Abstract
Background
Renal blood flow (RBF) decreases with exercise, but this change is only temporary, and habitual exercise may be an effective method to improve renal function. The kidney shows structural and functional changes with aging, but it is unclear how aging affects the hemodynamic response of the kidneys to exercise. Therefore, we evaluated the differences in the hemodynamic response of the kidneys to high-intensity exercise between younger and older men.
Methods
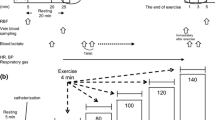
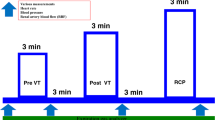
Sixteen men (8 young and 8 older) underwent an incremental exercise test using a cycle ergometer with a 1-min warm up followed by exercise at 10–20 W/min until the discontinuation criteria were met. Renal hemodynamics were assessed before exercise, immediately after exercise, and at 60-min after exercise using ultrasound echo.
Results
High-intensity exercise significantly reduced RBF in both groups (younger: ∆ – 53 ± 16%, p = 0.0005; older: ∆ – 53 ± 19%, p = 0.0004). In the younger group, RBF returned to the pre-exercise level 60-min after exercise (∆ – 0.4 ± 5.7%, p > 0.9999). In contrast, RBF 60-min after exercise was significantly lower than that before exercise in the older group (∆ – 24 ± 19%, p = 0.0006). The older group had significantly lower RBF than younger adults 60-min after exercise (423 ± 32 vs. 301 ± 98 mL/min, p = 0.0283).
Conclusions
Our findings demonstrate that RBF following high-intensity exercise recovered 60-min after exercise in younger group, whereas RBF recovery was delayed in the older group.





Similar content being viewed by others
References
Poortmans JR, Mathieu N, de Plaen P. Influence of running different distances on renal glomerular and tubular impairment in humans. Eur J Appl Physiol Occup Physiol. 1996;72:522–7.
Grimby G. Renal clearances during prolonged supine exercise at different loads. J Appl Physiol. 1965;20:1294–8.
Ene-Iordache B, Perico N, Bikbov B, Carminati S, Remuzzi A, Perna A, et al. Chronic kidney disease and cardiovascular risk in six regions of the world (ISN-KDDC): a cross-sectional study. Lancet Glob Health. 2016;4:e307–19.
Juett LA, James LJ, Mears SA. Effects of exercise on acute kidney injury biomarkers and the potential influence of fluid intake. Ann Nutr Metab. 2020;76:53–9.
Sehl ME, Yates FE. Kinetics of human aging: I. Rates of senescence between ages 30 and 70 years in healthy people. J Gerontol A Biol Sci Med Sci. 2001;56:B198–208.
Rule AD, Amer H, Cornell LD, Taler SJ, Cosio FG, Kremers WK, et al. The association between age and nephrosclerosis on renal biopsy among healthy adults. Ann Intern Med. 2010;152:561–7.
Poortmans JR, Ouchinsky M. Glomerular filtration rate and albumin excretion after maximal exercise in aging sedentary and active men. J Gerontol A Biol Sci Med Sci. 2006;61:1181–5.
Davies DF, Shock NW. Age changes in glomerular filtration rate, effective renal plasma flow, and tubular excretory capacity in adult males. J Clin Invest. 1950;29:496–507.
Berg UB. Differences in decline in GFR with age between males and females. Reference data on clearances of inulin and PAH in potential kidney donors. Nephrol Dial Transplant. 2006;21:2577–82.
Kenney WL, Zappe DH. Effect of age on renal blood flow during exercise. Aging Clin Exp Res. 1994;6:293–302.
Suzuki M, Ishiyama I, Seino T. Age-associated changes in renal function after exhaustive exercise in healthy males ranging in age from 8–80 years old. Adv Exerc Sport Physiol. 2006;12:65–72.
Castenfors J. Renal clearances and urinary sodium and potassium excretion during supine exercise in normal subjects. Acta Physiol Scand. 1967;70:207–14.
Kawakami S, Yasuno T, Matsuda T, Fujimi K, Ito A, Yoshimura S, et al. Association between exercise intensity and renal blood flow evaluated using ultrasound echo. Clin Exp Nephrol. 2018;22:1061–8.
Kotoku K, Yasuno T, Kawakami S, Fujimi K, Matsuda T, Nakashima S, et al. Effect of exercise intensity on renal blood flow in patients with chronic kidney disease stage 2. Clin Exp Nephrol. 2019;23:621–8.
Kawakami S, Yasuno T, Kawakami S, Ito A, Fujimi K, Matsuda T, et al. The moderate-intensity continuous exercise maintains renal blood flow and does not impair the renal function. Physiol Rep. 2022;10: e15420.
