Abstract
Purpose
Transitional lumbosacral vertebrae (TLSV) are a congenital anomaly of the lumbosacral region that is characterized by the presence of a vertebra with morphological properties of both the lumbar and sacral vertebrae, with a prevalence of up to 36% in asymptomatic patients and 20% in adolescent idiopathic scoliosis patients. In patients with TLSV, because of these morphological changes and the different numbers of lumbar vertebrae, there are two optional reference sacral endplates that can be selected intently or inadvertently to measure the spinopelvic parameters: upper and lower endplates. The spinopelvic parameters measured using the upper and lower endplates are significantly different from each other as well as from the normative values. Therefore, the selection of a reference endplate changes the spinopelvic parameters, lumbar lordosis (LL), and surgical goals, which can result in surgical over- or under-correction. Because there is no consensus on the selection of sacral endplate among these patients, it is unclear as to which of these parameters should be used in diagnosis or surgical planning. The present study describes a standardization method for measuring the spinopelvic parameters and LL in patients with TLSV.
Methods
Upper and lower endplate spinopelvic parameters (i.e., pelvic incidence [PI], sacral slope [SS], and pelvic tilt) and LL of 108 patients with TLSV were measured by computed tomography. In addition, these parameters were measured for randomly selected subjects without TLSV. The PI value in the TLSV group, which was closer to the mean PI value of the control group, was accepted as valid and then used to create an optimum PI (OPI) group. Finally, the spinopelvic parameters and LL of the OPI and control groups were compared.
Results
Except for SS, all spinopelvic parameters and LL were comparable between the OPI and control groups. In the OPI group, 60% of the patients showed valid upper endplate parameters, and 40% showed valid lower endplate parameters. No difference was noted in the frequency of valid upper or lower endplates between the sacralization and lumbarization groups. Both the OPI and control groups showed nearly comparable correlations between their individual spinopelvic parameters and LL, except for PI and LL in the former.
Conclusions
Because PI is unique for every individual, the endplate whose PI value is closer to the normative value should be selected as the reference sacral endplate in patients with TLSV.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The spinopelvic parameters are used to evaluate the three-dimensional alignment and balance of the spine and pelvis [1,2,3]. The most important spinopelvic parameter is pelvic incidence (PI), which refers to the sum of pelvic tilt (PT) and sacral slope (SS). PI is a fixed value for every individual after bone maturation and does not change with posture. The spinopelvic parameters have been reported to be correlated with certain spinal pathologies, such as scoliosis, spondylolisthesis, and degenerative spine and disk diseases [4,5,6], as well as with pain, disability, and impaired health-related quality of life scores [7, 8]. Considering that PI also affects lumbar lordosis (LL), some authors have developed formulas to predict the ideal LL for surgical planning [9].
Generally, the upper endplate of the sacrum (S1) is used as the reference line for measuring the spinopelvic parameters and LL. However, in patients with a transitional lumbosacral vertebra (TLSV), the identification of the S1 endplate may be difficult because there are two options for sacral endplates [10]: upper and lower endplates. A TLSV is a congenital segmentation abnormality of the lumbosacral region observed in approximately 36% of asymptomatic and symptomatic patients and in 20% of adolescent idiopathic scoliosis patients [11,12,13]. It originates from either the L5 or the S1 vertebra and possesses morphological characteristics of both the vertebrae. On lateral radiographs, a TLSV usually mimics the vertebra other than its origin; in such a situation, a TLSV originating from L5 appears morphologically similar to S1 and can be labeled as a sacralized L5, whereas an S1 vertebra resembling the lumbar vertebrae, especially with a well-developed disk space below, can be labeled as a lumbarized sacral vertebra [10]. However, intermediate cases are not rare, and the origin of TLSV can be determined only after vertebral counting in lumbarization cases with six lumbar vertebrae, including TLSV, whereas sacralization cases contain five lumbar vertebrae, including TLSV. The spinopelvic parameters are usually reported according to the false sacral endplate (upper endplate in sacralized L5 cases and lower endplate in lumbarized S1 cases) [14, 15]. The other endplate (lower endplate of sacralize L5 and the upper endplate of summarized S1) is true. Determining the endplate holds a special value in such conditions because there are statistically significant differences between the spinopelvic parameters for the upper and lower endplates, which differ considerably from the normative values [10], although there is no consensus on the selection of sacral endplate in patients with TLSV.
