Abstract
Objective
The frequency and pattern of endocrine abnormalities among patients with traumatic brain injury have been the subject matter of very few studies. This study was intended to assess the pattern of endocrine dysfunction following severe head injury.
Methods
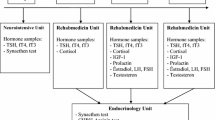
Severe head injury patients admitted to the Department of Neurosurgery, All India Institute of Medical Sciences, New Delhi, from January to December in 1 year formed the study group. Apart from clinical assessment, NCCT of the head was performed on all patients on admission. A complete anterior pituitary hormone analysis was performed within 24 h of injury and was repeated at 2 weeks, 3 months and 6 months amongst patients who survived.
Results
A total of 99 patients were included in the study. Forty of our patients succumbed in the hospital. Rest of the patients were followed up for 6 months. Elevations of cortisol followed by prolactin were the most common hormonal derangements at admission. Midline shift on CT scans was inversely related to cortisol elevation and directly related to GH elevation. Infarct on CT scans was inversely related to cortisol and LH elevation. A significant alteration was found in the decreasing trend of the mean T4 values and normalisation or a decreasing trend from initially elevated mean cortisol and GH levels during follow-up (p < 0.05).
Conclusions
This study reveals that abnormalities in hormonal profiles appear to be relatively common in severe traumatic brain injury and fluctuate significantly over at least 6 months; there is a correlation with age and radiological findings. Performance of hormonal analysis evaluation should be considered in patients with severe brain injury so that appropriate hormonal replacement can be done to optimise the clinical outcome.
Similar content being viewed by others
References
Acerini CL, Tasker RC (2008) Neuroendocrine consequences of traumatic brain injury. J Pediatr Endocrinol Metab 21:611–619
Agha A, Thompson CJ (2006) Anterior pituitary dysfunction following traumatic brain injury (TBI). Clin Endocrinol (Oxf) 64:481–488
Altman R, Pruzanski W (1961) Post traumatic hypopituitarism. Anterior pituitary insufficiency following skull fracture. Ann Intern Med 55:149–154
Barreca T, Perria C, Sannia A, Magnani G, Rolandi E (1980) Evaluation of anterior pituitary function in patients with post-traumatic diabetes insipidus. J Clin Endocrinol Metab 51:1270–1282
Beck-Peccoz P, Amr S, Menezes FM, Faglia G, Weintraub BD (1985) Decreased receptor binding of biologically inactive thyrotrophin in central hypothyroidism. N Engl J Med 312:1085–1090
Behan LA, Phillips J, Thompson CJ, Agha A (2008) Neuroendocrine disorders after traumatic brain injury. J Neurol Neurosurg Psychiatry 79:753–759
Bondanelli M, Ambrosio MR, Margutti A, Boldrini P, Basaglia N, Franceschetti P, Zatelli MC (2002) Evidence for integrity of the growth hormone/ insulin-like growth factor-I. Axis in patients with severe head trauma during rehabilitation. Metabolism 51:1363–1369
Bondanelli M, De Marinis L, Ambrosio MR, Monesi M, Valle D, Zatelli MC, Fusco A, Bianchi A, Farneti M, degli Uberti EC (2004) Occurrence of pituitary dysfunction following traumatic brain injury. J Neurotrauma 21:685–696
Bushnik T, Englander J, Katznelson L (2007) Fatigue after TBI: association with neuroendocrine abnormalities. Brain Inj 21:559–566
Childer MK, Rupright J, Jones PS, Merveille O (1990) Assessment of neuroendocrine dysfunction following traumatic brain injury. Brain Injury 12:517–523
Chioléro R, Lemarchand T, Schutz Y, de Tribolet N, Felber JP, Freeman J, Jéquier E (1998) Plasma pituitary hormone levels in severe trauma with or without head injury. J Trauma 28:1368–1374
Clark JDA, Reggatt PR, Edwards OM (1992) Abnormalities of the hypothalamo-pituitary-gonadal axis after head injury. Clin Endocrinol 36:481–485
Cumming DC, Quigley MF, Yen SSC (1983) Acute suppression of circulating testosterone levels by cortisol in men. J Clin Endocrinol Metab 57:671–673
De Marinis L, Mancini A, Valle D, Bianchi A, Gentilella R, Liberale I, Mignani V, Pennisi M, Della Corte F (1999) Hypothalamic deranagement in traumatized patients: growth hormone (GH) and prolactin response to thyrotrophin-releasing hormone and GH-releasing hormone. Clin Endocrinol (Oxf) 50:741–747
