Abstract
Introduction
In recent surgical literature, gender-specific differences in the outcome of hernia surgery has been analyzed. We already know that female patients are at higher risk to develop chronic postoperative pain after inguinal, incisional, and umbilical hernia surgery. In this study, we evaluated the impact of gender on the outcome after epigastric hernia surgery.
Methods
A covariable-adjusted matched-paired analysis with data derived from the Herniamed registry was performed. In total of 15,925 patients with 1-year follow-up data were included in the study. Propensity score matching was performed for the 7786 female (48.9%) and 8139 male (51.1%) patients, creating 6350 pairs (81.6%).
Results
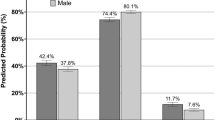
Matched-paired analysis revealed a significant disadvantage for female patients for pain on exertion (12.1% vs. 7.6%; p < 0.001) compared to male patients. The same effect was demonstrated for pain at rest (6.2% in female patients vs. 4.1% in male patients; p < 0.001) and pain requiring treatment (4.6% in female patients vs. 3.1% in male patients; p < 0.001). All other outcome parameters showed no significant differences between female and male patients.
Conclusions
Female patients are at a higher risk for chronic pain after elective epigastric hernia repairs compared to the male patient population. These results complete findings of previous studies showing the same effect in inguinal, umbilical, and incisional hernia repair.



Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author (HH) upon reasonable request.
References
Mansukhani NA, Yoon DY, Teter KA, Stubbs VC, Helenowski IB, Woodruff TK, Kibbe MR (2016) Sex bias exists in human surgical clinical research. JAMA Surg 118:6072–6078. https://doi.org/10.1002/cncr.27633.Percutaneous
Howard R, Telem D (2019) Gender matters—mandating sex as a biologic variable in hernia research. Ann Surg 270:10–11. https://doi.org/10.1097/SLA.0000000000003323
Köckerling F, Bittner R, Kofler M, Mayer F, Adolf D, Kuthe A, Weyhe D (2019) Lichtenstein versus total extraperitoneal patch plasty versus transabdominal patch plasty technique for primary unilateral inguinal hernia repair. Ann Surg 269:351–357. https://doi.org/10.1097/sla.0000000000002541
Hoffmann H, Walther D, Bittner R, Köckerling F, Adolf D, Kirchhoff P (2020) Smaller inguinal hernias are independent risk factors for developing chronic postoperative inguinal pain (CPIP): a registry-based multivariable analysis of 57,999 patients. Ann Surg. https://doi.org/10.1097/SLA.0000000000003065
Niebuhr H, Wegner F, Hukauf M, Lechner M, Fortelny R, Bittner R, Schug-Pass C, Köckerling F (2018) What are the influencing factors for chronic pain following TAPP inguinal hernia repair: an analysis of 20,004 patients from the Herniamed Registry. Surg Endosc 32:1971–1983. https://doi.org/10.1007/s00464-017-5893-2
Köckerling F, Lorenz R, Hukauf M, Grau H, Jacob D, Fortelny R, Koch A (2019) Influencing factors on the outcome in female groin hernia repair. Ann Surg 270:1. https://doi.org/10.1097/sla.0000000000003271
Köckerling F, Koch A, Lorenz R (2019) Groin hernias in women—a review of the literature. Front Surg 6:1–8. https://doi.org/10.3389/fsurg.2019.00004
Lappen JR, Sheyn D, Hackney DN (2016) Does pregnancy increase the risk of abdominal hernia recurrence after prepregnancy surgical repair? Am J Obs Gynecol 215:390.e1-390.e5. https://doi.org/10.1016/j.ajog.2016.05.003
Köckerling F, Adolf D, Lorenz R, Stechemesser B, Kuthe A, Conze J, Lammers B, Fortelny R, Mayer F, Zarras K, Reinpold W, Hoffmann H, Weyhe D (2022) Perioperative outcome in groin hernia repair: what are the most important influencing factors? Hernia 26:201–215. https://doi.org/10.1007/s10029-021-02417-5
Jacob DA, Hackl JA, Bittner R, Kraft B, Köckerling F (2015) Perioperative outcome of unilateral versus bilateral inguinal hernia repairs in TAPP technique: analysis of 15,176 cases from the Herniamed Registry. Surg Endosc Other Interv Tech 29:3733–3740. https://doi.org/10.1007/s00464-015-4146-5
Jakobsson E, Lundström K-J, Holmberg H, de la Croix H, Nordin P (2022) Chronic pain after groin hernia surgery in women: a patient-reported outcome study based on data from the Swedish Hernia Register. Ann Surg 275:213–219
Tolver MA, Strandfelt P, Rosenberg J, Bisgaard T (2013) Female gender is a risk factor for pain, discomfort, and fatigue after laparoscopic groin hernia repair. Hernia 17:321–327. https://doi.org/10.1007/s10029-012-0956-8