Khalsa et al. reported weak interobserver reliability of PI measurement in patients with TLSV owing to differences in the selection of the sacral endplate [16]. Zhou et al. reported that the spinopelvic parameters measured from the inferior endplate may indicate malalignment [10]. In this regard, Tatara et al. recently proposed a method to select the optimum vertebral level using PI and PT in patients with TLSV; however, this method was found to be unsatisfactory in 23% of the patients [17]. To address this concern, the present study has described a simple method to achieve standardization in the measurement of spinopelvic parameters and LL in patients with TLSV.
Materials and methods
This retrospective and observational study was conducted at the Department of Neurosurgery, Harran University, Sanliurfa, Turkey, after obtaining approval from the Local Ethics Committee. No additional informed consent for participation was required because of the retrospective nature of the study. We reviewed the medical records and abdominal computed tomography (CT) scans of all patients who were admitted to the hospital between January 2020 and December 2021 with the complaints of abdominal and urological symptoms. Of these patients, those (age 18–65 years; body mass index 20–35 kg/m2) without any symptoms or a history of surgery or trauma of the spine, pelvis, or lower extremity were included in the study. Patients without any spinal symptoms but whose CT image indicated obvious spinal deformity, spondylotic changes, spondylolisthesis, or spinal fracture were excluded from the study.
The Revolution GS/256 MSCT (General Electric, USA) scanner was used for all CT scans; measurements were performed using the Clear Canvas Workstation system (Synaptive Medical, Canada). First, the coronal images of TLSV were established as per the Castellvi classification (Table 1) [18]. If unilateral or bilateral bony fusion or articulation between the transverse process of most caudal vertebra and sacrum was detected, the diagnosis of TLSV was established. Second, coronal and axial images of the thoracolumbar junction were examined. Most caudal vertebrae with articulated ribs, including unilateral and hypoplastic ribs, were accepted as T12 vertebrae, and the first cranial vertebra without ribs was considered as L1 vertebrae according to the spinal deformity group radiographic measurement manual [19]. Next, on the midsagittal CT images, the upper endplate of the L1 vertebra and upper and lower endplates of the TLSV were determined, and the lumbar vertebrae above the TLSV were counted (Fig. 1). If case of four lumbar vertebrae above the TLSV, the case was a sacralized L5, whereas in case of five vertebrae above the TLSV, the case was a lumbarized S1. The spinopelvic parameters and LL were measured according to the upper and lower endplates. Therefore, in the sacralized L5 cases, upper and lower endplate-based LLs included four and five lumbar vertebrae, respectively, whereas in the lumbarized S1 cases, upper and lower endplate-based LLs included five and six lumbar vertebrae, respectively.
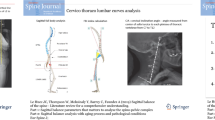
Diagnosis of TLSV and vertebral counting: A coronal CT scan image of a patient with TLSV Castellvi type 3A (arrow) and B coronal image of the same patient with a horizontal plane crossing through T12 vertebra (green line). Arrow showing most caudal unilateral costae. C Midsagittal image of the same patient with a green line showing same horizontal plane in Fig. 1B, crossing through T12 vertebra. There are four lumbar vertebrae above TLSV, so the case is a sacralized L5
The method used to measure the spinopelvic parameters (PI, PT, and SS) has been described in our previous study [20] (Fig. 2). Briefly, we determined the X and Y coordinates of both the femoral heads; the average value of the X and Y coordinates was used as the hip axis point in the midsagittal image, which was then used as the reference point to measure the spinopelvic parameters, as detailed below:
-
(1)
PI: Angle formed between the line perpendicular to the sacral endplate at its midpoint and the line connecting this point to the midpoint of the femoral head axes.
