Abstract
Background and objective
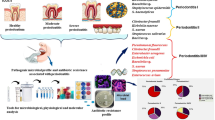
Aggregatibacter actinomycetemcomitans and Porphyromonas gingivalis have been frequently isolated in periodontitis patients in Morocco. Its persistence after the subgingival debridement of the biofilm has been correlated with worse clinical outcomes. The aim of this study was to evaluate the antimicrobial susceptibilities of A. actinomycetemcomitans and P. gingivalis, to amoxicillin, amoxicillin plus clavulanate, metronidazole, and azithromycin. In addition, microbiological profiles of patients harbouring A. actinomycetemcomitans, P. gingivalis, or both were compared.
Material and methods
In 45 consecutive periodontitis Moroccan patients, subgingival samples were taken and processed by culture. Twenty-four A. actinomycetemcomitans and 30 P. gingivalis colonies were isolated (54 strains) and susceptibility tests, using the epsilometric method, were run for amoxicillin, amoxicillin plus clavulanate, metronidazole, and azithromycin. Minimum inhibitory concentrations for 50 (MIC50) and 90% (MIC90) of the organisms were calculated.
Results
The prevalence of A. actinomycetemcomitans and P. gingivalis was 79.5 and 84.4%, respectively. A. actinomycetemcomitans showed susceptibility to amoxicillin, amoxicillin plus clavulanate, while 28% of the isolated strains were resistant to azithromycin and 61.7% towards metronidazole. No P. gingivalis resistance towards amoxicillin, amoxicillin plus clavulanate, metronidazole, and azithromycin was found.
Conclusion
A. actinomycetemcomitans and P. gingivalis were frequently detected in Moroccan patients with periodontitis, while antimicrobial resistance was only detected for A. actinomycetemcomitans to metronidazole and azithromycin.
Clinical relevance
A. actinomycetemcomitans resistance against some antimicrobials in periodontitis patients in Morocco can influence the selection of the therapeutic approaches.


Similar content being viewed by others
References
Offenbacher S (1996) Periodontal diseases: pathogenesis. Ann Periodontol 1:821–878
Thomas RZ, Loos BG, Teeuw W, Kunnen A, van Winkelhoff AJ, Abbas F (2015) Periodontitis and systemic diseases: from science to clinical practice. Ned Tijdschr Tandheelkd 122:542–548
Llambes F, Arias-Herrera S, Caffesse R (2015) Relationship between diabetes and periodontal infection. World J Diabetes 6:927–935
Ferreira MC, Dias-Pereira AC, Branco-de-Almeida LS, Martins CC, Paiva SM (2017) Impact of periodontal disease on quality of life: a systematic review. J Periodontal Res 52:651–665
Mira A, Simon-Soro A, Curtis MA (2017) Role of microbial communities in the pathogenesis of periodontal diseases and caries. J Clin Periodontol 44(Suppl. 18):S23–S38
Marsh PD (2005) Dental plaque: biological significance of a biofilm and community life-style. J Clin Periodontol 32:7–15
Haubek D, Ennibi OK, Poulsen K, Poulsen S, Benzarti N, Kilian M (2001) Early-onset periodontitis in Morocco is associated with the highly leukotoxic clone of Actinobacillus actinomycetemcomitans. J Dent Res 80:1580–1583
Haubek D, Ennibi OK, Vaeth M, Poulsen S, Poulsen K (2009) Stability of the JP2 clone of Aggregatibacter actinomycetemcomitans. J Dent Res 88:856–860
Haubek D, Ennibi OK, Poulsen K, Vaeth M, Poulsen S, Kilian M (2008) Risk of aggressive periodontitis in adolescent carriers of the JP2 clone of Aggregatibacter (Actinobacillus) actinomycetemcomitans in Morocco: a prospective longitudinal cohort study. Lancet 371:237–242
Minguez M, Ennibi OK, Pousa X, Lakhdar L, Abdellaoui L, Sanchez M et al (2016) Characterization of A. actinomycetemcomitans strains in subgingival samples from periodontitis subjects in Morocco. Clin Oral Investig 20:1809–1818
Haffajee AD, Socransky SS, Dibart S, Kent RL (1996) Response to periodontal therapy in patients with high or low levels of P. gingivalis, P. intermedia, R nigrescens and B. forsythus. J Clin Periodontol 23:336–345
Holt SC, Kesavalu L, Walker S, Genco CA (1999) Virulence factors of Porphyromonas gingivalis. Periodontol 2000 20:168–238
Chahboun H, Arnau MM, Herrera D, Sanz M, Ennibi OK (2015) Bacterial profile of aggressive periodontitis in Morocco: a cross-sectional study. BMC Oral Health 15:25
Van der Velden U, Abbas F, Armand S, Loos BG, Timmerman MF, Van der Weijden GA et al (2006) Java project on periodontal diseases. The natural development of periodontitis: risk factors, risk predictors and risk determinants. J Clin Periodontol 33:540–548
Hirschfeld L, Wasserman B (1978) A long-term survey of tooth loss in 600 treated periodontal patients. J Periodontol 49:225–237
Renvert S, Wikstrom M, Dahlen G, Slots J, Egelberg J (1990) Effect of root debridement on the elimination of Actinobacillus actinomycetemcomitans and Bacteroides gingivalis from periodontal pockets. J Clin Periodontol 17:345–350
Herrera D, Sanz M, Jepsen S, Needleman I, Roldan S (2002) A systematic review on the effect of systemic antimicrobials as an adjunct to scaling and root planing in periodontitis patients. J Clin Periodontol 29(Suppl 3):136–159 discussion 60-2
