ARRIVE guidelines 20. PLoS Biol. 2020;18:e3000411.
Biguetti CC, Vieira AE, Cavalla F, Fonseca AC, Colavite PM, Silva RM, Trombone APF, Garlet GP. CCR2 contributes to F4/80+ cells migration along intramembranous bone healing in maxilla, but its deficiency does not critically affect the healing outcome. Front Immunol. 2018;9:1804.
Bouxsein ML, Boyd SK, Christiansen BA, Guldberg RE, Jepsen KJ, Müller R. Guidelines for assessment of bone microstructure in rodents using micro-computed tomography. J Bone Miner Res. 2010;25:1468–86.
Laidler PM, Taga EM, Van Etten RL. Human liver acid phosphatases: cysteine residues of the low-molecular-weight enzyme. Arch Biochem Biophys. 1982;216:512–21.
Chaves Neto AH, Machado D, Yano CL, Ferreira CV. Antioxidant defense and apoptotic effectors in ascorbic acid and β-glycerophosphate-induced osteoblastic differentiation. Dev Growth Differ. 2011;53:88–96.
Granjeiro JM, Taga EM, Aoyama H. Purification and characterization of a low-molecular-weight bovine kidney acid phosphatase. An Acad Bras Cienc. 1997;69(4):451–60.
Janckila AJ, Parthasarathy RN, Parthasarathy LK, Seelan RS, Hsueh YC, Rissanen J, Alatalo SL, Halleen JM, Yam LT. Properties and expression of human tartrate-resistant acid phosphatase isoform 5a by monocyte-derived cells. J Leukoc Biol. 2005;77:209–18.
Karmen A. A note on the spectrometric assay of glutamic-oxalacetic transaminase in human blood serum. J Clin Invest. 1955;34:131–3.
Henry RJ, Chiamorin N, Bolub OJ, Berkman S. Revised spectrophotometric methods for the determination of glutamic-oxalacetic transaminase, glutamic-pyruvic transaminase, and lactic acid dehydrogenase. Am J Clin Pathol. 1960;34:381–98.
Garcia C, Qiao M, Chen D, Kirchen M, Gallwitz W, Mundy GR, Bonewald LF. Effects of synthetic peptido-leukotrienes on bone resorption in vitro. J Bone Miner Res. 1996;11:521–9.
Traianedes K, Dallas MR, Garrett IR, Mundy GR, Bonewald LF. 5-Lipoxygenase metabolites inhibit bone formation in vitro. Endocrinology. 1998;139:3178–84.
Silva RCS, Agrelli A, Andrade AN, Mendes-Marques CL, Arruda IRS, Santos LRL, Vasconcelos NF, Machado G. Titanium dental implants: an overview of applied nanobiotechnology to improve biocompatibility and prevent infections. Materials. 2022;15:3150.
Barone A, Ricci M, Tonelli P, Santini S, Covani U. Tissue changes of extraction sockets in humans: a comparison of spontaneous healing vs. ridge preservation with secondary soft tissue healing. Clin Oral Implants Res. 2013;24:1231–7.
Shuto T, Sarkar G, Bronk JT, Matsui N, Bolander ME. Osteoblasts express types I and II activin receptors during early intramembranous and endochondral bone formation. J Bone Miner Res. 1997;12:403–11.
Denzlinger C, Rapp S, Hagmann W, Keppler D. Leukotrienes as mediators in tissue trauma. Science. 1985;230:330–2.
Akino K, Mineda T, Mori N, Hirano A, Imaizumi T, Akita S. Attenuation of cysteinyl leukotrienes induces human mesenchymal stem cell differentiation. Wound Repair Regen. 2006;14:343–9.
Kang JH, Lim H, Lee DS, Yim M. Montelukast inhibits RANKL-induced osteoclast formation and bone loss via CysLTR1 and P2Y12. Mol Med Rep. 2018;18:2387–98.
Tintinger GR, Feldman C, Theron AJ, Anderson R. Montelukast: more than a cysteinyl leukotriene receptor antagonist? Sci World J. 2010;10:2403–13.