-
(2)
PT: Angle formed among an imaginary line joining the midpoints of the sacral endplate, the femoral head axes, and the vertical plumb line.
-
(3)
SS: Angle formed between a line parallel to the sacral endplate and the horizontal.
-
(4)
LL: Angle between the L1 and S1 upper endplates.
-
(5)
PI–LL: PI value minus LL value.
The steps of radiological evaluation are summarized in Table 2.
Statistical analysis
Two sets of radiological spinopelvic parameters were measured using the upper and lower endplates. In addition, we measured the spinopelvic parameters and LL of randomly selected patients without TLSV to be used as control. An average PI was calculated for both the sets of measurements (using the upper and lower endplates); a value closer to the mean PI of the control group was accepted as the valid PI value. Using this valid PI, a subgroup of patients was created and labeled as the optimum PI (OPI) group.
T-test and ANOVA were employed to compare two or more groups. In addition, the Chi-square test was used to determine the effect of sex and Castellvi classification group. It was also used to test the effects of sacralization and lumbarization on valid endplate selection. Pearson’s correlation coefficient was used to determine the correlation between different spinopelvic parameters in the control and OPI groups. Finally, linear regression analysis was performed to express the predictive formulas for LL using PI.
Results
We reviewed CT scans for 1420 patients, of which 108 had Castellvi type 2 or more TLSV. The average age of the patients with TLSV was 39.77 years (male: n = 56; female: n = 52). The TLSV and control groups were statistically comparable in terms of age and sex. A total of 64 patients had sacralized L5 (60%), and 44 patients had lumbarized S1 (40%).
In the TLSV group, all parameters measured according to the lower sacral endplate were significantly greater than those measured using the upper endplate (mean difference: PI = 27°; LL = 17°). These parameters were also different from the control group values; the spinopelvic parameters and LL of the control group were greater than those measured using the upper endplate, albeit lesser than those measured using the lower endplate (Table 3).
The average PI in the control group was 48.87°. Using this value as the reference, either the upper or lower endplate parameters of the TLSV group patients were accepted as valid, whichever was closer. Accordingly, the OPI group was created using the upper endplate parameters in 65 patients (60%) and lower endplate parameters in the remaining 43 patients (40%) (Figs. 3 and 4). Using these data, we obtained the following average spinopelvic parameters and LL values for the OPI group: PI = 45.9° ± 8.53°; PT = 9.37° ± 6.20°; SS = 36.52° ± 6.93°; LL = 45.35° ± 9.42°; and PI–LL: 0.55° ± 9.72°.
Midsagittal CT images of a patient with TLSV: spinopelvic parameters of upper endplate (A) and lower endplate (B). Upper endplate PI is closer to mean PI values of normal cohort (48.87°) so, upper endplates values are valid. TLSV is a sacralized L5, so upper and lower endplate LLs include four and five lumbar vertebrae, respectively. TLSV: Transitional lumbosacral vertebra, LL: Lumbar lordosis. PI: Pelvic incidence, PT: Pelvic tilt, SS: Sacral slope
Midsagittal CT images of another patient with TLSV: spinopelvic parameters of upper endplate (A) and lower endplate (B). Lower endplate parameters are valid. TLSV is a lumbarized S1, so upper and lower endplate LLs include five and six lumbar vertebrae, respectively. TLSV: Transitional lumbosacral vertebra, LL: Lumbar lordosis. PI: Pelvic incidence, PT: Pelvic tilt, SS: Sacral slope
On comparing the OPI group values with the normative values, no statistically significant difference was noted in the spinopelvic parameters and LL, except for SS (p:0.0314), which was statistically insignificant when computed at p < 0.01 (Table 4). The upper endplate was found to be valid in 40 (63%) patients with sacralization and in 25 (57%) patients with lumbarization, whereas the lower endplate was valid in 24 (37%) sacralization patients and 19 (43%) lumbarization patients. There was no difference in the frequency distribution of valid endplates between the sacralization and lumbarization groups (Table 5).