Desai D, March R, Watters JM (1989) Hyperglycemia after trauma increases with age. J Trauma 29:719–723
Edwards OM, Clark JDA (1986) Posttraumatic hypopituitarism. Six cases and a review of the literature. Medicine 65:281–290
Jambart S, Turpin G, de Gennes JL (1980) Panhypopituitarism secondary to head trauma: evidence for a hypothalamic origin of the deficit. Acta Endocrinol 93:264–270
Kanade A, Ruiz AE, Tornyos K, Wakabayashi I, Kastin AJ (1978) Panhypopituitarism and anemia secondary to traumatic fracture of the sella turcica. J Endocrinol Invest 1:263–268
Kelly DF, Gonzalo IT, Cohan P, Berman N, Swerdloff R, Wang C (2000) Hypopituitarism following traumatic brain injury and aneurysmal subarachnoid hemorrhage: a preliminary report. J Neurosurg 93:743–752
King LR, Knowles HC, McLaurin RL, Brielmaier J, Perisutti G, Piziak VK (1981) Pituitary hormone response to head injury. Neurosurgery 9:229–235
King LR, McLaurin RL, Lewis HP, Knowles HC Jr (1970) Plasma cortisol levels after head injury. Ann Surg 172:975–984
Liddle GW, Island DP, Meador CK (1962) Normal and abnormal regulation of corticotrophin secretion in man. Recent Prog Hormone Res 18:125
Markianos M, Seretis A, Kotsou A, Christopoulos M (1996) CSF neurotransmitter metabolites in comatose head injury patients during changes in their clinical states. Acta neurochirurgica 138:57–59
Matsura H, Nakazawa S, Wakabahyashi I (1985) Thyrotropin releasing hormone provocative release of prolactin and thyrotropin in acute head injury. Neurosurgery 16:791–765
Moses AM, Miller M (1968) Stimulation and inhibition of ACTH release in patients with pituitary disease. J Clin Endocr 28:1581
Muller EE, Salerno F, Cocchi D, Locatelli V, Panerai AE (1979) Interaction between the thyrotropin releasing hormone induced growth hormone rise and dopaminergic drugs; studies in pathological conditions in the animal and man. Clin Endocrinol 11:645–656
Niederland T, Makovi H, Gál V, Andréka B, Abrahám CS, Kovács J (2007) Abnormalities of pituitary function after traumatic brain injury in children. J Neurotrauma 24:119–127
Oppenheimer IH, Fisher LV, Jailer JW (1961) Disturbance of the pituitary adrenal interrelationship in disease of the central nervous system. J Clin Endocr 21:1023
Popovic V (2005) GH deficiency as the most common pituitary defect after TBI: clinical implications. Pituitary 8:239–243
Schneider M, Schneider HJ, Stalla GK (2005) Anterior pituitary hormone abnormalities following traumatic brain injury. J Neurotrauma 22:937–946
Soules MR, Sheldon GW (1979) Traumatic hypopituitarism: anterior hypophyseal insufficiency from indirect cranial trauma. South Med J 72:1592–1596
Valenta LJ, De Feo DR (1980) Post traumatic hypopituitarism due to a hypothalamic lesion. Am J Med 68:614–617
Wartofsky L, Burman KD (1998) Alterations in thyroid function in patients with systemic illness: the euthyroid sick syndrome. Endocr Rev 3:164–217
Weiss SR, Jacobi JD, Fishman LM, Lemaire WJ (1982) Hypopituitarism following head trauma. Am J Med 72:861–873
Woolf PD (1992) Hormonal responses to trauma. Crit Care Med 20:216–226
Woolf PD, Hamill RW, McDonald VJ, Lee LA, Kelly M (1986) Transient hypogonadotrophic hypogonadism after head trauma: effects on steroid precursors and correlation with sympathetic nervous system activity. Clin Endocrinol 25:265–274
Author information
Authors and Affiliations
Corresponding author
Additional information
Comment
This paper researches an area of increasing attention, namely pituitary dysfunction following severe brain trauma. This paper suggests its most valuable function is predictive, and certainly the cortisol and thyroid axis should be investigated early in TBI, although for the most part the hormones appear to increase, in those we rely on in the short term.
Michael Powell
London, United Kingdom
Rights and permissions
About this article
Cite this article
Tandon, A., Suri, A., Kasliwal, M.K. et al. Assessment of endocrine abnormalities in severe traumatic brain injury: a prospective study. Acta Neurochir 151, 1411–1417 (2009). https://doi.org/10.1007/s00701-009-0444-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-009-0444-9