Abstract
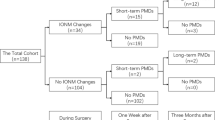
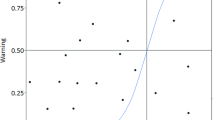
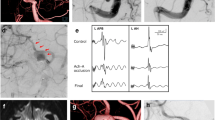
To explore the relationship between postoperative motor deficits and the duration of reduced motor-evoked potentials (MEPs) in patients with middle cerebral artery (MCA) aneurysm. This study included 285 cases of MCA aneurysm treated with clipping surgery with MEP monitoring. The effects of MEP changes on postoperative motor function were assessed, and the key time point for minimizing the incidence of postoperative motor dysfunction was found through receiver operating characteristic (ROC) curve analysis. Motor dysfunction was significantly associated with the occurrence of MEP changes, and patients with irreversible changes were more likely to suffer motor dysfunction than were those with reversible changes. The critical duration of MEP changes that minimized the risk of postoperative motor dysfunction was 8.5 min. This study revealed that MEP monitoring is an effective method for preventing ischemic brain injury during surgical treatment of MCA aneurysm and proposes a critical cutoff for the duration of MEP deterioration of 8.5 min for predicting postoperative motor dysfunction.

Similar content being viewed by others
References
Brisman JL, Song JK, Newell DW (2006) Cerebral aneurysms. N Engl J Med 355:928–939. https://doi.org/10.1056/NEJMra052760
Chalouhi N, Hoh BL, Hasan D (2013) Review of cerebral aneurysm formation, growth, and rupture. Stroke 44:3613–3622. https://doi.org/10.1161/STROKEAHA.113.002390
Choi HH, Ha EJ, Cho WS, Kang HS, Kim JE (2017) Effectiveness and limitations of intraoperative monitoring with combined motor and somatosensory evoked potentials during surgical clipping of unruptured intracranial aneurysms. World neurosurgery 108:738–747. https://doi.org/10.1016/j.wneu.2017.09.096
Guo L, Gelb AW (2011) The use of motor evoked potential monitoring during cerebral aneurysm surgery to predict pure motor deficits due to subcortical ischemia. Clin Neurophysiol 122:648–655. https://doi.org/10.1016/j.clinph.2010.09.001
Horiuchi K, Suzuki K, Sasaki T, Matsumoto M, Sakuma J, Konno Y, Oinuma M, Itakura T, Kodama N (2005) Intraoperative monitoring of blood flow insufficiency during surgery of middle cerebral artery aneurysms. J Neurosurg 103:275–283. https://doi.org/10.3171/jns.2005.103.2.0275
Hwang JS, Hyun MK, Lee HJ, Choi JE, Kim JH, Lee NR, Kwon JW, Lee E (2012) Endovascular coiling versus neurosurgical clipping in patients with unruptured intracranial aneurysm: a systematic review. BMC Neurol 12:99. https://doi.org/10.1186/1471-2377-12-99
Jones TH, Morawetz RB, Crowell RM, Marcoux FW, FitzGibbon SJ, DeGirolami U, Ojemann RG (1981) Thresholds of focal cerebral ischemia in awake monkeys. J Neurosurg 54:773–782. https://doi.org/10.3171/jns.1981.54.6.0773
Li H, Pan R, Wang H, Rong X, Yin Z, Milgrom DP, Shi X, Tang Y, Peng Y (2013) Clipping versus coiling for ruptured intracranial aneurysms: a systematic review and meta-analysis. Stroke 44:29–37. https://doi.org/10.1161/STROKEAHA.112.663559
Li Z, Fan X, Wang M, Tao X, Qi L, Ling M, Guo D, Qiao H (2019) Prediction of postoperative motor deficits using motor evoked potential deterioration duration in intracranial aneurysm surgery. Clinical neurophysiology : official journal of the International Federation of Clinical Neurophysiology 130:707–713. https://doi.org/10.1016/j.clinph.2019.02.010
Lindgren A, Vergouwen MD, van der Schaaf I, Algra A, Wermer M, Clarke MJ, Rinkel GJ (2018) Endovascular coiling versus neurosurgical clipping for people with aneurysmal subarachnoid haemorrhage. Cochrane Database System Rev 8:CD003085. https://doi.org/10.1002/14651858.CD003085.pub3
Malcharek MJ, Hesse J, Hesselbarth K, Thoma K, Wegner C, Sablotzki A, Hennig G, Gille J (2019) Warning criteria for MEP monitoring during carotid endarterectomy: a retrospective study of 571 patients. J Clin Monit Comput:1–7. https://doi.org/10.1007/s10877-019-00345-5
Suzuki K, Kodama N, Sasaki T, Matsumoto M, Konno Y, Sakuma J, Oinuma M, Murakawa M (2003) Intraoperative monitoring of blood flow insufficiency in the anterior choroidal artery during aneurysm surgery. J Neurosurg 98:507–514. https://doi.org/10.3171/jns.2003.98.3.0507
Szelenyi A, Langer D, Kothbauer K, De Camargo AB, Flamm ES, Deletis V (2006) Monitoring of muscle motor evoked potentials during cerebral aneurysm surgery: intraoperative changes and postoperative outcome. J Neurosurg 105:675–681. https://doi.org/10.3171/jns.2006.105.5.675
Thirumala PD, Crammond DJ, Loke YK, Cheng HL, Huang J, Balzer JR (2017) Diagnostic accuracy of motor evoked potentials to detect neurological deficit during idiopathic scoliosis correction: a systematic review. J Neurosurg Spine 26:374–383. https://doi.org/10.3171/2015.7.SPINE15466
Thomas B, Guo D (2017) The diagnostic accuracy of evoked potential monitoring techniques during intracranial aneurysm surgery for predicting postoperative ischemic damage: a systematic review and meta-analysis. World Neurosurg 103(829–840):e823. https://doi.org/10.1016/j.wneu.2017.04.071
Funding
This work was supported by Capital Foundation of Medical Developments, grant number 2018-2-1075, Principle Investigator: Professor Hui Qiao.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethical approval
The current study was approved by the ethical committee of our hospital.
Informed consent
Informed consent was obtained for all enrolled patients.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Dongze Guo and Xing Fan are co-first authors.
Rights and permissions
About this article
Cite this article
Guo, D., Fan, X., You, H. et al. Prediction of postoperative motor deficits using intraoperative motor-evoked potentials in middle cerebral artery aneurysm. Neurosurg Rev 44, 495–501 (2021). https://doi.org/10.1007/s10143-020-01235-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10143-020-01235-0