Furthermore, both the OPI and control groups showed similar values for the association between PI and LL in the respective groups; however, the correlation between PI and LL was weaker in the OPI group than in the control group (Table 6).
Finally, using linear regression, we obtained two equations for predicting LL based on the PI values of the control (LL: 0.886 PI + 4.8 [Control]) and OPI (LL: 0.448 PI + 25.15) [OPI] groups. These two regression lines had different slopes, but they crossed at 46° PI, which was indicated the mean PI in the OPI group. Furthermore, the two patient clusters in the OPI group (upper and lower endplate selected patient groups) were also close to the regression line of the normal cohort (Fig. 5). No statistically significant difference was noted between the selected upper and lower endplate parameters in terms of the Castellvi classification.
Discussion
The previous studies on the spinopelvic parameters in TLSV employed the false sacral endplate as the reference line [14, 15, 21, 22], that is, the upper endplate was used as the reference line in sacralization cases and the lower endplate in lumbarization cases. A previous study described two key facts about TLSV [23]. First, sacralization and lumbarization do not affect the upper and lower endplate spinopelvic parameters and LL per se, although they have different numbers of lumbar vertebrae. Second, when measured separately, a statistically significant difference was noted between the spinopelvic parameters and LL of the upper and lower endplates. In the current study, the differences between the PI and LL values for the upper and lower endplates were relatively constant (27° and 14°, respectively). Therefore, it can be reasonably deduced that the selection of the reference sacral plate can affect surgical alignment goals.
Nevertheless, there is no consensus yet on the optimal sacral endplate for patients with TLSV. Zhou et al. calculated the upper and lower endplate spinopelvic parameters and LL of 70 patients with TLSV and spinal pathologies and reported that the lower endplate parameters may imply sagittal malalignment because of the high PT and PI–LL values. The difference between the average values of some of the parameters calculated in our study, and the normative values can be attributed to the positional effect of a CT-based study [20]. In the supine position, PT and LL values decrease by 3°–4°, while SS and PI–LL increased by the same amount [24]. Therefore, in our study, the average PT and PI–LL of lower endplate were approximately 22° and 6° in the standing position, respectively.
When classifying spinal deformities, PT and PI–LL are the chief modifiers of this classification system and should be < 20° and 10°, respectively [25]. On the other hand, the average PT value in healthy subjects was reported to between − 5° and 35° [26]. Thus, there is no optimal PI–LL value, which should be calculated on the basis of individual PI [27,28,29]. According to Le Huec [30], the relationship between PI and LL is not linear, and the formula PI–LL < 10° is valid only for small PI values. Based on this evidence, it can be assumed that, in asymptomatic subjects with TLSV, the upper endplate parameters indicate a low PI alignment, whereas lower endplate parameters indicate a high PI alignment. This observation also implies that both the sets of parameters may not be within the normal ranges in some cases.