Köckerling F, Heine T, Adolf D, Zarras K, Weyhe D, Lammers B, Mayer F, Reinpold W, Jacob D (2021) Trends in emergent groin hernia repair—an analysis from the Herniamed Registry. Front Surg 8:1–13. https://doi.org/10.3389/fsurg.2021.655755
Köckerling F, Brunner W, Mayer F, Fortelny R, Adolf D, Niebuhr H, Lorenz R, Reinpold W, Zarras K, Weyhe D (2021) Assessment of potential influencing factors on the outcome in small (<2 cm) umbilical hernia repair: a registry-based multivariable analysis of 31,965 patients. Hernia 25:587–603. https://doi.org/10.1007/s10029-020-02305-4
Köckerling F, Hoffmann H, Adolf D, Weyhe D, Reinpold W, Koch A, Kirchhoff P (2020) Female sex as independent risk factor for chronic pain following elective incisional hernia repair: registry-based, propensity score-matched comparison. Hernia 24:567–576. https://doi.org/10.1007/s10029-019-02089-2
Köckerling F, Hoffmann H, Reinpold W, Adolf D, Mayer F, Kirchhoff P, Lammers B, Weyhe D, Emmanuel K (2020) Potential influencing factors on the outcome in incisional hernia repair : a registry—based multivariable analysis of 22,895 patients. Hernia. https://doi.org/10.1007/s10029-020-02184-9
Cox TC, Huntington CR, Blair LJ, Prasad T, Lincourt AE, Heniford BT, Augenstein VA (2016) Predictive modeling for chronic pain after ventral hernia repair. Am J Surg 212:501–510. https://doi.org/10.1016/j.amjsurg.2016.02.021
Stirler VMA, Schoenmaeckers EJP, De Haas RJ, Raymakers JTFJ, Rakic S (2014) Laparoscopic repair of primary and incisional ventral hernias: the differences must be acknowledged—a prospective cohort analysis of 1088 consecutive patients. Surg Endosc 28:891–895. https://doi.org/10.1007/s00464-013-3243-6
Köckerling F, Schug-Paß C, Adolf D, Reinpold W, Stechemesser B (2015) Is pooled data analysis of ventral and incisional hernia repair acceptable? Front Surg 2:15. https://doi.org/10.3389/fsurg.2015.00015
Stechemesser B, Jacob DA, Schug-Pass C, Köckerling F (2012) Herniamed: an internet-based registry for outcome research in hernia surgery. Hernia 16:269–276. https://doi.org/10.1007/s10029-012-0908-3
Köckerling F, Adolf D, Zarras K, Fortelny R, Lorenz R, Lammers B, Reinpold W, Stechemesser B, Schug-Pass C, Weyhe D (2021) What is the reality in epigastric hernia repair?–a trend analysis from the Herniamed Registry. Hernia 25:1083–1094. https://doi.org/10.1007/s10029-021-02408-6
Köckerling F, Simon T, Hukauf M, Hellinger A, Fortelny R, Reinpold W, Bittner R (2018) The importance of registries in the postmarketing surveillance of surgical meshes. Ann Surg 268:1097–1104. https://doi.org/10.1097/SLA.0000000000002326
Langbach O, Bukholm I, Benth JŠ, Røkke O (2015) Long term recurrence, pain and patient satisfaction after ventral hernia mesh repair. World J Gastrointest Surg 7:384–393. https://doi.org/10.4240/wjgs.v7.i12.384
Gronnier C, Wattier J-M, Favre H, Piessen G, Mariette C (2012) Risk factors for chronic pain after open ventral hernia repair by underlay mesh placement. World J Surg 36:1548–1554. https://doi.org/10.1007/s00268-012-1523-2
Köckerling F, Hoffmann H, Weyhe D, Adolf D, Koch A, Reinpold W (2019) Female sex as independent risk factor for chronic pain following elective incisional hernia repair: registry-based, propensity score-matched comparison. Hernia. https://doi.org/10.1007/s10029-019-02089-2
Erritzøe-Jervild L, Christoffersen MW, Helgstrand F, Bisgaard T (2013) Long-term complaints after elective repair for small umbilical or epigastric hernias. Hernia 17:211–215. https://doi.org/10.1007/s10029-012-0960-z
Christoffersen MW, Helgstrand F, Rosenberg J, Kehlet H, Strandfelt P, Bisgaard T (2015) Long-term recurrence and chronic pain after repair for small umbilical or epigastric hernias: a regional cohort study. Am J Surg 209:725–732. https://doi.org/10.1016/j.amjsurg.2014.05.021
Correll D (2017) Chronic postoperative pain: recent findings in understanding and management. F1000Research 6:1054 . doi: https://doi.org/10.12688/f1000research.11101.1
Lillemoe KD (2018) Joint statement by the surgery journal editors group. Ann Surg 267:991. https://doi.org/10.1097/TA.0000000000002005
Dominguez CA, Kalliomäki M, Gunnarsson U, Moen A, Sandblom G, Kockum I, Lavant E, Olsson T, Nyberg F, Rygh LJ, Røe C, Gjerstad J, Gordh T, Piehl F (2013) The DQB1*03:02 HLA haplotype is associated with increased risk of chronic pain after inguinal hernia surgery and lumbar disc herniation. Pain 154:427–433. https://doi.org/10.1016/j.pain.2012.12.003
Woo AK (2010) Depression and anxiety in pain. Rev Pain 4:8–12. https://doi.org/10.1177/204946371000400103