Perwad F, Azam N, Zhang MY, Yamashita T, Tenenhouse HS, Portale AA. Dietary and serum phosphorus regulate fibroblast growth factor 23 expression and 1,25-dihydroxyvitamin D metabolism in mice. Endocrinology. 2005;146:5358–64.
Lieben L, Masuyama R, Torrekens S, Van Looveren R, Schrooten J, Baatsen P, Lafage-Proust MH, Dresselaers T, Feng JQ, Bonewald LF, Meyer MB, Pike JW, Bouillon R, Carmeliet G. Normocalcemia is maintained in mice under conditions of calcium malabsorption by vitamin D-induced inhibition of bone mineralization. J Clin Invest. 2012;122:1803–15.
Härle D, Rådmark O, Samuelsson B, Steinhilber D. Calcitriol and transforming growth factor-beta upregulate 5-lipoxygenase mRNA expression by increasing gene transcription and mRNA maturation. Eur J Biochem. 1998;254:275–81.
Seuter S, Väisänen S, Rådmark O, Carlberg C, Steinhilber D. Functional characterization of vitamin D responding regions in the human 5-Lipoxygenase gene. Biochim Biophys Acta. 2007;1771:864–72.
Stelmach I, Olszowiec-Chlebna M, Jerzynska J, Grzelewski T, Stelmach W, Majak P. Inhaled corticosteroids may have a beneficial effect on bone metabolism in newly diagnosed asthmatic children. Pulm Pharmacol Ther. 2011;24:414–20.
Everts V, de Vries TJ, Helfrich MH. Osteoclast heterogeneity: lessons from osteopetrosis and inflammatory conditions. Biochim Biophys Acta. 2009;1792:757–65.
Currie GP, Srivastava P, Dempsey OJ, Lee DK. Therapeutic modulation of allergic airways disease with leukotriene receptor antagonists. QJM. 2005;98:171–82.
Clarridge K, Chin S, Eworuke E, Seymour S. A Boxed Warning for Montelukast: The FDA Perspective. J Allergy Clin Immunol Pract. 2021;9:2638–41.
Incecik F, Onlen Y, Sangun O, Akoglu S. Probable montelukast-induced hepatotoxicity in a pediatric patient: case report. Ann Saudi Med. 2007;27:462–3.
Calapai G, Casciaro M, Miroddi M, Calapai F, Navarra M, Gangemi S. Montelukast-induced adverse drug reactions: a review of case reports in the literature. Pharmacology. 2014;94:60–70.
Lebensztejn DM, Bobrus-Chociej A, Kłusek M, Uscinowicz M, Lotowska J, Sobaniec-Lotowska M, Kaczmarski M. Hepatotoxicity caused by montelukast in a paediatric patient. Prz Gastroenterol. 2014;9:121–3.
El-Boghdady NA, Abdeltawab NF, Nooh MM. Resveratrol and Montelukast alleviate paraquat-induced hepatic injury in mice: modulation of oxidative stress, inflammation, and apoptosis. Oxid Med Cell Longev. 2017;2017:9396425.
Pu S, Liu Q, Li Y, Li R, Wu T, Zhang Z, Huang C, Yang X, He J. Montelukast prevents mice against acetaminophen-induced liver injury. Front Pharmacol. 2019;10:1070.
El-Kashef DH, Zaghloul RA. Ameliorative effect of montelukast against carbon tetrachloride-induced hepatotoxicity: Targeting NLRP3 inflammasome pathway. Life Sci. 2022;304: 120707.
Acknowledgements
KHCR was supported by Fundação de Amparo à Pesquisa do Estado do Amazonas (Grant #42338.63998.1205.2019). MAM was supported by Fundação de Amparo à Pesquisa do Estado de São Paulo (Grant #2019/16067-3).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by KHCR, RB ParraS, ACBR, AJMB, ACZB, EE, MAHD, WDF, AHCN, CCB, MAM. The first draft of the manuscript was written by CCB and MAM and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ribeiro, K.H.C., da Silva, R.B.P., Roseno, A.C.B. et al. Dose–response effect of Montelukast on post-extraction dental socket repair and skeletal phenotype of mice. Odontology 111, 891–903 (2023). https://doi.org/10.1007/s10266-023-00800-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10266-023-00800-5