Tatara et al. recently proposed a method to standardize the selection of endplates in patients with TLSV. They determined a reference range (mean ± 2 standard deviation [SD]) for PI and PT using values from patients with degenerative spine disease, but without imbalance and TLSV. If either PI, PT, or both endplates were out of the reference range, the other endplate was accepted as the optimum vertebral level. When both the upper and lower endplate PI and PT values came within this mean ± 2 SD range, the situation was interpreted as an “intermediate type” and other parameters such as LL, TK, and C7-plumbline were recruited for decision [17]. Apparently, this method may seem similar to that used in our study, except for some major differences. First, it is more complex and confusing than our current method. Second, they used both PI and PT for the detection of the optimum endplate and determined the upper endplate as the optimum vertebral level in 52% of the cases because the PT value of the lower endplate in their study was frequently out of the normative range and not PI. The main reason for the high PT indicated by the authors was pelvic retroversion to compensate for sagittal balance in patients with degenerative lumbar spine disease. As seen in their example of the upper reference endplate, it is evident that in several cases, the results of Tatara et al.’s method and our method would be different. However, the most important disadvantage of Tatara et al.’s method, in 23% of the cases, was unsatisfactory, and it is unclear how to manage these cases. In addition, the average values of the selected spinopelvic parameters and LL were not reported [17]. In contrast, we observed no statistically significant difference between the spinopelvic parameters and LL of the OPI and control groups, except for SS (difference = 2.5°), which was insignificant at p < 0.01. In the OPI group, for 60% of the cases, the upper endplate parameters were selected, whereas the lower endplate parameters were selected in the remaining 40%. This finding is not surprising because the average PI value of the upper endplate was closer to the normative PI value relative to that of the lower endplate. In terms of sacralization and lumbarization, no statistically significant difference was noted in the frequency distribution of valid endplates between the two groups, although the frequency of valid upper endplates in the sacralization group was higher than that in the lumbarization group (63% vs. 57%). This finding conforms with the result of our previous study wherein the upper and lower endplate parameters were found to be similar between the sacralization and lumbarization groups [23].
Furthermore, nearly similar correlations were observed between the spinopelvic parameters of both the OPI and control groups, expect for the correlation between PI and LL in the former (r = 0.382 versus 0.796); however, this correlation was also statistically significant (r = 0.382, p = 0.007).
The linear regression analysis offered different LL predictive formulas for the OPI and control groups. The two regression lines crossed at 46° PI, and the OPI group appeared as two clusters of patients–one at ~ 41° (average PI of upper endplate selected patients) and the other at ~ 54° (average PI of lower endplate selected patients). The range of PI in the OPI group (32.8°–65.6°) was also narrower than that in the control group (22.3°–72.4°); in this narrow range, the regression lines were very close to each other. In the first cluster, the LL of the OPI group was 2°–3° greater than that of the control group, whereas in the second cluster (PI ~ 54°), the LL of the OPI group was 2°–3° lesser than that of the control group. Therefore, the formula obtained for predicting LL using PI in the control group can be used in patients with TLSV.
Similarly, the PT and PI–LL values of the OPI group appeared as two clusters instead of a normal distribution. These clusters were present at around 6.77° and 14.9° for PT and − 3.5° and 7.27° for PI–LL, respectively; nevertheless, all values were within the normal ranges.
In some previous studies, the authors excluded cases with Castellvi type 2 because they did not have a true bony union between the transverse processes of the TLSV and the sacrum [10]. Moreover, there is a moveable disk between the TLSV and sacrum in this variety. Therefore, it is presumed that TLSV is a part of the pelvis, and hence, the upper endplate should be considered the functional endplate in Castellvi type 3–4 [17]; accordingly, the lower endplate should be used as the functional endplate in Castellvi type 2. However, there is a strong evidence that the joints in Castellvi type 2 restrict movement and absorb the load [31, 32]. Furthermore, disk height is lower than normal at the inferior level of TLSV, implying the presence of a less mobile (and more stable) disk at TLSV [32]. In below the TLSV, there is no option of using the upper endplate as a reference line. As a result, disk degeneration and adjacent segment disease usually occur at the vertebral level above the TLSV; therefore, we included Castellvi type 2 cases in our study. Nevertheless, in cases of disk degeneration below the TLSV, there is no option of using the upper endplate as a reference line.
There are some limitations in this study. First, we included only asymptomatic subjects in the analysis. The inclusion of surgical candidates and results in symptomatic patients may have added more value to our results. Second, this was a CT-based study, and the spinopelvic parameters were measured in the supine position. Apart from PI, all other spinopelvic parameters changed with the position, and comparing them with normative values from the standing position did not seem appropriate. On the other hand, using CT scans was a strong point of this study as it is a more reliable imaging modality than plain radiography in the diagnosis and classification of TLSV [33]. CT scan is superior to X-ray for the detection of hypoplastic or short ribs simulating transverse processes on X-ray [34].