Liguori G, Feito Y, Fountaine C, Roy B. ACSM’s guidelines for exercise testing and prescription. 11th ed. Philadelphia: Lippincott Williams & Wilkins; 2021.
Arbeille PH, Roncin A, Berson M, Patat F, Pourcelot L. Exploration of the fetal cerebral blood flow by duplex doppler—linear array system in normal and pathological pregnancies. Ultrasound Med Biol. 1987;13:329–37.
Gosling RG, Dunbar G, King DH, Newman DL, Side CD, Woodcock JP, et al. The Quantitative analysis of occlusive peripheral arterial disease by a non-intrusive ultrasonic technique. Angiology. 1971;22:52–5.
Hiraki K, Otobe Y, Izawa KP, Sakurada T, Shibagaki Y. Physical activity in patients with pre-dialysis chronic kidney disease is associated with decreased renal function. Clin Exp Nephrol. 2021;25:683–4.
Suzuki M, Sudoh M, Matsubara S, Kawakami K, Shiota M, Ikawa S. Changes in renal blood flow measured by radionuclide angiography following exhausting exercise in humans. Eur J Appl Physiol Occup Physiol. 1996;74:1–7.
Hollenberg NK, Adams DF, Solomon HS, Rashid A, Abrams HL, Merrill JP. Senescence and the renal vasculature in normal man. Circ Res. 1974;34:309–16.
Ungvari Z, Tarantini S, Kiss T, Wren JD, Giles CB, Griffin CT, et al. Endothelial dysfunction and angiogenesis impairment in the ageing vasculature. Nat Rev Cardiol. 2018;15:555–65.
Reckelhoff JF, Kellum JA, Blanchard EJ, Bacon EE, Wesley AJ, Kruckeberg WC. Changes in nitric oxide precursor, L-arginine, and metabolites, nitrate and nitrite, with aging. Life Sci. 1994;55:1895–902.
Graf H, Stummvoll H, Luger A, Prager R. Effect of amino acid infusion on glomerular filtration rate. N Engl J Med. 1983;308:159–60.
ter Wee PM, Rosman JB, van der Geest S, Sluiter WJ, Donker AJM. Renal hemodynamics during separate and combined infusion of amino acids and dopamine. Kidney Int. 1986;29:870–4.
Fliser D, Zeier M, Nowack R, Ritz E. Renal functional reserve in healthy elderly subjects. J Am Soc Nephrol. 1993;3:1371–7.
Bude RO, Rubin JM. Relationship between the resistive index and vascular compliance and resistance. Radiology. 1999;211:411–7.
Di Nicolò P, Granata A. Renal resistive index: not only kidney. Clin Exp Nephrol. 2017;21:359–66.
Halimi J-M, Vernier L-M, Gueguen J, Goin N, Gatault P, Sautenet B, et al. End-diastolic velocity mediates the relationship between renal resistive index and the risk of death. J Hypertens. 2023;41:27–34.
Acknowledgements
The authors acknowledge the contribution of the staff at Fukuoka University, who helped with the recruitment of participants. The authors thank the volunteers who participated in this study.
Funding
This work was supported by Japan Society for the Promotion of Science (JSPS) (Grant numbers: 22K11489 to S. K., and 15H03082 to Y.H.) and Fukuoka University Institute for Physical Activity, Fukuoka, Japan.
Author information
Authors and Affiliations
Contributions
SK, TY, KK, SK, and AI performed experiments; SK analyzed data; SK, TY, KK, YH, and RM. interpreted results of experiments; SK prepared figures; SK Writing – original draft; SK, TY, KK, SK, AI, KF, TM, SN, KM, YU, YH, and RM Writing – review and editing; SK, TY, KK, SK, AI, KF, TM, SN, KM, YU, YH, and RM approved final version of manuscript and SK, TY, YH, and RM conceived and designed research.
Corresponding author
Ethics declarations
Conflict of interest
No conflicts of interest, financial or otherwise, are declared by the authors.
Ethical approval
The study protocol in this study complied with the Declaration of Helsinki and the principles of Good Clinical Practice and was approved by the Ethics Committee of Fukuoka University (21-07-M1, 16-4-01).
Informed consent
All potential risks and procedures were explained to the participants, who provided written informed consent in this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Kawakami, S., Yasuno, T., Kotoku, K. et al. The differences in renal hemodynamic response following high-intensity exercise between younger and older males. Clin Exp Nephrol 27, 972–980 (2023). https://doi.org/10.1007/s10157-023-02381-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10157-023-02381-7