Abstract
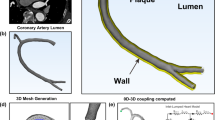
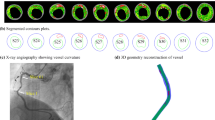
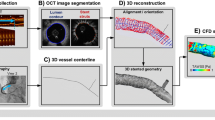
Plaque rupture is related to the mechanical stress it suffered. The value and distribution of the mechanical stress in plaque could help on assessing plaque vulnerability. To look into the stress conditions in the coronary artery, a patient-specific coronary model was created by using optical coherence tomography (OCT) and angiography imaging data. The reconstructed coronary model consisted of the structure of the lumen, the arterial wall and plaque components. Benefited by the high resolution of OCT, detailed structures such as the thin fibrous cap could be observed and built into the geometry. On this reconstructed coronary model, a fully coupled fluid–structure interaction (FSI) simulation was performed. The principle stress in coronary plaque and the wall shear stress (WSS) were analyzed. The FSI simulation results show that the cap thickness had a significant effect on the stress, and the principle stress at the thin cap area was more than double of those at the locations with a larger thickness. WSS is thought as an important parameter to assess the potentially dangerous areas of the atherosclerosis-prone (caused by low WSS) and the plaque rupture (high WSS). From the WSS plots of our FSI model, the area with abnormal WSS value was detected around the position where a lipid core existed. The FSI simulation results were compared with the results from the conventional structure-only and the computational fluid dynamics (CFD)-only computational models to quantify the difference between the three models. We found little difference in the principle stress results between the FSI and the structure-only model, but a significant difference between the FSI and the CFD-only model when looking into the WSS. The WSS values at the two observation spots from the CFD-only model were higher than the values from the FSI model by 17.95% and 22.66% in average, respectively. Furthermore, the FSI model detected more areas of low WSS, because the fluid domain could expand circumferentially when pressure loaded on the flexible arterial. This study suggests that OCT-based FSI model may be useful for plaque vulnerability assessment and it may be critical to perform the FSI simulation if an accurate WSS value is required.










Similar content being viewed by others
References
Augst AD et al (2003) Accuracy and reproducibility of CFD predicted wall shear stress using 3D ultrasound images. J Biomech Eng 125(2):218. https://doi.org/10.1115/1.1553973
Auricchio F et al (2014) A simple framework to generate 3D patient-specific model of coronary artery bifurcation from single-plane angiographic images. Comput Biol Med 44(1):97–109. https://doi.org/10.1016/j.compbiomed.2013.10.027
Australian Institute of Health and Welfare (2018) Australia’ s health 2018: in brief. https://doi.org/10.1145/3173574.3174019
Benjamin EJ et al (2018) Heart disease and stroke statistics—2018 update: a report from the American Heart Association, Circulation. https://doi.org/10.1161/cir.0000000000000558
Bourantas CV et al (2005) A method for 3D reconstruction of coronary arteries using biplane angiography and intravascular ultrasound images. Comput Med Imaging Graph 29(8):597–606. https://doi.org/10.1016/j.compmedimag.2005.07.001
Chimakurthi SK et al (2018) ANSYS workbench system coupling: a state-of-the-art computational framework for analyzing multiphysics problems. Eng Comput 34(2):385–411. https://doi.org/10.1007/s00366-017-0548-4
Dolan JM, Kolega J, Meng H (2013) High wall shear stress and spatial gradients in vascular pathology: a review. Ann Biomed Eng 41(7):1411–1427. https://doi.org/10.1007/s10439-012-0695-0
Dong J, Wong KKL, Tu J (2013) Hemodynamics analysis of patient-specific carotid bifurcation: a CFD model of downstream peripheral vascular impedance. Int J Numer Methods Biomed Eng 29(4):476–491. https://doi.org/10.1002/cnm.2529
Dong J et al (2015) Fluid–structure interaction analysis of the left coronary artery with variable angulation. Comput Methods Biomech Biomed Eng. https://doi.org/10.1080/10255842.2014.921682