Conclusion
In patients with TLSV, the endplate associated with a PI value closer to the mean normative PI value can be selected as the reference line to measure the spinopelvic parameters and LL. This finding indicates that normative values for spinopelvic parameters and LL can serve as a criteria for diagnosis and surgical indications in patients with TLSV.
References
Legaye J, Duval-Beaupère G, Hecquet J, Marty C (1998) Pelvic incidence: a fundamental pelvic parameter for three-dimensional regulation of spinal sagittal curves. Eur Spine J 7(2):99–103. https://doi.org/10.1007/s005860050038
Vaz G, Roussouly P, Berthonnaud E, Dimnet J (2002) Sagittal morphology and equilibrium of pelvis and spine. Eur Spine J 11(1):80–87. https://doi.org/10.1007/s005860000224
Roussouly P, Gollogly S, Berthonnaud E, Dimnet J (2005) Classification of the normal variation in the sagittal alignment of the human lumbar spine and pelvis in the standing position. Spine (Phila Pa 1976) 30(3):346–53. https://doi.org/10.1097/01.brs.0000152379.54463.65
Mac-Thiong J-M, Labelle H, Charlebois M, Huot M-P, de JacquesGuise A (1976) Sagittal plane analysis of the spine and pelvis in adolescent idiopathic scoliosis according to the coronal curve type. Spine (Phila Pa 2003) 28(13):1404–9. https://doi.org/10.1097/01.BRS.0000067118.60199.D1
Le Huec JC, Leijssen P, Duarte M, Aunoble S (2011) Thoracolumbar imbalance analysis for osteotomy planification using a new method: FBI technique. Eur Spine J 20(Suppl 5):669–80. https://doi.org/10.1007/s00586-011-1935-y
Labelle H, Roussouly P, Berthonnaud E, Transfeldt E, O’Brien M, Chopin D, Hresko T, Dimnet J (1976) Spondylolisthesis, pelvic incidence, and spinopelvic balance: a correlation study. Spine (Phila Pa 1976) 29(18):2049–54. https://doi.org/10.1097/01.brs.0000138279.53439.cc
Kyrölä K, Repo J, Mecklin J-P, Ylinen J, Kautiainen H, Häkkinen A (2018) Spinopelvic changes based on the simplified SRS-Schwab adult spinal deformity classification: relationships with disability and health-related quality of life in adult patients with prolonged degenerative spinal disorders. Spine (Phila Pa 1976) 43(7):497–502. https://doi.org/10.1097/BRS.0000000000002370
Takemoto M, Boissière L, Vital J-M, Pellisé F, Perez-Grueso FJS, Kleinstück F, Acaroglu ER, Alanay A, Obeid I (2017) Are sagittal spinopelvic radiographic parameters significantly associated with quality of life of adult spinal deformity patients? Multivariate linear regression analyses for pre-operative and short-term post-operative health-related quality of life. Eur Spine J 26(8):2176–2186. https://doi.org/10.1007/s00586-016-4872-y
Schwab F, Patel A, Ungar B, Farcy J-P, Lafage V (2010) Adult spinal deformity-postoperative standing imbalance: how much can you tolerate? An overview of key parameters in assessing alignment and planning corrective surgery. Spine (Phila Pa 1976) 35(25):2224–31. https://doi.org/10.1097/BRS.0b013e3181ee6bd4
Zhou PL, Moon JY, Tishelman JC, Errico TJ, Protopsaltis TS, Passias PG, Buckland AJ (2018) Interpretation of spinal radiographic parameters in patients with transitional lumbosacral vertebrae. Spine Deform 6(5):587–592. https://doi.org/10.1016/j.jspd.2018.01.004