Herrera D, Alonso B, Leon R, Roldan S, Sanz M (2008) Antimicrobial therapy in periodontitis: the use of systemic antimicrobials against the subgingival biofilm. J Clin Periodontol 35:45–66
Ardila CM, Granada MI, Guzman IC (2010) Antibiotic resistance of subgingival species in chronic periodontitis patients. J Periodontal Res 45:557–563
Herrera D, van Winkelhoff AJ, Dellemijn-Kippuw N, Winkel EG, Sanz M (2000) Beta-lactamase producing bacteria in the subgingival microflora of adult patients with periodontitis. A comparison between Spain and The Netherlands. J Clin Periodontol 27:520–525
Van Winkelhoff AJ, Gonzales DH, Winkel EG, Dellemijn-Kippuw N, Vandenbroucke-Grauls CMJE, Sanz M (2000) Antimicrobial resistance in the subgingival microflora in patients with adult periodontitis. J Clin Periodontol 27:79–86
Van Winkelhoff AJ, Herrera D, Oteo A, Sanz M (2005) Antimicrobial profiles of periodontal pathogens isolated from periodontitis patients in The Netherlands and Spain. J Clin Periodontol 32:893–898
Soares GMS, Figueiredo LC, Faveri M, Cortelli SC, Duarte PM, Feres M (2012) Mechanisms of action of systemic antibiotics used in periodontal treatment and mechanisms of bacterial resistance to these drugs. J Appl Oral Sci 20:295–309
Armitage GC (1999) Development of a classification system for periodontal diseases and conditions. Ann Periodontol 4:1–6
Mombelli A, McNabb H, Lang NP (1991) Black-pigmenting Gram-negative bacteria in periodontal disease. II. Screening strategies for detection of P. gingivalis. J Periodontal Res 26:308–313
Syed SA, Loesche WJ (1972) Survival of human dental plaque flora in various transport media. Appl Microbiol 24:638–644
Alsina M, Olle E, Frias J (2001) Improved, low-cost selective culture medium for Actinobacillus actinomycetemcomitans. J Clin Microbiol 39:509–513
Nachnani S, Scuteri A, Newman MG, Avanessian AB, Lomeli SL (1992) E-test: a new technique for antimicrobial susceptibility testing for periodontal microorganisms. J Periodontol 63:576–583
The European Committee on Antimicrobial Susceptibility Testing (2016) Breakpoint tables for interpretation of MICs and zone diameters. Version 6.0, 2016
Benrachadi L, Bouziane A, Azziman Z, Bouziane-Ouartini F, Ennibi O (2012) Screening for periodontopathogenic bacteria in severe chronic periodontitis in a Moroccan population. Med Mal Infect 42:599–602
Kulik EM, Lenkeit K, Chenaux S, Meyer J (2008) Antimicrobial susceptibility of periodontopathogenic bacteria. J Antimicrob Chemother 61:1087–1091
Japoni A, Vasin A, Noushadi S, Kiany F, Japoni S, Alborzi A (2011) Antibacterial susceptibility patterns of Porphyromonas gingivalis isolated from chronic periodontitis patients. Med Oral Patol Oral Cir Bucal 16:1031–1035
Veloo AC, Seme K, Raangs E, Rurenga P, Singadji Z, Wekema-Mulder G et al (2012) Antibiotic susceptibility profiles of oral pathogens. Int J Antimicrob Agents 40:450–454
Dahlen G, Preus HR (2017) Low antibiotic resistance among anaerobic Gram-negative bacteria in periodontitis 5 years following metronidazole therapy. Anaerobe 43:94–98
Acknowledgments
We thank Itziar González and Ana O’Connor from the Laboratory of Dental Research, University Complutense, Madrid, for their technical assistance.
Funding
The work was supported by the ETEP (Aetiology and Therapy of Periodontal Diseases) Research Group, University Complutense, Madrid, Spain.
Author information
Authors and Affiliations
Contributions
MM carried out acquisition of data, performed the antimicrobial susceptibility tests, and drafted the manuscript. LL and AL carried out the acquisition of data. PP and MCS processed the samples. DH conceived of the study, participated in the design of the study, and revised critically the manuscript. MS participated in the design of the study and its coordination. OKE took part in the coordination of the study, in the collection of the data, and revised critically the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Highlights
• In a group of Moroccan patients with chronic or aggressive periodontitis, the prevalence of Aggregatibacter actinomycetemcomitans and Porphyromonas gingivalis was 79.5 and 84.4%, respectively.
• A. actinomycetemcomitans showed susceptibility for amoxicillin and amoxicillin plus clavulanate, while 28% of the isolated strains were resistant to azithromycin and 61.7% towards metronidazole.
• No resistance towards amoxicillin, amoxicillin plus clavulanate, metronidazole, and azithromycin was found for P. gingivalis in this Moroccan periodontitis patient cohort.
Rights and permissions
About this article
Cite this article
Mínguez, M., Ennibi, O.K., Perdiguero, P. et al. Antimicrobial susceptibilities of Aggregatibacter actinomycetemcomitans and Porphyromonas gingivalis strains from periodontitis patients in Morocco. Clin Oral Invest 23, 1161–1170 (2019). https://doi.org/10.1007/s00784-018-2539-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-018-2539-2