Abstract
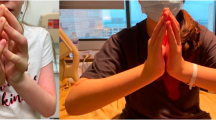
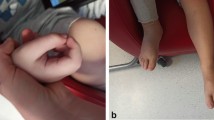
Eosinophilic fasciitis (EF) is a rare connective tissue disease that causes inflammation and fibrosis of the fascia, inducing pain and motor dysfunction. Characteristic skin manifestations, such as edema, erythema, induration, peau d’orange appearance, and the groove sign, are of diagnostic significance and observed in the majority of patients with EF. We herein report a case of EF without these characteristic skin manifestations. A 66-year-old Japanese woman developed progressive limb pain and motor dysfunction. No skin changes were observed. We diagnosed the patient with EF based on the clinical course, magnetic resonance imaging, and en bloc biopsy containing fascia and muscle. Oral prednisolone therapy markedly attenuated limb pain and motor dysfunctions. Through a systemic search of the medical literature, we retrieved 4 juvenile cases and 8 adult cases of EF without characteristic skin manifestations during the clinical course. We herein present a systemic review on EF without skin manifestations and discuss differences between the two proposed sets of diagnostic criteria of EF.



Similar content being viewed by others
Data availability
The datasets obtained and/or analyzed during the current study available from the corresponding author on reasonable request.
References
Shulman LE (1984) Diffuse fasciitis with hypergammaglobulinemia and eosinophilia: a new syndrome? J Rheumatol 11(5):569–570
Fett N, Arthur M (2018) Eosinophilic fasciitis: current concepts. Clin Dermatol 36(4):487–497. https://doi.org/10.1016/j.clindermatol.2018.04.006
Mango RL, Bugdayli K, Crowson CS, Drage LA, Wetter DA, Lehman JS, Peters MS, Davis MD, Chowdhary VR (2020) Baseline characteristics and long-term outcomes of eosinophilic fasciitis in 89 patients seen at a single center over 20 years. Int J Rheum Dis 23(2):233–239. https://doi.org/10.1111/1756-185X.13770
Lakhanpal S, Ginsburg WW, Michet CJ, Doyle JA, Moore SB (1988) Eosinophilic fasciitis: clinical spectrum and therapeutic response in 52 cases. Semin Arthritis Rheum 17(4):221–231. https://doi.org/10.1016/0049-0172(88)90008-x
Wright NA, Mazori DR, Patel M, Merola JF, Femia AN, Vleugels RA (2016) Epidemiology and treatment of eosinophilic fasciitis: an analysis of 63 patients from 3 tertiary care centers. JAMA Dermatol 152(1):97–99. https://doi.org/10.1001/jamadermatol.2015.3648
Mazori DR, Femia AN, Vleugels RA (2017) Eosinophilic fasciitis: an updated review on diagnosis and treatment. Curr Rheumatol Rep 19(12):74. https://doi.org/10.1007/s11926-017-0700-6
Kurimoto R, Ikeda K, Nakagomi D, Nakajima H (2016) Eosinophilic fasciitis illustrated by [(18)F] FDG-PET/CT. Intern Med (Tokyo, Japan) 55(16):2321–2322. https://doi.org/10.2169/internalmedicine.55.6937
Suzuki S, Noda K, Ohira Y, Shikino K, Ikusaka M (2015) Finger stiffness or edema as presenting symptoms of eosinophilic fasciitis. Rheumatol Int 35(10):1769–1772. https://doi.org/10.1007/s00296-015-3338-6
Thönnes S, Sorg H, Hauser J, Tilkorn DJ (2017) Localized eosinophilic fasciitis (Shulman’s disease) as a differential diagnosis of nerve compression syndrome. Innov Surg Sci 2(1):23–25. https://doi.org/10.1515/iss-2016-0203
Pillen S, van Engelen B, van den Hoogen F, Fiselier T, van der Vossen P, Drost G (2006) Eosinophilic fasciitis in a child mimicking a myopathy. Neuromuscul Disord 16(2):144–148. https://doi.org/10.1016/j.nmd.2005.12.001
Huppke P, Wilken B, Brockmann K, Sattler B, Hanefeld F (2002) Eosinophilic fasciitis leading to painless contractures. Eur J Pediatr 161(10):528–530. https://doi.org/10.1007/s00431-002-1038-1
Papa R, Nozza P, Granata C, Caorsi R, Gattorno M, Martini A, Picco P (2016) Juvenile eosinophilic fasciitis: three case reports with review of the literature. Clin Exp Rheumatol 34(3):527–530
Lebeaux D, Francès C, Barete S, Wechsler B, Dubourg O, Renoux J, Maisonobe T, Benveniste O, Gatfossé M, Bourgeois P, Amoura Z, Cacoub P, Piette JC, Sène D (2012) Eosinophilic fasciitis (Shulman disease): new insights into the therapeutic management from a series of 34 patients. Rheumatology (Oxford, England) 51(3):557–561. https://doi.org/10.1093/rheumatology/ker366
Tsoi KL, Custers M, Bij de Vaate L, Jacobs JW (2012) Eosinophilic fasciitis. BMJ Case Rep. https://doi.org/10.1136/bcr.2012.6158
Suresh E, Doherty V, Schofield O, Goddard C, Dhillon V (2005) Eosinophilic fasciitis and eosinophilic colitis: a rare association. Rheumatology (Oxford, England) 44(3):411–413. https://doi.org/10.1093/rheumatology/keh510
Huemer M, Seeber A, Huemer C (2000) Scleroderma-like syndrome in a child: eosinophilic fasciitis or scleredema adultorum? Eur J Pediatr 159(7):520–522. https://doi.org/10.1007/s004310051323