Apazidis A, Ricart PA, Diefenbach CM, Spivak JM (2011) The prevalence of transitional vertebrae in the lumbar spine. Spine J 11(9):858–862. https://doi.org/10.1016/j.spinee.2011.08.005
Tang M, Yang X-F, Yang S-W, Han Peng, Ma Y, Yu H, Zhu B (2014) Lumbosacral transitional vertebra in a population-based study of 5860 individuals: prevalence and relationship to low back pain. Eur J Radiol 83(9):1679–1682
Garg B, Mehta N, Goyal A, Rangaswamy N, Upadhayay A (2021) Variations in the number of thoracic and lumbar vertebrae in patients with adolescent idiopathic scoliosis: a retrospective. Observ Study Int J Spine Surg 15(2):359–367. https://doi.org/10.14444/8047
Price R, Okamoto M, Le Huec JC, Hasegawa K (2016) Normative spino-pelvic parameters in patients with the lumbarization of S1 compared to a normal asymptomatic population. Eur Spine J 25(11):3694–3698. https://doi.org/10.1007/s00586-016-4794-8
Dominguez D, Faundez A, Demezon H, Cogniet A, Le Huec JC (2016) Normative values for the L5 incidence in a subgroup of transitional anomalies extracted from 147 asymptomatic subjects. Eur Spine J 25(11):3602–3607. https://doi.org/10.1007/s00586-015-4371-6
Khalsa AS, Mundis GM Jr, Yagi M, Fessler RG, Bess S, Park P, Than KD, Daniels A, Iorio J, Ledesma JB, Tran S, Eastlack RK (2018) International spine study group variability in assessing spinopelvic parameters with lumbosacral transitional vertebrae. Spine 43(12):813–816
Tatara Y, Niimura T, Sakaguchi A, Katayama H, Mihara H (2022) Optimum vertebral level of castellvi type iii or higher lumbosacral transitional vertebrae when measuring spinopelvic parameters. Int J Spine Surg 16(5):868–874. https://doi.org/10.14444/8346
Castellvi AE, Goldstein LA, Chan DP (1984) Lumbosacral transitional vertebrae and their relationship with lumbar extradural defects. Spine (Phila Pa 1976) 9(5):493–5. https://doi.org/10.1097/00007632-198407000-00014
O’Brien MF, Kuklo TR,Blanke KM, Lenke LG (2008) Spinal deformity study group. Radiographic measurement manual. Medtronic Sofamor Danek USA
İplikçioğlu AC, Karabağ H (2022) Validity and reliability of spinopelvic parameters measured on computed tomography. Int J Spine Surg 16(5):875–880. https://doi.org/10.14444/8344
Yokoyama K, Kawanishi M, Yamada M, Tanaka H, Ito Y, Kawabata S, Kuroiwa T (2016) Spinopelvic alignment and sagittal balance of asymptomatic adults with 6 lumbar vertebrae. Eur Spine J 25(11):3583–3588. https://doi.org/10.1007/s00586-015-4284-4
Kyrölä K, Kautiainen H, Ylinen J, Lehtola R, Kiviranta I, Häkkinen A (2019) Spinopelvic parameters and sagittal alignment of symptomatic degenerative adult spinal disorder patients with 6 lumbar vertebrae. Clin Spine Surg 32(1):E43–E49. https://doi.org/10.1097/BSD.0000000000000715
Karabag H, Iplikçioğlu AC (2024) Analysis of spinopelvic parameters and lumbar lordosis in patients with transitional lumbosacral vertebrae, with special reference to sacralization and lumbarization, World Neurosurg (Accepted for publishing)
Chevillotte T, Coudert P, Derek Cawley D, Bouloussa H, Mazas S, Boissière L, Gille O (2018) Influence of posture on relationships between pelvic parameters and lumbar lordosis: comparison of the standing, seated, and supine positions. A preliminary study. Orthop Traumatol Surg Res 104(5):565–568. https://doi.org/10.1016/j.otsr.2018.06.005