Wiering B, de Boer D, Delnoij D (2017) Meeting patient expectations: patient expectations and recovery after hip or knee surgery. Musculoskelet Surg. https://doi.org/10.1007/s12306-017-0523-7
Wallace LM (1985) Surgical patients’ expectations of pain and discomfort: does accuracy of expectations minimise post-surgical pain and distress? Pain 22:363–373
Waljee J, McGlinn EP, Sears ED, Chung KC (2014) Patient expectations and patient-reported outcomes in surgery: a systematic review. Surgery 155:799–808. https://doi.org/10.1016/j.surg.2013.12.015
Leegaard M, Nåden D, Fagermoen MS (2008) Postoperative pain and self-management: women’s experiences after cardiac surgery. J Adv Nurs 63:476–485. https://doi.org/10.1111/j.1365-2648.2008.04727.x
Solheim N, Östlund S, Gordh T, Rosseland LA (2017) Women report higher pain intensity at a lower level of inflammation after knee surgery compared with men. Pain Rep 2:1–8. https://doi.org/10.1097/PR9.0000000000000595
Reinpold W (2017) Risk factors of chronic pain after inguinal hernia repair: a systematic review. Innov Surg Sci 2:61–68. https://doi.org/10.1515/iss-2017-0017
Kokotovic D, Sjølander H, Gögenur I, Helgstrand F (2016) Watchful waiting as a treatment strategy for patients with a ventral hernia appears to be safe. Hernia 20:281–287. https://doi.org/10.1007/s10029-016-1464-z
Lauscher JC, Leonhardt M, Martus P, ZurHausen G, Aschenbrenner K, Zurbuchen U, Thielemann H, Kohlert T, Schirren R, Simon T, Buhr HJ, Ritz J-P, Kreis ME (2016) Watchful waiting vs surgical repair of oligosymptomatic incisional hernias: current status of the AWARE study. Der Chir 87:47–55. https://doi.org/10.1007/s00104-015-0011-2
Hannan EL, Cozzens K, King SB, Walford G, Shah NR (2012) The New York state cardiac registries: history, contributions, limitations, and lessons for future efforts to assess and publicly report healthcare outcomes. J Am Coll Cardiol 59:2309–2316. https://doi.org/10.1016/J.JACC.2011.12.051
Henriksen NA, Montgomery A, Kaufmann R, Berrevoet F, East B, Fischer J, Hope W, Klassen D, Lorenz R, Renard Y, Garcia Urena MA (2020) Guidelines for treatment of umbilical and epigastric hernias from the European Hernia Society and Americas Hernia Society. Brit J Surg 107:171–190. https://doi.org/10.1002/bjs.11489
Haapaniemi S, Nilsson E (2002) Recurrence and pain three years after groin hernia repair. Validation of postal questionnaire and selective physical examination as a method of follow-up. Eur J Surg 168:22–28. https://doi.org/10.1080/110241502317307535
McLean KA, Sheng Z, O’Neill S, Boyce K, Jones C, Wigmore SJ, Harrison EM (2017) The influence of clinical and patient-reported outcomes on post-surgery satisfaction in cholecystectomy patients. World J Surg 41:1752–1761. https://doi.org/10.1007/s00268-017-3917-7
Köckerling F, Maneck M, Günster C, Adolf D, Hukauf M (2020) Comparing routine administrative data with registry data for assessing quality of hospital care in patients with inguinal hernia. Hernia 24:143–151. https://doi.org/10.1007/s10029-019-02009-4
Funding
Dr. Köckerling has grants to fund Herniamed from Johnson & Johnson, Norderstedt, Karl Storz, Tuttlingen, pfm medical, Cologne, Dahlhausen, Cologne, B Braun, Tuttlingen, Men- keMed, Munich, Bard, Karlsruhe. Personal fees from Bard, Karlsruhe, outside the submitted work. All other authors have nothing to disclose.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Dr. Köckerling reports grants to fund Herniamed from Johnson & Johnson, Norderstedt, Karl Storz, Tuttlingen, pfm medical, Cologne, Dahlhausen, Cologne, B.Braun, Tuttlingen, MenkeMed, Munich, and personal fees from Bard-B, Karlsruhe. All other authors have nothing to disclose.
Ethical approval
Only cases of routine hernia surgery were documented in the Herniamed Registry and all patients have signed a special informed consent declaration agreeing to participate. The Herniamed Registry has ethical approval (BASEC Nr 2016–00,123, 287/2017BO2).
Human and animal rights
This article does not contain any study with animals performed by any of the authors.
Informed consent
All patients with routine hernia surgery documented in the Herniamed Registry have signed an informed consent declaration agreeing to participate.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Hoffmann, H., Mechera, R., Nowakowski, D. et al. Gender differences in epigastric hernia repair: a propensity score matching analysis of 15,925 patients from the Herniamed registry. Hernia 27, 829–838 (2023). https://doi.org/10.1007/s10029-023-02799-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-023-02799-8