Doulaverakis C et al (2013) IVUSAngio tool: a publicly available software for fast and accurate 3D reconstruction of coronary arteries. Comput Biol Med 43(11):1793–1803. https://doi.org/10.1016/j.compbiomed.2013.08.013
Ellwein LM et al (2011) Optical coherence tomography for patient-specific 3D artery reconstruction and evaluation of wall shear stress in a left circumflex coronary artery. Cardiovasc Eng Technol 2(3):212–227. https://doi.org/10.1007/s13239-011-0047-5
Escolar E et al (2006) New imaging techniques for diagnosing coronary artery disease. CMAJ: Can Med Assoc J 174(4):487–495. https://doi.org/10.1503/cmaj.050925
Eshtehardi P et al (2017) ‘High wall shear stress and high-risk plaque: an emerging concept. Int J Cardiovasc Imaging 33(7):1089–1099. https://doi.org/10.1007/s10554-016-1055-1
Gao H et al (2009a) Carotid arterial plaque stress analysis using fluid-structure interactive simulation based on in vivo magnetic resonance images of four patients. J Biomech 42(10):1416–1423. https://doi.org/10.1016/j.jbiomech.2009.04.010
Gao H et al (2009b) Study of reproducibility of human arterial plaque reconstruction and its effects on stress analysis based on multispectral in vivo magnetic resonance imaging. J Magn Reson Imaging 30(1):85–93. https://doi.org/10.1002/jmri.21799
Garcìa-Garcìa HM et al (2011) IVUS-based imaging modalities for tissue characterization: similarities and differences. Int J Cardiovasc Imaging 27(2):215–224. https://doi.org/10.1007/s10554-010-9789-7
Garreau M et al (1991) A knowledge-based approach for 3-D reconstruction and labeling of vascular networks from biplane angiographic projections. IEEE Trans Med Imaging 10(2):122–131. https://doi.org/10.1109/42.79469
Gholipour A et al (2018) Three-dimensional biomechanics of coronary arteriesx. Three Dimens Biomechan Coron Arter 130:93–114. https://doi.org/10.1016/j.ijengsci.2018.03.002
Guggenheim N et al (1991) Spatial reconstruction of coronary arteries from angiographic images. Phys Med Biol 36(1):99–110. https://doi.org/10.1088/0031-9155/36/1/009
Guo X et al (2017) Combining IVUS and optical coherence tomography for more accurate coronary cap thickness quantification and stress/strain calculations: a patient-specific three-dimensional fluid-structure interaction modeling approach. J Biomech Eng 140(April):1–12. https://doi.org/10.1115/1.4038263
Huang X et al (2009) Patient-specific artery shrinkage and 3D zero-stress state in multi-component 3D FSI models for carotid atherosclerotic plaques based on in vivo MRI data NIH public access. Mol Cell Biomech 6(2):121–134. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2681261/pdf/nihms89307.pdf
Huang X et al (2016) 3D MRI-based multicomponent thin layer structure only plaque models for atherosclerotic plaques. J Biomechan 49(13):2726–2733. https://doi.org/10.1016/j.jbiomech.2016.06.002
Insull W (2009) The pathology of atherosclerosis: plaque development and plaque responses to medical treatment. Am J Med 122(1):S3–S14. https://doi.org/10.1016/j.amjmed.2008.10.013
Kousera CA et al (2014) Patient-specific coronary stenoses can be modeled using a combination of OCT and flow velocities to accurately predict hyperemic pressure gradients. IEEE Trans Biomed Eng 61(6):1902–1913. https://doi.org/10.1109/TBME.2014.2310954
Kwak BR et al (2014) Biomechanical factors in atherosclerosis: mechanisms and clinical implications. Eur Heart J 35(43):3013–3020. https://doi.org/10.1093/eurheartj/ehu353
Laban M et al (2004) ANGUS: a new approach to three-dimensional reconstruction of coronary vessels by combined use of angiography and intravascular ultrasound. In: Computers in cardiology 1995. IEEE, pp 325–328. https://doi.org/10.1109/cic.1995.482638
Li ZY et al (2006) Stress analysis of carotid plaque rupture based on in vivo high resolution MRI. J Biomech 39(14):2611–2622. https://doi.org/10.1016/j.jbiomech.2005.08.022
Li ZY et al (2007) Structural analysis and magnetic resonance imaging predict plaque vulnerability: a study comparing symptomatic and asymptomatic individuals. J Vasc Surg 45(4):768–775. https://doi.org/10.1016/j.jvs.2006.12.065
Liu B, Tang D (2011) Influence of non-Newtonian properties of blood on the wall shear stress in human atherosclerotic right coronary arteries. Mol Cell Biomech 8(1):73–90. https://doi.org/10.3970/mcb.2011.008.073