Schwab F, Ungar B, Blondel B, Buchowski J, Coe J, Deinlein D, DeWald C, Mehdian H, Shaffrey C, Tribus C, Lafage V (2012) Scoliosis Research Society-Schwab adult spinal deformity classification: a validation study. Spine (Phila Pa 1976) 37(12):1077–82. https://doi.org/10.1097/BRS.0b013e31823e15e2
Cho Y, Jo DJ, Hyun S-J, Park JH, Yang NR (2023) From the spinopelvic parameters to global alignment and proportion scores in adult spinal deformity. Neurospine 20(2):467–477. https://doi.org/10.14245/ns.2346374.187
Inami S, Moridaira H, Takeuchi D, Shiba Y, Nohara Y, Taneichi H (2016) Optimum pelvic incidence minus lumbar lordosis value can be determined by individual pelvic incidence. Eur Spine J 25(11):3638–3643. https://doi.org/10.1007/s00586-016-4563-8
Yilgor C, Sogunmez N, Yavuz Y, Abul K, Boissiére L, Haddad S, Obeid I, Kleinstück F, Pérez-Grueso FJS, Acaroğlu E, Mannion AF, Pellise F, Alanay A, European Spine Study Group (2017) Relative lumbar lordosis and lordosis distribution index: individualized pelvic incidence-based proportional parameters that quantify lumbar lordosis more precisely than the concept of pelvic incidence minus lumbar lordosis. Neurosurg Focus 43(6):5. https://doi.org/10.3171/2017.8
Bourret S, Cerpa M, Kelly MP, Hasegawa K, Hey HWD, Wong H-K, Liu G, Sardar ZM, Riahi H, Lenke LG, Le Huec JC (2022) Correlation analysis of the PI-LL mismatch according to the pelvic incidence from a database of 468 asymptomatic volunteers. Eur Spine J 31(6):1413–1420. https://doi.org/10.1007/s00586-021-07087-6
Le Huec JC, Thompson W, Mohsinaly Y, Barrey C, Faundez A (2019) Sagittal balance of the spine. Eur Spine J 28(9):1889–1905. https://doi.org/10.1007/s00586-019-06083-1
Konin GP, Walz DM (2010) Lumbosacral transitional vertebrae: classification, imaging findings, and clinical relevance. AJNR Am J Neuroradiol 31(10):1778–86. https://doi.org/10.3174/ajnr.A2036
Luoma K, Vehmas T, Raininko R, Luukkonen R, Riihimäki H (2004) Lumbosacral transitional vertebra: relation to disc degeneration and low back pain. Spine (Phila Pa 1976) 29(2):200–5. https://doi.org/10.1097/01.BRS.0000107223.02346.A8
Hou L, Bai X, Li H, Gao T, Li W, Wen T, He Q, Ruan D, Shi L, Bing W (2020) Lumbar plain radiograph is not reliable to identify lumbosacral transitional vertebra types according to Castellvi classification principle. BMC Musculoskelet Disord 21:333–340. https://doi.org/10.1186/s12891-020-03358-3
Tatara Y, Niimura T, Sekiya T, Mihara H (2021) Changes in lumbosacral anatomy and vertebral numbering in patients with thoracolumbar and/or lumbosacral transitional vertebrae. JB JS Open Access 6(3):e2000167. https://doi.org/10.2106/JBJS.OA.20.00167
Funding
Open access funding provided by the Scientific and Technological Research Council of Türkiye (TÜBİTAK). The financing of the article has been met by the authors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
There is no conflict of interest between the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Iplikcioglu, A.C., Karabag, H. A simple method for the selection of valid spinopelvic parameters and lumbar lordosis in patients with transitional lumbosacral vertebrae. Eur Spine J (2024). https://doi.org/10.1007/s00586-024-08220-x
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00586-024-08220-x