Ching DW, Petrie JP (1991) Childhood eosinophilic fasciitis presenting as inflammatory polyarthritis and associated with selective IgA deficiency. Ann Rheum Dis 50(9):647–648. https://doi.org/10.1136/ard.50.9.647
Barnes L, Rodnan GP, Medsger TA, Short D (1979) Eosinophilic fasciitis. A pathologic study of twenty cases. Am J Pathol 96(2):493–518
Uruha A, Nishikawa A, Tsuburaya RS, Hamanaka K, Kuwana M, Watanabe Y, Suzuki S, Suzuki N, Nishino I (2017) Sarcoplasmic MxA expression: a valuable marker of dermatomyositis. Neurology 88(5):493–500. https://doi.org/10.1212/WNL.0000000000003568
Tanboon J, Nishino I (2019) Classification of idiopathic inflammatory myopathies: pathology perspectives. Curr Opin Neurol 32(5):704–714. https://doi.org/10.1097/WCO.0000000000000740
Suzuki S, Yonekawa T, Kuwana M, Hayashi YK, Okazaki Y, Kawaguchi Y, Suzuki N, Nishino I (2014) Clinical and histological findings associated with autoantibodies detected by RNA immunoprecipitation in inflammatory myopathies. J Neuroimmunol 274(1-2):202–208. https://doi.org/10.1016/j.jneuroim.2014.07.006
Noguchi E, Uruha A, Suzuki S, Hamanaka K, Ohnuki Y, Tsugawa J, Watanabe Y, Nakahara J, Shiina T, Suzuki N, Nishino I (2017) Skeletal muscle involvement in antisynthetase syndrome. JAMA Neurol 74(8):992–999. https://doi.org/10.1001/jamaneurol.2017.0934
Aringer M, Costenbader K, Daikh D, Brinks R, Mosca M, Ramsey-Goldman R, Smolen JS, Wofsy D, Boumpas DT, Kamen DL, Jayne D, Cervera R, Costedoat-Chalumeau N, Diamond B, Gladman DD, Hahn B, Hiepe F, Jacobsen S, Khanna D, Lerstrøm K, Johnson SR (2019) 2019 European League Against Rheumatism/American College of Rheumatology classification criteria for systemic lupus erythematosus. Arthritis Rheumatol (Hoboken, N.J.) 71(9):1400–1412. https://doi.org/10.1002/art.40930
García-Morteo O, Nitsche A, Maldonado-Cocco JA, Barceló HA (1987) Eosinophilic fasciitis and retroperitoneal fibrosis in a patient with systemic lupus erythematosus. Arthritis Rheum 30(11):1314–1315. https://doi.org/10.1002/art.1780301118
Sills EM (1988) Systemic lupus erythematosus in a patient previously diagnosed as having Shulman disease. Arthritis Rheum 31(5):694–695. https://doi.org/10.1002/art.1780310519
Baffoni L, Frisoni M, Maccaferri M, Ferri S (1995) Systemic lupus erythematosus and eosinophilic fasciitis: an unusual association. Clin Rheumatol 14(5):591–592. https://doi.org/10.1007/BF02208164
Gallardo F, Vadillo M, Mitjavila F, Servitje O (1998) Systemic lupus erythematosus after eosinophilic fasciitis: a case report. J Am Acad Dermatol 39(2 Pt 1):283–285. https://doi.org/10.1016/s0190-9622(98)70091-x
Kitamura Y, Hatamochi A, Hamasaki Y, Ikeda H, Yamazaki S (2007) Association between eosinophilic fasciitis and systemic lupus erythematosus. J Dermatol 34(2):150–152. https://doi.org/10.1111/j.1346-8138.2006.00238.x
Mrabet D, Saadi F, Chelly I, Trojet S, Zaraa I, Sahli H, Haouet S, Ben Osmane A, Meddeb N, Sellami S (2010) A case of Shulman disease in a patient with systemic lupus erythematosus. Lupus 19(14):1674–1675. https://doi.org/10.1177/0961203310376524
Pinal-Fernandez I, Selva-O'Callaghan A, Grau JM (2014) Diagnosis and classification of eosinophilic fasciitis. Autoimmun Rev 13(4-5):379–382. https://doi.org/10.1016/j.autrev.2014.01.019
Ihn H (2019) Eosinophilic fasciitis: from pathophysiology to treatment. Allergol Int: Off J JapanSoc Allergol 68(4):437–439. https://doi.org/10.1016/j.alit.2019.03.001
Acknowledgments
We would like to thank Professor Masataka Kuwana (Department of Allergy and Rheumatology, Nippon Medical School Graduate School of Medicine, Tokyo, Japan) for performing serum anti-ARS antibody tests, Dr. Sho Nishikawa and Professor Masayuki Iwano (Department of Nephrology, Faculty of Medical Sciences, University of Fukui, Fukui, Japan) for evaluating renal biopsy specimens, and Dr. Hiroshi Kasamatsu (Department of Dermatology, Faculty of Medical Sciences, University of Fukui, Fukui, Japan) for obtaining en bloc biopsy specimens.
Funding
This study was supported partly by Intramural Research Grant (2-5 and 29-4) for Neurological and Psychiatric Disorders of NCNP.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
None.
Ethics approval
All procedures used in this research were approved by the Ethical Committee of University of Fukui.
Consent for participate and publication
Informed consent for participation and publication of the case was obtained from the patient.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Asaoka, K., Watanabe, Y., Itoh, K. et al. A case of eosinophilic fasciitis without skin manifestations: a case report in a patient with lupus and literature review. Clin Rheumatol 40, 2477–2483 (2021). https://doi.org/10.1007/s10067-020-05416-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-020-05416-6