Long Q et al (2000) Reconstruction of blood flow patterns in a human carotid bifurcation: a combined CFD and MRI study. J Magn Reson Imaging 11(3):299–311. https://doi.org/10.1002/(SICI)1522-2586(200003)11:3%3c299:AID-JMRI9%3e3.0.CO;2-M
Lowe HC et al (2011) Intracoronary optical diagnostics: current status, limitations, and potential. JACC Cardiovasc Interv 4(12):1257–1270. https://doi.org/10.1016/j.jcin.2011.08.015
Malek AM (1999) Hemodynamic shear stress and its role in atherosclerosis. JAMA 282(21):2035. https://doi.org/10.1001/jama.282.21.2035
Mehta LS et al (2016) Acute myocardial infarction in women : a scientific statement from the American Heart Association. Circulation. https://doi.org/10.1161/cir.0000000000000351
Messenger JC et al (2000) 3D coronary reconstruction from routine single-plane coronary angiograms: clinical validation and quantitative analysis of the right coronary artery in 100 patients. Int J Card Imaging 16(6):413–427. https://doi.org/10.1023/A:1010643426720
Naghavi M et al (2003) From vulnerable plaque to vulnerable patient: a call for new definitions and risk assessment strategies: part I. Circulation 108(15):1772–1778. https://doi.org/10.1161/01.cir.0000087481.55887.c9
Paritala PK et al (2018) Numerical investigation of atherosclerotic plaque rupture using optical coherence tomography imaging and XFEM. Eng Fract Mech 204:531–541. https://doi.org/10.1016/j.engfracmech.2018.11.002
Prati F et al (2010) Expert review document on methodology, terminology, and clinical applications of optical coherence tomography: physical principles, methodology of image acquisition, and clinical application for assessment of coronary arteries and atherosclerosis. Eur Heart J 31(4):401–415. https://doi.org/10.1093/eurheartj/ehp433
Regar E et al (2003) Optical coherence tomography. Cardiovasc Radiat Med 4(4):198–204. https://doi.org/10.1016/j.carrad.2003.12.003
Tang D et al (2004) Effect of a lipid pool on stress/strain distributions in stenotic arteries: 3-D fluid-structure interactions (FSI) models. J Biomech Eng 126(3):363. https://doi.org/10.1115/1.1762898
Tang D et al (2005) Quantifying effects of plaque structure and material properties on stress distributions in human atherosclerotic plaques using 3D FSI models. J Biomech Eng 127(7):1185. https://doi.org/10.1115/1.2073668
Townsend N et al (2016) Cardiovascular disease in Europe: epidemiological update 2016. Eur Heart J 37(42):3232–3245. https://doi.org/10.1093/eurheartj/ehw334
Vancraeynest D et al (2011) Imaging the vulnerable plaque. J Am Coll Cardiol 57(20):1961–1979. https://doi.org/10.1016/j.jacc.2011.02.018
Wang L et al (2015) Morphological and stress vulnerability indices for human coronary plaques and their correlations with cap thickness and lipid percent: an IVUS-Based fluid-structure interaction multi-patient study. PLoS Comput Biol 11(12):1–15. https://doi.org/10.1371/journal.pcbi.1004652
Zhu C et al (2010) Normalized wall index specific and MRI-based stress analysis of atherosclerotic carotid plaques. Circ J 74(11):2360–2364. https://doi.org/10.1253/circj.CJ-10-0305
Acknowledgements
Computational resources and services used in this work were provided by the HPC and Research Support Group, Queensland University of Technology, Brisbane, Australia.
Funding
This work was supported in part by the National Natural Science Foundation of China (NSFC) (Grant Nos. 11772093, 61821002), Australian Research Council (ARC) (FT140101152, DP180103009), and the Prince Charles Hospital Foundation (NI2019-19).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethics
The QUT University Human Research Ethics Committee assessed this research as meeting the conditions for exemption from HREC review and approval in accordance with section 5.1.22 of the National Statement on Ethical Conduct in Human Research (2007).
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Wang, J., Paritala, P.K., Mendieta, J.B. et al. Optical coherence tomography-based patient-specific coronary artery reconstruction and fluid–structure interaction simulation. Biomech Model Mechanobiol 19, 7–20 (2020). https://doi.org/10.1007/s10237-019-01191-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10237-019-01191-9