Abstract
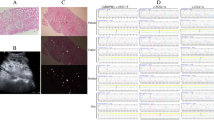
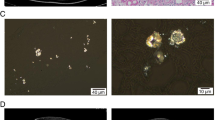
A 32-year-old male was suspected to have primary hyperoxaluria type 1 (PH1) and eventually underwent liver transplantation (LT). He was diagnosed with nephrolithiasis at 9 years of age. Right heminephrectomy was performed for a staghorn calculus. He underwent urethrotomy for urinary retention at 12 years of age. Percutaneous nephrolithotomy was performed for nephrolithiasis when he was 16 years of age. He underwent frequent extracorporeal shock wave lithotripsy for recurrent nephrolithiasis from 18 to 24 years of age. PH1 was suspected at 32 years of age, and pharmacological therapy was also initiated. He developed renal failure at 36 years of age, which was treated with intensive hemodialysis. A definitive diagnosis of PH1 was made based on a liver needle biopsy 1 month later. He received a living-donor LT at 38 years of age, and a living-donor kidney transplant from the same donor 8 months later. Though he made a good recovery, an early diagnosis and preemptive LT are important for PH1 patients.

Similar content being viewed by others
References
Cochat P, Fargue S, Harambat J. Primary hyperoxaluria type 1: strategy for organ transplantation. Curr Opin Organ Transplant. 2010;15:590–3.
Jamieson NV, Jamieson KA. Primary hyperoxaluria type 1: gene therapy by liver transplantation. Transplantation. 2009;87:1273–4.
Malla I, Lysy PA, Godefroid N, Smets F, Malaise J, Reding R, et al. Two-step transplantation for primary hyperoxaluria: cadaveric liver followed by living donor related kidney transplantation. Pediatr Transplant. 2009;13:782–4.
Hori T, Uemoto S, Takada Y, Oike F, Ogura Y, Ogawa K, et al. Does a positive lymphocyte cross-match contraindicate living-donor liver transplantation? Surgery. 2010;147:840–4.
Cibrik DM, Kaplan B, Arndorfer JA, Meier-Kriesche HU. Renal allograft survival in patients with oxalosis. Transplantation. 2002;74:707–10.
Raju DL, Cantarovich M, Brisson ML, Tchervenkov J, Lipman ML. Primary hyperoxaluria: clinical course, diagnosis, and treatment after kidney failure. Am J Kidney Dis. 2008;51:e1–5.
Bergstralh EJ, Monico CG, Lieske JC, Herges RM, Langman CB, Hoppe B, et al. Transplantation outcomes in primary hyperoxaluria. Am J Transplant. 2010;10:2493–501.
Sutherland SM, Alexander SR, Sarwal MM, Berquist WE, Concepcion W. Combined liver–kidney transplantation in children: indications and outcome. Pediatr Transplant. 2008;12:835–46.
Scheinman JI. Liver transplantation in oxalosis prior to advanced chronic kidney disease. Pediatr Nephrol. 2010;25:2217–22.
Ogawa K, Kasahara M, Sakamoto S, Ito T, Taira K, Oike F, et al. Living donor liver transplantation with reduced monosegments for neonates and small infants. Transplantation. 2007;83:1337–40.
Shirouzu Y, Kasahara M, Morioka D, Sakamoto S, Taira K, Uryuhara K, et al. Vascular reconstruction and complications in living donor liver transplantation in infants weighing less than 6 kilograms: the Kyoto experience. Liver Transpl. 2006;12:1224–32.
Eytan Mor MD, Weismann I. Current treatment for primary hyperoxaluria type 1: when should liver/kidney transplantation be considered. Pediatr Transplant. 2009;13:805–7.
Acknowledgments
We are grateful to Eiichiro Watanabe, Sho Koyasu, Akio Nakajima, Kazuhiro Kami and Nao Kawaguchi (Department of Surgery, Kyoto University Hospital, Kyoto, Japan) for their support. This work was partially supported by a grant to T. Hori from the Uehara Memorial Foundation (No. 200940051, Tokyo 171-0033, Japan).
Conflict of interest
All authors have no financial conflicts of interest to declare.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hori, T., Kaido, T., Tamaki, N. et al. An adult with primary hyperoxaluria type 1 regrets not receiving preemptive liver transplantation during childhood: report of a case. Surg Today 43, 1185–1187 (2013). https://doi.org/10.1007/s00595-012-0310-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-012-0310-x