Abstract
Objective
To analyze the variables determining morbidity, mortality and outcome in subjects with brain abscesses treated at a single center over a 10-year period.
Methods
A retrospective study was conducted on a series of 59 patients with brain abscesses surgically treated with stereotactically guided aspiration or open craniotomy excision. Such variables as age, gender, clinical presentation, number of days to diagnosis, location, number of lesions, predisposing factors, mechanism of infection, etiological agent, and therapy were analyzed independently. Complications were defined as any deviation from the normal postoperative course occurring within 30 days of surgery, and classified according to a four-point gradual severity scale. Postoperative outcome was appraised through the Glasgow Outcome Scale (GOS) 6 months after surgery, 0–4 points were considered poor outcome and 5 points good outcome.
Results
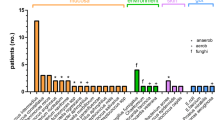
Eighty abscesses were diagnosed and surgically managed in 59 patients. The mean age was 44.69 years (range: 0.16-77); 59.3% were female. The median number of days to diagnosis was 7. Most frequent clinical presentations included fever (52.5%), headache (42.4%), and focal neurologic deficits (39%). Mechanism of infection was mainly hematogenous spread (32.2%). Stereotactically guided aspiration was the treatment of choice for 74.6% of the patients, whereas 25.4% of the cases were managed through open craniotomy excision. Outcome was favorable in 81.35% (n = 48) of the subjects. General morbidity was 27.1%, and mortality stood at 10.16%. Out of a total 38.98% (n = 23) of complications, two-thirds were due to medical causes. The analysis of variables revealed that only age (p = 0.02), immunosuppression (OR 5.83; p = 0.012) and hematogenous spread (p < 0.01) were associated with poor outcomes.
Conclusions
Immunosuppression, hematogenous spread and advanced age were predictors of poor prognosis. Most of the complications following brain abscess management were not directly related to surgery or surgical technique.


Similar content being viewed by others
References
Besada CH, Migliaro M, Christiansen SB, Funes JA, Ajler PM, Mónaco RD (2010) Restricted diffusion in a ring-enhancing mucoid metastasis with histological confirmation: case report. J Comput Assist Tomogr 34(5):770–772
Carpenter JL (1994) Brain stem abscesses: cure with medical therapy, case report, and review. Clin Infect Dis 18:219
Carpenter J, Stapleton S, Holliman R (2007) Retrospective analysis de 49 cases of brain abscess and review of the literature. Eur J Cin Microbiol Infect Dis 26:1–11
Cavuşoglu H, Kaya RA, Türkmenoglu ON, Colak I, Aydin Y (2008) Brain abscess: analysis of results in a series of 51 patients with a combined surgical and medical approach during an 11-year period. Neurosurg Focus 24:E9
Favre J, Curty B, Steel T, Baltuch G, Genné D, Kernan J, Fankhauser H (1998) Recurrent nocardial brain abscesses treated by repeated stereotactic aspirations. J Clin Neurosci 5(1):98–101
Fellows GA, Kalsi P, Martin AJ (2007) Nocardial brain abscess in a patient without immunocompromise. Br J Neurosurg 21(3):301–306
Hall WA (1994) Cerebral infectious processes. In: Loftus CM (ed) Neurosurgical emergencies, vol 1. American Association of Neurological Surgeons Publications, Park Ridge, pp 165–182
Kao PT, Tseng HK, Liu CP, Su SC, Lee CM (2003) Brain abscess: clinical analysis of 53 cases. J Microbiol Immunol Infect 36:129–136
Kapsalaki EZ, Gotsis ED, Fountas KN (2008) The role of proton magnetic resonance spectroscopy in the diagnosis and categorization of cerebral abscesses. Neurosurg Focus 24(6):E7
Kothari M, Goel A (2008) Brain abscess: a cogent clarifier of the confused concept of immunity. Neurosurg Focus 24(6):E16
Landriel Ibañez FA, Hem S, Ajler P, Vecchi E, Ciraolo C, Baccanelli M, Tramontano R, Knezevich F, Carrizo A (2011) A new classification of complications in neurosurgery. World Neurosurg 75(5–6):709–715
Lu CH, Chang WN, Lui CC (2006) Strategies for the management of bacterial brain abscess. J Clin Neurosci 13:979–985
Mamelak A, Obana W, Flaherty J, Rosenblum M (1994) Nocardial brain abscess: treatment strategies and factors influencing outcome. Clinical study. Neurosurgery 35(4):622–631
Mamelak A, Mampalam T, Obana W, Rosenblum M (1995) Improved management of multiple brain abscesses: a combined surgical and medial approach, clinical study. Neurosurgery 36(1):76–86
Mampalam TJ, Rosenblum ML (1988) Trends in the management of bacterial brain abscesses: a review of 102 cases over 17 years. Neurosurgery 23:451
Mathisen GE, Johnson JP (1997) Brain abscess. Clin Infect Dis 25:763
Nathoo N, Nadvi SS, Narotam PK, van Dellen JR (2011) Brain abscess: management and outcome analysis of a computed tomography era experience with 973 patients. World Neurosurg 75(5–6):716–726
Ng PY, Seow WT, Ong PL (1995) Brain abscesses: review of 30 cases treated with surgery. Aust N Z J Surg 65:664
Quartey GR, Johnston JA, Rozdilsky B (1976) Decadron in the treatment of cerebral abscess. An experimental study. J Neurosurg 45:301
Schliamser SE, Bäckman K, Norrby SR (1988) Intracranial abscesses in adults: an analysis of 54 consecutive cases. Scand J Infect Dis 20:1
Seydoux C, Francioli P (1992) Bacterial brain abscesses: factors influencing mortality and sequelae. Clin Infect Dis 15:394
Su TM, Lan CM, Tsai YD, Lee TC, Lu CH, Chang WN (2008) Multiloculated pyogenic brain abscess: experience in 25 patients. Neurosurgery 62(Suppl 2):556
Tattevin P, Bruneel F, Clair B, Lellouche F, de Broucker T, Chevret S, Bédos JP, Wolff M, Régnier B (2003) Bacterial brain abscesses: a retrospective study of 94 patients admitted to an intensive care unit (1980 to 1999). Am J Med 115:143
Tseng JH, Tseng MY (2006) Brain abscess in 142 patients: factors influencing outcome and mortality. Surg Neurol 65:557–562
Xiao F, Tseng MY, Teng LJ, Tseng HM, Tsai JC (2005) Brain abscess: clinical experience and analysis of prognostic factors. Surg Neurol 63(5):442–449
Chang Y-T, Lu C-H, Chuang M-J, Huang C-R, Chuang Y-C, Tsai N-W, Chen S-F, Chang C-C, Chang W-N (2010) supratentorial deep-seated bacterial brain abscess in adults: clinical characteristics and therapeutic outcomes. Acta Neurol Taiwan 19:178–183
Acknowledgments
We thank Omar Konsol M.D., Santiago Portillo M.D. and Carlos Ciraolo M.D. for their assistance with the manuscript preparation and pediatric patient’s data and images.
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Landriel, F., Ajler, P., Hem, S. et al. Supratentorial and infratentorial brain abscesses: surgical treatment, complications and outcomes—a 10-year single-center study. Acta Neurochir 154, 903–911 (2012). https://doi.org/10.1007/s00701-012-1299-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-012-1299-z